Abstract
Background
The approaches currently used in osteoarthritis (OA) are mainly short-term solutions with unsatisfactory outcomes. Cell-based therapies are still controversial (in terms of the sources of cells and the results) and require strict culture protocol, quality control, and may have side-effects. A distinct population of stromal cells has an interesting secretome composition that is underrated and commonly ends up as biological waste. Their unique properties could be used to improve the existing techniques due to protective and anti-ageing properties.
Scope of Review
In this review, we seek to outline the advantages of the use of conditioned media (CM) and exosomes, which render them superior to other cell-based methods, and to summarise current information on the composition of CM and their effect on chondrocytes.
Major Conclusions
CM are obtainable from a variety of mesenchymal stromal cell (MSC) sources, such as adipose tissue, bone marrow and umbilical cord, which is significant to their composition. The components present in CMs include proteins, cytokines, growth factors, chemokines, lipids and ncRNA with a variety of functions. In most in vitro and in vivo studies CM from MSCs had a beneficial effect in enhance processes associated with chondrocyte OA pathomechanism.
General Significance
This review summarises the information available in the literature on the function of components most commonly detected in MSC-conditioned media, as well as the effect of CM on OA chondrocytes in in vitro culture. It also highlights the need to standardise protocols for obtaining CM, and to conduct clinical trials to transfer the effects obtained in vitro to human subjects.
Graphical Abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
Hyaline cartilage is a subtype of connective tissue that provides a smooth surface reducing friction and resistance to compressive forces during movement [1,2,3]. Its function is made possible due to a dense extracellular matrix (ECM) [1, 2, 4, 5], consisting of a network of collagen fibres, proteoglycans, and non-collagenous proteins [1, 4, 6]. Cartilage is basically composed of a single cell type –chondrocytes [1, 4], which once the organism has reached skeletal maturity, are unable to divide and maintain the quiescent state [6]. These cells are responsible for synthesising ECM components and proteolytic enzymes, that remodel surrounding tissue [4, 6]. The histological architecture of the cartilage also includes neither blood, lymphatic vessels nor neural tissue, which in general provides an ease of movement. The features of this tissue consequently preclude the regeneration of damaged tissue, which may lead to the development of osteoarthritis [7].
OA is a chronic degenerative disease, the development of which is affected by several factors, such as obesity, genetic predispositions, age and extensive stress on the joints [4, 8, 9]. This damages the dense ECM and affects the secretome of the local microenvironment, disrupting the balance between catabolic and anabolic actions in the metabolism of the chondrocytes. The primary causes of the idiopathic disease are yet to be fully explained, but it is thought to be closely related to the inflammatory process. Unlike any other arthritis, however, it is directly related to a severe inflammatory response with an autoimmune background [10]. The interleukin 1β (IL-1β) and tumour necrosis factor α (TNFα) are the most prominent cytokines involved in the progression of OA and the most commonly used during in vitro modelling [4, 5, 9]. The secretion of these inflammatory mediators leads to the release of even more chemokines and pro-inflammatory cytokines, as well as ECM-degrading enzymes: matrix metalloproteinases (MMPs) and aggrecanases [4, 9].
Among the ways of treating OA, we may distinguish methods consisting mainly in fighting the symptoms of the disease, such as the use of painkillers or joint injections, e.g. with hyaluronic acid (HA), corticosteroids or platelet-rich plasma (PRP) [3, 5, 11,12,13]. In addition to symptomatic treatment, there is also surgical management, which involves: microfracture, the use of cells and tissue engineering (autologous chondrocyte implantation (ACI) or matrix-induced autologous implantation (MACI)), osteochondral autograft transplantation and alloplasty, the most invasive [1, 5, 11, 14]. Comparisons of these methods, together with their pros and cons have been already described in a number of reputable studies [5, 14, 15]. The main drawbacks of these procedures tend to be the formation of fibrocartilage, the lifespan of the implants and the invasiveness of these procedures. New sources of cells and materials for tissue engineering purposes are therefore necessary, as are alternative methods for preventing the development of OA or significantly retarding it [1, 11, 15, 16]. This would offer a better quality of life and delay extensive surgical interventions.
Cell engineering has mainly been applied in ACI and MACI procedures [3,4,5, 13]. Initially, it involves collecting chondrocytes from the patient, cultivating them through cell culture and retransplanting them into the site of the defect [4]. The main advantage of cell-based therapies is that the cellular material needed can be taken from various sources, which is extremely hopeful for patients with degenerative diseases, elderly patients and those with genetic and metabolic dysfunctions [3, 15]. Neither do cell-based methods require complex surgery, reducing invasiveness [1, 15, 17]. Among the MSCs that may be used in therapy a variety may be distinguished, but not exclusively osteoblasts, chondrocytes, adipocytes, astrocytes and cardiomyocytes, and they exhibit anti-inflammatory outcomes. They may therefore make it possible to reconstruct the joint and, through immunomodulation, reduce the locally induced immune response [1, 4, 11, 18]. The availability of autologous material for the treatment minimises the risk of patients rejecting it [1, 4]. The efficiency of cell therapy is to a great extent determined by the donor’s health and age, as well as the properties and viability of the cells collected [15]. One of the risks associated with cellular-based therapies is insufficient integration of the cells at the site of the implantation, which significantly reduces the efficacy of the treatment [19,20,21]. The cost of cell therapy, adequately qualified staff and suitable facility core are other limitations on its everyday clinical use.
These limitations have led to the search for new solutions involving various cell populations in the management of OA. The use of MSCs has emerged as a promising source, but it has failed to eliminate most of the drawbacks. During the 1970s and 1980s it was observed that MSCs owe their effect largely to paracrine activity, which has led to research on CM as a cellular substitute for regenerative purposes [22]. Secreted factors are thought to act even in the absence of cells leading to tissue repair [23]. Up to 80% of the regenerative potential initially attributed to transplanted cells also belongs to paracrine-secreted cellular factors [24].
This review will summarise recent data on the suitability of conditioned media from different cellular sources for cartilage regeneration purposes.
New Promising Treatment Approaches: The Conditioned Medium
The term 'conditioned medium' refers to the liquid phase of a cell culture environment enriched with the secretome of cultivated tissue [22]. Its composition is affected by various factors in the microenvironment of the cell culture, including the inhibition of cell contact, cell aggregation, cell growth and differentiation ability, and physical and chemical parameters [22].
Therapies based on a combination of CM with an appropriate population of cells could be an alternative or might improve existing procedures. Among the advantages that may determine the superiority of CM and the agents they contain over cell-based therapies is immunocompatibility. The exclusion of cells obviates the selection of donors and recipients in therapy [21, 23].
Additionally, cells prepared for the therapy die in culture or during delivery to the site of the defect, whilst, CM contains no live material and therefore entails no such inconvenience [24]. CM is easily manufactured, packaged, frozen and transported [23]. Laboratory sterility is only needed at the stage of CM production, while media application may occur under non-sterile conditions [21, 23]. In addition, CM is produced under controlled laboratory conditions, to enable inspection of the composition [24]. CM may therefore easily be applied to regenerative therapies that require only ambulatory conditions. Time and cost could also be saved in therapies involving CM, as the method requires no waiting for the cells reach maturity and it is possible to obtain the medium several times from cells that have been seeded only once [25].
Like any method, the use of CM in regenerative medicine as a new field carries many unknowns. One such unknown is the lack of common recommendations and standards for bioprocessing and quality control of CM-based therapies, resulting in a wide variation and a composition depending on the method and the time of culture [26]. Possible hypersensitivity reactions related to the components of the base medium administered to the cells to obtain the conditioned medium may also be a risk. The long-term effect of their use is not well known, due to the low number of clinical trials in this area. The detailed list of advantages and disadvantages is summarised in Table 1.
The issues mentioned above could be rendered relatively meaningless against the benefits from their application. Gunawardena et al. emphasise that a conditioned medium could be used effectively in managing a number of conditions, so it is necessary to identify the factors responsible for treating or inhibiting OA. A few aspects must, however, be established: the specific knowledge regarding CM components, dosage and delivery method to gain a favourable outcome [21, 28]. It is crucial to select a suitable source of cells secreting specific paracrine factors.
In vitro studies allow for the examination of individual patients' responses to the administration of the CM, so that the semi-retention period of the medium factors in the body may be partially determined. The efficacy of CM-mediated treatment may also be greatly enhanced by modifying the medium composition with patient-specific factors at the manufacturing level, which will enable the development of safe and efficacious, personalised therapies for many conditions [21].
Conditioned Media: Cell Sources
The elements essential in order to produce the CM are cells, most with stromal cells abilities, since these cells have been proven to secrete a variety of cytokines, growth factors and exosomes, responsible for therapeutic effect and tissue regeneration [29,30,31,32]. The most commonly used source across studies are MSCs, due to their capacity for self-renewal and their multipotent nature [25]. They migrate to the site of the damaged tissue and differentiate into the desired cell types, rendering them essential in tissue repair [33]. Another equally interesting aspect of MSC-mediated tissue repair is the fact that these cells secrete several molecules that activate and mobilise cells at the site of the damage, contributing to the modulation of the inflammatory process, which is also thought to accelerate the healing of tissue [34].
In this review the abbreviation MSC stands for 'mesenchymal stromal cells' and refers to work published by Caplan, who has repeatedly emphasised that the term 'stem cells' is misused for what MSCs represent and maintains that they should be referred to as mesenchymal stromal cells. This may confuse clinicians, researchers and patients [35, 36]. The International Society for Cell and Gene Therapy (ISCT®) has defined the minimum criteria cells must fulfil to qualify as MSCs. Firstly, MSCs must be plastic-adherent in in vitro culture. Secondly, they must be characterised as expressing CD105, CD73 and CD90, but lack expression of CD45, CD34, CD14, CD11b, CD79α, CD19 and human leukocyte antigen-DR surface molecules. Lastly, they must differentiate in vitro into osteoblasts, adipocytes and chondrocytes [37]. Caplan emphasises that mesenchymal stem cells are often used for cell populations that fail to fulfil the above characteristics, leading to a misunderstanding and misinterpretation in studies [36]. This paper therefore employs the term 'stromal cells' for MSCs for a more precise explanation of the topic.
Induced mesenchymal stromal cells (iMSCs) have been extensively used in cartilage regeneration therapies because their properties allow multilineage differentiation. Additionally, the MSC secretome modulates the anti-inflammatory and immunosuppressive properties of the microenvironment and protect cartilage from further damage [38]. The differentiation of MSCs into chondrocytes at the site of injury may also lead to a reduction in prostaglandin concentration in synovial fluid, which could reduce the progression of OA [38]. In general, MSCs also display the ability to inhibit the proliferation and the activation of immune cells (T cells, B-cells, NK cells (natural killer cells), and DC (dendritic cells)) [39].
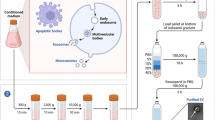
The most common sources of stromal cells are bone marrow-MSCs (BM-MSCs), synovial membrane-MSCs (SM-MSCs), adipose tissue-derived-MSCs (AD-MSCs), placenta-derived-MSCs, amnion-derived-MSCs, umbilical cord-MSCs (UC-MSCs), umbilical cord blood-MSCs (UCB-MSCs), Wharton's jelly-MSCs (WJ-MSCs), dental pulp stromal cells (DPSCs), and also human exfoliated deciduous teeth stromal cells (SHED), shown in Fig. 1.
The commonly used cell sources and obtaining the conditioned medium. CM for cartilage regeneration therapies may be obtained from stromal and stem cell populations such as BM-MSCs, SM-MSCs, AD-MSCs, placenta-derived-MSCs, amnion-derived-MSCs, UC-MSCs, UCB-MSCs, WJ-MSCs, DPSCs, SHED and iPSC (induced pluripotent stem cells). Isolated homogenic populations of cells are expanded in in vitro culture. After a reasonable period of time or when adequate cell confluence is achieved CM might be collected, precleared and stored for the future use. circRNA, circular RNA; CCL2, C–C motif chemokine ligand 2; DKK-1, dickkopf 1; ECM, extracellular matrix; FGF, fibroblast growth factor; HGF, hepatocyte growth factor; HIPK3, homeodomain interacting protein kinase 3; IFN-γ, interferon γ; IL-6 /-10, interleukin 6 /10; LIF, leukemia inhibitory factor; lncKLF3-AS1, KLF Transcription Factor 3 Antisense RNA 1; lncRNA, long-non coding RNA; LYRM4, LYR Motif-Containing Protein 4; miR, micro RNA; MMPs, matrix metalloproteinases; ncRNA, non-coding RNA; PDGF, platelet derived growth factor; PGE2, prostaglandin-E2; SDF-1, stromal cell-derived factor 1; SEA, N-stearoylethanolamide; SERPINE, serine proteinase inhibitor; TGF-β, transforming growth factor β; TIMPs, tissue inhibitor of metalloproteinases; VEGF, vascular endothelial growth factor; VIM, vimentin
The most commonly used and best-characterised stromal cells in regenerative therapies are BM-MSC and AD-MSC. They differ in their origin and their properties, i.e. in the secreted cytokines. The lack of a defined protocol for obtaining CM means there is a great variability among the CMs discussed in the studies [40]. This was emphasised in the study by Alexandrushkina et al., who investigated the secretome of MSC cultured in monolayers and cell sheets (CS). They demonstrated that CS contain more factors that are involved in chemotaxis and the maturation of blood vessels [41]. Zisa et al. also demonstrated that the number of secreted trophic factors depends on the origin of the cells and showed that human BM-MSC secretes less vascular endothelial growth factor (VEGF) than porcine BM-MSCs [42]. The most common sources of CM are AD-MSC [34, 41, 43], BM-MSC [44,45,46], UC-MSC or WJ-MSC [34, 44, 47] and SHED [30, 31, 44]. The effect of the conditioned medium will also vary depending on the type of cells to which the CM is administrated and the time, method and conditions under which the test cells are cultured. Each cell type was found to differ from the others in the terms of the secreted factors: AD-MSCs secreted collagen I, II and III at the highest levels; WJ-MSCs secreted small amounts of ECM components; BM-MSCs secreted higher amounts of heparin sulphate than the other cells [34]. Cells derived from adipose tissue also secrete higher amounts of pro-angiogenic factors, including VEGF, hepatocyte growth factor (HGF), fibroblast growth factor (FBF), platelet-derived growth factor (PDGF) and angiopoietin-1 (Ang-1) and angiopoietin-2 [48]. AD-MSCs, however, secrete the highest amount of matrix metalloproteinases (MMP-1, MMP-3, MMP-13) compared to WJ-MSCs and BM-MSCs [34].
Their origin means that WJ-MSCs have a greater regenerative capacity and exhibit a better proliferative potential, but become problematic when the patients cryopreserve no umbilical cord cells [34]. Wharton's jelly mesenchymal stromal cells are an attractive source of cells for therapy, due not only to their high proliferative capacity, non-controversial nature and ability to differentiate into three germ lineages, but also because of their prolonged stemness trait and non-cancerous character [49].
Researchers also indicate the regenerative potential of DPSCs. Kichenbrand et al. emphasised that DPSCs represent an attractive option for obtaining the MSCs. A dental pulp source provides a large number of cells. Isolation may be performed by enzymatic and mechanical methods from adult or baby teeth during ordinary dental procedures. DPSCs display a higher proliferation and better ability to induce mineralisation than BM-MSCs, making them a promising cell source for OA therapy. These cells can also be combined with scaffolds to achieve even better anti-inflammatory and immunomodulatory effects in regenerative therapies [50]. Nosrat et al. also emphasise that DPSCs produce neurotrophic factors in culture, promoting neuron survival. Their neuroregenerative properties were also demonstrated when transplanted into the spinal cord [51]. This transplantation led to an increased number of rescued motoneurons, indicating the significant role for factors secreted by DPSCs in cell proliferation [51]. In contrast, Wang et al. demonstrated that SHEDs, also derived from dental pulp, exhibit a higher proliferation rate, better differentiation and mineralisation capacity after transplantation than DPSCs [52]. Compared to DPSCs, SHEDs are characterised by a higher expression of MMP-1 and MMP-2, which may discourage the use of these cells in the treatment of articular cartilage. Factors showing elevated expression in SHED cells also include tissue inhibitor of metalloproteinases 1 (TIMP-1), tissue inhibitor of metalloproteinases 2 (TIMP-2) and interleukin 6 (IL-6), which promote the regeneration of cartilage tissue [52].
iPSCs are another promising source for regenerative therapies. Due to their foetal-like tissue nature, it is suspected that they may act more efficaciously in regenerative therapies than MSCs. iPS cells are derived from adult somatic cells and then genetically reprogrammed into embryonic stem-like (ES-like) cells. Because they are obtained as in a laboratory rather than isolated from the blastocyst’s inner mass they entail no ethical issues [53, 54]. Due to the ability of iPS cells to differentiate into cartilage tissue cells, they may be used in cell-based OA therapies such as ACI and MACI procedures [55,56,57]. iPS cells may also be used to design disease models, e.g. for OA, in order to study pathological processes during the disease more precisely [56]. Using these cells in therapies may, however, carry the risk of teratoma formation [55]. Tissues generated from iPS cells will be nearly identical to donor cells, making them almost ideal for regenerative medicine [53] if only precise and effective protocols are developed for differentiating iPSCs into chondrocytes.
