Abstract
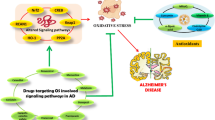
Different pathological conditions that begin with slow and progressive deformations, cause irreversible affliction by producing loss of neurons and synapses. Commonly it is referred to as ‘protein misfolding’ diseases or proteinopathies and comprises the latest definition of neurological disorders (ND). Protein misfolding dynamics, proteasomal dysfunction, aggregation, defective degradation, oxidative stress, free radical formation, mitochondrial dysfunctions, impaired bioenergetics, DNA damage, neuronal Golgi apparatus fragmentation, axonal transport disruption, Neurotrophins (NTFs) dysfunction, neuroinflammatory or neuroimmune processes, and neurohumoral changes are the several mechanisms that embark the pathogenesis of ND. Capsaicin (8-Methyl-N-vanillyl-6-nonenamide) one of the major phenolic components in chili peppers (Capsicum) distinctively triggers the unmyelinated C-fiber and acts on Transient Receptor Potential Vanilloid-1, which is a Ca2+ permeable, non-selective cation channel. Several studies have shown the neuroprotective role of capsaicin against oxidative damage, behavioral impairment, with 6-hydroxydopamine (6-OHDA) induced Parkinson's disease, pentylenetetrazol-induced seizures, global cerebral ischemia, and streptozotocin-induced Alzheimer’s disease. Based on these lines of evidence, capsaicin can be considered as a potential constituent to develop suitable neuro-pharmacotherapeutics for the management and treatment of ND. Furthermore, exploring newer horizons and carrying out proper clinical trials would help to bring out the promising effects of capsaicin to be recommended as a neuroprotectant.



Similar content being viewed by others
References
Reddy PH (2008) Mitochondrial medicine for aging and neurodegenerative diseases. Neuromolecular Med 10:291–315. https://doi.org/10.1007/s12017-008-8044-z
Golde TE, Miller VM (2009) Proteinopathy-induced neuronal senescence: a hypothesis for brain failure in Alzheimer’s and other neurodegenerative diseases. Alzheimers Res Ther 1:5. https://doi.org/10.1186/alzrt5
Uversky VN (2009) Intrinsic disorder in proteins associated with neurodegenerative diseases. Front Biosci (Landmark Ed) 14:5188–5238. https://doi.org/10.2741/3594
Muchowski PJ, Wacker JL (2005) Modulation of neurodegeneration by molecular chaperones. Nat Rev Neurosci 6:11–22. https://doi.org/10.1038/nrn1587
Dou F, Netzer WJ, Tanemura K, Li F, Hartl FU, Takashima A, Gouras GK, Greengard P, Xu H (2003) Chaperones increase association of tau protein with microtubules. Proc Natl Acad Sci U S A 100:721–726. https://doi.org/10.1073/pnas.242720499
Petrucelli L, Dickson D, Kehoe K, Taylor J, Snyder H, Grover A, De Lucia M, McGowan E, Lewis J, Prihar G, Kim J, Dillmann WH, Browne SE, Hall A, Voellmy R, Tsuboi Y, Dawson TM, Wolozin B, Hardy J, Hutton M (2004) CHIP and Hsp70 regulate tau ubiquitination, degradation and aggregation. Hum Mol Genet 13:703–714. https://doi.org/10.1093/hmg/ddh083
Shimura H, Schwartz D, Gygi SP, Kosik KS (2004) CHIP-Hsc70 complex ubiquitinates phosphorylated tau and enhances cell survival. J Biol Chem 279:4869–4876. https://doi.org/10.1074/jbc.M305838200
Klucken J, Shin Y, Masliah E, Hyman BT, McLean PJ (2004) Hsp70 reduces alpha-synuclein aggregation and toxicity. J Biol Chem 279:25497–25502. https://doi.org/10.1074/jbc.M400255200
Auluck PK, Chan HY, Trojanowski JQ, Lee VM, Bonini NM (2002) Chaperone suppression of alpha-synuclein toxicity in a Drosophila model for Parkinson’s disease. Science 295:865–868. https://doi.org/10.1126/science.1067389
Bruening W, Roy J, Giasson B, Figlewicz DA, Mushynski WE, Durham HD (2002) Up-regulation of protein chaperones preserves viability of cells expressing toxic Cu/Zn-superoxide dismutase mutants associated with amyotrophic lateral sclerosis. J Neurochem 72:693–699
Shinder GA, Lacourse MC, Minotti S, Durham HD (2001) Mutant Cu/Zn-superoxide dismutase proteins have altered solubility and interact with heat shock/stress proteins in models of amyotrophic lateral sclerosis. J Biol Chem 276:12791–12796. https://doi.org/10.1074/jbc.M010759200
Takeuchi H, Kobayashi Y, Yoshihara T, Niwa J, Doyu M, Ohtsuka K, Sobue G (2002) Hsp70 and Hsp40 improve neurite outgrowth and suppress intracytoplasmic aggregate formation in cultured neuronal cells expressing mutant SOD1. Brain Res 949:11–22. https://doi.org/10.1016/s0006-8993(02)02568-4
Auluck PK, Bonini NM (2002) Pharmacological prevention of Parkinson disease in Drosophila. Nat Med 8:1185–1186. https://doi.org/10.1038/nm1102-1185
Chai Y, Koppenhafer SL, Bonini NM, Paulson HL (1999) Analysis of the role of heat shock protein (Hsp) molecular chaperones in polyglutamine disease. J Neurosci 19:10338–10347
Jana NR, Tanaka M, Wang G, Nukina N (2000) Polyglutamine length-dependent interaction of Hsp40 and Hsp70 family chaperones with truncated N-terminal huntingtin: their role in suppression of aggregation and cellular toxicity. Hum Mol Genet 9:2009–2018. https://doi.org/10.1093/hmg/9.13.2009
