Abstract
Metabolic syndrome (MetS) is a prevalent and intricate health condition affecting a significant global population, characterized by a cluster of metabolic and hormonal disorders disrupting lipid and glucose metabolism pathways. Clinical manifestations encompass obesity, dyslipidemia, insulin resistance, and hypertension, contributing to heightened risks of diabetes and cardiovascular diseases. Existing medications often fall short in addressing the syndrome’s multifaceted nature, leading to suboptimal treatment outcomes and potential long-term health risks. This scenario underscores the pressing need for innovative therapeutic approaches in MetS management. RNA-based treatments, employing small interfering RNAs (siRNAs), microRNAs (miRNAs), and antisense oligonucleotides (ASOs), emerge as promising strategies to target underlying biological abnormalities. However, a summary of research available on the role of RNA-based therapeutics in MetS and related co-morbidities is limited. Murine models and human studies have been separately interrogated to determine whether there have been recent advancements in RNA-based therapeutics to offer a comprehensive understanding of treatment available for MetS. In a narrative fashion, we searched for relevant articles pertaining to MetS co-morbidities such as cardiovascular disease, fatty liver disease, dementia, colorectal cancer, and endocrine abnormalities. We emphasize the urgency of exploring novel therapeutic avenues to address the intricate pathophysiology of MetS and underscore the potential of RNA-based treatments, coupled with advanced delivery systems, as a transformative approach for achieving more comprehensive and efficacious outcomes in MetS patients.
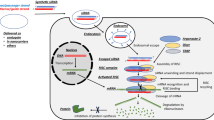
Graphical abstract
Incorporating the basis of RNA therapeutics in metabolic syndrome. RNA ribonucleic acid, mRNA messenger RNA, ASO anti-sense oligonucleotide, miRNA microRNA, siRNA small interfering RNA



Similar content being viewed by others
Data availability
No data available.
References
Fahed G et al (2022) Metabolic syndrome: updates on pathophysiology and management in 2021. Int J Mol Sci 23(2):786
Dobrowolski P et al (2022) Metabolic syndrome—a new definition and management guidelines: a joint position paper by the Polish Society of Hypertension, Polish Society for the Treatment of Obesity, Polish Lipid Association, Polish Association for Study of Liver, Polish Society of Family Medicine, Polish Society of Lifestyle Medicine, Division of Prevention and Epidemiology Polish Cardiac Society, “Club 30” Polish Cardiac Society, and Division of Metabolic and Bariatric Surgery Society of Polish Surgeons. Arch Med Sci 18(5):1133–1156
Altabas V (2013) Drug treatment of metabolic syndrome. Curr Clin Pharmacol 8(3):224–231
Rochlani Y et al (2017) Metabolic syndrome: pathophysiology, management, and modulation by natural compounds. Ther Adv Cardiovasc Dis 11(8):215–225
Fellmann L et al (2013) Murine models for pharmacological studies of the metabolic syndrome. Pharmacol Ther 137(3):331–340
Dad HA et al (2021) Plant exosome-like nanovesicles: emerging therapeutics and drug delivery nanoplatforms. Mol Ther 29(1):13–31
Ganju A et al (2017) miRNA nanotherapeutics for cancer. Drug Discov Today 22(2):424–432
Shinde SS et al (2023) therapeutic delivery of tumor suppressor miRNAs for breast cancer treatment. Biology 12(3):467
Zafar U et al (2018) Metabolic syndrome: an update on diagnostic criteria, pathogenesis, and genetic links. Hormones 17(3):299–313
Huang PL (2009) A comprehensive definition for metabolic syndrome. Dis Model Mech 2(5–6):231–237
Alberti KGMM, Zimmet PZ (1998) Definition, diagnosis and classification of diabetes mellitus and its complications. Part 1: diagnosis and classification of diabetes mellitus. Provisional report of a WHO consultation. Diabet Med 15(7):539–553
Expert Panel on Detection, Evaluation and Treatment of High Blood Cholesterol in Adults (2001) Executive summary of the third report of the National Cholesterol Education Program (NCEP) expert panel on detection, evaluation, and treatment of high blood cholesterol in adults (adult treatment panel III). JAMA 285(19):2486–2497
Luo L, Liu M (2016) Adipose tissue in control of metabolism. J Endocrinol 231(3):R77–R99
Recinella L et al (2020) Adipokines: new potential therapeutic target for obesity and metabolic, rheumatic, and cardiovascular diseases. Front Physiol 11:578966
Mair KM, Gaw R, MacLean MR (2020) Obesity, estrogens and adipose tissue dysfunction—implications for pulmonary arterial hypertension. Pulm Circ 10(3):2045894020952019
Obradovic M et al (2021) Leptin and obesity: role and clinical implication. Front Endocrinol 12:585887
Emamgholipour S et al (2020) Acetylation and insulin resistance: a focus on metabolic and mitogenic cascades of insulin signaling. Crit Rev Clin Lab Sci 57(3):196–214
