Abstract
Purpose
This study primarily investigated the effects of hypoglycemic compounds (Imeglimin derivatives) on insulin secretion in type 2 diabetes mellitus (T2DM), and further explored the possible mechanism underlying these effects.
Methods
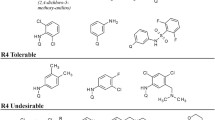
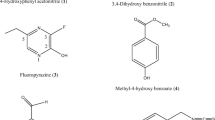
Firstly, Metformin was used as the initiating compound to synthesize three sets of derivatives which contained Imeglimin structure core. At the cellular level, we screened compounds with better effect on the activity of insulin receptor tyrosine protein kinase (IFcTPK) after the islet β cells were treated with the compounds of different concentrations. The insulin secretion was assessed using radioimmunoassay and the cytotoxicity to islet β cells was evaluated by means of MTT assay following treatment with the compounds. The Ca2+-related mechanism by which these compounds promote insulin secretion was elucidated with whole cell recordings from current-clamp mode.
Results
Totally, 48 synthesized compounds were generated, wherein 10 compounds could increase the activity of IFcTPK in HIT-T15 cells better among these compounds. The modified Imeglimin, especially in the structure of hydrophilic hydroxyl or piperidine rings, could improve the activity of the compound to promote insulin secretion. Furthermore, the compounds 8a, 8b, 8k, and 9h revealed high insulin secretion-promoting activity. These compounds enhanced insulin secretion in islet β cells by repressing the ATP-sensitive K(+) and voltage-gated K+ pathway.
Conclusions
Our findings indicate that the hypoglycemic compounds 8a, 8b, 8k, and 9h confer better promotive effect on insulin secretion, which provides a reference for the development of drugs with better hypoglycemic activity.










Similar content being viewed by others
Data availability
The datasets generated/analyzed during the current study are available.
Abbreviations
- IFcTPK:
-
insulin receptor tyrosine protein kinase
- T2DM:
-
Type 2 diabetes mellitus
- TPK:
-
tyrosine protein kinase
- PBS:
-
phosphate-buffered saline
- ANOVA:
-
analysis of variance
- TLC:
-
thin layer chromatography
References
R.A. DeFronzo, E. Ferrannini, L. Groop, R.R. Henry, W.H. Herman, J.J. Holst, F.B. Hu, C.R. Kahn, I. Raz, G.I. Shulman, D.C. Simonson, M.A. Testa, R. Weiss, Type 2 diabetes mellitus. Nat. Rev. Dis. Prim. 1, 15019 (2015). https://doi.org/10.1038/nrdp.2015.19
G. Ning, Decade in review-type 2 diabetes mellitus: at the centre of things. Nat. Rev. Endocrinol. 11(11), 636–638 (2015). https://doi.org/10.1038/nrendo.2015.147
A.A. Tahrani, A.H. Barnett, C.J. Bailey, Pharmacology and therapeutic implications of current drugs for type 2 diabetes mellitus. Nat. Rev. Endocrinol. 12, 566–592 (2016). https://doi.org/10.1038/nrendo.2016.86
R.F. Rocha, T. Rodrigues, A.C.O. Menegatti, G.J.L. Bernardes, H. Terenzi, The antidiabetic drug lobeglitazone has the potential to inhibit PTP1B activity. Bioorg. Chem. 100, 103927 (2020). https://doi.org/10.1016/j.bioorg.2020.103927
D.M. Irwin, Variation in the rates of evolution of the insulin and glucagon hormone and receptor genes in rodents. Gene 728, 144296 (2020). https://doi.org/10.1016/j.gene.2019.144296
T.D. Olver, Z.I. Grunewald, T. Ghiarone, R.M. Restaino, A.R.K. Sales, L.K. Park, P.K. Thorne, R.R. Ganga, C.A. Emter, P.W.R. Lemon, J.K. Shoemaker, C. Manrique-Acevedo, L.A. Martinez-Lemus, J. Padilla, Persistent insulin signaling coupled with restricted PI3K activation causes insulin-induced vasoconstriction. Am. J. Physiol. Heart Circ. Physiol. 317, H1166–H1172 (2019). https://doi.org/10.1152/ajpheart.00464.2019