Kobayashi Y, Sobue G (2001) Protective effect of chaperones on polyglutamine diseases. Brain Res Bull 56:165–168. https://doi.org/10.1016/s0361-9230(01)00593-7
Wyttenbach A, Sauvageot O, Carmichael J, Diaz-Latoud C, Arrigo AP, Rubinsztein DC (2002) Heat shock protein 27 prevents cellular polyglutamine toxicity and suppresses the increase of reactive oxygen species caused by huntingtin. Hum Mol Genet 11:1137–1151. https://doi.org/10.1093/hmg/11.9.1137
Przedborski S, Vila M, Jackson-Lewis V (2003) Neurodegeneration: what is it and where are we? J Clin Invest 111:3–10. https://doi.org/10.1172/JCI17522
Jellinger KA (2010) Basic mechanisms of neurodegeneration: a critical update. J Cell Mol Med 14:457–487. https://doi.org/10.1111/j.1582-4934.2010.01010.x
Jellinger KA (2009) Recent advances in our understanding of neurodegeneration. J Neural Transm (Vienna) 116:1111–1162. https://doi.org/10.1007/s00702-009-0240-y
Sharma SK, Vij AS, Sharma M (2013) Mechanisms and clinical uses of capsaicin. Eur J Pharmacol 720:55–62. https://doi.org/10.1016/j.ejphar.2013.10.053
Wisniewski T, Frangione B (1996) Molecular biology of brain aging and neurodegenerative disorders. Acta Neurobiol Exp (Wars) 56:267–279
Morrison JH, Hof PR (1997) Life and death of neurons in the aging brain. Science 278:412–419. https://doi.org/10.1126/science.278.5337.412
Gibb WR, Lees AJ (1989) The significance of the Lewy body in the diagnosis of idiopathic Parkinson’s disease. Neuropathol Appl Neurobiol 15:27–44. https://doi.org/10.1111/j.1365-2990.1989.tb01147.x
Anderton BH (2002) Ageing of the brain. Mech Ageing Dev 123:811–817. https://doi.org/10.1016/s0047-6374(01)00426-2
Kumar GP, Khanum F (2012) Neuroprotective potential of phytochemicals. Pharmacogn Rev 6:81–90. https://doi.org/10.4103/0973-7847.99898
Nascimento PLA, Nascimento TCE, Ramos NSM, Silva GR, Silva TMS, Moreira KA, Porto ALF (2013) Antimicrobial and antioxidant activities of Pimenta malagueta (Capsicum frutescens). Afr J Microbiol Res 7:3526–3533. https://doi.org/10.5897/AJMR2012.2401
Sia SuG, David P, Tan L, Sia SuM, Sison M, Ragragio E, Arollado EC, de Guzman T (2013) Phytochemical screening and antimicrobial activity of Capsicum frutescens Linn. crude fruit extract on selected microorganisms. J Pharm Biomed Sci 37:1922–1926
Park SY, Kim JY, Lee SM, Jun CH, Cho SB, Park CH, Joo YE, Kim HS, Choi SK, Rew JS (2014) Capsaicin induces apoptosis and modulates MAPK signaling in human gastric cancer cells. Mol Med Rep 9:499–502. https://doi.org/10.3892/mmr.2013.1849
Cho AS, Jeon SM, Kim MJ, Yeo J, Seo KI, Choi MS, Lee MK (2010) Chlorogenic acid exhibits anti-obesity property and improves lipid metabolism in high-fat diet-induced-obese mice. Food Chem Toxicol 48:937–943. https://doi.org/10.1016/j.fct.2010.01.003
Chaiyasit K, Khovidhunkit W, Wittayalertpanya S (2009) Pharmacokinetic and the effect of capsaicin in Capsicum frutescens on decreasing plasma glucose level. J Med Assoc Thai 92:108–113
Okumura T, Tsukui T, Hosokawa M, Miyashita K (2012) Effect of caffeine and capsaicin on the blood glucose levels of obese/diabetic KK-A(y) mice. J Oleo Sci 61:515–523. https://doi.org/10.5650/jos.61.515
De Lucca AJ, Boue S, Palmgren MS, Maskos K, Cleveland TE (2006) Fungicidal properties of two saponins from Capsicum frutescens and the relationship of structure and fungicidal activity. Can J Microbiol 52:336–342. https://doi.org/10.1139/w05-137
Soumya SL, Nair BR (2012) Antifungal efficacy of Capsicum frutescens L. extracts against some prevalent fungal strains associated with groundnut storage. J Agric Technol 8:739–750
Harada N, Okajima K (2009) Effects of capsaicin and isoflavone on blood pressure and serum levels of insulin-like growth factor-I in normotensive and hypertensive volunteers with alopecia. Biosci Biotechnol Biochem 73:1456–1459. https://doi.org/10.1271/bbb.80883
Patane S, Marte F, La Rosa FC, La Rocca R (2010) Capsaicin and arterial hypertensive crisis. Int J Cardiol 144:e26-27. https://doi.org/10.1016/j.ijcard.2008.12.080
Kim CS, Kawada T, Kim BS, Han IS, Choe SY, Kurata T, Yu R (2003) Capsaicin exhibits anti-inflammatory property by inhibiting IkB-a degradation in LPS-stimulated peritoneal macrophages. Cell Signal 15:299–306. https://doi.org/10.1016/s0898-6568(02)00086-4
Jolayemi AT, Ojewole JA (2013) Comparative anti-inflammatory properties of Capsaicin and ethyl-a acetate extract of Capsicum frutescens linn [Solanaceae] in rats. Afr Health Sci 13:357–361. https://doi.org/10.4314/ahs.v13i2.23
Kim Y, Lee J (2014) Anti-inflammatory activity of capsaicin and dihydrocapsaicin through heme oxygenase-1 induction in Raw264.7 macrophages. J Food Biochem 38:381–387. https://doi.org/10.1111/jfbc.12064
Hassan MH, Edfawy M, Mansour A, Hamed AA (2012) Antioxidant and antiapoptotic effects of capsaicin against carbon tetrachloride-induced hepatotoxicity in rats. Toxicol Ind Health 28:428–438. https://doi.org/10.1177/0748233711413801
Maksimova V, Koleva Gudeva L, Ruskovska T, Gulaboski R, Cvetanovska A (2014) Antioxidative effect of Capsicum oleoresins compared with pure capsaicin. IOSR Journal of Pharmacy 4:44–48