The CM above iPS cells is yet to be explored for use in the context of OA, but it has been shown to enhance proliferation, migration and maintenance of morphology in bovine corneal endothelial cells (B-CECs) [58]. The action of iPSC-CM on endothelial cells is thought to involve phosphorylation of the Akt signalling pathway and regulation of the PI3-kinase pathway, as well as leading to an increase in the expression of activin-A [58]. In another study Hsieh et al. demonstrated that iPSC-CM protects against tumour-induced immunosuppression by increasing the activity of host NK cells [59]. Su et al. found that CM of iPSCs reduced neutrophil recruitment associated with the pathogenesis of acute lung injury by inhibiting their endothelial migration and promoting endogenous leukaemia inhibitory factor (LIF), as well as reducing the endothelial leakage of immune cells [60]. Researchers also highlight that the medium reduces NF-κB activity and neutrophil chemotaxis [60]. Zhou et al. demonstrated that the application of iPSC-CM leads to improved lung structure in mice with pulmonary fibrosis and promotes the repair of damaged tissue by inhibiting the Transforming growth factor β1/Suppressor of Mothers Against Decapentaplegic (TGF-B1/Smad) signalling pathway [61]. This confirms the protective effect of CM on lung tissue and its involvement in the prevention of pulmonary fibrosis. The above-mentioned studies demonstrate the enormous potential of iPSC-CM in the treatment of many diseases, especially in the context of regenerative medicine.
Composition of Conditioned Media
The idea of testing the composition of CM emerged from the unexplained association between efficacious MSC engraftment and improved functionality at the site of implantation [35, 62]. Observations suggested that the process might involve the paracrine properties of these cells [21, 23, 48]. The increasing interest in the secretome of MSCs has allowed the initial identification of several elements with which CM is enriched: proteins, lipids, nucleic acids and extracellular vesicles [40, 63]. Researchers have further distinguished a group of molecules that includes cytokines, chemokines, receptors, growth factors and inflammatory factors [64, 65]. The function of major CM components in chondrocyte biology is shown in Table 2. It is important to highlight that the compositions of presented CM are depend largely on the type of cells from which they are derived, the method and conditions of cell culture, the media used and the methods of purification.
As was mentioned above, several factors have been identified in the composition of CM derived from distinct populations of cells, one being a group of extracellular matrix metalloproteinases, MMP-2, MMP-9, MMP-13 and MMP-19. These proteins belong to the family of zinc-containing proteolytic enzymes and their role is to remodel the ECM of surrounding tissues [66, 123].
MMP-2, also known as gelatinase A, catalyses the breakdown of elements that form the extracellular matrix and promotes cell attachment, proliferation, differentiation processes and programmed cell death [67]. MMP-2 also regulates the activity of one of the most important growth factors, TGF-β, whose disrupted signalling pathways cause the destruction of cartilage tissue and the development of osteoarthritis [68]. Researchers emphasise, however, that the presence of MMP-2 is essential because they drive tissue remodelling with their ability to recruit cells, including osteoblasts, and are involved in inflammatory processes [66, 69]. MMP-9 brings similar properties. Its expression in cartilage is increased in patients with OA [124]. MMP-9 is mainly responsible for recruiting osteoclasts into the hypertrophic zones of the cartilage plate, thus allowing bone formation [68].
In contrast, MMP-13 is a collagenase that cleaves collagen types I, II and III. It digests both cellular matrix and non-cellular components [72]. Its properties, mean that it is involved in cartilage breakdown in OA [83]. Another component, MMP-19, is involved in the degradation of the cartilage cell matrix, aggrecan, Cartilage Oligomeric Matrix (COMP) proteins, types I and IV collagen, laminin, fibronectin and nidogen, a glycoprotein that is part of basic membranes [73, 74].
Among other components of CM are inhibitors of the metalloproteinases mentioned above, TIMP-1 and TIMP-2. These proteins are characterised by anti-fibrotic activity and may prevent cartilage degradation [43, 76]. TIMP proteins have also been attributed to the suppression of pain, which is explained by the reduction of mechanical and thermal hypersensitivity after nerve injury through inhibition of the activity of MMPs [77, 78].
Researchers highlight another component, vimentin (VIM) in the CM may play a role in the chondrogenic differentiation of adult mesenchymal chondro-progenitor cells (MPCs). It is also required adequately to express cartilage genes and regulate the synthesis of ECM’s in chondrocytes and MPCs undergoing chondrogenesis [79, 80]. Bobick et al. demonstrated that inhibition of vimentin expression resulted in a reduction of the expression of the cartilage markers aggrecan, type II collagen, SRY-Box Transcription Factor 5 (SOX5), SRY-Box Transcription Factor 6 (SOX6) and SRY-Box Transcription Factor 9 (SOX9) [79]. A similar relationship was demonstrated by Blain et al. suggesting that the intermediate filament network of vimentin contributes to the maintenance of the chondrocyte phenotype and that its disruption may lead to the development of OA [80].
Serine proteinase inhibitor (SERPINE) family proteins, such as vimentin, maintain the structure of cartilage, but at the tissue level, perform a more precise function in preventing cartilage breakdown. SERPINE1 is involved in the remodelling of tissue and the formation of fibre, due to its ability to inhibit plasmin and cellular matrix metalloproteinases [82]. SERPINE2 inhibits the expression of MMP-13 and reduces cartilage breakdown caused by metalloproteinase [83].
Among the most commonly mentioned growth factors are TGF-β, VEGF, HGF, FGF, and PDGF. Growth factors of the TGF-β family play a key role in every aspect of the tissue development, including chondrogenesis. They control the proliferation, differentiation, and maintenance of the chondrocytes that form cartilage. They also act as inhibitors of the hypertrophic process and reduce oxidative stress [84, 85].
Another component widely described in CM composition is VEGF, a protein responsible for the proliferation and migration of endothelial progenitor cells and angiogenesis. It plays a crucial role in the late stages of chondrogenesis, enabling infiltration and the formation of blood vessels [92,93,94]. Increased VEGF levels correlate with the progression of OA, specifically with Kellgren and Lawrence (K&L) classification [115]. VEGF signalling has been reported to be involved in OA pain as a growth factor-mediated angiogenesis induction. It increases the inflammatory process and the sensitivity of pain receptors [95].
The other growth factor, HGF, has a significant impact on overall cell survival and proliferation, cellular matrix metabolism, induction and enhancement of the expression of MMPs, and the enhancement of Th2-mediated immune responses [97, 125, 126]. In the context of the osteochondral system, it plays a significant role in osteochondral turnover, bone remodelling and the regeneration of osteoarticular tissue [97, 127].
FGF acts as a mechano-transducer by binding to heparan sulphate proteoglycan chains in the ECM [102]. It is reported that it may also be released in higher concentrations in response to damage to cells [128]. Increased FGF release leads to activation of the extracellular-signal-regulated kinase (ERK) signalling pathway in cartilage [103]. Researchers highlight the chondroprotective properties of FGF due to the factor's ability to inhibit A Disintegrin and Metalloproteinase with Thrombospondin motifs-5 (ADAMTS-5) -mediated aggrecan degradation [102]. It is also thought that FGF induces the synthesis of TIMP-1, MMP-1 and MMP-3, influencing cartilage protection and inhibiting the degradation of its components [103]. FGF also regulates neurogenesis and protects neurons from degeneration after injury, which implies functions in tissue remodelling and repair processes that may be observed against in tissues, such as cartilage [128].
PDGF is a growth factor known for its beneficial properties in healing wounds by affecting chemotaxis, angiogenesis and cell mitosis [104]. It has also been established that PDGF inhibits inflammatory processes and apoptosis in in vitro models by reducing the expression of apoptotic proteins protein 38 (p38), BCL2 Associated X (Bax) and caspase-3 with a parallel increase in the expression of the protein responsible for cell survival, ERK [105]. In chondrogenesis it increases the level of type II collagen that builds cartilage, reduces the level of collagen X in hypertrophic chondrocytes and alleviates cartilage hyperplasia [105].
Other CM components include chemokine, C–C Motif Chemokine Ligand 2 (CCL2) and cytokine, LIF. CCL2 plays the role of chemoattractant for monocytes, macrophages and activated T lymphocytes involved in the inflammatory response [89]. In patients with OA, CCL2 levels are significantly increased in the blood and synovial fluid, suggesting a correlation with the pathogenesis of the disease [129]. The use of this factor as a marker for the diagnosis and treatment of OA is highlighted in some studies [89].
LIF is present in the fluid of patients with arthritis, both rheumatoid arthritis and osteoarthritis [98]. It is involved in the resorption of proteoglycans in cartilage, inflammatory, and catabolic processes. It is thought to be a mediator in the pathogenesis of arthritis [98,99,100]. The pleiotropic actions of LIF include the ability to regulate cell differentiation, acute phase protein synthesis, stimulation of calcium ion release in bone, proteoglycan resorption and immune response, but are by no means limited to these [101].
Another factor, whose elevated levels may be observed in patients with OA and rheumatoid arthritis (RA), and which is present in CM, is interferon γ (IFN-γ)[81, 130]. It is also known as type II interferon and is produced by T lymphocytes and NK cells. It tends to be responsible for communicating immune cells and activating the body's defence mechanisms. In the context of OA, it contributes to the M1 polarisation of macrophages, which produces reactive oxygen species (ROS) and pro-inflammatory cytokines. These processes are associated with the progression of osteoarthritis [106]. T cells producing the above cytokine also induce osteoclastogenesis by expressing Receptor Activator for Nuclear Factor κβ Ligand (RANKL), leading to bone resorption [107].
Like LIF, the dualistic nature, pro-inflammatory and anti-inflammatory, is demonstrated by IL-6. The pro-inflammatory functions of interleukin are associated with the induction of intercellular adhesion molecule-1 (ICAM-1) expression, downregulation of type II collagen expression and the maintenance of acute inflammation or conversion to a chronic form [98, 111]. IL-6 is also associated with the immune response, as it induces differentiation of B lymphocytes, making these cells capable of producing antibodies [112]. It is also an important factor in homeostasis in bone insofar as it increases the expression of RANKL, which induces osteoclast differentiation and leads to excessive bone resorption [113]. IL-6 influences RA development by participating in vascular inflammation pathogenesis. It is associated with excessive angiogenesis and vascular permeability caused by increased VEGF expression [114]. Researchers suspect that IL-6 may modulate the balance between MMPs and TIMPs. Disruption of this balance leads to the degradation of articular cartilage and the development of osteoarthritis [98].
Interleukin 10 (IL-10), like IL-6, is elevated in patients with OA. It tends to perform anti-inflammatory functions by inhibiting proinflammatory factors such as IL-1β, TNF and MMPs. It also upregulates interleukin-1 receptor antagonist (IL-1Ra) and TIMP [111, 115]. IL-10 exhibits chondroprotective activity by reducing the apoptosis of cartilage tissue cells and counteracting pro-inflammatory IL-1 [115, 116].
Stromal cell-derived factor 1 (SDF-1) or C-X-C motif chemokine 12 (CXCL12) belongs to the group of pro-inflammatory chemokines. It is present in the synovial membranes and synovial fluid of OA patients and also in subchondral bone [117, 131]. It tends to be produced by BM-MSCs and osteoblasts, whereas chondrocytes in healthy tissue do not express this factor [131]. SDF-1 binds to its ligand, C-X-C chemokine receptor type 4 (CXCR4), which conjugates to a G-protein on the surface of chondrocytes, allowing the activation of multiple signalling pathways [117, 131] responsible for apoptosis and release of MMP, increased expression of IL-1, TNFα [118, 119]. It has been credited with a role in the degradation of cartilage and the enhancing of the inflammatory process in OA by reducing the expression of type II collagen and aggrecan [117,118,119,120]. SDF-1 intraarticular injection has been shown to induce the OA model in the knee in rabbits more efficiently than traditional surgical methods [119]. It has been stressed that treatment targeting the SDF1/CXCR4 signalling pathway may be a promising therapeutic method for the treatment of arthritis [118].
The ingredient responsible for the ageing of chondrocytes by the upregulation of MMPs and inflammatory factors such as SDF-1 and VEGF is Dickkopf 1 (DKK-1) [108, 109]. It is a growth factor and antagonist of the canonical Wnt/β-catenin signalling pathway. DKK-1 is thought largely to regulate bone remodelling in arthritis [108, 110]. The Wnt/β-catenin signalling pathway plays a role in bone resorption, and joint degradation in the pathogenesis of RA [108, 109]. The expression of DKK-1 is increased in RA patients in synovial fluids and synovial fibroblasts [108].
Among the components of the CM were detected a number of lipids, which are involved in the development of inflammatory processes, prostaglandin-E2 (PGE2) and N-stearoylethanolamide (SEA). PGE2 may play both pro-inflammatory and anti-inflammatory roles, depending on its concentration [64]. It induces macrophages to produce the anti-inflammatory IL-10, reduces apoptosis in hepatocytes and reduces the expression of plasminogen activator inhibitor (SERPINE1/PAI)-1 mRNA [86]. PGE2 is present in articular cartilage with inflammatory arthropathy [82], downregulates aggrecan expression and regulates plasmin activator secretion and proteinase expression, which may lead to extracellular matrix degradation [82]. SEA, in contrast, is a lipid of endogenous origin, of the N-acylethanolamides family, which has anti-inflammatory and immunomodulatory properties [64]. It is thought to be involved in downregulating the expression of many pro-inflammatory factors, but its exact role in OA is not fully understood [64, 122]. The effect of the listed factors on articular cartilage is summarised in Fig. 2.
CM components and their effect on articular cartilage biology. Distinct factors included in conditioned media as free molecules or delivered by extracellular vesicles can affect several biological processes, such as the interplay between regeneration/degradation of ECM, proliferation, migration of chondrocytes, and modulation of local inflammation response
Effect of Conditioned Media from Mesenchymal Stromal Cells on OA Chondrocytes
MSCs are the most popular source of cells for use in regenerative medicine, due to their availability and wide clinical application in different fields of medicine. Several clinical trials regarding their use are taking place [132]. As mentioned above, their unique paracrine parameters provide the beneficial effect of stromal cells in tissue regeneration processes [64, 65]. Stromal cells produce exosomes and growth factors that may hinder degradation processes and induce tissue regeneration [133]. The MSC secretome, CM containing factors, exosomes and microvesicles, also reduces inflammation and boosts regeneration processes, rendering it a promising option for OA therapy [134]. A significant advantage of using CM over cells to treat OA is that treatment with CM requires no surgery, but a simple ambulatory procedure [87]. This advantage entails quicker recovery time for the patient and also entails with financial benefits. For CM to be applied to OA therapy, however, standardisation of protocols for obtaining and harvesting the culture medium is needed, as well as a precise definition of its composition [29]. Table 3 summarises recent advances in the field of the application of CM in OA management with its various detailed composition of CM and potential active agents.
