Abstract
Purpose
To investigate whether an elevated serum uric acid (SUA) level is an independent risk factor for rapid decline in renal function or new-onset chronic kidney disease (CKD) in a Chinese health checkup population.
Methods
A cohort study of 6495 Chinese individuals who underwent health checkups with normal estimated glomerular filtration rate (eGFR) at baseline was carried out from May 2011 to April 2016. Examinations included a questionnaire, physical measurements, and blood sampling. The gender-specific quartiles of blood uric acid were used to present baseline descriptive data. Rapid decline of renal function was defined as eGFR loss of > 3 mL/min/1.73 m2/year. New-onset CKD was defined as follow-up eGFR < 60 mL/min/1.73 m2 or positive proteinuria. Multivariable logistic regression was used to assess the relationship between serum uric acid and the following outcomes: rapid decline of renal function, incident CKD, and combined renal outcomes.
Results
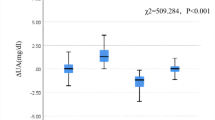
During mean follow-up of 52.8 months, 1608 (24.8%) individuals reached combined renal events. Rapid decline in renal function developed in 1506 (23.2%) individuals, and incident CKD was documented in 372 (5.7%) individuals. In a multivariate model adjusted for age, BMI, diabetes, hypertension, alcohol drinking, SBP, total cholesterol, and eGFR, the odds ratio for rapid decline of renal function increased across quartiles of serum uric acid level, reaching a 1.32 (95% CI 1.02–2.97) for the top quartile compared to the lowest quartile (P for trend < 0.001). Meanwhile, higher SUA was also associated with incident CKD in all models. Furthermore, an increased risk of reaching renal outcomes across increasing quartiles of SUA levels appeared to be similar among subgroups stratified according to age, eGFR, and SBP (P < 0.05 in all).
Conclusions
These findings suggest that higher SUA may predict progressive renal damage and dysfunction in a health checkup population in China.

Similar content being viewed by others
References
Dunkler D, Kohl M, Heinze G, Teo KK, Rosengren A, Pogue J, Gao P, Gerstein H, Yusuf S, Oberbauer R, Mann JF (2015) Modifiable lifestyle and social factors affect chronic kidney disease in high-risk individuals with type 2 diabetes mellitus. Kidney Int 87(4):784–791. https://doi.org/10.1038/ki.2014.370
Sharma SK, Ghimire A, Carminati S, Remuzzi G, Perico N (2014) Management of chronic kidney disease and its risk factors in eastern Nepal. Lancet Glob Health 2(9):e506–e507. https://doi.org/10.1016/S2214-109X(14)70281-5
Dunkler D, Kohl M, Teo KK, Heinze G, Dehghan M, Clase CM, Gao P, Yusuf S, Mann JF, Oberbauer R (2015) Dietary risk factors for incidence or progression of chronic kidney disease in individuals with type 2 diabetes in the European Union. Nephrol Dial Transplant 30(Suppl 4):iv76–iv85. https://doi.org/10.1093/ndt/gfv086
Zammit AR, Katz MJ, Derby C, Bitzer M, Lipton RB (2015) Chronic kidney disease in non-diabetic older adults: associated roles of the metabolic syndrome, inflammation, and insulin resistance. PLoS ONE 10(10):e0139369. https://doi.org/10.1371/journal.pone.0139369
Sakurai M, Kobayashi J, Takeda Y, Nagasawa SY, Yamakawa J, Moriya J, Mabuchi H, Nakagawa H (2016) sex differences in associations among obesity, metabolic abnormalities, and chronic kidney disease in Japanese men and women. J Epidemiol. https://doi.org/10.2188/jea.JE20150208
Isaka Y, Takabatake Y, Takahashi A, Saitoh T, Yoshimori T (2016) Hyperuricemia-induced inflammasome and kidney diseases. Nephrol Dial Transplant 31(6):890–896. https://doi.org/10.1093/ndt/gfv024
Li L, Yang C, Zhao Y, Zeng X, Liu F, Fu P (2014) Is hyperuricemia an independent risk factor for new-onset chronic kidney disease?: a systematic review and meta-analysis based on observational cohort studies. BMC Nephrol 15:122. https://doi.org/10.1186/1471-2369-15-122
Hisatome I, Kuwabara M (2016) Hyperuricemia plays pivotal role in progression of kidney disease. Circ J 80(8):1710–1711. https://doi.org/10.1253/circj.CJ-16-0605
Liu H, Zhang XM, Wang YL, Liu BC (2014) Prevalence of hyperuricemia among Chinese adults: a national cross-sectional survey using multistage, stratified sampling. J Nephrol 27(6):653–658. https://doi.org/10.1007/s40620-014-0082-z
Perloff D, Grim C, Flack J, Frohlich ED, Hill M, McDonald M, Morgenstern BZ (1993) Human blood pressure determination by sphygmomanometry. Circulation 88(5 Pt 1):2460–2470
Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF 3rd, Feldman HI, Kusek JW, Eggers P, Van Lente F, Greene T, Coresh J (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150(9):604–612
Cheng HT, Huang JW, Chiang CK, Yen CJ, Hung KY, Wu KD (2012) Metabolic syndrome and insulin resistance as risk factors for development of chronic kidney disease and rapid decline in renal function in elderly. J Clin Endocrinol Metab 97(4):1268–1276. https://doi.org/10.1210/jc.2011-2658