Mason L, Moore RA, Derry S, Edwards JE, McQuay HJ (2004) Systematic review of topical capsaicin for the treatment of chronic pain. BMJ 328:991. https://doi.org/10.1136/bmj.38042.506748.EE
Anand P, Bley K (2011) Topical capsaicin for pain management: therapeutic potential and mechanisms of action of the new high-concentration capsaicin 8% patch. Br J Anaesth 107:490–502. https://doi.org/10.1093/bja/aer260
Uceyler N, Sommer C (2014) High-dose capsaicin for the treatment of neuropathic pain: what we know and what we need to know. Pain Ther 3:73–84. https://doi.org/10.1007/s40122-014-0027-1
Narang N, Jiraungkoorskul W, Jamrus P (2017) current understanding of antiobesity property of capsaicin. Pharmacogn Rev 11:23–26. https://doi.org/10.4103/phrev.phrev_48_16
Fragasso G, Palloshi A, Piatti PM, Monti L, Rossetti E, Setola E, Montano C, Bassanelli G, Calori G, Margonato A (2004) Nitric-oxide mediated effects of transdermal capsaicin patches on the ischemic threshold in patients with stable coronary disease. J Cardiovasc Pharmacol 44:340–347. https://doi.org/10.1097/01.fjc.0000137161.76616.85
Patane S, Marte F, Di Bella G, Cerrito M, Coglitore S (2009) Capsaicin, arterial hypertensive crisis and acute myocardial infarction associated with high levels of thyroid stimulating hormone. Int J Cardiol 134:130–132. https://doi.org/10.1016/j.ijcard.2007.12.032
Abdel-Salam OME, Sleem AA, Hassan NS, Sharaf HA, Gy M (2006) Capsaicin ameliorates hepatic injury caused by carbon tetrachloride in the rat. J Pharmacol Toxicol 1:147–156
Mohammed F, Sultan A, Abas A (2014) Chemopreventive and therapeutic effect of capsaicin against diethylnitrosamine induced liver injury and hepatocellular carcinoma in rats. Int J Biol Pharm Res 5:630–642
Desai BS, Schneider JA, Li JL, Carvey PM, Hendey B (2009) Evidence of angiogenic vessels in Alzheimer’s disease. J Neural Transm (Vienna) 116:587–597. https://doi.org/10.1007/s00702-009-0226-9
Szolcsanyi J (2014) Capsaicin and sensory neurones: a historical perspective. Prog Drug Res 68:1–37. https://doi.org/10.1007/978-3-0348-0828-6_1
Fattori V, Hohmann MS, Rossaneis AC, Pinho-Ribeiro FA, Verri WA (2016) Capsaicin: current understanding of its mechanisms and therapy of pain and other pre-clinical and clinical uses. Molecules 21:844. https://doi.org/10.3390/molecules21070844
Pershing LK, Reilly CA, Corlett JL, Crouch DJ (2004) Effects of vehicle on the uptake and elimination kinetics of capsaicinoids in human skin in vivo. Toxicol Appl Pharmacol 200:73–81. https://doi.org/10.1016/j.taap.2004.03.019
Rollyson WD, Stover CA, Brown KC, Perry HE, Stevenson CD, McNees CA, Ball JG, Valentovic MA, Dasgupta P (2014) Bioavailability of capsaicin and its implications for drug delivery. J Control Release 196:96–105. https://doi.org/10.1016/j.jconrel.2014.09.027
Suresh D, Srinivasan K (2010) Tissue distribution & elimination of capsaicin, piperine & curcumin following oral intake in rats. Indian J Med Res 131:682–691
Chanda S, Bashir M, Babbar S, Koganti A, Bley K (2008) In vitro hepatic and skin metabolism of capsaicin. Drug Metab Dispos 36:670–675. https://doi.org/10.1124/dmd.107.019240
Kawada T, Iwai K (2014) In vivo and in vitro metabolism of dihydrocapsaicin, a pungent principle of hot pepper, in rats. Agric Biol Chem 49:441–448. https://doi.org/10.1080/00021369.1985.10866743
Pingle SC, Matta JA, Ahern GP (2007) Capsaicin receptor: TRPV1 a promiscuous TRP channel. Handb Exp Pharmacol. https://doi.org/10.1007/978-3-540-34891-7_9
Karai LJ, Russell JT, Iadarola MJ, Olah Z (2004) Vanilloid receptor 1 regulates multiple calcium compartments and contributes to Ca2+-induced Ca2+ release in sensory neurons. J Biol Chem 279:16377–16387. https://doi.org/10.1074/jbc.M310891200
Liu M, Liu MC, Magoulas C, Priestley JV, Willmott NJ (2003) Versatile regulation of cytosolic Ca2+ by vanilloid receptor I in rat dorsal root ganglion neurons. J Biol Chem 278:5462–5472. https://doi.org/10.1074/jbc.M209111200
Caterina MJ, Schumacher MA, Tominaga M, Rosen TA, Levine JD, Julius D (1997) The capsaicin receptor: a heat-activated ion channel in the pain pathway. Nature 389:816–824. https://doi.org/10.1038/39807
Cortright DN, Szallasi A (2004) Biochemical pharmacology of the vanilloid receptor TRPV1. An update. Eur J Biochem 271:1814–1819. https://doi.org/10.1111/j.1432-1033.2004.04082.x
Tominaga M, Tominaga T (2005) Structure and function of TRPV1. Pflugers Arch 451:143–150. https://doi.org/10.1007/s00424-005-1457-8
Mozsik G, Szolcsanyi J, Racz I (2005) Gastroprotection induced by capsaicin in healthy human subjects. World J Gastroenterol 11:5180–5184. https://doi.org/10.3748/wjg.v11.i33.5180
Szolcsanyi J (1990) Effect of capsaicin, resiniferatoxin and piperine on ethanol-induced gastric ulcer of the rat. Acta Physiol Hung 75(Suppl):267–268
Bevan S, Szolcsanyi J (1990) Sensory neuron-specific actions of capsaicin: mechanisms and applications. Trends Pharmacol Sci 11:330–333. https://doi.org/10.1016/0165-6147(90)90237-3