In their study Manferdini et al., compared the effects of CM and the coculture system on chondrocytes. Adipose stromal cells (ASCs) taken from healthy patients who undergo liposuction of subcutaneous abdominal fat were used to obtain CM and coculture. CM was harvested from cells (seeded at 1 × 105 per well) on the 2nd and 7th day after administration of complete serum-free Dulbecco's Modified Eagle Medium (DMEM) to cells in culture and then pooled. Chondrocytes and synoviocytes were collected from OA patients showing K&L 3 or 4. Cells were then cocultured with ASC and treated with a CM for 7 days. The study failed to show that culture with CM led to a reduction in expression levels of IL-6, monocyte chemotactic protein 1 (MCP-1), macrophage inflammatory protein-1 α (MIP1-α) and regulated upon activation, normal T cell expressed and presumably secreted (RANTES) in the cells examined compared to the coculture system. The culture with CM also failed to reduce interleukin 8 (IL-8) and growth-regulated α protein (GROα) levels in synoviocytes, but partially reduced chondrocytes. The use of CM showed a less effective reduction in MMP-13, ADAMTS4 and ADAMTS5; an increase in TIMP-1 and TIMP-3, rather than the coculture of cells with ASC. The CM contains too low a concentration of PGE2 to reduce inflammatory processes in chondrocytes and synoviocytes. It was therefore concluded that ASC-CM displays a limited ability to reduce inflammation and down-regulate proteases that contribute to ECM degradation [135].
Mendia et al. compared the effects of CM and HA on the coculture of chondrocytes with synoviocytes. CM was obtained from human AD-MSCs taken from total or partial hip arthroplasty patients and stimulated with IL-1β for 24 h. Stimulation with IL-1β triggered ECM degradation and activation of mediators and effectors of progressive cartilage loss. AD-MSCs were seeded 2 × 106 in Dulbecco's Modified Eagle Medium/Nutrient Mixture F-12 (DMEM/F12), and the medium was harvested when cells reached between 80 and 90% confluence. The results were compared for the coculture of IL-1β-induced cells cultured in DMEM/F12 with HA or CM. CM was found to lead to a reduction in glycosaminoglycans (GAGs) levels, and HA. A reduction in nitric oxide (NO) production was also only confirmed in the sample with the addition of CM. Culture with CM also reduces the expression of IL-1β, MMP-13 and ADAMTS5 in cartilage and the expression of MMP-13 and ADAMTS5 in the synovium. In contrast, HA only reduces MMP-13 and ADAMTS5 levels in cartilage and ADAMTS5 in the synovium. CM, like HA, leads to the upregulation of the expression of TIMP-1 in both cartilage and synovium. This demonstrates that both HA and AD-MSC-CM show beneficial effects in OA therapy, but the impact of CM is more prominent [136].
As in the studies described above, Niada et al. used stromal cells derived from adipose tissue. ASCs were collected from healthy patients undergoing aesthetic or prosthetic surgery. The medium was obtained from cultured cells after the 4th passage showing between 80 and 90% confluence after being cultured in serum-free DMEM for 72 h in starving conditions. Cartilage tissue cells were collected from patients undergoing total hip replacement from femoral heads. Chondrocytes in culture were initially stimulated with TNFα to induce hypertrophy; then with or without ASC-CM in a 1:5 ratio with DMEM supplemented with 1% fetal bovine serum (FBS) for 24 h, 48 h or 72 h. The results highlighted that CM blunted TNFα-induced hypertrophy and reduced osteocalcin, collagen type X (COL10), MMP-3 and MMP-13 activity. ASC-CM also contained chondroprotective factors such as osteoprotegerin (OPG), and DKK-1. The study established that CM exhibits anti-hypertrophic and anti-catabolic effects [137].
Platas et al., a group of researchers who also used stromal cells derived from adipose tissue, used cells obtained during abdominoplasty. The cells were cultured before or after the 1st passage to achieve semi-confluence. During culture, the medium used was DMEM/F12 supplemented with antibiotics and 15% human serum, derived from donors with AB blood group. 48 h after the beginning of the culture, the medium was collected from above the cells and pooled. Chondrocytes were obtained from the knee cartilage of patients with advanced osteoarthritis. OA-specific inflammation was induced in the cells with IL-1β and then cultured for between 1 and 7 days in complete DMEM/F12 with or without CM. 1 ml ASC-CM for 6-well plates or 2 ml for 3.5 cm plates was added. CM reduced markers of IL-1β-induced senescence-like accumulation of yH2A.X foci and the formation of actin stress fibres. CM also reduced the production of oxidative stress, reduced the activation of myogen-activated protein kinases, downregulated the expression of caveolin-1 and protein 21 (p21), and also reduced protein 53 (p53) acetylation. These results concluded that ASC-CM shows a protective effect in degenerative joint conditions and could be used as a potential therapy for OA [138].
Adipose tissue cells and those from the umbilical cord have been used to obtain CM for OA therapy. In their study Famian et al. isolated WJ-MSCs from the umbilical cord of women who had undergone a caesarean section. MSCs were cultured in serum-free DMEM until the 4th passage, and then the medium was harvested when the cells reached 70% confluence. The effect of CM was tested on chondrocytes collected from patients undergoing joint replacement for femoral neck fractures. Chondrocytes were cultured until the 3rd passage and then seeded at 1 × 106 in both monolayer and mass culture. The cells were then cultured in DMEM medium with FBS alone or with the addition of WJ-MSC-CM for between 3 and 6 days, and analyses were performed. It was demonstrated that the expression of the cartilage genes collagen type II α 1 chain (COL2A1), aggrecan (ACAN), COMP and SOX9 was significantly upregulated after the 3rd and the 6th day of culture in both monolayer and mass cultured cells. After 6 days of culture with CM, however, a decrease in the expression of the above-mentioned genes was observed in monolayer cultured cells, while cells in mass culture continued to show high gene expression. The results presented by Famian et al. indicate that WJ-MSC-CM has a beneficial effect on cartilage gene expression in chondrocytes cultured in both monolayer and mass cultures. The long-lasting effect is, however, only seen in cells cultured in the mass culture system [49].
The research group of Kusuma et al. also used WJ-MSC to obtain a CM. The stromal cells, isolated for previous studies [141], were seeded at 3 × 105 cells per well in a complete medium. Some MSCs were induced with insulin-like growth factor 1 (IGF-1) (150 ng/ml) for 7 days and CM was then harvested. The stromal cells were induced to secrete more factors to stabilise the chondrocyte phenotype and lead to more efficient ECM production. The cartilage tissue cells also came from a commercial source and were CHON002 chondrocytes (ATCC CRL-2847). Chondrocytes were seeded with 5 × 105 cells per T-25 flask and cultured in the presence of CM (15% or 30%) for 48 h. After a time, the CM was removed and cells were treated with IL-1β for 5 days to induce an OA-specific phenotype. The researchers highlighted that the most significant increase in the expression of type II collagen was observed in the trial in which WJ-MSCs were initially induced with IGF-1 and CM was applied at a concentration of 15%. The study demonstrated a beneficial effect of WJ-MSC-CM on the reduction of anti-inflammatory cytokines, such as TNFα and IL-10, as well as the reduction in the expression of MMP-3 in OA chondrocytes [47].
The same research group published a similar study a year later, in which CM was derived from human SM-MSCs. Stromal cells were collected from patients with OA with K&L 4 during knee joint biopsies. They were then seeded at 5 × 105 per flask in a complete medium, and CMs were harvested when the cells reached 80% confluence. MSCs were also induced with IGF-1 for 7 days. In the initial stages of the study, cell induction was shown to be most effective using IGF-1 at a concentration of 150 ng/ml, which was used in the following stages of the study. As in the study by Kusuma et al., the effect of CM was tested on cell line CHON002 [47]. Chondrocytes were seeded 1 × 106 cells per flask in complete DMEM supplemented with 15% or 30% SM-MSC-CM and, after removal of the medium, cells were induced with IL-1β. It has been shown that preconditioning SM-MSCs with IGF-1 leads to a more significant decrease in hypertrophy markers and an increase in those factors that are thought to prevent chondrocyte hypertrophy. The IGF-1-SM-MSC-CM increases the expression of SOX9 and COL2 with a parallel reduction in the expression of COL10, MMP-13 and ADAMTS4, hypertrophic markers. Previous studies suggest a more beneficial effect of medium-conditioned neural stromal cells in chondrocyte cultures than those exhibiting an OA-specific phenotype [139].
Muhammad et al. detail another source from which MSCs were obtained for CM. The researchers isolated human SHED cells from deciduous molars and seeded them at 5 × 103 per cm2 and cultured them in serum-free DMEM until 70% confluence was achieved. When the appropriate confluence was reached, the medium in the cells was changed and CM was harvested after 48 h or 72 h. The effect of the CM was studied on chondrocytes collected from OA patients undergoing total knee arthroplasty. Chondrocytes (1 × 104 cells/cm2) were initially stimulated with IL-1β and then treated with SHED-CM. The CM was shown to increase the concentration of anti-inflammatory factors and stimulate the expression of hyaline cartilage markers, COL2 and ACAN, as well as leading to a reduction in the expression of MMP-13 and nuclear factor κB (NF-κB), a mediator of pro-inflammatory and catabolic factors. This suggests a beneficial effect of CM on OA chondrocytes and potential in regenerating ECM proteins and mitigating inflammation induced by the upregulation of the expression of NF-κB and MMP-13 [31].
BM-MSCs are also a potential source of CM. They were used by Chen et al. in their study. The research was designed to evaluate the effects of BM-MSC-CM on the rat model of OA induced by the anterior cruciate ligament transaction and destabilisation of the meniscus. Human BM-MSCs obtained from ScienCell Research Laboratories were cultured until the 3rd passage. Once cells reached 70% confluence, the culture medium was changed to serum-free medium w/o antibiotics and pooled after 48 h. CM was administered to rats in the form of intraarticular injection. The analyses carried out confirmed the overall alleviating effect of symptoms and inconvenience associated with the development of OA after the application of CM. A morphologically well-preserved subchondral bone structure was confirmed in those animals receiving CM, along with more abundant cartilage matrix. The use of a CM also inhibited rats’ chondrocytes apoptosis. The immunohistochemical staining showed a reduced ratio of MMP-13 to TIMP-1, confirming the beneficial effects of MSC-CM in OA management [140].
Despite the different sources of MSCs, most studies and protocols presented support the thesis that the beneficial effects on cartilage tissue cells in in vitro culture may be achieved with stromal cell-conditioned media. These beneficial effects may include the inhibition of hypertrophy, oxidative stress, ageing, the degradation of ECM, the upregulation of chondrogenic-related genes and the secretion of chondroprotective factors. Due to its properties, MSC-CM shows potential for application in OA therapy. To do this, however, it is necessary to develop appropriate protocols for obtaining CM based on a serum-free system, so that an excessive immune response in the patient is avoided.
Exosomes are an Essential Component of the Conditioned Medium
Besides freely excreted molecules, highly organised membranous structures, commonly called extracellular vesicles (EVs), could be found among the stem cell secretome [142, 143]. We can distinguish among them (depending on the origin and size) microvesicles/ectosomes (surface of the cell; 100 – 1000 nm), apoptotic bodies (cells undergoing apoptosis; 50 – 5000 nm) and exosomes (internal compartments of the cells; 30–150 nm) [144]. A vast majority of the literature is focused on the properties and functionality of the exosomes – the endosomal-origin bilipid layer structures with cup-like shape morphology [145]. They already have gained an undoubtful place in cancer biology, acting as a potential source of biomarkers in early detection and prognostic purposes [146,147,148]. Cancer cells use them to manipulate the immune system and local/distal tissue environment to form a metastatic niche [149, 150]. They have strong immunomodulatory properties, are responsible for immune tolerance and are crucial players in intracellular communication in local and distal areas of the organism [151]. They have a unique composition of lipids, proteins and nucleic acids (the main source of miRNA, lncRNA), which could be modified in response to physical or chemical stimulation, acting as an indicator of environment changes [152, 153].
Exosomes have gained considerable interest in their applications as a drug delivery platform since their structure enable the protection of molecular cargo [143, 154]. Additionally, modification of their composition through overexpression of particular molecules (especially miRNA packaging) could lead to the formation of tools for targeted therapy [143, 155]. They are unable to proliferate, exhibit properties of parental cells, and are highly tolerable by the recipient, could cross the blood–brain barrier, which makes them almost a universal solution for regenerative medicine purposes [156,157,158]. Since exosomes are dependent on the physiological state of the parental cell, the standardisation of their isolation protocol is still needed to be established, as well as cell source, culture system, the medium supplementation with appropriate growth factors/chemical compounds, and knowledge about their exact molecular profile [159,160,161,162]. One of the critical roles in their harvesting is formulation of the medium, which should be serum- and xeno-free, due to the vast amounts of EVs from animal origin. Consequently, their cargo profile could also change [163]. Besides these facts, their unique protective and immunomodulatory properties has found potent usefulness in a few fields of regenerative medicine, such as attenuation of the effect of myocardial infarction [164], kidney ischemia [165], brain ischemic stroke [166], improved regeneration with limited scarring during wound healing [167], increases angiogenesis [168], reduction of lung fibrosis caused by the biological or chemical factor [60, 169], diminishing the damages of nucleus pulposus or temporomandibular joints [170,171,172,173]. Several studies have also implied that exosomal cargo is a crucial player in the modulation of the chondrogenesis of MSC, depending on the source of EVs [174, 175].
In this part of the review, we would like to focus on their potent application in managing damaged large joints affected by OA. In recent years, many studies regarding using exosomes isolated from distinct MSC sources in the management of musculoskeletal diseases have been published [176]. They were likely ideal candidates as a delivery platform for the several non-coding RNA with therapeutic potentiation [177]. It was shown that they were able to modify the local environment through the attenuation of inflammation by internalising their cargo into macrophages (causing their polarisation into M2 type) and synoviocytes (limiting their inflammatory-related secretome) [178,179,180]. Most importantly, EVs derived from MSC could diminish and reduce the impact of the OA induced chemically (IL-β, TNF-α or collagenase type II) or via mechanical damages on chondrocytes biology [179, 181,182,183,184]. It was assessed by maintaining significantly high expression of markers related to hyaline cartilage (i.e. COL2A1, SOX9, ACAN) with simultaneous downregulation of markers responsible for chondrocytes maturation/hypertrophy and ECM degradation (i.e. MMP13, ADAMTS, RUNX2) [45, 185, 186]. Exosomes also positively impacted the migration, proliferation, and survival of chondrocytes, which caused the slower degradation of ECM, reduced tissue depletion and slower disease progression of OA-affected joints in in vivo models [185, 187,188,189]. These processes were partially regulated via the NF-κB signalling pathway, a crucial one in the inflammatory response in OA, and the WNT/β-catenin signalling pathway, which is responsible for chondrogenic differentiation and chondrocytes catabolic/anabolic homeostasis [154, 162, 177, 186, 190]. Interestingly, among these studies, there was no mention of the negative impact or side effects, which could decline their usage in future clinical trials. However, there was no common mechanism which could provide a universal solution. Studies presented below gave information about the partial protective properties of EVs derived from MSC, but none of them was able to provide full-thickness recovery. As suggested, their usage should be limited to the early stages of OA. The outcomes of the latest studies regarding their use in the management of OA are summarised in Table 4 and molecules involved in OA biology are presented in Fig. 2.
Clinical Trials Using Conditioned Medium
The benefits obtained from using CM in the manipulation of chondrocyte biology and the increasingly well-understood properties of the secretome of MSC-CM may open a new approach to the management of OA [87]. In addition to the current studies, the effects of the CM on the exact large-scale manufacturing process and its composition are needed [29, 134]. Further steps include in vivo studies confirming observed effect CM’s on chondrocytes in in vitro experiments are also necessary [140]. As mentioned above, Chen et al. conducted an in vivo study, but they emphasise that before CM could be used clinically, research on larger animals, animals more alike to humans in size and whose joint movements are more similar to those of humans, is necessary [140]. The final steps that would allow CM to be used in OA therapy are clinical trials, which are underdeveloped and conducted in small numbers.