Shlipak MG, Katz R, Kestenbaum B, Siscovick D, Fried L, Newman A, Rifkin D, Sarnak MJ (2009) Rapid decline of kidney function increases cardiovascular risk in the elderly. J Am Soc Nephrol 20(12):2625–2630. https://doi.org/10.1681/ASN.2009050546
Madero M, Peralta C, Katz R, Canada R, Fried L, Najjar S, Shlipak M, Simonsick E, Lakatta E, Patel K, Rifkin D, Hawkins M, Newman A, Sarnak M (2013) Association of arterial rigidity with incident kidney disease and kidney function decline: the Health ABC study. Clin J Am Soc Nephrol 8(3):424–433. https://doi.org/10.2215/CJN.07900812
Krishnan E (2014) Interaction of inflammation, hyperuricemia, and the prevalence of hypertension among adults free of metabolic syndrome: NHANES 2009-2010. J Am Heart Assoc 3(2):e000157. https://doi.org/10.1161/JAHA.113.000157
Whelton A (2012) Hyperuricemia and hypertension: a confluence of concepts. Hypertension 60(5):1112–1113. https://doi.org/10.1161/HYPERTENSIONAHA.112.198341
Krishnan E, Pandya BJ, Chung L, Hariri A, Dabbous O (2012) Hyperuricemia in young adults and risk of insulin resistance, prediabetes, and diabetes: a 15-year follow-up study. Am J Epidemiol 176(2):108–116. https://doi.org/10.1093/aje/kws002
Rodenbach KE, Schneider MF, Furth SL, Moxey-Mims MM, Mitsnefes MM, Weaver DJ, Warady BA, Schwartz GJ (2015) Hyperuricemia and progression of CKD in children and adolescents: the chronic kidney disease in children (CKiD) cohort study. Am J Kidney Dis 66(6):984–992. https://doi.org/10.1053/j.ajkd.2015.06.015
Hsu CY, Iribarren C, McCulloch CE, Darbinian J, Go AS (2009) Risk factors for end-stage renal disease: 25-year follow-up. Arch Intern Med 169(4):342–350. https://doi.org/10.1001/archinternmed.2008.605
Zhu P, Liu Y, Han L, Xu G, Ran JM (2014) Serum uric acid is associated with incident chronic kidney disease in middle-aged populations: a meta-analysis of 15 cohort studies. PLoS ONE 9(6):e100801. https://doi.org/10.1371/journal.pone.0100801
Kim WJ, Kim SS, Bae MJ, Yi YS, Jeon YK, Kim BH, Song SH, Kim IJ, Kim YK (2014) High-normal serum uric acid predicts the development of chronic kidney disease in patients with type 2 diabetes mellitus and preserved kidney function. J Diabetes Complicat 28(2):130–134. https://doi.org/10.1016/j.jdiacomp.2013.11.006
Chonchol M, Shlipak MG, Katz R, Sarnak MJ, Newman AB, Siscovick DS, Kestenbaum B, Carney JK, Fried LF (2007) Relationship of uric acid with progression of kidney disease. Am J Kidney Dis 50(2):239–247. https://doi.org/10.1053/j.ajkd.2007.05.013
Kawashima M, Wada K, Ohta H, Terawaki H, Aizawa Y (2011) Association between asymptomatic hyperuricemia and new-onset chronic kidney disease in Japanese male workers: a long-term retrospective cohort study. BMC Nephrol 12:31. https://doi.org/10.1186/1471-2369-12-31
Soltani Z, Rasheed K, Kapusta DR, Reisin E (2013) Potential role of uric acid in metabolic syndrome, hypertension, kidney injury, and cardiovascular diseases: is it time for reappraisal? Curr Hypertens Rep 15(3):175–181. https://doi.org/10.1007/s11906-013-0344-5
Ryu ES, Kim MJ, Shin HS, Jang YH, Choi HS, Jo I, Johnson RJ, Kang DH (2013) Uric acid-induced phenotypic transition of renal tubular cells as a novel mechanism of chronic kidney disease. Am J Physiol Renal Physiol 304(5):F471–F480. https://doi.org/10.1152/ajprenal.00560.2012
Moynihan J, Moore H (2010) Endocrine system dynamics and MS epidemiology. Med Hypotheses 74(5):814–817. https://doi.org/10.1016/j.mehy.2009.12.008
Wang Y, Bao X (2013) Effects of uric acid on endothelial dysfunction in early chronic kidney disease and its mechanisms. Eur J Med Res 18:26. https://doi.org/10.1186/2047-783X-18-26
Moe OW (2010) Posing the question again: does chronic uric acid nephropathy exist? J Am Soc Nephrol 21(3):395–397. https://doi.org/10.1681/ASN.2008101115
Nagahama K, Inoue T, Kohagura K, Kinjo K, Ohya Y (2015) Associations between serum uric acid levels and the incidence of hypertension and metabolic syndrome: a 4-year follow-up study of a large screened cohort in Okinawa, Japan. Hypertens Res 38(3):213–218. https://doi.org/10.1038/hr.2014.161
Acknowledgements
This work was supported in part by a grant from the Natural Science Foundation of Hunan Province, China (2017JJ3470). We thank Chang Liu, for his help in programming and statistical analyses as well as all participants for their contribution.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee at which the studies conducted (IRB Approval Number: 2017S102).
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Cao, X., Wu, L. & Chen, Z. The association between elevated serum uric acid level and an increased risk of renal function decline in a health checkup cohort in China. Int Urol Nephrol 50, 517–525 (2018). https://doi.org/10.1007/s11255-017-1732-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-017-1732-6