J.L. Tarry-Adkins, C.E. Aiken, S.E. Ozanne, Neonatal, infant, and childhood growth following metformin versus insulin treatment for gestational diabetes: a systematic review and meta-analysis. PLoS Med. 16, e1002848 (2019). https://doi.org/10.1371/journal.pmed.1002848
S.J. Pilla, J.R. Dotimas, N.M. Maruthur, J.M. Clark, H.C. Yeh, Changes in metformin use and other antihyperglycemic therapies after insulin initiation in patients with type 2 diabetes. Diabetes Res. Clin. Pr. 139, 221–229 (2018). https://doi.org/10.1016/j.diabres.2018.02.032
R. Yendapally, D. Sikazwe, S.S. Kim, S. Ramsinghani, R. Fraser-Spears, A.P. Witte, B. La-Viola, A review of phenformin, metformin, and imeglimin. Drug Dev. Res. (2020). https://doi.org/10.1002/ddr.21636
G. Vial, M.A. Chauvin, N. Bendridi, A. Durand, E. Meugnier, A.M. Madec, N. Bernoud-Hubac, J.P. Pais de Barros, E. Fontaine, C. Acquaviva, S. Hallakou-Bozec, S. Bolze, H. Vidal, J. Rieusset, Imeglimin normalizes glucose tolerance and insulin sensitivity and improves mitochondrial function in liver of a high-fat, high-sucrose diet mice model. Diabetes 64, 2254–2264 (2015). https://doi.org/10.2337/db14-1220
R.J. Perry, R.L. Cardone, M.C. Petersen, D. Zhang, P. Fouqueray, S. Hallakou-Bozec, S. Bolze, G.I. Shulman, K.F. Petersen, R.G. Kibbey, Imeglimin lowers glucose primarily by amplifying glucose-stimulated insulin secretion in high-fat-fed rodents. Am. J. Physiol. Endocrinol. Metab. 311, E461–E470 (2016). https://doi.org/10.1152/ajpendo.00009.2016
J.Y. Cho, J. Choi, J.G. Park, Y.S. Yi, M.J. Hossen, H. Kim, J. Ro, B.C. Cha, E.S. Yoo, J.H. Kim, J. Lee, Alcohol-induced hyperlipidemia is ameliorated by orally administered DWP208, a sodium succinate form of ZYM201. Korean J. Physiol. Pharm. 18, 469–474 (2014). https://doi.org/10.4196/kjpp.2014.18.6.469
S.Y. Kodera, M. Yoshida, K. Dezaki, T. Yada, T. Murayama, M. Kawakami, M. Kakei, Inhibition of insulin secretion from rat pancreatic islets by dexmedetomidine and medetomidine, two sedatives frequently used in clinical settings. Endocr. J. 60, 337–346 (2013). https://doi.org/10.1507/endocrj.ej12-0308
R. Meng, J. Mahadevan, E. Oseid, S. Vallerie, R.P. Robertson, Silymarin Activates c-AMP phosphodiesterase and stimulates insulin secretion in a glucose-dependent manner in HIT-T15 Cells. Antioxidants 5, (2016). https://doi.org/10.3390/antiox5040047
M.Y. Ali, M. Whiteman, C.M. Low, P.K. Moore, Hydrogen sulphide reduces insulin secretion from HIT-T15 cells by a KATP channel-dependent pathway. J. Endocrinol. 195, 105–112 (2007). https://doi.org/10.1677/JOE-07-0184
Z. Qi, Y. Xu, Z. Liang, S. Li, J. Wang, Y. Wei, B. Dong, Baicalein alters PI3K/Akt/GSK3beta signaling pathway in rats with diabetes-associated cognitive deficits. Int J. Clin. Exp. Med. 8, 1993–2000 (2015)
J. Herrington, Y.P. Zhou, R.M. Bugianesi, P.M. Dulski, Y. Feng, V.A. Warren, M.M. Smith, M.G. Kohler, V.M. Garsky, M. Sanchez, M. Wagner, K. Raphaelli, P. Banerjee, C. Ahaghotu, D. Wunderler, B.T. Priest, J.T. Mehl, M.L. Garcia, O.B. McManus, G.J. Kaczorowski, R.S. Slaughter, Blockers of the delayed-rectifier potassium current in pancreatic beta-cells enhance glucose-dependent insulin secretion. Diabetes 55, 1034–1042 (2006). https://doi.org/10.2337/diabetes.55.04.06.db05-0788
