Abstract
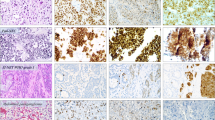
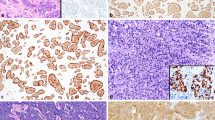
Neuroendocrine neoplasms (NENs) are derived from endocrine cells in various organs and share common morphological features. This study aimed to clarify whether NENs of different organs are comparable at the molecular pathologic level. We retrospectively collected 99 cases of NENs from gastro-entero-pancreatic, lung, and other organs and reclassified these according to identical criteria. Grade, site, and molecular expression profile including NE markers, Ki-67, p53, somatostatin receptor type 2A (SSTR2A), and phosphatase and tensin homolog (PTEN) were compared. PTEN immunoreactivity was also compared with genomic copy number by fluorescence in situ hybridization (FISH) and droplet digital polymerase chain reaction (ddPCR). No significant differences were observed in the immunoreactivities of NE markers, p53, SSTR2A, or PTEN expression in NENs between the different organ sites. PTEN and p53 functional inactivation along with the loss of membranous SSTR2A expression appeared to be commonly involved in high-grade NEN. FISH results were significantly correlated with the level of PTEN immunoreactivity and with the findings of ddPCR analyses. The demonstration that these tumors are comparable at the molecular level will likely contribute to the broadening of therapeutic options such as the use of somatostatin analogues and mTOR inhibitors against NENs regardless of the affected organ, whereas molecular characterization of tumor grade will be useful for determining treatment strategy.



Similar content being viewed by others
References
Yao JC, Hassan M, Phan A et al. (2008) One Hundred Years After “Carcinoid”: epidemiology of and prognostic factors for neuroendocrine tumors in 35,825 cases in the United States. J Clin Oncol 26:3063–3072.
Travis WD, Gazdar A, Brambilla E et al. (2004) Carcinoid tumour. In: Travis WD, Brambilla E, Burke AP, Marx A, Nicholson AG (eds) Pathology and genetics of tumours of the lung, pleura, thymus and heart (World Health Organization Classification of Tumours). IARC Press, Lyon, pp 59–62.
Klimstra DS, Arnold R, Capella C et al. Neuroendocrine neoplasms of the pancreas. (2010) In: Bosman FT, Carneiro F, Hruban RH Theise ND (ed) WHO classification of tumours of the digestive system (World Health Organization Classification of Tumours). IARC Press, Lyon, pp 322–326.
Dacic S, Finkelstein SD, Baksh FK, Swalsky PA, Barnes LE, Yousem SA (2002) Small-cell neuroendocrine carcinoma displays unique profiles of tumor-suppressor gene loss in relationship to the primary site of formation. Hum Pathol 33:927–932.
Ross JS, Wang K, Elkadi OR et al. (2014) Next-generation sequencing reveals frequent consistent genomic alterations in small cell undifferentiated lung cancer. J Clin Pathol 67:772–776.
Mussazhanova Z, Miura S, Stanojevic B et al. (2014) Radiation-associated small cell neuroendocrine carcinoma of the thyroid: a case report with molecular analyses. Thyroid 24:593–598.
Raymond E, Dahan L, Raoul J et al. (2011) Sunitinib malate for the treatment of pancreatic neuroendocrine tumors. N Engl J Med 364:501–513.
Yao JC, Shah MH, Ito T et al. (2011) Everolimus for advanced pancreatic neuroendocrine tumors. N Engl J Med 10:514–523.
Pavel ME, Hainsworth JD, Baudin E et al. (2011) Everolimus plus octreotide long-acting repeatable for the treatment of advanced neuroendocrine tumours associated with carinoid syndrome (RADIANT-2): a randomised, placebo- controlled, phase 3 study. Lancet 10:2005–2012.
Missiaglia E, Dalai I, Barbi S et al. (2010) Pancreatic endocrine tumors: expression profiling evidences a role for AKT-mTOR pathway. J Clin Oncol 28:245–255.