To date, clinical usage of CM is uncommon. The recently registered trials in the ClinicalTrials.gov database (search performed using the following parameters (Condition or disease: Osteoarthritis; Other terms: conditioned medium OR exosomes OR extracellular vesicles) show eight studies (Table 5) [208]. We have included only six studies in the table because the trials number NCT05546541 and NTC03448796 were only related to the biological profiling of EVs cargo but not their usage as a treatment platform. The newest study NCT05579665 will compare the efficacy of PRP, UC-MSCs-CM and HA in knee osteoarthritis patients. At the time of searching, the trial is active, but yet to recruit. The trial numbered NCT04314661 involved injecting the knee joint using UC-MSC cells or a CM derived from them. On the search date (28 January 2023) the status of the study was ‘recruiting’. The following research, NCT04223622, was designed to investigate the effect of a CM derived from ASCs on human osteochondral explants. The other goal of this study was to compare the effect of CM and extracellular vesicles, and what should support their usefulness as a cell-free therapeutic agent. However, there is a lack of results for this trial due to the ongoing recruitment of the participants. Another exciting study (NCT05060107) is related to the influence of EVs on OA cartilage biology. Researchers are focused on estimating the safety of a single intraarticular injection of EVs derived from MSC in symptomatic mild/moderate knee OA. Due to the lack of ongoing recruitment of the participants, the conclusions are unknown. The study (NCT04225481) involves obtaining an intra-articular stromal vascular fraction (SVF) injection from adipose tissue and then extracting CM from the resulting fraction. The effect of CM will be tested on chondrocytes from patients with OA. Study NCT04223622 is recruiting, while study NCT04225481 has unknown status as the date of analysis. The last searched study (NCT03800810) also has an unknown status. The study was designed to compare the efficacy of UC-MSC implantation, HA therapy and treatment with recombinant human somatropin, which does not directly address the use of a CM. The fewness of clinical trials, undefined protocols and the incomplete understanding of the composition of the CM and its effects argue in favour of developing research towards the understanding and application of CM in the treatment of OA.
Conclusion
Due to the limitations and invasiveness of traditional methods of OA management, tissue engineering techniques have developed significantly. These methods entail drawbacks, however, associated with the use of cells, such as stromal cells. The beneficial effects exerted by MSCs have been attributed to their paracrine abilities, thanks to the development of stromal cell research. It gave rise to CM, which were previously treated as cell culture biowaste.
The usage of CM in the management of OA has its pros and cons, the advantages, however, outweighing the disadvantages. CM may be obtained from a various stromal cells and iPS cells, but the secretome of the latter is yet to be sufficiently explored. A CM includes proteins, cytokines, growth factors, chemokines and lipids, with both anti-inflammatory and pro-inflammatory effects related to chondrocyte catabolic and anabolic processes.
Since there are several factors included in the CM such as proteins and ncRNA, which have multiple targets in the joint environment, establishing one exact mechanism responsible for the action of secretome derived from MSC is impossible. From the one side, it looks like a continuous interplay between the pro-inflammatory anti-inflammatory factors allows remodelling to occur and ultimately improves cartilage's structure and biomechanical properties. On the other hand, the modification of developing local inflammation is partially the key to the deceleration of OA progression by attenuating activated macrophages and synoviocytes secreting the massive amount of metabolites, harmful for articular cartilage ECM and chondrocytes. As mentioned above the combination of a few protein/ncRNAs inhibit enhanced expression of proteins related to the NF-κB signalling pathway, a master of several inflammation-related processes, and mild modification of the WNT/β-catenin signalling pathway, a key modulator of chondrogenic homeostasis, would provide a potential therapeutic approach in deceleration of OA-related.
The results of most of presented studies on the effects of stromal cell secretome on OA chondrocytes confirmed the beneficial effects of CM, alleviating processes associated with the pathomechanism of the disease.
Further studies leading to standardised protocols for obtaining CMs and EVs, as well as clinical trials to relate the results obtained in in vitro studies to the human body, are needed, however, before CM from MSCs and iPSCs may find application in the treatment of OA.
Data Availability
Not applicable.
Abbreviations
- ACAN:
-
Aggrecan
- ACI:
-
Autologous chondrocyte implantation
- ADAMTS:
-
A Disintegrin and Metalloproteinase with Thrombospondin motifs
- AD-MSCs:
-
Adipose tissue-derived MSCs
- Ang-1 /-2:
-
Angiopoietin-1 /-2
- ASCs:
-
Adipose stromal cells
- Bax:
-
BCL2 Associated X
- B-CECs:
-
Bovine corneal endothelial cells
- BM-MSCs:
-
Bone marrow MSCs
- CCL2:
-
C-C motif chemokine ligand 2
- CDH11:
-
Cadherin 11
- circRNA:
-
Circular RNA
- CM:
-
Conditioned media
- COL10:
-
Collagen type X
- COL2A1:
-
Collagen type II α 1 chain
- COMP:
-
Cartilage oligomeric matrix protein
- CS:
-
Cell sheets
- CXCL12:
-
C-X-C motif chemokine 12
- CXCR4:
-
C-X-C chemokine receptor type 4
- DC:
-
Dendritic cells
- DKK-1:
-
Dickkopf 1
- DMEM:
-
Dulbecco's Modified Eagle Medium
- DMEM/F12:
-
Dulbecco's Modified Eagle Medium/Nutrient Mixture F-12
- DPSCs:
-
Dental pulp stromal cells
- E2F2:
-
E2F transcription factor 2
- ECM:
-
Extracellular matrix
- ELF3:
-
E74 Like ETS Transcription Factor 3
- ERK:
-
Extracellular-signal-regulated kinase
- ERK1/2:
-
Extracellular signal‑regulated protein kinase
- ESCs:
-
Embryonic stem cells
- EVs:
-
Extracellular vesicles
- FBS:
-
Fetal bovine serum
- FGF:
-
Fibroblast growth factor
- GAGs:
-
Glycosaminoglycans
- GIT1:
-
ARF GTPase-Activating Protein
- GROα:
-
Growth-regulated α protein
- GRPR:
-
Gastrin Releasing Peptide Receptor
- HA:
-
Hyaluronic acid
- HGF:
-
Hepatocyte growth factor
- HIPK3:
-
Homeodomain interacting protein kinase 3
- ICAM-1:
-
Intercellular adhesion molecule-1
- IFN-γ:
-
Interferon γ
- IGF-1:
-
Insulin-like growth factor 1
- IL-1Ra:
-
Interleukin-1 receptor antagonist
- IL-1β /-6 /-8 /-10:
-
Interleukin 1β /6 /8 /10
- iMSCs:
-
induced mesenchymal stromal cells
- iPSC:
-
induced pluripotent stem cells
- ISCT®:
-
The International Society for Cell and Gene Therapy
- K&L:
-
Kellgren and Lawrence
- KDMA2:
-
Lysine Demethylase 2A
- LIF:
-
leukemia inhibitory factor
- lncKLF3-AS1:
-
KLF Transcription Factor 3 Antisense RNA 1
- lncRNA:
-
long-non coding RNA
- LYRM4:
-
LYR Motif-Containing Protein 4
- MACI:
-
matrix-induced autologous chondrocyte implantation
- MCP-1:
-
monocyte chemotactic protein 1
- METTL3:
-
Methyltransferase 3
- MIP1-α:
-
macrophage inflammatory protein 1α
- miRNA:
-
micro RNA
- MMPs:
-
matrix metalloproteinases
- MPCs:
-
mesenchymal chondro-progenitor cells
- MSC:
-
mesenchymal stromal cell
- MYH9:
-
myosin heavy chain 9
- NF-κB:
-
nuclear factor kappa-light-chain-enhancer of activated B cells
- NK:
-
natural killer cells
- NLRP3:
-
NLR family pyrin domain containing 3
- NO:
-
nitric oxide
- OA:
-
osteoarthritis
- OPG:
-
osteoprotegerin
- p21 /p38 /p53:
-
protein 21 /38 /53
- PAI:
-
plasminogen activator inhibitor
- DDLA-PEG-PDDLA:
-
Poly(D,L-lactide)-block-poly(ethylene glycol)-block-poly(D,L-lactide)
- PDGF:
-
platelet derived growth factor
- PGE2:
-
prostaglandin-E2
- PHLDA2:
-
pleckstrin homology‐like domain family 2
- PI3K/Akt:
-
phosphatidylinositol 3-kinase/Protein Kinase B
- PRP:
-
platelet-rich plasma
- PTEN:
-
phosphatase and tensin homolog deleted on chromosome ten
- RA:
-
rheumatoid arthritis
- RANKL:
-
receptor activator for nuclear factor κβ ligand
- RANTES:
-
regulated upon activation, normal T cell expressed and presumably secreted
- ROS:
-
reactive oxygen species
- RUNX2:
-
RUNX family transcription factor 2
- SA-β-gal:
-
senescence-associated β-galactosidase
- SDC1:
-
Syndecan 1
- SDF-1:
-
stromal cell-derived factor 1
- SEA:
-
N-stearoylethanolamide
- SERPINE:
-
serine proteinase inhibitor
- SHED:
-
human exfoliated deciduous teeth stromal cells
- SM-MSCs:
-
synovial membrane MSCs
- SOX5 /6 /9:
-
SRY-Box transcription factor 5 /6 /9
- SVF:
-
stromal vascular fraction
- TAK1:
-
Transforming Growth Factor-Beta-Activated Kinase 1
- TGF-β1/Smad:
-
transforming growth factor β1/suppressor of mothers against decapentaplegic
- TIMP-1 /-2:
-
tissue inhibitor of metalloproteinases-1 /-2
- TNFα:
-
tumour necrosis factor α
- UCB-MSCs:
-
umbilical cord blood MSCs
- UC-MSCs:
-
umbilical cord MSCs
- VEGF:
-
vascular endothelial growth factor
- VIM:
-
vimentin
- WJ-MSCs:
-
Wharton's jelly MSCs
- WNT/β-catenin:
-
Wingless and Int-1/Beta-catenin signalling pathway
- WNT5a/b:
-
Wnt Family Member 5A/5B
References
Hulme, C. H., Perry, J., McCarthy, H. S., Wright, K. T., Snow, M., Mennan, C., & Roberts, S. (2021). Cell therapy for cartilage repair. Emerging Topics in Life Sciences, 5(4), 575–589. https://doi.org/10.1042/ETLS20210015
Parvizi, J., & Kim, G. K. (2010). Cartilage. High Yield Orthopaedics, 80–81. https://doi.org/10.1016/B978-1-4160-0236-9.00050-X.
Ramasamy, T. S., Yee, Y. M., & Khan, I. M. (2021). Chondrocyte Aging: The Molecular Determinants and Therapeutic Opportunities. Frontiers in Cell and Developmental Biology, 9, 1295. https://doi.org/10.3389/FCELL.2021.625497/BIBTEX
Demoor, M., Ollitrault, D., Gomez-Leduc, T., Bouyoucef, M., Hervieu, M., Fabre, H., … Galera, P. (2014). Cartilage tissue engineering: molecular control of chondrocyte differentiation for proper cartilage matrix reconstruction. Biochimica et Biophysica Acta, 1840(8), 2414–2440. https://doi.org/10.1016/J.BBAGEN.2014.02.030.
Medvedeva, E. V., Grebenik, E. A., Gornostaeva, S. N., Telpuhov, V. I., Lychagin, A. V., Timashev, P. S., & Chagin, A. S. (2018). Repair of Damaged Articular Cartilage: Current Approaches and Future Directions. International Journal of Molecular Sciences, 19(8), 2366. https://doi.org/10.3390/IJMS19082366.
Alan M. Rosenberg, R. E. P. (2021). Structure and function. In P. Ross E. Petty MD, PhD, DSc (Hon), FRCPC, Ronald M. Laxer MDCM, FRCPC, Carol B. Lindsley MD, Lucy R. Wedderburn MD, MA, PhD, FRCP, Elizabeth D. Mellins MD and Robert C. Fuhlbrigge MD (Ed.), Textbook of Pediatric Rheumatology, Eighth Edition (Eighth Edi., pp. 1–11.e2). Elsevier. https://doi.org/10.1007/978-90-481-2888-4.
Wang, Y., Ding, C., Wluka, A. E., Davis, S., Ebeling, P. R., Jones, G., & Cicuttini, F. M. (2006). Factors affecting progression of knee cartilage defects in normal subjects over 2 years. Rheumatology, 45(1), 79–84. https://doi.org/10.1093/RHEUMATOLOGY/KEI108
Cope, P. J., Ourradi, K., Li, Y., & Sharif, M. (2019). Models of osteoarthritis: The good, the bad and the promising. Osteoarthritis and Cartilage, 27(2), 230. https://doi.org/10.1016/J.JOCA.2018.09.016
Łȩgosz, P., Sarzyńska, S., Pulik, Ł, Kotrych, D., & Małdyk, P. (2020). The complexity of molecular processes in osteoarthritis of the knee joint. Open medicine (Warsaw, Poland), 15(1), 366–375. https://doi.org/10.1515/MED-2020-0402
Woetzel, D., Huber, R., Kupfer, P., Pohlers, D., Pfaff, M., Driesch, D., … Kinne, R. W. (2014). Identification of rheumatoid arthritis and osteoarthritis patients by transcriptome-based rule set generation. Arthritis Research & Therapy, 16(2). https://doi.org/10.1186/AR4526.
Peláez, P., Damiá, E., Torres-Torrillas, M., Chicharro, D., Cuervo, B., Miguel, L., … Rubio, M. (2021). Cell and Cell Free Therapies in Osteoarthritis. Biomedicines, 9(11). https://doi.org/10.3390/BIOMEDICINES9111726.
Mattiuzzo, E., Faggian, A., Venerando, R., Benetti, A., Belluzzi, E., Abatangelo, G., … Brun, P. (2021). In Vitro Effects of Low Doses of β-Caryophyllene, Ascorbic Acid and d-Glucosamine on Human Chondrocyte Viability and Inflammation. Pharmaceuticals (Basel, Switzerland), 14(3). https://doi.org/10.3390/PH14030286.
Uzieliene, I., Kalvaityte, U., Bernotiene, E., & Mobasheri, A. (2021). Non-viral Gene Therapy for Osteoarthritis. Frontiers in Bioengineering and Biotechnology, 8. https://doi.org/10.3389/FBIOE.2020.618399.
Gomoll, A. H., Filardo, G., de Girolamo, L., Esprequeira-Mendes, J., Marcacci, M., Rodkey, W. G., … Kon, E. (2011). Surgical treatment for early osteoarthritis. Part I: cartilage repair procedures. Knee Surgery, Sports Traumatology, Arthroscopy, 20(3), 450–466. https://doi.org/10.1007/S00167-011-1780-X.
Loo, S., & Wong, N. (2021). Advantages and challenges of stem cell therapy for osteoarthritis (Review). Biomedical Reports, 15(2). https://doi.org/10.3892/BR.2021.1443.
Z, L., Z, H., & L, B. (2021). Cell Interplay in Osteoarthritis. Frontiers in Cell and Developmental Biology, 9. https://doi.org/10.3389/FCELL.2021.720477.
Lach, M. S., Rosochowicz, M. A., Richter, M., Jagiełło, I., Suchorska, W. M., & Trzeciak, T. (2022). The Induced Pluripotent Stem Cells in Articular Cartilage Regeneration and Disease Modelling: Are We Ready for Their Clinical Use? Cells, 11(3), 529. https://doi.org/10.3390/CELLS11030529.
Fernández-Pernas, P., Barrachina, L., Marquina, M., Rodellar, C., Arufe, M. C., & Costa, C. (2020). Mesenchymal stromal cells for articular cartilage repair: preclinical studies. European Cells & Materials, 40, 88–114. https://doi.org/10.22203/ECM.V040A06.
Kim, Y. G., Choi, J., & Kim, K. (2020). Mesenchymal Stem Cell-Derived Exosomes for Effective Cartilage Tissue Repair and Treatment of Osteoarthritis. Biotechnology Journal, 15(12). https://doi.org/10.1002/BIOT.202000082.
Vinatier, C., Bouffi, C., Merceron, C., Gordeladze, J., Brondello, J.-M., Jorgensen, C., … Noel, D. (2009). Cartilage tissue engineering: towards a biomaterial-assisted mesenchymal stem cell therapy. Current Stem Cell Research & Therapy, 4(4), 318–329. https://doi.org/10.2174/157488809789649205.
Gunawardena, T. N. A., Rahman, M. T., Abdullah, B. J. J., & Kasim, N. H. A. (2019). Conditioned media derived from mesenchymal stem cell cultures: The next generation for regenerative medicine. Journal of Tissue Engineering and Regenerative Medicine, 13(4), 569–586. https://doi.org/10.1002/TERM.2806
Solursh, M., & Meier, S. (1973). A conditioned medium (CM) factor produced by chondrocytes that promotes their own differentiation. Developmental Biology, 30(2), 279–289. https://doi.org/10.1016/0012-1606(73)90089-4
Pawitan, J. A. (2014). Prospect of stem cell conditioned medium in regenerative medicine. BioMed Research International, 2014. https://doi.org/10.1155/2014/965849.