Nair AB, Jacob S (2016) A simple practice guide for dose conversion between animals and human. J Basic Clin Pharm 7:27–31. https://doi.org/10.4103/0976-0105.177703
Kivipelto M, Mangialasche F, Ngandu T (2018) Lifestyle interventions to prevent cognitive impairment, dementia and Alzheimer disease. Nat Rev Neurol 14:653–666. https://doi.org/10.1038/s41582-018-0070-3
Miller G (2012) Alzheimer’s research. Stopping Alzheimer’s before it starts Science 337:790–792. https://doi.org/10.1126/science.337.6096.790
Murphy MP, LeVine H 3rd (2010) Alzheimer’s disease and the amyloid-beta peptide. J Alzheimers Dis 19:311–323. https://doi.org/10.3233/JAD-2010-1221
Pogue AI, Lukiw WJ (2004) Angiogenic signaling in Alzheimer’s disease. NeuroReport 15:1507–1510. https://doi.org/10.1097/01.wnr.0000130539.39937.1d
Shibuya M (2009) Brain angiogenesis in developmental and pathological processes: therapeutic aspects of vascular endothelial growth factor. FEBS J 276:4636–4643. https://doi.org/10.1111/j.1742-4658.2009.07175.x
Tarkowski E, Issa R, Sjogren M, Wallin A, Blennow K, Tarkowski A, Kumar P (2002) Increased intrathecal levels of the angiogenic factors VEGF and TGF-beta in Alzheimer’s disease and vascular dementia. Neurobiol Aging 23:237–243. https://doi.org/10.1016/s0197-4580(01)00285-8
Min JK, Han KY, Kim EC, Kim YM, Lee SW, Kim OH, Kim KW, Gho YS, Kwon YG (2004) Capsaicin inhibits in vitro and in vivo angiogenesis. Cancer Res 64:644–651. https://doi.org/10.1158/0008-5472.can-03-3250
Shalaby MA, Nounou HA, Deif MM (2019) The potential value of capsaicin in modulating cognitive functions in a rat model of streptozotocin-induced Alzheimer’s disease. Egypt J Neurol Psychiatry Neurosurg 55:48. https://doi.org/10.1186/s41983-019-0094-7
Cuadrado-Tejedor M, Ricobaraza A, Frechilla D, Franco R, Perez-Mediavilla A, Garcia-Osta A (2012) Chronic mild stress accelerates the onset and progression of the Alzheimer’s disease phenotype in Tg2576 mice. J Alzheimers Dis 28:567–578. https://doi.org/10.3233/JAD-2011-110572
Rothman SM, Herdener N, Camandola S, Texel SJ, Mughal MR, Cong WN, Martin B, Mattson MP (2012) 3xTgAD mice exhibit altered behavior and elevated Abeta after chronic mild social stress. Neurobiol Aging 33(830):e831–e812. https://doi.org/10.1016/j.neurobiolaging.2011.07.005
Li HB, Mao RR, Zhang JC, Yang Y, Cao J, Xu L (2008) Antistress effect of TRPV1 channel on synaptic plasticity and spatial memory. Biol Psychiatry 64:286–292. https://doi.org/10.1016/j.biopsych.2008.02.020
Pakaski M, Hugyecz M, Santha P, Jancso G, Bjelik A, Domokos A, Janka Z, Kalman J (2009) Capsaicin promotes the amyloidogenic route of brain amyloid precursor protein processing. Neurochem Int 54:426–430. https://doi.org/10.1016/j.neuint.2009.01.012
Jiang X, Jia LW, Li XH, Cheng XS, Xie JZ, Ma ZW, Xu WJ, Liu Y, Yao Y, Du LL, Zhou XW (2013) Capsaicin ameliorates stress-induced Alzheimer’s disease-like pathological and cognitive impairments in rats. J Alzheimers Dis 35:91–105. https://doi.org/10.3233/JAD-121837
Kang JH, Goto T, Han IS, Kawada T, Kim YM, Yu R (2010) Dietary capsaicin reduces obesity-induced insulin resistance and hepatic steatosis in obese mice fed a high-fat diet. Obesity (Silver Spring) 18:780–787. https://doi.org/10.1038/oby.2009.301
Chen J, Li L, Li Y, Liang X, Sun Q, Yu H, Zhong J, Ni Y, Chen J, Zhao Z, Gao P, Wang B, Liu D, Zhu Z, Yan Z (2015) Activation of TRPV1 channel by dietary capsaicin improves visceral fat remodeling through connexin43-mediated Ca2+ influx. Cardiovasc Diabetol 14:22. https://doi.org/10.1186/s12933-015-0183-6
Wang P, Yan Z, Zhong J, Chen J, Ni Y, Li L, Ma L, Zhao Z, Liu D, Zhu Z (2012) Transient receptor potential vanilloid 1 activation enhances gut glucagon-like peptide-1 secretion and improves glucose homeostasis. Diabetes 61:2155–2165. https://doi.org/10.2337/db11-1503
Akiba Y, Kato S, Katsube K, Nakamura M, Takeuchi K, Ishii H, Hibi T (2004) Transient receptor potential vanilloid subfamily 1 expressed in pancreatic islet beta cells modulates insulin secretion in rats. Biochem Biophys Res Commun 321:219–225. https://doi.org/10.1016/j.bbrc.2004.06.149
Liu Y, Liu F, Grundke-Iqbal I, Iqbal K, Gong CX (2011) Deficient brain insulin signalling pathway in Alzheimer’s disease and diabetes. J Pathol 225:54–62. https://doi.org/10.1002/path.2912
de la Monte SM (2012) Brain insulin resistance and deficiency as therapeutic targets in Alzheimer’s disease. Curr Alzheimer Res 9:35–66. https://doi.org/10.2174/156720512799015037
Xu W, Yang Y, Yuan G, Zhu W, Ma D, Hu S (2015) Exendin-4, a glucagon-like peptide-1 receptor agonist, reduces Alzheimer disease-associated tau hyperphosphorylation in the hippocampus of rats with type 2 diabetes. J Investig Med 63:267–272. https://doi.org/10.1097/JIM.0000000000000129
Yang Y, Ma D, Wang Y, Jiang T, Hu S, Zhang M, Yu X, Gong CX (2013) Intranasal insulin ameliorates tau hyperphosphorylation in a rat model of type 2 diabetes. J Alzheimers Dis 33:329–338. https://doi.org/10.3233/JAD-2012-121294