Lipkin JS, Rizvi SM, Gatalica Z et al. (2015) Therapeutic approach guided by genetic alteration: use of MTOR inhibitor in renal medullary carcinoma with loss of PTEN expression. Cancer Biol Ther 16:28–33.
Liu H, Du L, Wang R et al. (2015) High frequency of loss of PTEN expression in human solid salivary adenoid cystic carcinoma and its implication for targeted therapy. Oncotarget 6:11477–11491.
Anlauf M, Perren A, Henopp T et al. (2007) Allelic deletion of the MEN1 gene in duodenal gastrin and somatostatin cell neoplasms and their precursor lesions. Gut 56:637–644.
Rinke A, Müller HH, Schade-Brittinger C et al. (2009) Placebo-controlled, double-blind, prospective, randomized study on the effect of octreotide LAR in the control of tumor growth in patients with metastatic neuroendocrine midgut tumors: A report From the PROMID Study Group. J Clin Oncol 27:4656–4663.
Travis WD. The concept of pulmonary neuroendocrine tumours. (2004) In: Travis WD, Brambilla E, Burke AP, Marx A, Nicholson AG (eds) Pathology and genetics of tumours of the lung, pleura, thymus and heart (World Health Organization Classification of Tumours). IARC Press, Lyon, 19–20.
Volante M, Brizzi MP, Faqqiano A et al. (2007) Somatostatin receptor type 2A immunohistochemistry in neuroendocrine tumors: a proposal of scoring system correlated with somatostatin receptor scintigraphy. Mod Pathol 20:1172–1182.
Oikawa M, Yoshiura K, Kondo H, Miura S, Nagayasu T, Nakashima M. (2011) Significance of genomic instability in breast cancer in atomic bomb survivors: analysis of microarray-comparative genomic hybridisation. Radiat Oncol 6:168.
Pasaoglu E, Dursun N, Ozyalvacli G, Hacihasanoglu E, Behzatoglu K, Calay O. (2015) Comparison of World Health Organization 2000/2004 and World Health Organization 2010 classifications for gastrointestinal and pancreatic neuroendocrine tumors. Ann Diagn Pathol 19:81–87.
Karakuş E, Helvacı A, Ekinci O, Dursun A. (2014) Comparison of WHO 2000 and WHO 2010 classifications of gastroenteropancreatic neuroendocrine tumors. Turk J Gastroenterol 25:81–87.
Estrozi B, Bacchi CE. (2011) Neuroendocrine tumors involving the gastroenteropancreatic tract: a clinicopathological evaluation of 773 cases. Clinics (Sao Paulo) 66:1671–1675.
Fazio N, Granberg D, Grossman A et al. (2013) Everolimus plus octreotide long-acting repeatable in patients with advanced lung neuroendocrine tumors: analysis of the phase 3, randomized, placebo-controlled RADIANT-2 study. Chest 143:955–962.
Travis WD. (2010) Advances in neuroendocrine lung tumors. Ann Oncol 21:vii65–71.
Asamura H, Kameya T, Matsuno Y et al. (2006) Neuroendocrine neoplasms of the lung: a prognostic spectrum. J Clin Oncol 24:70–76.
Przygodzky RM, Finkelstein SD, Langer JC et al. (1996) Analysis of p53, K-ras-2, and C-raf-1 in pulmonary neuroendocrine tumors. Correlation with histological subtype and clinical outcome. Am J Pathol 148:1531–1541.
Leotlela PD, Jauch A, Holtgreve-Grez H, Thakker RV. (2003) Genetics of neuroendocrine and carcinoid tumours. Endocr Relat Cancer 10:437–450.
Grabowski P, Schrader J, Wanger J et al. (2008) Loss of nuclear p27 expression and Its prognostic role in relation to cyclin E and p53 mutation in gastroenteropancreatic neuroendocrine tumors. Clin Cancer Res 14:7378–7384.