Maguire, G. (2013). Stem cell therapy without the cells. Communicative & Integrative Biology, 6(6). https://doi.org/10.4161/CIB.26631.
Chuang, T. J., Lin, K. C., Chio, C. C., Wang, C. C., Chang, C. P., & Kuo, J. R. (2012). Effects of secretome obtained from normoxia-preconditioned human mesenchymal stem cells in traumatic brain injury rats. Journal of Trauma and Acute Care Surgery, 73(5), 1161–1167. https://doi.org/10.1097/TA.0B013E318265D128
KichenbrandCharlène, VelotEmilie, MenuPatrick, & MobyVanessa. (2019). Dental Pulp Stem Cell-Derived Conditioned Medium: An Attractive Alternative for Regenerative Therapy. https://home.liebertpub.com/teb, 25(1), 78–88. https://doi.org/10.1089/TEN.TEB.2018.0168.
Marlina, M., Armenia, A., Rahmadian, R., Aviani, J. K., Sholihah, I. A., Kusuma, H. S. W., … Widowati, W. (2021). Conditioned Medium of IGF1-Induced Synovial Membrane Mesenchymal Stem Cells Increases Chondrogenic and Chondroprotective Markers in Chondrocyte Inflammation. Bioscience Reports, 41(7), BSR20202038. https://doi.org/10.1042/BSR20202038
Makridakis, M., Roubelakis, M. G., & Vlahou, A. (2013). Stem cells: Insights into the secretome. Biochimica et Biophysica Acta (BBA) - Proteins and Proteomics, 1834(11), 2380–2384. https://doi.org/10.1016/J.BBAPAP.2013.01.032.
Sagaradze, G., Grigorieva, O., Nimiritsky, P., Basalova, N., Kalinina, N., Akopyan, Z., & Efimenko, A. (2019). Conditioned Medium from Human Mesenchymal Stromal Cells: Towards the Clinical Translation. International Journal of Molecular Sciences, 20(7). https://doi.org/10.3390/IJMS20071656.
Ogasawara, N., Kano, F., Hashimoto, N., Mori, H., Liu, Y., Xia, L., … Yamamoto, A. (2020). Factors secreted from dental pulp stem cells show multifaceted benefits for treating experimental temporomandibular joint osteoarthritis. Osteoarthritis and Cartilage, 28(6), 831–841. https://doi.org/10.1016/J.JOCA.2020.03.010.
Muhammad, S. A., Nordin, N., Hussin, P., Mehat, M. Z., Kasim, N. H. A., & Fakurazi, S. (2020). Protective effects of stem cells from human exfoliated deciduous teeth derived conditioned medium on osteoarthritic chondrocytes. PLOS ONE, 15(9), e0238449. https://doi.org/10.1371/JOURNAL.PONE.0238449.
Lee, Y., Park, Y. S., Choi, N. Y., Kim, Y. Il, & Koh, Y. G. (2021). Proteomic Analysis Reveals Commonly Secreted Proteins of Mesenchymal Stem Cells Derived from Bone Marrow, Adipose Tissue, and Synovial Membrane to Show Potential for Cartilage Regeneration in Knee Osteoarthritis. Stem Cells International, 2021. https://doi.org/10.1155/2021/6694299.
Kholodenko, I. V, Konieva, A. A., Kholodenko, R. V, & Yarygin, K. N. (2013). Molecular mechanisms of migration and homing of intravenously transplanted mesenchymal stem cells. Journal of Regenerative Medicine and Tissue Engineering, 2(1), 2. https://doi.org/10.7243/2050-1218-2-4.
Amable, P. R., Teixeira, M. V. T., Carias, R. B. V., Granjeiro, J. M., & Borojevic, R. (2014). Protein synthesis and secretion in human mesenchymal cells derived from bone marrow, adipose tissue and Wharton’s jelly. Stem Cell Research & Therapy, 5(2), 53. https://doi.org/10.1186/SCRT442
Caplan, A. I. (2017). Mesenchymal Stem Cells: Time to Change the Name! STEM CELLS Translational Medicine, 6(6), 1445–1451. https://doi.org/10.1002/sctm.17-0051
Caplan A. I. (2010). What's in a name?. Tissue engineering. Part A, 16(8), 2415–2417. https://doi.org/10.1089/TEN.TEA.2010.0216.
Dominici, M., Blanc, K. Le, Mueller, I., Slaper-Cortenbach, I., Marini, F. ., Krause, D. S., … Horwitz, E. M. (2006). Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy, 8(4), 315–317. https://doi.org/10.1080/14653240600855905.
Kusuma, H. S. W., Widowati, W., Gunanegara, R. F., Juliandi, B., Lister, N. E., Arumwardana, S., … Murti, H. (2020). Effect of conditioned medium from igf1-induced human wharton’s jelly mesenchymal stem cells (Igf1-hwjmscs-cm) on osteoarthritis. Avicenna Journal of Medical Biotechnology, 12(3), 172–178.
P. De Miguel, M., Fuentes-Julian, S., Blazquez-Martinez, A., Y. Pascual, C., A. Aller, M., Arias, J., & Arnalich-Montiel, F. (2012). Immunosuppressive properties of mesenchymal stem cells: advances and applications. Current Molecular Medicine, 12(5), 574–591.https://doi.org/10.2174/156652412800619950.
Bogatcheva, N. V., & Coleman, M. E. (2019). Conditioned Medium of Mesenchymal Stromal Cells: A New Class of Therapeutics. Biochemistry (Moscow) 2019 84:11, 84(11), 1375–1389. https://doi.org/10.1134/S0006297919110129.
Alexandrushkina, N., Nimiritsky, P., Eremichev, R., Popov, V., Arbatskiy, M., Danilova, N., … Makarevich, P. (2020). Cell Sheets from Adipose Tissue MSC Induce Healing of Pressure Ulcer and Prevent Fibrosis via Trigger Effects on Granulation Tissue Growth and Vascularization. International Journal of Molecular Sciences, 21(15), 5567. https://doi.org/10.3390/IJMS21155567.
Zisa, D., Shabbir, A., Suzuki, G., & Lee, T. (2009). Vascular endothelial growth factor (VEGF) as a key therapeutic trophic factor in bone marrow mesenchymal stem cell-mediated cardiac repair. Biochemical and Biophysical Research Communications, 390(3), 834–838. https://doi.org/10.1016/J.BBRC.2009.10.058
Basalova, N., Sagaradze, G., Arbatskiy, M., Evtushenko, E., Kulebyakin, K., Grigorieva, O., … Efimenko, A. (2020). Secretome of Mesenchymal Stromal Cells Prevents Myofibroblasts Differentiation by Transferring Fibrosis-Associated microRNAs within Extracellular Vesicles. Cells, 9(5), 1272. https://doi.org/10.3390/CELLS9051272.
Konala, V. B. R., Bhonde, R., & Pal, R. (2020). Secretome studies of mesenchymal stromal cells (MSCs) isolated from three tissue sources reveal subtle differences in potency. In Vitro Cellular & Developmental Biology - Animal, 56(9), 689–700. https://doi.org/10.1007/S11626-020-00501-1.
Cosenza, S., Ruiz, M., Toupet, K., Jorgensen, C., & Noël, D. (2017). Mesenchymal stem cells derived exosomes and microparticles protect cartilage and bone from degradation in osteoarthritis. Scientific Reports, 7(1), 1–12. https://doi.org/10.1038/s41598-017-15376-8.
Maffioli, E., Nonnis, S., Angioni, R., Santagata, F., Calì, B., Zanotti, L., … Tedeschi, G. (2017). Proteomic analysis of the secretome of human bone marrow-derived mesenchymal stem cells primed by pro-inflammatory cytokines. Journal of Proteomics, 166, 115–126. https://doi.org/10.1016/J.JPROT.2017.07.012.
Kusuma, H. S. W., Widowati, W., Gunanegara, R. F., Juliandi, B., Lister, N. E., Arumwardana, S., … Murti, H. (2020). Effect of Conditioned Medium from IGF1-Induced Human Wharton’s Jelly Mesenchymal Stem Cells (IGF1-hWJMSCs-CM) on Osteoarthritis. Avicenna Journal of Medical Biotechnology, 12(3), 172.
Maumus, M., Jorgensen, C., & Noël, D. (2013). Mesenchymal stem cells in regenerative medicine applied to rheumatic diseases: Role of secretome and exosomes. Biochimie, 95(12), 2229–2234. https://doi.org/10.1016/J.BIOCHI.2013.04.017
Famian, M. H., Saheb, S. M., & Montaseri, A. (2017). Conditioned Medium of Wharton’s Jelly Derived Stem Cells Can Enhance the Cartilage Specific Genes Expression by Chondrocytes in Monolayer and Mass Culture Systems. Advanced Pharmaceutical Bulletin, 7(1), 123–130. https://doi.org/10.15171/APB.2017.016.
Ch. Kichenbrand, E. Velot, P. Menu, & V. Moby. (2019). Dental Pulp Stem Cell-Derived Conditioned Medium: An Attractive Alternative for Regenerative Therapy. https://home.liebertpub.com/teb, 25(1), 78–88. https://doi.org/10.1089/TEN.TEB.2018.0168.
Nosrat, I. V., Widenfalk, J., Olson, L., & Nosrat, C. A. (2001). Dental Pulp Cells Produce Neurotrophic Factors, Interact with Trigeminal Neurons in Vitro, and Rescue Motoneurons after Spinal Cord Injury. Developmental Biology, 238(1), 120–132. https://doi.org/10.1006/DBIO.2001.0400
Wang, X., Sha, X. J., Li, G. H., Yang, F. S., Ji, K., Wen, L. Y., … Xuan, K. (2012). Comparative characterization of stem cells from human exfoliated deciduous teeth and dental pulp stem cells. Archives of Oral Biology, 57(9), 1231–1240. https://doi.org/10.1016/J.ARCHORALBIO.2012.02.014.
Ye, L., Swingen, C., & Zhang, J. (2013). Induced Pluripotent Stem Cells and Their Potential for Basic and Clinical Sciences. Current Cardiology Reviews, 9(1), 63–72. https://doi.org/10.2174/157340313805076278
Wakao, S., Kitada, M., Kuroda, Y., Shigemoto, T., Matsuse, D., Akashi, H., … Dezawa, M. (2011). Multilineage-differentiating stress-enduring (Muse) cells are a primary source of induced pluripotent stem cells in human fibroblasts. Proceedings of the National Academy of Sciences, 108(24), 9875–9880. https://doi.org/10.1073/PNAS.1100816108.
Sakata, R., Iwakura, T., & Reddi, A. H. (2015). Regeneration of Articular Cartilage Surface: Morphogens, Cells, and Extracellular Matrix Scaffolds. Tissue Engineering. Part B, Reviews, 21(5), 461–473. https://doi.org/10.1089/TEN.TEB.2014.0661.
Csobonyeiova, M., Polak, S., Nicodemou, A., Zamborsky, R., & Danisovic, L. (2021). iPSCs in Modeling and Therapy of Osteoarthritis. Biomedicines, 9(2), 1–12. https://doi.org/10.3390/BIOMEDICINES9020186
Murphy, C., Mobasheri, A., Táncos, Z., Kobolák, J., & Dinnyés, A. (2018). The Potency of Induced Pluripotent Stem Cells in Cartilage Regeneration and Osteoarthritis Treatment. Advances in Experimental Medicine and Biology, 1079, 55–68. https://doi.org/10.1007/5584_2017_141
Liu, Q., Guo, Y., Liu, S., Wang, P., Xue, Y., Cui, Z., & Chen, J. (2019). Characterization of the iPSC-derived conditioned medium that promotes the growth of bovine corneal endothelial cells. PeerJ, 7(4). https://doi.org/10.7717/PEERJ.6734.
Hsieh, C. T., Luo, Y. H., Chien, C. S., Wu, C. H., Tseng, P. C., Chiou, S. H., … Chen, Y. M. (2016). Induced Pluripotent Stem Cell-conditioned Medium Suppressed Melanoma Tumorigenicity Through the Enhancement of Natural-Killer Cellular Immunity. Journal of Immunotherapy (Hagerstown, Md. : 1997), 39(4), 153–159. https://doi.org/10.1097/CJI.0000000000000117.
Su, V. Y. F., Chiou, S. H., Chen, W. C., Yu, W. K., Wu, H. H., Chen, H., & Yang, K. Y. (2021). Induced Pluripotent Stem Cell-Derived Conditioned Medium Promotes Endogenous Leukemia Inhibitory Factor to Attenuate Endotoxin-Induced Acute Lung Injury. International Journal of Molecular Sciences, 22(11). https://doi.org/10.3390/IJMS22115554.
Zhou, Y., Zhang, Q., Gao, Y., Tan, M., Zheng, R., Zhao, L., & Zhang, X. (2018). Induced pluripotent stem cell-conditioned medium suppresses pulmonary fibroblast-to-myofibroblast differentiation via the inhibition of TGF-β1/Smad pathway. International Journal of Molecular Medicine, 41(1), 473–484. https://doi.org/10.3892/IJMM.2017.3199
Madrigal, M., Rao, K. S., & Riordan, N. H. (2014). A review of therapeutic effects of mesenchymal stem cell secretions and induction of secretory modification by different culture methods. Journal of Translational Medicine, 12(1), 1–14. https://doi.org/10.1186/S12967-014-0260-8.
Tjalsma, H., Antelmann, H., Jongbloed, J. D. H., Braun, P. G., Darmon, E., Dorenbos, R., … Dijl, J. M. van. (2004). Proteomics of Protein Secretion by Bacillus subtilis: Separating the “Secrets” of the Secretome. Microbiology and Molecular Biology Reviews, 68(2), 207–233. https://doi.org/10.1128/MMBR.68.2.207-233.2004.
Giannasi, C., Niada, S., Della Morte, E., Casati, S., Orioli, M., Gualerzi, A., & Brini, A. T. (2021). Towards Secretome Standardization: Identifying Key Ingredients of MSC-Derived Therapeutic Cocktail. Stem Cells International, 2021. https://doi.org/10.1155/2021/3086122.
D’Arrigo, D., Roffi, A., Cucchiarini, M., Moretti, M., Candrian, C., & Filardo, G. (2019). Secretome and Extracellular Vesicles as New Biological Therapies for Knee Osteoarthritis: A Systematic Review. Journal of Clinical Medicine, 8(11), 1867. https://doi.org/10.3390/JCM8111867.
Bryk, M., Chwastek, J., Mlost, J., Kostrzewa, M., & Starowicz, K. (2021). Sodium Monoiodoacetate Dose-Dependent Changes in Matrix Metalloproteinases and Inflammatory Components as Prognostic Factors for the Progression of Osteoarthritis. Frontiers in Pharmacology, 0, 566. https://doi.org/10.3389/FPHAR.2021.643605.
Mosig, R. A., Dowling, O., DiFeo, A., Ramirez, M. C. M., Parker, I. C., Abe, E., … Martignetti, J. A. (2007). Loss of MMP-2 disrupts skeletal and craniofacial development and results in decreased bone mineralization, joint erosion and defects in osteoblast and osteoclast growth. Human Molecular Genetics, 16(9), 1113–1123. https://doi.org/10.1093/HMG/DDM060.
Vu, T. H. (2001). Don’t mess with the matrix. Nature Genetics 2001 28:3, 28(3), 202–203. https://doi.org/10.1038/90023.
Hannocks, M. J., Zhang, X., Gerwien, H., Chashchina, A., Burmeister, M., Korpos, E., … Sorokin, L. (2019). The gelatinases, MMP-2 and MMP-9, as fine tuners of neuroinflammatory processes. Matrix Biology, 75–76, 102–113. https://doi.org/10.1016/J.MATBIO.2017.11.007.
Lozito, T. P., & Tuan, R. S. (2011). Mesenchymal stem cells inhibit both endogenous and exogenous MMPs via secreted TIMPs. Journal of Cellular Physiology, 226(2), 385–396. https://doi.org/10.1002/JCP.22344
Amodeo, G., Niada, S., Moschetti, G., Franchi, S., Savadori, P., Brini, A. T., & Sacerdote, P. (2021). Secretome of human adipose-derived mesenchymal stem cell relieves pain and neuroinflammation independently of the route of administration in experimental osteoarthritis. Brain, Behavior, and Immunity, 94, 29–40. https://doi.org/10.1016/J.BBI.2021.03.011
Visse, R., & Nagase, H. (2003). Matrix metalloproteinases and tissue inhibitors of metalloproteinases: Structure, function, and biochemistry. Circulation Research, 92(8), 827–839. https://doi.org/10.1161/01.RES.0000070112.80711.3D
Stracke, J. O., Hutton, M., Stewart, M., Pendás, A. M., Smith, B., López-Otin, C., … Knäuper, V. (2000). Biochemical Characterization of the Catalytic Domain of Human Matrix Metalloproteinase 19: EVIDENCE FOR A ROLE AS A POTENT BASEMENT MEMBRANE DEGRADING ENZYME *. Journal of Biological Chemistry, 275(20), 14809–14816. https://doi.org/10.1074/JBC.275.20.14809.