Yang HJ, Kwon DY, Kim MJ, Kang S, Moon NR, Daily JW, Park S (2015) Red peppers with moderate and severe pungency prevent the memory deficit and hepatic insulin resistance in diabetic rats with Alzheimer’s disease. Nutr Metab (Lond) 12:9. https://doi.org/10.1186/s12986-015-0005-6
Hwang E, Lee TH, Lee WJ, Shim WS, Yeo EJ, Kim S, Kim SY (2016) A novel synthetic Piper amide derivative NED-180 inhibits hyperpigmentation by activating the PI3K and ERK pathways and by regulating Ca2+ influx via TRPM1 channels. Pigment Cell Melanoma Res 29:81–91. https://doi.org/10.1111/pcmr.12430
Zhang Y, Zhang T, Wu C, Xia Q, Xu D (2017) ASIC1a mediates the drug resistance of human hepatocellular carcinoma via the Ca(2+)/PI3-kinase/AKT signaling pathway. Lab Invest 97:53–69. https://doi.org/10.1038/labinvest.2016.127
Wang Y, Ali Y, Lim CY, Hong W, Pang ZP, Han W (2014) Insulin-stimulated leptin secretion requires calcium and PI3K/Akt activation. Biochem J 458:491–498. https://doi.org/10.1042/BJ20131176
Xu W, Liu J, Ma D, Yuan G, Lu Y, Yang Y (2017) Capsaicin reduces Alzheimer-associated tau changes in the hippocampus of type 2 diabetes rats. PLoS ONE 12:e0172477. https://doi.org/10.1371/journal.pone.0172477
Garcia-Alloza M, Borrelli LA, Rozkalne A, Hyman BT, Bacskai BJ (2007) Curcumin labels amyloid pathology in vivo, disrupts existing plaques, and partially restores distorted neurites in an Alzheimer mouse model. J Neurochem 102:1095–1104. https://doi.org/10.1111/j.1471-4159.2007.04613.x
Yang F, Lim GP, Begum AN, Ubeda OJ, Simmons MR, Ambegaokar SS, Chen PP, Kayed R, Glabe CG, Frautschy SA, Cole GM (2005) Curcumin inhibits formation of amyloid beta oligomers and fibrils, binds plaques, and reduces amyloid in vivo. J Biol Chem 280:5892–5901. https://doi.org/10.1074/jbc.M404751200
Dairam A, Fogel R, Daya S, Limson JL (2008) Antioxidant and iron-binding properties of curcumin, capsaicin, and S-allylcysteine reduce oxidative stress in rat brain homogenate. J Agric Food Chem 56:3350–3356. https://doi.org/10.1021/jf0734931
Liu CH, Bu XL, Wang J, Zhang T, Xiang Y, Shen LL, Wang QH, Deng B, Wang X, Zhu C, Yao XQ, Zhang M, Zhou HD, Wang YJ (2016) The associations between a capsaicin-rich diet and blood amyloid-beta levels and cognitive function. J Alzheimers Dis 52:1081–1088. https://doi.org/10.3233/JAD-151079
Selkoe DJ, Hardy J (2016) The amyloid hypothesis of Alzheimer’s disease at 25 years. EMBO Mol Med 8:595–608
Hardy J, Selkoe DJ (2002) The amyloid hypothesis of Alzheimer’s disease: progress and problems on the road to therapeutics. Science 297:353–356. https://doi.org/10.1126/science.1072994
Postina R, Schroeder A, Dewachter I, Bohl J, Schmitt U, Kojro E, Prinzen C, Endres K, Hiemke C, Blessing M, Flamez P, Dequenne A, Godaux E, van Leuven F, Fahrenholz F (2004) A disintegrin-metalloproteinase prevents amyloid plaque formation and hippocampal defects in an Alzheimer disease mouse model. J Clin Invest 113:1456–1464. https://doi.org/10.1172/JCI20864
Kuhn PH, Wang H, Dislich B, Colombo A, Zeitschel U, Ellwart JW, Kremmer E, Rossner S, Lichtenthaler SF (2010) ADAM10 is the physiologically relevant, constitutive alpha-secretase of the amyloid precursor protein in primary neurons. EMBO J 29:3020–3032. https://doi.org/10.1038/emboj.2010.167
Jorissen E, Prox J, Bernreuther C, Weber S, Schwanbeck R, Serneels L, Snellinx A, Craessaerts K, Thathiah A, Tesseur I, Bartsch U, Weskamp G, Blobel CP, Glatzel M, De Strooper B, Saftig P (2010) The disintegrin/metalloproteinase ADAM10 is essential for the establishment of the brain cortex. J Neurosci 30:4833–4844. https://doi.org/10.1523/JNEUROSCI.5221-09.2010
Wang J, Sun BL, Xiang Y, Tian DY, Zhu C, Li WW, Liu YH, Bu XL, Shen LL, Jin WS, Wang Z, Zeng GH, Xu W, Chen LY, Chen XW, Hu Z, Zhu ZM, Song W, Zhou HD, Yu JT, Wang YJ (2020) Capsaicin consumption reduces brain amyloid-beta generation and attenuates Alzheimer’s disease-type pathology and cognitive deficits in APP/PS1 mice. Transl Psychiatry 10:230. https://doi.org/10.1038/s41398-020-00918-y
Shi Z, El-Obeid T, Riley M, Li M, Page A, Liu J (2019) High chili intake and cognitive function among 4582 adults: an open cohort study over 15 years. Nutrients. https://doi.org/10.3390/nu11051183
Braak H, Del Tredici K, Rub U, de Vos RA, Jansen Steur EN, Braak E (2003) Staging of brain pathology related to sporadic Parkinson’s disease. Neurobiol Aging 24:197–211. https://doi.org/10.1016/s0197-4580(02)00065-9
Kalia LV, Lang AE (2015) Parkinson’s disease. Lancet 386:896–912. https://doi.org/10.1016/S0140-6736(14)61393-3
Athauda D, Foltynie T (2015) The ongoing pursuit of neuroprotective therapies in Parkinson disease. Nat Rev Neurol 11:25–40. https://doi.org/10.1038/nrneurol.2014.226
Lindholm D, Makela J, Di Liberto V, Mudo G, Belluardo N, Eriksson O, Saarma M (2016) Current disease modifying approaches to treat Parkinson’s disease. Cell Mol Life Sci 73:1365–1379. https://doi.org/10.1007/s00018-015-2101-1
Morgese MG, Cassano T, Cuomo V, Giuffrida A (2007) Anti-dyskinetic effects of cannabinoids in a rat model of Parkinson’s disease: role of CB(1) and TRPV1 receptors. Exp Neurol 208:110–119. https://doi.org/10.1016/j.expneurol.2007.07.021