Hu W, Feng Z, Modica I et al. (2010) Gene amplifications in well-differentiated pancreatic neuroendocrine tumors inactivate the p53 pathway. Genes Cancer 1:360–368.
Yachida S, Vakiani E, White CM et al. (2012) Small cell and large cell neuroendocrine carcinomas of the pancreas are genetically similar and distinct from well-differentiated pancreatic neuroendocrine tumors. Am J Surg Pathol 36:173– 184.
Tan HL, Sood A, Rahimi HA et al. (2014) Rb loss is characteristic of prostatic small cell neuroendocrine carcinoma. Clin Cancer Res. 20:890–903.
Pyronnet S, Bousquet C, Najib S, Azar R, Laklai H, Susini C. (2008) Antitumor effects of somatostatin. Mol Cell Endocrinol 286:230–237.
Fan X, Aalto Y, Sanko SG, Knuutila S, Klatzmann D, Castresana JS. (2002) Genetic profile, PTEN mutation and therapeutic role of PTEN in glioblastomas. Int J Oncol 21:1141–1150.
Deichmann M, Thome M, Benner A, Egner U, Hartschuh W, Näher H. (2002) PTEN/MMAC1 expression in melanoma resection specimens. Br J Cancer 87:1431–1436.
Halachmi N, Halachmi S, Evron E et al. (1998) Somatic mutations of the PTEN tumor suppressor gene in sporadic follicular thyroid tumors. Genes Chromosomes Cancer 23:239–243.
Bose S, Wang SI, Terry MB, Hibshoosh H, Parsons R. (1998) Allelic loss of chromosome 10q23 is associated with tumor progression in breast carcinomas. Oncogene 17:123–127.
Martini M, Ciccarone M, Garganese G et al. (2002) Possible involvement of hMLH1, p16(INK4a) and PTEN in the malignant transformation of endometriosis. Int J Cancer 102:398–406.
Risinger JI, Hayes AK, Berchuk A, Barrett JC. (1997) PTEN/MMAC1 mutations in endometrial cancers. Cancer Res 57:4736–4738.
Fujii H, Matsumoto T, Yoshida M et al. (2002) Genetics of synchronous uterine and ovarian endometrioid carcinoma: combined analyses of loss of heterozygosity, PTEN mutation, and microsatellite instability. Hum Pathol 33:421–428
Mutter GL. (2001) Pten, a protean tumor suppressor. Am J Pathol 158:1895–1898
Jiao Y, Shi C, Edil BH et al. (2011) DAXX/ATRX, MEN1, and mTOR pathway genes are frequently altered in pancreatic neuroendocrine tumors. Science 331:1199–1203.
Voortman J, Lee JH, Killian JK et al. (2010) Array comparative genomic hybridization-based characterization of genetic alterations in pulmonary neuroendocrine tumors. Proc Natl Acad Sci U S A 107:13040–13045.
Acknowledgments
This work was supported in part by a collaborative research grant from the Atomic Bomb Disease Institute, Nagasaki University. We would like to thank Editage (www.editage.jp) for English language editing.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Compliance with Ethical Standards
The present study was an unlinkable anonymized study strictly following the principles established in the Declaration of Helsinki and was approved by the Committee for Ethical Issues of Nagasaki University Graduate School of Biomedical Sciences (Date of approval; Aug. 20, 2015, Protocol No. 15682035). As this was a retrospective research study involving minimal risk to the participants, detailed information of the research was released to the public on the institution’s homepage (http://www-sdc.med.nagasaki-u.ac.jp/pathology/index.html) following the guidelines of the Ethical Committee’s official disclosure system.
Conflict of Interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Wada, H., Matsuda, K., Akazawa, Y. et al. Expression of Somatostatin Receptor Type 2A and PTEN in Neuroendocrine Neoplasms Is Associated with Tumor Grade but Not with Site of Origin. Endocr Pathol 27, 179–187 (2016). https://doi.org/10.1007/s12022-016-9436-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12022-016-9436-5