Titz, B., Dietrich, S., Sadowski, T., Beck, C., Petersen, A., & Sedlacek, R. (2004). Activity of MMP-19 inhibits capillary-like formation due to processing of nidogen-1. Cellular and Molecular Life Sciences CMLS, 61(14), 1826–1833. https://doi.org/10.1007/S00018-004-4105-0.
Kalinina, N., Kharlampieva, D., Loguinova, M., Butenko, I., Pobeguts, O., Efimenko, A., … Govorun, V. (2015). Characterization of secretomes provides evidence for adipose-derived mesenchymal stromal cells subtypes. Stem Cell Research and Therapy, 6(1), 1–12. https://doi.org/10.1186/S13287-015-0209-8/FIGURES/3.
Ragni, E., Perucca Orfei, C., De Luca, P., Mondadori, C., Viganò, M., Colombini, A., & De Girolamo, L. (2020). Inflammatory priming enhances mesenchymal stromal cell secretome potential as a clinical product for regenerative medicine approaches through secreted factors and EV-miRNAs: The example of joint disease. Stem Cell Research and Therapy, 11(1), 1–19. https://doi.org/10.1186/S13287-020-01677-9/FIGURES/6
Kawasaki, Y., Xu, Z. Z., Wang, X., Park, J. Y., Zhuang, Z. Y., Tan, P. H., … Ji, R. R. (2008). Distinct roles of matrix metalloproteases in the early- and late-phase development of neuropathic pain. Nature Medicine, 14(3), 331–336. https://doi.org/10.1038/nm1723.
Knight, B. E., Kozlowski, N., Havelin, J., King, T., Crocker, S. J., Young, E. E., & Baumbauer, K. M. (2019). TIMP-1 Attenuates the Development of Inflammatory Pain Through MMP-Dependent and Receptor-Mediated Cell Signaling Mechanisms. Frontiers in Molecular Neuroscience, 12, 220. https://doi.org/10.3389/FNMOL.2019.00220/BIBTEX
Bobick, B. E., Tuan, R. S., & Chen, F. H. (2010). The intermediate filament vimentin regulates chondrogenesis of adult human bone marrow-derived multipotent progenitor cells. Journal of Cellular Biochemistry, 109(1), 265–276. https://doi.org/10.1002/JCB.22419
Blain, E. J., Gilbert, S. J., Hayes, A. J., & Duance, V. C. (2006). Disassembly of the vimentin cytoskeleton disrupts articular cartilage chondrocyte homeostasis. Matrix Biology : Journal of the International Society for Matrix Biology, 25(7), 398–408. https://doi.org/10.1016/j.matbio.2006.06.002
Lee, K., Min, H. K., Koh, S. H., Lee, S. H., Kim, H. R., Ju, J. H., & Kim, H. Y. (2022). Prognostic signature of interferon-γ and interleurkin-17A in early rheumatoid arthritis. Clinical and experimental rheumatology, 40(5), 999–1005. hhttps://doi.org/10.55563/clinexprheumatol/mkbvch
Masuko, K., Murata, M., Suematsu, N., Okamoto, K., Yudoh, K., Shimizu, H., … Kato, T. (2009). A suppressive effect of prostaglandin E2 on the expression of <em>SERPINE1</em>/plasminogen activator inhibitor-1 in human articular chondrocytes: An <em>in vitro</em> pilot study. Open Access Rheumatology: Research and Reviews, 1(1), 9–15. https://doi.org/10.2147/OARRR.S5508.
Santoro, A., Conde, J., Scotece, M., Abella, V., Lois, A., Lopez, V., … Gualillo, O. (2015). SERPINE2 Inhibits IL-1α-Induced MMP-13 Expression in Human Chondrocytes: Involvement of ERK/NF-κB/AP-1 Pathways. PLOS ONE, 10(8), e0135979. https://doi.org/10.1371/JOURNAL.PONE.0135979.
Wang, W., Rigueur, D., & Lyons, K. M. (2014). TGFβ signaling in cartilage development and maintenance. Birth defects research. Part C, Embryo today : reviews, 102(1), 37–51. https://doi.org/10.1002/bdrc.21058.
I, K., Y, A., H, T., T, S., M, T., M, K., … Y, N. (2021). TGFβ1 signaling protects chondrocytes against oxidative stress via FOXO1-autophagy axis. Osteoarthritis and Cartilage.https://doi.org/10.1016/J.JOCA.2021.07.015.
Eleuteri, S., & Fierabracci, A. (2019). Insights into the Secretome of Mesenchymal Stem Cells and Its Potential Applications. International Journal of Molecular Sciences, 20(18), 4597. https://doi.org/10.3390/IJMS20184597.
Kay, A. G., Long, G., Tyler, G., Stefan, A., Broadfoot, S. J., Piccinini, A. M., … Kehoe, O. (2017). Mesenchymal Stem Cell-Conditioned Medium Reduces Disease Severity and Immune Responses in Inflammatory Arthritis. Scientific Reports, 7(1), 1–11. https://doi.org/10.1038/s41598-017-18144-w.
Succar, P., Breen, E. J., Kuah, D., & Herbert, B. R. (2015). Alterations in the Secretome of Clinically Relevant Preparations of Adipose-Derived Mesenchymal Stem Cells Cocultured with Hyaluronan. Stem Cells International, 2015. https://doi.org/10.1155/2015/421253.
Guo, Q., Liu, Z., Wang, M., Guo, S., Cong, H., & Liu, L. (2021). Analysis on the expression and value of CCL2 and CCL3 in patients with osteoarthritis. Experimental and Molecular Pathology, 118, 104576. https://doi.org/10.1016/J.YEXMP.2020.104576.
Gómez-Aristizábal, A., Sharma, A., Bakooshli, M. A., Kapoor, M., Gilbert, P. M., Viswanathan, S., & Gandhi, R. (2017). Stage-specific differences in secretory profile of mesenchymal stromal cells (MSCs) subjected to early- vs late-stage OA synovial fluid. Osteoarthritis and Cartilage, 25(5), 737–741. https://doi.org/10.1016/J.JOCA.2016.11.010
Niada, S., Giannasi, C., Gualerzi, A., Banfi, G., & Brini, A. T. (2018). Differential proteomic analysis predicts appropriate applications for the secretome of adipose-derived mesenchymal stem/stromal cells and dermal fibroblasts. Stem Cells International, 2018. https://doi.org/10.1155/2018/7309031.
Pirosa, A., Tankus, E. B., Mainardi, A., Occhetta, P., Dönges, L., Baum, C., … Barbero, A. (2021). Modeling In Vitro Osteoarthritis Phenotypes in a Vascularized Bone Model Based on a Bone-Marrow Derived Mesenchymal Cell Line and Endothelial Cells. International Journal of Molecular Sciences, 22(17), 9581. https://doi.org/10.3390/IJMS22179581.
Tsai, C. H., Chen, C. J., Gong, C. L., Liu, S. C., Chen, P. C., Huang, C. C., … Tang, C. H. (2021). CXCL13/CXCR5 axis facilitates endothelial progenitor cell homing and angiogenesis during rheumatoid arthritis progression. Cell Death & Disease, 12(9), 1–11. https://doi.org/10.1038/s41419-021-04136-2.
Nagao, M., Hamilton, J. L., Kc, R., Berendsen, A. D., Duan, X., Cheong, C. W., … Olsen, B. R. (2017). Vascular Endothelial Growth Factor in Cartilage Development and Osteoarthritis. Scientific Reports, 7(1), 1–16. https://doi.org/10.1038/s41598-017-13417-w.
Rodriguez-Fontenla, C., Calaza, M., Evangelou, E., Valdes, A. M., Arden, N., Blanco, F. J., … Gonzalez, A. (2014). Assessment of osteoarthritis candidate genes in a meta-analysis of nine genome-wide association studies. Arthritis and Rheumatology, 66(4), 940–949. https://doi.org/10.1002/ART.38300/ABSTRACT.
Ratajczak, M. Z., Kucia, M., Jadczyk, T., Greco, N. J., Wojakowski, W., Tendera, M., & Ratajczak, J. (2011). Pivotal role of paracrine effects in stem cell therapies in regenerative medicine: can we translate stem cell-secreted paracrine factors and microvesicles into better therapeutic strategies? Leukemia, 26(6), 1166–1173. https://doi.org/10.1038/leu.2011.389.
Tonomura, H., Takahashi, K., Nagae, M., Takatori, R., Ishibashi, H., & Itsuji, T. (2020). The Potential Role of Hepatocyte Growth Factor in Degenerative Disorders of the Synovial Joint and Spine. International Journal of Molecular Sciences, 21(22), 8717. https://doi.org/10.3390/IJMS21228717.
Wong, P. K. K., Campbell, I. K., Egan, P. J., Ernst, M., & Wicks, I. P. (2003). The role of the interleukin-6 family of cytokines in inflammatory arthritis and bone turnover. Arthritis & Rheumatism, 48(5), 1177–1189. https://doi.org/10.1002/ART.10943
Nummenmaa, E., Hämäläinen, M., Pemmari, A., Moilanen, L. J., Tuure, L., Nieminen, R. M., … Moilanen, E. (2020). Transient Receptor Potential Ankyrin 1 (TRPA1) Is Involved in Upregulating Interleukin-6 Expression in Osteoarthritic Chondrocyte Models. International Journal of Molecular Sciences, 22(1), 87. https://doi.org/10.3390/IJMS22010087.
Lotz, M., Moats, T., & Villiger, P. M. (1992). Leukemia inhibitory factor is expressed in cartilage and synovium and can contribute to the pathogenesis of arthritis. The Journal of Clinical Investigation, 90(3), 888–896. https://doi.org/10.1172/JCI115964
Carroll, G. J., & Bell, M. C. (1993). Leukaemia inhibitory factor stimulates proteoglycan resorption in porcine articular cartilage. Rheumatology International, 13(1), 5–8. https://doi.org/10.1007/BF00290327.
Chia, S. L., Sawaji, Y., Burleigh, A., McLean, C., Inglis, J., Saklatvala, J., & Vincent, T. (2009). Fibroblast growth factor 2 is an intrinsic chondroprotective agent that suppresses ADAMTS-5 and delays cartilage degradation in murine osteoarthritis. Arthritis & Rheumatism, 60(7), 2019–2027. https://doi.org/10.1002/ART.24654
Vincent, T., Hermansson, M., Bolton, M., Wait, R., & Saklatvala, J. (2002). Basic FGF mediates an immediate response of articular cartilage to mechanical injury. Proceedings of the National Academy of Sciences, 99(12), 8259–8264. https://doi.org/10.1073/PNAS.122033199
Alvarez, R. H., Kantarjian, H. M., & Cortes, J. E. (2006). Biology of Platelet-Derived Growth Factor and Its Involvement in Disease. Mayo Clinic Proceedings, 81(9), 1241–1257. https://doi.org/10.4065/81.9.1241
Zhu, P., Wang, Z., Sun, Z., Liao, B., & Cai, Y. (2021). Recombinant platelet-derived growth factor-BB alleviates osteoarthritis in a rat model by decreasing chondrocyte apoptosis in vitro and in vivo. Journal of Cellular and Molecular Medicine, 25(15), 7472–7484. https://doi.org/10.1111/JCMM.16779
Tian, Z., Zeng, F., Zhao, C., & Dong, S. (2021). Angelicin Alleviates Post-Trauma Osteoarthritis Progression by Regulating Macrophage Polarization via STAT3 Signaling Pathway. Frontiers in Pharmacology, 0, 1326. https://doi.org/10.3389/FPHAR.2021.669213.
Kotake, S., Nanke, Y., Mogi, M., Kawamoto, M., Furuya, T., Yago, T., … Kamatani, N. (2005). IFN-γ-producing human T cells directly induce osteoclastogenesis from human monocytes via the expression of RANKL. European Journal of Immunology, 35(11), 3353–3363. https://doi.org/10.1002/EJI.200526141.
Zheng, L., Hu, F., Bian, W., Li, Y., Zhang, L., Shi, L., … Li, Z. (2021). Dickkopf-1 perpetuated synovial fibroblast activation and synovial angiogenesis in rheumatoid arthritis. Clinical Rheumatology, 40(10), 4279–4288. https://doi.org/10.1007/S10067-021-05766-9.
Li, W., Xiong, Y., Chen, W., & Wu, L. (2020). Wnt/β-catenin signaling may induce senescence of chondrocytes in osteoarthritis. Experimental and Therapeutic Medicine, 20(3), 2631–2638. https://doi.org/10.3892/ETM.2020.9022
Cici, D., Corrado, A., Rotondo, C., & Cantatore, F. P. (2019). Wnt Signaling and Biological Therapy in Rheumatoid Arthritis and Spondyloarthritis. International Journal of Molecular Sciences, 20(22), 5552. https://doi.org/10.3390/IJMS20225552.
Kapoor, M., Martel-Pelletier, J., Lajeunesse, D., Pelletier, J. P., & Fahmi, H. (2010). Role of proinflammatory cytokines in the pathophysiology of osteoarthritis. Nature Reviews Rheumatology, 7(1), 33–42. https://doi.org/10.1038/nrrheum.2010.196.
Kang, S., Tanaka, T., Narazaki, M., & Kishimoto, T. (2019). Targeting Interleukin-6 Signaling in Clinic. Immunity, 50(4), 1007–1023. https://doi.org/10.1016/J.IMMUNI.2019.03.026
De Benedetti, F., Rucci, N., Del Fattore, A., Peruzzi, B., Paro, R., Longo, M., … Teti, A. (2006). Impaired skeletal development in interleukin-6–transgenic mice: A model for the impact of chronic inflammation on the growing skeletal system. Arthritis & Rheumatism, 54(11), 3551–3563. https://doi.org/10.1002/ART.22175.
Nakahara, H., Song, J., Sugimoto, M., Hagihara, K., Kishimoto, T., Yoshizaki, K., & Nishimoto, N. (2003). Anti–interleukin-6 receptor antibody therapy reduces vascular endothelial growth factor production in rheumatoid arthritis. Arthritis & Rheumatism, 48(6), 1521–1529. https://doi.org/10.1002/ART.11143
Nees, T. A., Rosshirt, N., Zhang, J. A., Reiner, T., Sorbi, R., Tripel, E., … Moradi, B. (2019). Synovial Cytokines Significantly Correlate with Osteoarthritis-Related Knee Pain and Disability: Inflammatory Mediators of Potential Clinical Relevance. Journal of Clinical Medicine, 8(9), 1343. https://doi.org/10.3390/JCM8091343.
Wang, Y., & Lou, S. (2001). Direct protective effect of interleukin-10 on articular chondrocytes in vitro. Chinese Medical Journal, 114(7), 723–725.
Jia, D., Li, Y., Han, R., Wang, K., Cai, G., He, C., & Yang, L. (2019). MiR-146a-5p expression is upregulated by the CXCR4 antagonist TN14003 and attenuates SDF-1-induced cartilage degradation. Molecular Medicine Reports, 49(5), 4388–4400. https://doi.org/10.3892/MMR.2019.10076/HTML
Zheng, X., Zhao, F. chao, Pang, Y., Li, D. ya, Yao, S. cheng, Sun, S. song, & Guo, K. jin. (2017). Downregulation of miR-221–3p contributes to IL-1β-induced cartilage degradation by directly targeting the SDF1/CXCR4 signaling pathway. Journal of Molecular Medicine, 95(6), 615–627. https://doi.org/10.1007/S00109-017-1516-6.