Gonzalez-Aparicio R, Moratalla R (2014) Oleoylethanolamide reduces L-DOPA-induced dyskinesia via TRPV1 receptor in a mouse model of Parkinson s disease. Neurobiol Dis 62:416–425. https://doi.org/10.1016/j.nbd.2013.10.008
Zhao Z, Wang J, Wang L, Yao X, Liu Y, Li Y, Chen S, Yue T, Wang X, Yu W, Liu Y (2017) Capsaicin protects against oxidative insults and alleviates behavioral deficits in rats with 6-OHDA-induced Parkinson’s disease via activation of TRPV1. Neurochem Res 42:3431–3438. https://doi.org/10.1007/s11064-017-2388-4
Nagatsu T, Sawada M (2006) Cellular and molecular mechanisms of Parkinson’s disease: neurotoxins, causative genes, and inflammatory cytokines. Cell Mol Neurobiol 26:781–802. https://doi.org/10.1007/s10571-006-9061-9
Park ES, Kim SR, Jin BK (2012) Transient receptor potential vanilloid subtype 1 contributes to mesencephalic dopaminergic neuronal survival by inhibiting microglia-originated oxidative stress. Brain Res Bull 89:92–96. https://doi.org/10.1016/j.brainresbull.2012.07.001
Lee TH, Lee JG, Yon JM, Oh KW, Baek IJ, Nahm SS, Lee BJ, Yun YW, Nam SY (2011) Capsaicin prevents kainic acid-induced epileptogenesis in mice. Neurochem Int 58:634–640. https://doi.org/10.1016/j.neuint.2011.01.027
Chung YC, Kim YS, Bok E, Yune TY, Maeng S, Jin BK (2013) MMP-3 contributes to nigrostriatal dopaminergic neuronal loss, BBB damage, and neuroinflammation in an MPTP mouse model of Parkinson’s disease. Mediators Inflamm 2013:370526. https://doi.org/10.1155/2013/370526
Bai L, Zhang X, Li X, Liu N, Lou F, Ma H, Luo X, Ren Y (2015) Somatostatin prevents lipopolysaccharide-induced neurodegeneration in the rat substantia nigra by inhibiting the activation of microglia. Mol Med Rep 12:1002–1008. https://doi.org/10.3892/mmr.2015.3494
Ji KA, Yang MS, Jeong HK, Min KJ, Kang SH, Jou I, Joe EH (2007) Resident microglia die and infiltrated neutrophils and monocytes become major inflammatory cells in lipopolysaccharide-injected brain. Glia 55:1577–1588. https://doi.org/10.1002/glia.20571
Gray MT, Woulfe JM (2015) Striatal blood-brain barrier permeability in Parkinson’s disease. J Cereb Blood Flow Metab 35:747–750. https://doi.org/10.1038/jcbfm.2015.32
Hernandez-Romero MC, Delgado-Cortes MJ, Sarmiento M, de Pablos RM, Espinosa-Oliva AM, Arguelles S, Bandez MJ, Villaran RF, Maurino R, Santiago M, Venero JL, Herrera AJ, Cano J, Machado A (2012) Peripheral inflammation increases the deleterious effect of CNS inflammation on the nigrostriatal dopaminergic system. Neurotoxicology 33:347–360. https://doi.org/10.1016/j.neuro.2012.01.018
Bok E, Chung YC, Kim KS, Baik HH, Shin WH, Jin BK (2018) Modulation of M1/M2 polarization by capsaicin contributes to the survival of dopaminergic neurons in the lipopolysaccharide-lesioned substantia nigra in vivo. Exp Mol Med 50:1–14. https://doi.org/10.1038/s12276-018-0111-4
Marinelli S, Di Marzo V, Berretta N, Matias I, Maccarrone M, Bernardi G, Mercuri NB (2003) Presynaptic facilitation of glutamatergic synapses to dopaminergic neurons of the rat substantia nigra by endogenous stimulation of vanilloid receptors. J Neurosci 23:3136–3144
de Lago E, de Miguel R, Lastres-Becker I, Ramos JA, Fernandez-Ruiz J (2004) Involvement of vanilloid-like receptors in the effects of anandamide on motor behavior and nigrostriatal dopaminergic activity: in vivo and in vitro evidence. Brain Res 1007:152–159. https://doi.org/10.1016/j.brainres.2004.02.016
Di Marzo V, Lastres-Becker I, Bisogno T, De Petrocellis L, Milone A, Davis JB, Fernandez-Ruiz JJ (2001) Hypolocomotor effects in rats of capsaicin and two long chain capsaicin homologues. Eur J Pharmacol 420:123–131. https://doi.org/10.1016/s0014-2999(01)01012-3
Lee J, Di Marzo V, Brotchie JM (2006) A role for vanilloid receptor 1 (TRPV1) and endocannabinnoid signalling in the regulation of spontaneous and L-DOPA induced locomotion in normal and reserpine-treated rats. Neuropharmacology 51:557–565. https://doi.org/10.1016/j.neuropharm.2006.04.016
Choi SH, Lee DY, Chung ES, Hong YB, Kim SU, Jin BK (2005) Inhibition of thrombin-induced microglial activation and NADPH oxidase by minocycline protects dopaminergic neurons in the substantia nigra in vivo. J Neurochem 95:1755–1765. https://doi.org/10.1111/j.1471-4159.2005.03503.x
Choi SH, Lee DY, Kim SU, Jin BK (2005) Thrombin-induced oxidative stress contributes to the death of hippocampal neurons in vivo: role of microglial NADPH oxidase. J Neurosci 25:4082–4090. https://doi.org/10.1523/JNEUROSCI.4306-04.2005
McGeer PL, McGeer EG (2008) Glial reactions in Parkinson’s disease. Mov Disord 23:474–483. https://doi.org/10.1002/mds.21751
Mirza B, Hadberg H, Thomsen P, Moos T (2000) The absence of reactive astrocytosis is indicative of a unique inflammatory process in Parkinson’s disease. Neuroscience 95:425–432. https://doi.org/10.1016/s0306-4522(99)00455-8