P. Llanos, A. Contreras-Ferrat, G. Barrientos, M. Valencia, D. Mears, C. Hidalgo, Glucose-dependent insulin secretion in pancreatic beta-cell islets from male rats requires Ca2+ release via ROS-stimulated ryanodine receptors. PLoS ONE 10, e0129238 (2015). https://doi.org/10.1371/journal.pone.0129238
Z. Laron, H. Werner, Insulin: a growth hormone and potential oncogene. Pediatr. Endocrinol. Rev. 17, 191–197 (2020). https://doi.org/10.17458/per.vol17.2020.lw.insulinghpotentialoncogene
M. Vakilian, Y. Tahamtani, K. Ghaedi, A review on insulin trafficking and exocytosis. Gene 706, 52–61 (2019). https://doi.org/10.1016/j.gene.2019.04.063
Y. Zhao, M. Sun, Metformin rescues Parkin protein expression and mitophagy in high glucose-challenged human renal epithelial cells by inhibiting NF-kappaB via PP2A activation. Life Sci. 246, 117382 (2020). https://doi.org/10.1016/j.lfs.2020.117382
L. Jennings, R. Hambly, R. Hughes, B. Moriarty, B. Kirby, Metformin use in hidradenitis suppurativa. J. Dermatol. Treat. 31, 261–263 (2020). https://doi.org/10.1080/09546634.2019.1592100
K. Hamano, K. Akita, Y. Takeuchi, T. Suwa, J. Takeda, S. Dodo, Glucose-responsive Insulinoma with Insulin Hypersecretion Suppressed by Metformin. Intern. Med. 58, 3563–3568 (2019). https://doi.org/10.2169/internalmedicine.3318-19
P. Fouqueray, S. Perrimond-Dauchy, S. Bolze, Imeglimin does not induce clinically relevant pharmacokinetic interactions when combined with either metformin or sitagliptin in healthy subjects. Clin. Pharmacokinet. (2020). https://doi.org/10.1007/s40262-020-00886-y
H. Yaribeygi, M. Maleki, T. Sathyapalan, T. Jamialahmadi, A. Sahebkar, Molecular mechanisms by which imeglimin improves glucose homeostasis. J. Diabetes Res. 2020, 8768954 (2020). https://doi.org/10.1155/2020/8768954
G. Pacini, A. Mari, P. Fouqueray, S. Bolze, M. Roden, Imeglimin increases glucose-dependent insulin secretion and improves beta-cell function in patients with type 2 diabetes. Diabetes Obes. Metab. 17, 541–545 (2015). https://doi.org/10.1111/dom.12452
K. Harada, J. Mizukami, S. Kadowaki, I. Matsuda, T. Watanabe, Y. Oe, Y. Kodama, K. Aoki, K. Suwa, S. Fukuda, S. Yata, T. Inaba, Design and synthesis of novel and potent GPR119 agonists with a spirocyclic structure. Bioorg. Med Chem. Lett. 28, 1228–1233 (2018). https://doi.org/10.1016/j.bmcl.2018.02.044
H.J. Mest, A. Raap, J. Schloos, I. Treinies, M. Paal, U. Giese, V. Koivisto, Glucose-induced insulin secretion is potentiated by a new imidazoline compound. Naunyn Schmiedebergs Arch. Pharm. 364, 47–52 (2001). https://doi.org/10.1007/s002100100415
G. da Luz, M.J. Frederico, A.J. Castro, A.L. Moraes, F.K. de Carvalho, L. Espindola, E.C. Schmidt, Z.L. Bouzon, M.G. Pizzolatti, F.R. Silva, Triterpene derivative: A potential signaling pathway for the fern-9(11)-ene-2alpha,3beta-diol on insulin secretion in pancreatic islet. Life Sci. 154, 58–65 (2016). https://doi.org/10.1016/j.lfs.2016.04.027
J. Ryu, A.K. Galan, X. Xin, F. Dong, M.A. Abdul-Ghani, L. Zhou, C. Wang, C. Li, B.M. Holmes, L.B. Sloane, S.N. Austad, S. Guo, N. Musi, R.A. DeFronzo, C. Deng, M.F. White, F. Liu, L.Q. Dong, APPL1 potentiates insulin sensitivity by facilitating the binding of IRS1/2 to the insulin receptor. Cell Rep. 7, 1227–1238 (2014). https://doi.org/10.1016/j.celrep.2014.04.006
F. Oriente, S. Iovino, S. Cabaro, A. Cassese, E. Longobardi, C. Miele, P. Ungaro, P. Formisano, F. Blasi, F. Beguinot, Prep1 controls insulin glucoregulatory function in liver by transcriptional targeting of SHP1 tyrosine phosphatase. Diabetes 60, 138–147 (2011). https://doi.org/10.2337/db10-0860