Li, C., He, Y., Li, Y., Wang, G., Liu, D., Cai, G., & He, C. (2021). A novel method to establish the rabbit model of knee osteoarthritis: Intra-articular injection of SDF-1 induces OA. BMC Musculoskeletal Disorders, 22(1), 1–10. https://doi.org/10.1186/S12891-021-04188-7/TABLES/2
Lu, J., Wu, Z., & Xiong, Y. (2021). Knockdown of long noncoding RNA HOTAIR inhibits osteoarthritis chondrocyte injury by miR-107/CXCL12 axis. Journal of Orthopaedic Surgery and Research, 16(1), 1–11. https://doi.org/10.1186/S13018-021-02547-7/FIGURES/7
Vaughan, D. E. (2005). PAI-1 and atherothrombosis. Journal of Thrombosis and Haemostasis, 3(8), 1879–1883. https://doi.org/10.1111/J.1538-7836.2005.01420.X
Casati, S., Giannasi, C., Niada, S., Bergamaschi, R. F., Orioli, M., & Brini, A. T. (2021). Bioactive Lipids in MSCs Biology: State of the Art and Role in Inflammation. International Journal of Molecular Sciences, 22(3), 1481. https://doi.org/10.3390/IJMS22031481.
Mehana, E. S. E., Khafaga, A. F., & El-Blehi, S. S. (2019). The role of matrix metalloproteinases in osteoarthritis pathogenesis: An updated review. Life Sciences, 234, 116786. https://doi.org/10.1016/J.LFS.2019.116786.
Bollmann, M., Pinno, K., Ehnold, L. I., Märtens, N., Märtson, A., Pap, T., … Bertrand, J. (2021). MMP-9 mediated Syndecan-4 shedding correlates with osteoarthritis severity. Osteoarthritis and Cartilage, 29(2), 280–289. https://doi.org/10.1016/J.JOCA.2020.10.009.
Nakamura, T., Sakai, K., Nakamura, T., & Matsumoto, K. (2011). Hepatocyte growth factor twenty years on: Much more than a growth factor. Journal of Gastroenterology and Hepatology, 26(Suppl 1), 188–202. https://doi.org/10.1111/j.1440-1746.2010.06549.x
Okunishi, K., Dohi, M., Fujio, K., Nakagome, K., Tabata, Y., Okasora, T., … Yamamoto, K. (2007). Hepatocyte growth factor significantly suppresses collagen-induced arthritis in mice. Journal of Immunology (Baltimore, Md. : 1950), 179(8), 5504–5513. https://doi.org/10.4049/JIMMUNOL.179.8.5504.
Wakitani, S., Imoto, K., Kimura, T., Ochi, T., Matsumoto, K., & Nakamura, T. (1997). Hepatocyte growth factor facilitates cartilage repair. Full thickness articular cartilage defect studied in rabbit knees. Acta Orthopaedica Scandinavica, 68(5), 474–480. https://doi.org/10.3109/17453679708996266.
Yoshimura, S., Teramoto, T., Whalen, M. J., Irizarry, M. C., Takagi, Y., Qiu, J., … Moskowitz, M. A. (2003). FGF-2 regulates neurogenesis and degeneration in the dentate gyrus after traumatic brain injury in mice. The Journal of Clinical Investigation, 112(8), 1202–1210. https://doi.org/10.1172/JCI16618.
Lin, Y. M., Hsu, C. J., Liao, Y. Y., Chou, M. C., & Tang, C. H. (2012). The CCL2/CCR2 Axis Enhances Vascular Cell Adhesion Molecule-1 Expression in Human Synovial Fibroblasts. PLOS ONE, 7(11), e49999. https://doi.org/10.1371/JOURNAL.PONE.0049999.
Key, L. L. J., Rodriguiz, R. M., Willi, S. M., Wright, N. M., Hatcher, H. C., Eyre, D. R., … Ries, W. L. (2009). Long-Term Treatment of Osteopetrosis with Recombinant Human Interferon Gamma. 332(24), 1594–1599. https://doi.org/10.1056/NEJM199506153322402.
Qin, H. J., Xu, T., Wu, H. T., Yao, Z. L., Hou, Y. L., Xie, Y. H., … Cui, Z. (2019). SDF-1/CXCR4 axis coordinates crosstalk between subchondral bone and articular cartilage in osteoarthritis pathogenesis. Bone, 125, 140–150. https://doi.org/10.1016/J.BONE.2019.05.010.
García-Bernal, D., García-Arranz, M., Yáñez, R. M., Hervás-Salcedo, R., Cortés, A., Fernández-García, M., … Zapata, A. G. (2021). The Current Status of Mesenchymal Stromal Cells: Controversies, Unresolved Issues and Some Promising Solutions to Improve Their Therapeutic Efficacy. Frontiers in Cell and Developmental Biology, 9, 609. https://doi.org/10.3389/FCELL.2021.650664/BIBTEX.
Zavatti, M., Beretti, F., Casciaro, F., Bertucci, E., & Maraldi, T. (2020). Comparison of the therapeutic effect of amniotic fluid stem cells and their exosomes on monoiodoacetate-induced animal model of osteoarthritis. BioFactors, 46(1), 106–117. https://doi.org/10.1002/BIOF.1576
Bousnaki, M., Bakopoulou, A., Kritis, A., & Koidis, P. (2020). The Efficacy of Stem Cells Secretome Application in Osteoarthritis: A Systematic Review of In Vivo Studies. Stem Cell Reviews and Reports, 16(6), 1222–1241. https://doi.org/10.1007/S12015-020-09980-X
Manferdini, C., Maumus, M., Gabusi, E., Paolella, F., Grassi, F., Jorgensen, C., … Lisignoli, G. (2015). Lack of anti-inflammatory and anti-catabolic effects on basal inflamed osteoarthritic chondrocytes or synoviocytes by adipose stem cell-conditioned medium. Osteoarthritis and Cartilage, 23(11), 2045–2057. https://doi.org/10.1016/J.JOCA.2015.03.025.
Simental-Mendía, M., Lozano-Sepúlveda, S. A., Pérez-Silos, V., Fuentes-Mera, L., Martínez-Rodríguez, H. G., Acosta-Olivo, C. A., … Vilchez-Cavazos, F. (2020). Anti‑inflammatory and anti‑catabolic effect of non‑animal stabilized hyaluronic acid and mesenchymal stem cell‑conditioned medium in an osteoarthritis coculture model. Molecular Medicine Reports, 21(5), 2243–2250. https://doi.org/10.3892/MMR.2020.11004.
S, N., C, G., M, G., D, S., S, C., & AT, B. (2019). Adipose-derived stromal cell secretome reduces TNFα-induced hypertrophy and catabolic markers in primary human articular chondrocytes. Stem Cell Research, 38. https://doi.org/10.1016/J.SCR.2019.101463.
Platas, J., Guillén, M. I., Pérez Del Caz, M. D., Gomar, F., Castejón, M. A., Mirabet, V., & Alcaraz, M. J. (2016). Paracrine effects of human adipose-derived mesenchymal stem cells in inflammatory stress-induced senescence features of osteoarthritic chondrocytes. Aging, 8(8), 1703–1717. https://doi.org/10.18632/aging.101007.
Marlina, M., Rahmadian, R., Armenia, A., Aviani, J. K., Sholihah, I. A., Kusuma, H. S. W., … Widowati, W. (2021). Conditioned medium of IGF1-induced synovial membrane mesenchymal stem cells increases chondrogenic and chondroprotective markers in chondrocyte inflammation. Bioscience Reports, 41(7). 10.1042/BSR20202038.
Chen, W., Sun, Y., Gu, X., Hao, Y., Liu, X., Lin, J., … Chen, S. (2019). Conditioned medium of mesenchymal stem cells delays osteoarthritis progression in a rat model by protecting subchondral bone, maintaining matrix homeostasis, and enhancing autophagy. Journal of Tissue Engineering and Regenerative Medicine, 13(9), 1618–1628. https://doi.org/10.1002/TERM.2916.
Widowati, W., Wijaya, L., Bachtiar, I., Gunanegara, R. F., Sugeng, S. U., Irawan, Y. A., … Aris Widodo, M. (2014). Effect of oxygen tension on proliferation and characteristics of Wharton’s jelly-derived mesenchymal stem cells. Biomarkers and Genomic Medicine, 6(1), 43–48. https://doi.org/10.1016/J.BGM.2014.02.001.
Simons, M., & Raposo, G. (2009). Exosomes-vesicular carriers for intercellular communication. Current Opinion in Cell Biology, 21(4), 575–581. https://doi.org/10.1016/j.ceb.2009.03.007
Lener, T., Gioma, M., Aigner, L., Börger, V., Buzas, E., Camussi, G., … Giebel, B. (2015). Applying extracellular vesicles based therapeutics in clinical trials - an ISEV position paper. Journal of Extracellular Vesicles, 4, 1–31. https://doi.org/10.3402/jev.v4.30087.
Harding, C. V., Heuser, J. E., & Stahl, P. D. (2013). Exosomes: Looking back three decades and into the future. The Journal of Cell Biology, 200(4), 367–371. https://doi.org/10.1083/jcb.201212113
Hosseini-Beheshti, E., Pham, S., Adomat, H., Li, N., & Tomlinson Guns, E. S. (2012). Exosomes as biomarker enriched microvesicles: Characterization of exosomal proteins derived from a panel of prostate cell lines with distinct AR phenotypes. Molecular & Cellular Proteomics : MCP, 11(10), 863–885. https://doi.org/10.1074/mcp.M111.014845
Dai, J., Su, Y., Zhong, S., Cong, L., Liu, B., Yang, J., … Jiang, Y. (2020). Exosomes: key players in cancer and potential therapeutic strategy. Signal Transduction and Targeted Therapy, 5(1), 145. https://doi.org/10.1038/s41392-020-00261-0.
Wróblewska, J. P., Lach, M. S., Rucinski, M., Piotrowski, I., Galus, L., Suchorska, W. M., … Marszałek, A. (2022). MiRNAs from serum-derived extracellular vesicles as biomarkers for uveal melanoma progression. Frontiers in Cell and Developmental Biology, 10. https://doi.org/10.3389/fcell.2022.1008901.
Dimik, M., Abeysinghe, P., Logan, J., & Mitchell, M. (2023). The exosome: A review of current therapeutic roles and capabilities in human reproduction. Drug Delivery and Translational Research, 13(2), 473–502. https://doi.org/10.1007/s13346-022-01225-3
Roma-Rodrigues, C., Fernandes, A. R., & Baptista, P. V. (2014). Exosome in tumour microenvironment: overview of the crosstalk between normal and cancer cells. BioMed Research International, 2014, 179486. https://doi.org/10.1155/2014/179486.
Beach, A., Zhang, H., Ratajczak, M. Z., & Kakar, S. S. (2014). Exosomes : An overview of biogenesis, composition and role in ovarian cancer Exosomes : An overview of biogenesis, composition and role in ovarian cancer. Journal of Ovarian Research, 7(1), 1–10. https://doi.org/10.1186/1757-2215-7-14
Ratajczak, M. Z., & Ratajczak, J. (2021). Innate Immunity Communicates Using the Language of Extracellular Microvesicles. Stem Cell Reviews and Reports, 17(2), 502–510. https://doi.org/10.1007/s12015-021-10138-6
Kucharzewska, P., & Belting, M. (2013). Emerging roles of extracellular vesicles in the adaptive response of tumour cells to microenvironmental stress. Journal of extracellular vesicles, 2, 20304. https://doi.org/10.3402/jev.v2i0.20304
Chen, S., Sun, F., Qian, H., Xu, W., & Jiang, J. (2022). Preconditioning and Engineering Strategies for Improving the Efficacy of Mesenchymal Stem Cell-Derived Exosomes in Cell-Free Therapy. Stem Cells International, 2022. https://doi.org/10.1155/2022/1779346.
Thomas, B. L., Eldridge, S. E., Nosrati, B., Alvarez, M., Thorup, A. S., Nalesso, G., … Dell’Accio, F. (2021). WNT3A-loaded exosomes enable cartilage repair. Journal of Extracellular Vesicles, 10(7). https://doi.org/10.1002/jev2.12088.
Fais, S., Logozzi, M., Lugini, L., Federici, C., Azzarito, T., Zarovni, N., & Chiesi, A. (2013). Exosomes: The ideal nanovectors for biodelivery. Biological Chemistry, 394(1), 1–15. https://doi.org/10.1515/hsz-2012-0236
Lee, Y. H., Park, H. K., Auh, Q. S., Nah, H., Lee, J. S., Moon, H. J., … Kwon, I. K. (2020). Emerging potential of exosomes in regenerative medicine for temporomandibular joint osteoarthritis. International Journal of Molecular Sciences, 21(4). https://doi.org/10.3390/ijms21041541.
Burke, J., Kolhe, R., Hunter, M., Isales, C., Hamrick, M., & Fulzele, S. (2016). Stem cell-derived exosomes: A potential alternative therapeutic agent in orthopaedics. Stem Cells International, 2016, 5–8. https://doi.org/10.1155/2016/5802529
Sampey, G. C., Meyering, S. S., Asad Zadeh, M., Saifuddin, M., Hakami, R. M., & Kashanchi, F. (2014). Exosomes and their role in CNS viral infections. Journal of Neurovirology, 20(3), 199–208. https://doi.org/10.1007/s13365-014-0238-6
Liu, S., Mahairaki, V., Bai, H., Ding, Z., Li, J., Witwer, K. W., & Cheng, L. (2019). Highly Purified Human Extracellular Vesicles Produced by Stem Cells Alleviate Aging Cellular Phenotypes of Senescent Human Cells. Stem cells (Dayton, Ohio), 37(6), 779–790. https://doi.org/10.1002/stem.2996
Esmaeili, A., Hosseini, S., Kamali, A., Hosseinzadeh, M., Shekari, F., & Baghaban Eslaminejad, M. (2022). Co-aggregation of MSC/chondrocyte in a dynamic 3D culture elevates the therapeutic effect of secreted extracellular vesicles on osteoarthritis in a rat model. Scientific Reports, 12(1), 19827. https://doi.org/10.1038/s41598-022-22592-4
Nguyen, T. H., Dao, H. H., Duong, C. M., Nguyen, X.-H., Hoang, D. H., Do, X.-H., … Than, U. T. T. (2022). Cytokine-primed umbilical cord mesenchymal stem cells enhanced therapeutic effects of extracellular vesicles on osteoarthritic chondrocytes. Frontiers in Immunology, 13(October), 1–12. https://doi.org/10.3389/fimmu.2022.1041592.
Qiu, B., Xu, X., Yi, P., & Hao, Y. (2020). Curcumin reinforces MSC-derived exosomes in attenuating osteoarthritis via modulating the miR-124/NF-kB and miR-143/ROCK1/TLR9 signalling pathways. Journal of Cellular and Molecular Medicine, 24(18), 10855–10865. https://doi.org/10.1111/jcmm.15714
Li, J., Lee, Y., Johansson, H. J., Mäger, I., Vader, P., Nordin, J. Z., … Andaloussi, S. EL. (2015). Serum-free culture alters the quantity and protein composition of neuroblastoma-derived extracellular vesicles. Journal of Extracellular Vesicles, 4(1), 26883. https://doi.org/10.3402/jev.v4.26883.
Pu, Y., Li, C., Qi, X., Xu, R., Dong, L., Jiang, Y., … Cheng, R. (2023). Extracellular Vesicles from NMN Preconditioned Mesenchymal Stem Cells Ameliorated Myocardial Infarction via miR ‑ 210 ‑ 3p Promoted Angiogenesis. Stem Cell Reviews and Reports, (0123456789). https://doi.org/10.1007/s12015-022-10499-6.
Kim, S., Lee, S. A., Yoon, H., Kim, M. Y., Yoo, J.-K., Ahn, S.-H., … Yoo, T.-H. (2021). Exosome-based delivery of super-repressor IκBα ameliorates kidney ischemia-reperfusion injury. Kidney International, 100(3), 570–584. https://doi.org/10.1016/j.kint.2021.04.039.
Seyedaghamiri, F., Salimi, L., Ghaznavi, D., Sokullu, E., & Rahbarghazi, R. (2022). Exosomes-based therapy of stroke, an emerging approach toward recovery. Cell Communication and Signaling, 20(1), 110. https://doi.org/10.1186/s12964-022-00919-y
Golchin, A., Shams, F., Basiri, A., Ranjbarvan, P., Kiani, S., Sarkhosh-Inanlou, R., … Rasmi, Y. (2022). Combination Therapy of Stem Cell-derived Exosomes and Biomaterials in the Wound Healing. Stem Cell Reviews and Reports, 18(6), 1892–1911. https://doi.org/10.1007/s12015-021-10309-5.