Chung YC, Kim SR, Jin BK (2010) Paroxetine prevents loss of nigrostriatal dopaminergic neurons by inhibiting brain inflammation and oxidative stress in an experimental model of Parkinson’s disease. J Immunol 185:1230–1237. https://doi.org/10.4049/jimmunol.1000208
Huh SH, Chung YC, Piao Y, Jin MY, Son HJ, Yoon NS, Hong JY, Pak YK, Kim YS, Hong JK, Hwang O, Jin BK (2011) Ethyl pyruvate rescues nigrostriatal dopaminergic neurons by regulating glial activation in a mouse model of Parkinson’s disease. J Immunol 187:960–969. https://doi.org/10.4049/jimmunol.1100009
Vroon A, Drukarch B, Bol JG, Cras P, Breve JJ, Allan SM, Relton JK, Hoogland PV, Van Dam AM (2007) Neuroinflammation in Parkinson’s patients and MPTP-treated mice is not restricted to the nigrostriatal system: microgliosis and differential expression of interleukin-1 receptors in the olfactory bulb. Exp Gerontol 42:762–771. https://doi.org/10.1016/j.exger.2007.04.010
Chung YC, Baek JY, Kim SR, Ko HW, Bok E, Shin WH, Won SY, Jin BK (2017) Capsaicin prevents degeneration of dopamine neurons by inhibiting glial activation and oxidative stress in the MPTP model of Parkinson’s disease. Exp Mol Med 49:e298. https://doi.org/10.1038/emm.2016.159
Abdel-Salam OME, Sleem A, Youness ER, Yassen NNY, Shaffie N, El-Toumy SA (2018) Capsicum protects against rotenone-induced toxicity in mice brain via reduced oxidative stress and 5-lipoxygenase activation. J Pharm Pharmacol Res 2:060075
Ara G, Afzal M, Jyoti S, Siddique YH (2017) Effect of myricetin on the oxidative stress markers in the brain of transgenic flies expressing human alpha-synuclein. International Journal of Nutrition, Pharmacology, Neurological Diseases 7:101–106
Rekha KR, Selvakumar GP, Sethupathy S, Santha K, Sivakamasundari RI (2013) Geraniol ameliorates the motor behavior and neurotrophic factors inadequacy in MPTP-induced mice model of Parkinson’s disease. J Mol Neurosci 51:851–862. https://doi.org/10.1007/s12031-013-0074-9
Siddique YH, Naz F, Jyoti S, Ali F, Fatima A, Rahul KS (2016) Protective effect of Geraniol on the transgenic Drosophila model of Parkinson’s disease. Environ Toxicol Pharmacol 43:225–231. https://doi.org/10.1016/j.etap.2016.03.018
Siddique YH, Naz F, Jyoti S (2018) Effect of capsaicin on the oxidative stress and dopamine content in the transgenic Drosophila model of Parkinson’s disease. Acta Biol Hung 69:115–124. https://doi.org/10.1556/018.69.2018.2.1
de Boer HM, Mula M, Sander JW (2008) The global burden and stigma of epilepsy. Epilepsy Behav 12:540–546. https://doi.org/10.1016/j.yebeh.2007.12.019
Rowley S, Patel M (2013) Mitochondrial involvement and oxidative stress in temporal lobe epilepsy. Free Radic Biol Med 62:121–131. https://doi.org/10.1016/j.freeradbiomed.2013.02.002
Geronzi U, Lotti F, Grosso S (2018) Oxidative stress in epilepsy. Expert Rev Neurother 18:427–434. https://doi.org/10.1080/14737175.2018.1465410
Skovronsky DM, Lee VM, Trojanowski JQ (2006) Neurodegenerative diseases: new concepts of pathogenesis and their therapeutic implications. Annu Rev Pathol 1:151–170. https://doi.org/10.1146/annurev.pathol.1.110304.100113
Abdel-Salam OME, Sleem AA, Sayed M, Youness ER, Shaffie N (2020) Capsaicin exerts anti-convulsant and neuroprotective effects in pentylenetetrazole-induced seizures. Neurochem Res 45:1045–1061. https://doi.org/10.1007/s11064-020-02979-3
Pezzoli M, Elhamdani A, Camacho S, Meystre J, Gonzalez SM, le Coutre J, Markram H (2014) Dampened neural activity and abolition of epileptic-like activity in cortical slices by active ingredients of spices. Sci Rep 4:6825. https://doi.org/10.1038/srep06825
Heinemann U, Draguhn A, Ficker E, Stabel J, Zhang CL (1994) Strategies for the development of drugs for pharmacoresistant epilepsies. Epilepsia 35(Suppl 5):S10-21. https://doi.org/10.1111/j.1528-1157.1994.tb05959.x
Fujikawa DG (2005) Prolonged seizures and cellular injury: understanding the connection. Epilepsy Behav 7(Suppl 3):S3-11. https://doi.org/10.1016/j.yebeh.2005.08.003
Pegorini S, Braida D, Verzoni C, Guerini-Rocco C, Consalez GG, Croci L, Sala M (2005) Capsaicin exhibits neuroprotective effects in a model of transient global cerebral ischemia in Mongolian gerbils. Br J Pharmacol 144:727–735. https://doi.org/10.1038/sj.bjp.0706115
Huang M, Cheng G, Tan H, Qin R, Zou Y, Wang Y, Zhang Y (2017) Capsaicin protects cortical neurons against ischemia/reperfusion injury via down-regulating NMDA receptors. Exp Neurol 295:66–76. https://doi.org/10.1016/j.expneurol.2017.05.001
Chiang H, Ohno N, Hsieh YL, Mahad DJ, Kikuchi S, Komuro H, Hsieh ST, Trapp BD (2015) Mitochondrial fission augments capsaicin-induced axonal degeneration. Acta Neuropathol 129:81–96. https://doi.org/10.1007/s00401-014-1354-3
Harry GJ, Kraft AD (2008) Neuroinflammation and microglia: considerations and approaches for neurotoxicity assessment. Expert Opin Drug Metab Toxicol 4:1265–1277. https://doi.org/10.1517/17425255.4.10.1265
Hwang MK, Bode AM, Byun S, Song NR, Lee HJ, Lee KW, Dong Z (2010) Cocarcinogenic effect of capsaicin involves activation of EGFR signaling but not TRPV1. Cancer Res 70:6859–6869. https://doi.org/10.1158/0008-5472.CAN-09-4393
