Abstract
Objective
Focal stereotactic radiosurgery to the surgical cavity lowers local recurrence after resection of brain metastases (BM). To evaluate local control (LC) and brain disease control (BDC) after intraoperative radiotherapy (IORT) for resected BM.
Methods
Adult patients with completely resected single supratentorial BM were recruited and underwent IORT to the cavity with a prescribed dose of 18 Gy to 1 mm-depth. Primary endpoints were actuarial LC and BDC. Local failure (LF) and distant brain failure (DBF), with death as a competing risk, were estimated. Secondary endpoints were overall survival (OS) and incidence of radiation necrosis (RN). Simon’s two-stage design was used and estimated an accrual of 10 patients for the first-stage analysis and a LC higher than 63% to proceed to second stage. We report the final analysis of the first stage.
Results
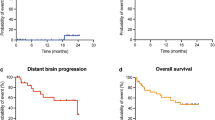
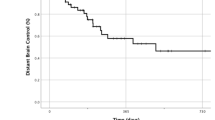
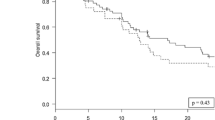
Between June 2019 to November 2020, 10 patients were accrued. Median clinical and imaging FU was 11.2 and 9.7 months, respectively. Median LC was not reached and median BDC was 5 months. The 6-month and 12-month LC was 87.5%. The 6-month and 12-month BDC was 39% and 13%, respectively. Incidence of LF at 6 and 12 months was 10% and of DBF at 6 and 12 months was 50% and 70%, respectively. Median OS was not reached. The 6-month and 12-month OS was 80%. One patient had asymptomatic RN.
Conclusion
IORT for completely resected BM is associated with a potential high local control and low risk of RN, reaching the pre-specified criteria to proceed to second stage and warranting further studies.


Similar content being viewed by others
References
Sperduto PW, Mesko S, Li J et al (2020) Survival in patients with brain metastases: report on the updated diagnosis-specific graded Prognostic Assessment and Definition of the eligibility quotient. J Clin Oncol 38(32):3773–3784
Chang EL, Wefel JS, Hess KR et al (2009) Neurocognition in patients with brain metastases treated with radiosurgery or radiosurgery plus whole-brain irradiation: a randomised controlled trial. Lancet Oncol 10(11):1037–1044
Brown PD, Jaeckle K, Ballman KV et al (2016) Effect of radiosurgery alone vs radiosurgery with whole brain radiation therapy on cognitive function in patients with 1 to 3 brain metastases: a randomized clinical trial. JAMA 316(4):401–409
Mahajan A, Ahmed S, McAleer MF et al (2017) Post-operative stereotactic radiosurgery versus observation for completely resected brain metastases: a single-centre, randomised, controlled, phase 3 trial. Lancet Oncol 18(8):1040–1048
Brown PD, Ballman KV, Cerhan JH et al (2017) Postoperative stereotactic radiosurgery compared with whole brain radiotherapy for resected metastatic brain disease (NCCTG N107C/CEC.3): a multicentre, randomised, controlled, phase 3 trial. Lancet Oncol 18(8):1049–1060
Weil RJ, Mavinkurve GG, Chao ST et al (2015) Intraoperative radiotherapy to treat newly diagnosed solitary brain metastasis: initial experience and long-term outcomes. J Neurosurg 122(4):825–832
Cifarelli CP, Brehmer S, Vargo JA et al (2019) Intraoperative (IORT) for surgically resected brain metastases: outcome analysis of an international cooperative study. J Neurooncol 145(2):391–397
Vargo JA, Sparks KM, Singh R, Jacobson GM, Hack JD, Cifarelli CP (2018) Feasibility of dose escalation using intraoperative radiotherapy following resection of large brain metastases compared to post-operative stereotactic radiosurgery. J Neuroncol 140(2):413–420
Gray RJ (1988) A class of K-sample tests for comparing the cumulative incidence of a competing risk. The Annals of Statistics 16(3):1141–1154
Kahl KH, Balagiannis N, Höck M et al (2021) Intraoperative with low-energy x-rays after neurosurgical resection of brain metastases - an Augsburg University Medical Center experience. Strahlen Onkol 197(12):1124–1130
Yamamoto M, Serizawa T, Shuto T et al (2014) Stereotactic radiosurgery for patients with multiple brain metastases (JLGK0901): a multi-institutional prospective observational study. Lancet Oncol 15(4):387–395
Robbins JR, Ryu S, Kalkanis S et al (2012) Radiosurgery to the surgical cavity as adjuvant therapy for resected brain metastasis. Neurosurgery 71(5):937–943
Diehl CD, Pigorsch SU, Gempt J et al (2023) Low-energy X-Ray Intraoperative Radiation Therapy (Lex-IORT) for resected brain metastases: a Single-Institution experience. Cancers 15:14
Patel KR, Burri SH, Asher AL et al (2016) Comparing preoperative with postoperative stereotactic radiosurgery for resectable brain metástases. Neurosurgery 79(2):279–285
Prabhu RS, Patel KR, Press RH et al (2019) Preoperative vs postoperative Radiosurgery for Resected Brain Metastases: a review. Neurosurgery 84(1):19–29
Herskind C, Wenz F, Giordano FA (2017) Immunotherapy Combined with large fractions of Radiotherapy: stereotactic radiosurgery for Brain Metastases-Implications for Intraoperative Radiotherapy after Resection. Front Oncol 7:147
Author information
Authors and Affiliations
Contributions
D.G.C. and P.I.S. concepted and organized the study. D.G.C. managed the study. All authors participated in the procedures or evaluation of patients. V.F.C. performed the statistical analysis and prepared figures. D.G.C. wrote the main manuscript. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
D.G.C. and F.A.G: travel and research grants from Carl Zeiss Meditec AG.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
de Castro, D.G., Sanematsu, P.I., Pellizzon, A.C.A. et al. Intraoperative radiotherapy for brain metastases: first-stage results of a single-arm, open-label, phase 2 trial. J Neurooncol 162, 211–215 (2023). https://doi.org/10.1007/s11060-023-04266-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-023-04266-x