Zhang, L., Ouyang, P., He, G., Wang, X., Song, D., Yang, Y., & He, X. (2021). Exosomes from microRNA-126 overexpressing mesenchymal stem cells promote angiogenesis by targeting the PIK3R2-mediated PI3K/Akt signalling pathway. Journal of Cellular and Molecular Medicine, 25(4), 2148–2162. https://doi.org/10.1111/jcmm.16192
Jamshidi, E., Babajani, A., Soltani, P., & Niknejad, H. (2021). Proposed Mechanisms of Targeting COVID-19 by Delivering Mesenchymal Stem Cells and Their Exosomes to Damaged Organs. Stem Cell Reviews and Reports, 17(1), 176–192. https://doi.org/10.1007/s12015-020-10109-3
AbuBakr, N., Fares, A. E., Mostafa, A., & Farag, D. B. E. (2022). Mesenchymal stem cells-derived microvesicles versus platelet-rich plasma in the treatment of monoiodoacetate-induced temporomandibular joint osteoarthritis in Albino rats. Heliyon, 8(10), e10857. https://doi.org/10.1016/j.heliyon.2022.e10857.
Wang, Y., Zhao, M., Li, W., Yang, Y., Zhang, Z., Ma, R., & Wu, M. (2021). BMSC-Derived Small Extracellular Vesicles Induce Cartilage Reconstruction of Temporomandibular Joint Osteoarthritis via Autotaxin–YAP Signaling Axis. Frontiers in Cell and Developmental Biology, 9(April), 1–16. https://doi.org/10.3389/fcell.2021.656153
Zhu, L., Shi, Y., Liu, L., Wang, H., Shen, P., & Yang, H. (2020). Mesenchymal stem cells-derived exosomes ameliorate nucleus pulposus cells apoptosis via delivering miR-142-3p: Therapeutic potential for intervertebral disc degenerative diseases. Cell Cycle, 19(14), 1727–1739. https://doi.org/10.1080/15384101.2020.1769301
Sun, Y., Zhang, W., & Li, X. (2021). Induced pluripotent stem cell-derived mesenchymal stem cells deliver exogenous miR-105-5p via small extracellular vesicles to rejuvenate senescent nucleus pulposus cells and attenuate intervertebral disc degeneration. Stem Cell Research and Therapy, 12(1), 1–14. https://doi.org/10.1186/s13287-021-02362-1
Gorgun, C., Palamà, M. E. F., Reverberi, D., Gagliani, M. C., Cortese, K., Tasso, R., & Gentili, C. (2021). Role of extracellular vesicles from adipose tissue- and bone marrow-mesenchymal stromal cells in endothelial proliferation and chondrogenesis. Stem Cells Translational Medicine, 10(12), 1680–1695. https://doi.org/10.1002/sctm.21-0107
Kim, M., Steinberg, D. R., Burdick, J. A., & Mauck, R. L. (2019). Extracellular vesicles mediate improved functional outcomes in engineered cartilage produced from MSC/chondrocyte cocultures. Proceedings of the National Academy of Sciences, 116(5), 1569–1578. https://doi.org/10.1073/pnas.1815447116
Malekpour, K., Hazrati, A., Zahar, M., Markov, A., Zekiy, A. O., Navashenaq, J. G., … Ahmadi, M. (2022). The Potential Use of Mesenchymal Stem Cells and Their Derived Exosomes for Orthopedic Diseases Treatment. Stem Cell Reviews and Reports, 18(3), 933–951. https://doi.org/10.1007/s12015-021-10185-z.
Tao, S. C., Yuan, T., Zhang, Y. L., Yin, W. J., Guo, S. C., & Zhang, C. Q. (2017). Exosomes derived from miR-140-5p-overexpressing human synovial mesenchymal stem cells enhance cartilage tissue regeneration and prevent osteoarthritis of the knee in a rat model. Theranostics, 7(1), 180–195. https://doi.org/10.7150/thno.17133
Zhang, J., Rong, Y., Luo, C., & Cui, W. (2020). Bone marrow mesenchymal stem cell-derived exosomes prevent osteoarthritis by regulating synovial macrophage polarization. Aging, 12(24), 25138–25152. https://doi.org/10.18632/aging.104110.
Zhou, Y., Ming, J., Li, Y., Li, B., Deng, M., Ma, Y., … Liu, S. (2021). Exosomes derived from miR-126–3p-overexpressing synovial fibroblasts suppress chondrocyte inflammation and cartilage degradation in a rat model of osteoarthritis. Cell Death Discovery, 7(1), 37. https://doi.org/10.1038/s41420-021-00418-y.
Li, C., Li, W., Pu, G., Wu, J., & Qin, F. (2022). Exosomes derived from miR-338-3p-modified adipose stem cells inhibited inflammation injury of chondrocytes via targeting RUNX2 in osteoarthritis. Journal of Orthopaedic Surgery and Research, 17(1), 567. https://doi.org/10.1186/s13018-022-03437-2
Kim, M., Shin, D. I., Choi, B. H., & Min, B. H. (2021). Exosomes from IL-1β-Primed Mesenchymal Stem Cells Inhibited IL-1β- and TNF-α-Mediated Inflammatory Responses in Osteoarthritic SW982 Cells. Tissue Engineering and Regenerative Medicine, 18(4), 525–536. https://doi.org/10.1007/s13770-020-00324-x
Liu, Y., Lin, L., Zou, R., Wen, C., Wang, Z., & Lin, F. (2018). MSC-derived exosomes promote proliferation and inhibit apoptosis of chondrocytes via lncRNA-KLF3-AS1/miR-206/GIT1 axis in osteoarthritis. Cell Cycle, 17(21–22), 2411–2422. https://doi.org/10.1080/15384101.2018.1526603
Zhu, Y., Wang, Y., Zhao, B., Niu, X., Hu, B., Li, Q., … Wang, Y. (2017). Comparison of exosomes secreted by induced pluripotent stem cell-derived mesenchymal stem cells and synovial membrane-derived mesenchymal stem cells for the treatment of osteoarthritis. Stem Cell Research & Therapy, 8(1), 64. https://doi.org/10.1186/s13287-017-0510-9.
Xia, Q., Wang, Q., Lin, F., & Wang, J. (2021). miR-125a-5p-abundant exosomes derived from mesenchymal stem cells suppress chondrocyte degeneration via targeting E2F2 in traumatic osteoarthritis. Bioengineered, 12(2), 11225–11238. https://doi.org/10.1080/21655979.2021.1995580
Li, S., Liu, J., Liu, S., Jiao, W., & Wang, X. (2021). Mesenchymal stem cell-derived extracellular vesicles prevent the development of osteoarthritis via the circHIPK3/miR-124-3p/MYH9 axis. Journal of Nanobiotechnology, 19(1), 194. https://doi.org/10.1186/s12951-021-00940-2
Wang, H., Shu, J., Zhang, C., Wang, Y., Shi, R., Yang, F., & Tang, X. (2022). Extracellular Vesicle-Mediated miR-150-3p Delivery in Joint Homeostasis: A Potential Treatment for Osteoarthritis? Cells, 11(17), 2766. https://doi.org/10.3390/cells11172766
Zhou, H., Shen, X., Yan, C., Xiong, W., Ma, Z., Tan, Z., … Liu, F. (2022). Extracellular vesicles derived from human umbilical cord mesenchymal stem cells alleviate osteoarthritis of the knee in mice model by interacting with METTL3 to reduce m6A of NLRP3 in macrophage. Stem Cell Research and Therapy, 13(1), 1–21. https://doi.org/10.1186/s13287-022-03005-9.
Tao, S.-C., Huang, J.-Y., Gao, Y., Li, Z.-X., Wei, Z.-Y., Dawes, H., & Guo, S.-C. (2021). Small extracellular vesicles in combination with sleep-related circRNA3503: A targeted therapeutic agent with injectable thermosensitive hydrogel to prevent osteoarthritis. Bioactive Materials, 6(12), 4455–4469. https://doi.org/10.1016/j.bioactmat.2021.04.031
Wang, S., Hou, Y., Li, X., Song, Z., Sun, B., Li, X., & Zhang, H. (2020). Comparison of exosomes derived from induced pluripotent stem cells and mesenchymal stem cells as therapeutic nanoparticles for treatment of corneal epithelial defects. Aging, 12(19), 19546–19562. https://doi.org/10.18632/aging.103904.
Usami, Y., Gunawardena, A. T., Iwamoto, M., & Enomoto-Iwamoto, M. (2016). Wnt signaling in cartilage development and diseases: Lessons from animal studies. Laboratory Investigation, 96(2), 186–196. https://doi.org/10.1038/labinvest.2015.142
Ye, P., Mi, Z., Wei, D., Gao, P., Ma, M., & Yang, H. (2022). miR-3960 from Mesenchymal Stem Cell-Derived Extracellular Vesicles Inactivates SDC1/Wnt/β-Catenin Axis to Relieve Chondrocyte Injury in Osteoarthritis by Targeting PHLDA2. Stem Cells International, 2022, 1–18. https://doi.org/10.1155/2022/9455152
Yang, H., Cong, M., Huang, W., Chen, J., Zhang, M., Gu, X., … Yang, H. (2022). The Effect of Human Bone Marrow Mesenchymal Stem Cell-Derived Exosomes on Cartilage Repair in Rabbits. Stem Cells International, 2022, 1–12. https://doi.org/10.1155/2022/5760107.
Li, P., Lv, S., Jiang, W., Si, L., Liao, B., Zhao, G., … Li, Y. (2022). Exosomes derived from umbilical cord mesenchymal stem cells protect cartilage and regulate the polarization of macrophages in osteoarthritis. Annals of Translational Medicine, 10(18), 976–976. https://doi.org/10.21037/atm-22-3912.
Pan, C., Huang, W., Chen, Q., Xu, J., Yao, G., Li, B., … Cheng, X. (2021). LncRNA Malat-1 From MSCs-Derived Extracellular Vesicles Suppresses Inflammation and Cartilage Degradation in Osteoarthritis. Frontiers in Bioengineering and Biotechnology, 9(December), 1–12. https://doi.org/10.3389/fbioe.2021.772002.
Dong, J., Li, L., Fang, X., & Zang, M. (2021). Exosome-encapsulated microrna-127-3p released from bone marrow-derived mesenchymal stem cells alleviates osteoarthritis through regulating cdh11-mediated wnt/β-catenin pathway. Journal of Pain Research, 14, 297–310. https://doi.org/10.2147/JPR.S291472
Wang, K., Li, F., Yuan, Y., Shan, L., Cui, Y., Qu, J., & Lian, F. (2020). Synovial Mesenchymal Stem Cell-Derived EV-Packaged miR-31 Downregulates Histone Demethylase KDM2A to Prevent Knee Osteoarthritis. Molecular Therapy - Nucleic Acids, 22(37), 1078–1091. https://doi.org/10.1016/j.omtn.2020.09.014
Yan, L., Liu, G., & Wu, X. (2021). Exosomes derived from umbilical cord mesenchymal stem cells in mechanical environment show improved osteochondral activity via upregulation of LncRNA H19. Journal of Orthopaedic Translation, 26(April 2020), 111–120. https://doi.org/10.1016/j.jot.2020.03.005.
Mao, G., Zhang, Z., Hu, S., Zhang, Z., Chang, Z., Huang, Z., … Kang, Y. (2018). Exosomes derived from miR-92a-3p-overexpressing human mesenchymal stem cells enhance chondrogenesis and suppress cartilage degradation via targeting WNT5A. Stem Cell Research & Therapy, 9(1), 247. https://doi.org/10.1186/s13287-018-1004-0.
Li, S., Stöckl, S., Lukas, C., Götz, J., Herrmann, M., Federlin, M., & Grässel, S. (2020). hBMSC-Derived Extracellular Vesicles Attenuate IL-1β-Induced Catabolic Effects on OA-Chondrocytes by Regulating Pro-inflammatory Signaling Pathways. Frontiers in Bioengineering and Biotechnology, 8(December), 1–14. https://doi.org/10.3389/fbioe.2020.603598
Li, K., Yan, G., Huang, H., Zheng, M., Ma, K., Cui, X., … Zhao, J. (2022). Anti-inflammatory and immunomodulatory effects of the extracellular vesicles derived from human umbilical cord mesenchymal stem cells on osteoarthritis via M2 macrophages. Journal of Nanobiotechnology, 20(1), 38. https://doi.org/10.1186/s12951-021-01236-1.
Chen, X., Shi, Y., Xue, P., Ma, X., Li, J., & Zhang, J. (2020). Mesenchymal stem cell-derived exosomal microRNA-136-5p inhibits chondrocyte degeneration in traumatic osteoarthritis by targeting ELF3. Arthritis Research & Therapy, 22(1), 256. https://doi.org/10.1186/s13075-020-02325-6
Cavallo, C., Merli, G., Borzì, R. M., Zini, N., D’Adamo, S., Guescini, M., … Filardo, G. (2021). Small Extracellular Vesicles from adipose derived stromal cells significantly attenuate in vitro the NF-κB dependent inflammatory/catabolic environment of osteoarthritis. Scientific Reports, 11(1), 1053. https://doi.org/10.1038/s41598-020-80032-7.
Duan, A., Shen, K., Li, B., Li, C., Zhou, H., Kong, R., … Liu, F. (2021). Extracellular vesicles derived from LPS-preconditioned human synovial mesenchymal stem cells inhibit extracellular matrix degradation and prevent osteoarthritis of the knee in a mouse model. Stem Cell Research and Therapy, 12(1), 1–20. https://doi.org/10.1186/s13287-021-02507-2.
Wan, S., Bao, D., Li, J., Lin, K., Huang, Q., Li, Q., & Li, L. (2022). Extracellular Vesicles from Hypoxic Pretreated Urine-Derived Stem Cells Enhance the Proliferation and Migration of Chondrocytes by Delivering miR-26a-5p. CARTILAGE, 13(2), 194760352210774. https://doi.org/10.1177/19476035221077401
Vonk, L. A., van Dooremalen, S. F. J., Liv, N., Klumperman, J., Coffer, P. J., Saris, D. B. F., & Lorenowicz, M. J. (2018). Mesenchymal Stromal/stem Cell-derived Extracellular Vesicles Promote Human Cartilage Regeneration In Vitro. Theranostics, 8(4), 906–920. https://doi.org/10.7150/thno.20746
Wang, X., Li, Z., Cui, Y., Cui, X., Chen, C., & Wang, Z. (2021). Exosomes Isolated From Bone Marrow Mesenchymal Stem Cells Exert a Protective Effect on Osteoarthritis via lncRNA LYRM4-AS1-GRPR-miR-6515-5p. Frontiers in Cell and Developmental Biology, 9(May), 1–15. https://doi.org/10.3389/fcell.2021.644380
Wang, Y., Yu, D., Liu, Z., Zhou, F., Dai, J., Wu, B., & Zhou, J. (2017). Exosomes from embryonic mesenchymal stem cells alleviate osteoarthritis through balancing synthesis and degradation of cartilage extracellular matrix, Stem Cell Research and Therapy 8(1), 189. https://doi.org/10.1186/s13287-017-0632-0.
Search of: Conditioned medium OR exosomes OR extracellular vesicles. Retrieved January 28, 2023, from https://clinicaltrials.gov/ct2/results?cond=Osteoarthritis&term=%27conditioned+medium%27+OR+%27exosomes%27+OR+%27extracellular+vesicles%27&cntry=&state=&city=&dist=.
Funding
This research was funded by the National Science Centre based on decision no. UMO-2019/33/B/NZ5/01989.
Author information
Authors and Affiliations
Contributions
Conceptualisation, MAR and MSL; writing—original draft preparation MAR and MSL; writing—review and editing, MAR, MSL, MR, WMS and TT; visualisation, MAR; supervision TT and WMS; and funding acquisition, TT.
All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no conflicts of interest.
Ethics Approval and Consent to Participate
Not applicable.
Consent for Publication
All authors consented to publish this paper.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Rosochowicz, M.A., Lach, M.S., Richter, M. et al. Conditioned Medium – Is it an Undervalued Lab Waste with the Potential for Osteoarthritis Management?. Stem Cell Rev and Rep 19, 1185–1213 (2023). https://doi.org/10.1007/s12015-023-10517-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12015-023-10517-1