Li T, Wang G, Hui VCC, Saad D, de Sousa VJ, La Montanara P, Nagy I (2021) TRPV1 feed-forward sensitisation depends on COX2 upregulation in primary sensory neurons. Sci Rep 11:3514. https://doi.org/10.1038/s41598-021-82829-6
Bhatia HS, Roelofs N, Munoz E, Fiebich BL (2017) Alleviation of microglial activation induced by p38 MAPK/MK2/PGE2 axis by capsaicin: potential involvement of other than TRPV1 mechanism/s. Sci Rep 7:116. https://doi.org/10.1038/s41598-017-00225-5
Lu CW, Lin TY, Hsie TY, Huang SK, Wang SJ (2017) Capsaicin presynaptically inhibits glutamate release through the activation of TRPV1 and calcineurin in the hippocampus of rats. Food Funct 8:1859–1868. https://doi.org/10.1039/c7fo00011a
Lee JG, Yon JM, Lin C, Jung AY, Jung KY, Nam SY (2012) Combined treatment with capsaicin and resveratrol enhances neuroprotection against glutamate-induced toxicity in mouse cerebral cortical neurons. Food Chem Toxicol 50:3877–3885. https://doi.org/10.1016/j.fct.2012.08.040
Liu J, Liu H, Zhao Z, Wang J, Guo D, Liu Y (2020) Regulation of Actg1 and Gsta2 is possible mechanism by which capsaicin alleviates apoptosis in cell model of 6-OHDA-induced Parkinson’s disease. Biosci Rep. https://doi.org/10.1042/BSR20191796
Sun Q, Wang Y, Zhang Y, Liu F, Cheng X, Hou N, Zhao X, Yang X (2007) Expression profiling reveals dysregulation of cellular cytoskeletal genes in HBx-induced hepatocarcinogenesis. Cancer Biol Ther 6:668–674. https://doi.org/10.4161/cbt.6.5.3955
Bunnell TM, Ervasti JM (2010) Delayed embryonic development and impaired cell growth and survival in Actg1 null mice. Cytoskeleton (Hoboken) 67:564–572. https://doi.org/10.1002/cm.20467
Kang KW, Lee SJ, Kim SG (2005) Molecular mechanism of nrf2 activation by oxidative stress. Antioxid Redox Signal 7:1664–1673. https://doi.org/10.1089/ars.2005.7.1664
Nagabhushan M, Bhide SV (1985) Mutagenicity of chili extract and capsaicin in short-term tests. Environ Mutagen 7:881–888. https://doi.org/10.1002/em.2860070609
Malagarie-Cazenave S, Olea-Herrero N, Vara D, Diaz-Laviada I (2009) Capsaicin, a component of red peppers, induces expression of androgen receptor via PI3K and MAPK pathways in prostate LNCaP cells. FEBS Lett 583:141–147. https://doi.org/10.1016/j.febslet.2008.11.038
Hoch-Ligeti C (1951) Production of liver tumours by dietary means; effect of feeding chilies [Capsicum frutescens and annuum (Linn.)] to rats. Acta Unio Int Contra Cancrum 7:606–611
Toth B, Gannett P (1992) Carcinogenicity of lifelong administration of capsaicin of hot pepper in mice. In Vivo 6:59–63
Agrawal RC, Wiessler M, Hecker E, Bhide SV (1986) Tumour-promoting effect of chilli extract in BALB/c mice. Int J Cancer 38:689–695. https://doi.org/10.1002/ijc.2910380512
Kim JP, Park JG, Lee MD, Han MD, Park ST, Lee BH, Jung SE (1985) Co-carcinogenic effects of several Korean foods on gastric cancer induced by N-methyl-N’-nitro-N-nitrosoguanidine in rats. Jpn J Surg 15:427–437. https://doi.org/10.1007/BF02470087
Erin N, Boyer PJ, Bonneau RH, Clawson GA, Welch DR (2004) Capsaicin-mediated denervation of sensory neurons promotes mammary tumor metastasis to lung and heart. Anticancer Res 24:1003–1009
Lopez-Carrillo L, Hernandez Avila M, Dubrow R (1994) Chili pepper consumption and gastric cancer in Mexico: a case-control study. Am J Epidemiol 139:263–271. https://doi.org/10.1093/oxfordjournals.aje.a116993
Notani PN, Jayant K (1987) Role of diet in upper aerodigestive tract cancers. Nutr Cancer 10:103–113. https://doi.org/10.1080/01635588709513945
Archer VE, Jones DW (2002) Capsaicin pepper, cancer and ethnicity. Med Hypotheses 59:450–457. https://doi.org/10.1016/s0306-9877(02)00152-4
Graham DY, Smith JL, Opekun AR (1988) Spicy food and the stomach. Evaluation by videoendoscopy. JAMA 260:3473–3475
Williams SR, Clark RF, Dunford JV (1995) Contact dermatitis associated with capsaicin: hunan hand syndrome. Ann Emerg Med 25:713–715. https://doi.org/10.1016/s0196-0644(95)70188-5
Kim-Katz SY, Anderson IB, Kearney TE, MacDougall C, Hudmon KS, Blanc PD (2010) Topical antacid therapy for capsaicin-induced dermal pain: a poison center telephone-directed study. Am J Emerg Med 28:596–602. https://doi.org/10.1016/j.ajem.2009.02.007
Acknowledgements
ST is thankful to the Indian Council of Medical Research (ICMR) for the Senior Research Fellowship for the ongoing Doctoral Program at DPSRU. Acknowledgments are due to DPSRU, Govt. of NCT of Delhi for needful infrastructure facility and support to the authors.
Author information
Authors and Affiliations
Contributions
All authors have equal contributions in the concept of review and writing the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors confirm that this article's content has no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tyagi, S., Shekhar, N. & Thakur, A.K. Protective Role of Capsaicin in Neurological Disorders: An Overview. Neurochem Res 47, 1513–1531 (2022). https://doi.org/10.1007/s11064-022-03549-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-022-03549-5