E. Choi, S. Kikuchi, H. Gao, K. Brodzik, I. Nassour, A. Yopp, A.G. Singal, H. Zhu, H. Yu, Mitotic regulators and the SHP2-MAPK pathway promote IR endocytosis and feedback regulation of insulin signaling. Nat. Commun. 10, 1473 (2019). https://doi.org/10.1038/s41467-019-09318-3
M. Niessen, F. Jaschinski, F. Item, M.P. McNamara, G.A. Spinas, T. Trub, Insulin receptor substrates 1 and 2 but not Shc can activate the insulin receptor independent of insulin and induce proliferation in CHO-IR cells. Exp. Cell. Res. 313, 805–815 (2007). https://doi.org/10.1016/j.yexcr.2006.11.015
B. Thorens, GLUT2, glucose sensing and glucose homeostasis. Diabetologia 58, 221–232 (2015). https://doi.org/10.1007/s00125-014-3451-1
A. Rathinam, L. Pari, Myrtenal ameliorates hyperglycemia by enhancing GLUT2 through Akt in the skeletal muscle and liver of diabetic rats. Chem. Biol. Interact. 256, 161–166 (2016). https://doi.org/10.1016/j.cbi.2016.07.009
N. Vedovato, O. Rorsman, K. Hennis, F.M. Ashcroft, P. Proks, Role of the C-terminus of SUR in the differential regulation of beta-cell and cardiac KATP channels by MgADP and metabolism. J. Physiol. 596, 6205–6217 (2018). https://doi.org/10.1113/JP276708
V. Djokic, S. Jankovic-Raznatovic, R. Novakovic, M. Kostic, J. Rajkovic, M. Labudovic-Borovic, J. Rakocevic, J. Stanisic, M. Djuric, L. Gojkovic-Bukarica, Effect of gestational diabetes mellitus and pregnancy-induced hypertension on human umbilical vein smooth muscle KATP channels. Exp. Mol. Pathol. 111, 104323 (2019). https://doi.org/10.1016/j.yexmp.2019.104323
Y. Sha, Y. Zhang, J. Cao, K. Qian, B. Niu, Q. Chen,, Loureirin B promotes insulin secretion through inhibition of KATP channel and influx of intracellular calcium. J. Cell Biochem. 119, 2012–2021 (2018). https://doi.org/10.1002/jcb.26362
Y. Yang, K. Shimomura, K. Sakuma, Y. Maejima, Y. Iwasaki, J. Galvanovskis, K. Dezaki, M. Nakata, T. Yada, Bupropion can close KATP channel and induce insulin secretion. J. Pediatr. Endocrinol. Metab. 26, 343–346 (2013). https://doi.org/10.1515/jpem-2012-0295
C.H. Lee, C.S. Chu, H.J. Tsai, L.Y. Ke, H.C. Lee, J.L. Yeh, C.H. Chen, B.N. Wu, Xanthine-derived KMUP-1 reverses glucotoxicity-activated Kv channels through the cAMP/PKA signaling pathway in rat pancreatic beta cells. Chem. Biol. Interact. 279, 171–176 (2018). https://doi.org/10.1016/j.cbi.2017.11.017
J. Gao, X. Zhong, Y. Ding, T. Bai, H. Wang, H. Wu, Y. Liu, J. Yang, Y. Zhang, Inhibition of voltage-gated potassium channels mediates uncarboxylated osteocalcin-regulated insulin secretion in rat pancreatic beta cells. Eur. J. Pharm. 777, 41–48 (2016). https://doi.org/10.1016/j.ejphar.2016.02.060
Acknowledgements
The authors would like to acknowledge the helpful comments on this paper received from the reviewers.
Funding
This work was supported by Qiqihar Science and Technology Bureau (No. SFGG-201940).
Author contributions
Conceived and designed research: L.H. and H.J.; Administrative support: L.H., H.J., and Z.J.; Provided materials or patients: Z.J., F.Y.L., Z.Y.X., S.X.Z., and Z.C.H.; Collected and assembled data: L.H., F.Y.L., Z.Y.X., Z.C.H., and W.F.; Analyzed and interpreted data: L.H. and H.J.; Drafted manuscript: L.H. and H.J.; Approved final version of manuscript: L.H. and H.J.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Li, H., Zhang, J., Fu, Y. et al. Antidiabetic compounds 8a, 8b, 8k, and 9h enhance insulin secretion: activity and mechanism. Endocrine 71, 365–377 (2021). https://doi.org/10.1007/s12020-020-02537-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-020-02537-5