Han CY (2016) Roles of reactive oxygen species on insulin resistance in adipose tissue. Diabetes Metab J 40(4):272–279
Maron BA, Leopold JA, Hemnes AR (2020) Metabolic syndrome, neurohumoral modulation, and pulmonary arterial hypertension. Br J Pharmacol 177(7):1457–1471
Dai Y et al (2013) LOX-1, a bridge between GLP-1R and mitochondrial ROS generation in human vascular smooth muscle cells. Biochem Biophys Res Commun 437(1):62–66
Esposito K, Giugliano D (2004) The metabolic syndrome and inflammation: association or causation? Nutr Metab Cardiovasc Dis 14(5):228–232
Ohta M et al (2020) IL-6 promotes cell adhesion in human endothelial cells via microRNA-126-3p suppression. Exp Cell Res 393(2):112094
Nie L et al (2018) Toll-like receptors, associated biological roles, and signaling networks in non-mammals. Front Immunol 9:1523
Jialal I, Kaur H, Devaraj S (2014) Toll-like receptor status in obesity and metabolic syndrome: a translational perspective. J Clin Endocrinol Metab 99(1):39–48
Jiang SZ et al (2016) Obesity and hypertension. Exp Ther Med 12(4):2395–2399
Zhu Y et al (2022) RNA-based therapeutics: an overview and prospectus. Cell Death Dis 13(7):644
Kim YK (2022) RNA therapy: rich history, various applications and unlimited future prospects. Exp Mol Med 54(4):455–465
Chen X et al (2018) RNA interference-based therapy and its delivery systems. Cancer Metastasis Rev 37(1):107–124
Liu W et al (2021) A novel delivery nanobiotechnology: engineered miR-181b exosomes improved osteointegration by regulating macrophage polarization. J Nanobiotechnol 19(1):269
Gandhi NS, Tekade RK, Chougule MB (2014) Nanocarrier mediated delivery of siRNA/miRNA in combination with chemotherapeutic agents for cancer therapy: current progress and advances. J Control Release 194:238–256
Cisa-Wieczorek S, Hernandez-Alvarez MI (2020) Deregulation of lipid homeostasis: a fa(c)t in the development of metabolic diseases. Cells 9(12):2605
Samovski D et al (2018) Regulation of insulin receptor pathway and glucose metabolism by CD36 signaling. Diabetes 67(7):1272–1284
Petersen MC, Shulman GI (2018) Mechanisms of insulin action and insulin resistance. Physiol Rev 98(4):2133–2223
Elchebly M et al (1999) Increased insulin sensitivity and obesity resistance in mice lacking the protein tyrosine phosphatase-1B gene. Science 283(5407):1544–1548
Teaney NA, Cyr NE (2023) FoxO1 as a tissue-specific therapeutic target for type 2 diabetes. Front Endocrinol 14:1286838
Nadkarni P, Chepurny OG, Holz GG (2014) Regulation of glucose homeostasis by GLP-1. Prog Mol Biol Transl Sci 121:23–65
Peng H et al (2021) Caveolin-1 is essential for the improvement of insulin sensitivity through AKT activation during glargine treatment on diabetic mice. J Diabetes Res 2021:9943344
Sud N, Taher J, Su Q (2015) MicroRNAs and noncoding RNAs in hepatic lipid and lipoprotein metabolism: potential therapeutic targets of metabolic disorders. Drug Dev Res 76(6):318–327
Creusot RJ et al (2008) Tissue-targeted therapy of autoimmune diabetes using dendritic cells transduced to express IL-4 in NOD mice. Clin Immunol 127(2):176–187
Alberti KG et al (2009) Harmonizing the metabolic syndrome: a joint interim statement of the International Diabetes Federation Task Force on Epidemiology and Prevention; National Heart, Lung, and Blood Institute; American Heart Association; World Heart Federation; International Atherosclerosis Society; and International Association for the Study of Obesity. Circulation 120(16):1640–1645
Tune JD et al (2017) Cardiovascular consequences of metabolic syndrome. Transl Res 183:57–70
Krychtiuk KA, Rader DJ, Granger CB (2022) RNA-targeted therapeutics in cardiovascular disease: the time is now. Eur Heart J Cardiovasc Pharmacother 9(1):94–99
Kerr TA, Davidson NO (2010) Therapeutic RNA manipulation in liver disease. Hepatology 51(3):1055–1061
Ray KK et al (2020) Two phase 3 trials of inclisiran in patients with elevated LDL cholesterol. N Engl J Med 382(16):1507–1519
Miya Shaik M et al (2018) The role of microRNAs in Alzheimer’s disease and their therapeutic potentials. Genes 9(4):174
Jenkins TA (2022) Metabolic syndrome and vascular-associated cognitive impairment: a focus on preclinical investigations. Curr Diab Rep 22(8):333–340
Wang P et al (2018) Systemic delivery of BACE1 siRNA through neuron-targeted nanocomplexes for treatment of Alzheimer’s disease. J Control Release 279:220–233
de Pretis N, Amodio A, Frulloni L (2018) Hypertriglyceridemic pancreatitis: epidemiology, pathophysiology and clinical management. United Eur Gastroenterol J 6(5):649–655
Yu T, Jhun BS, Yoon Y (2011) High-glucose stimulation increases reactive oxygen species production through the calcium and mitogen-activated protein kinase-mediated activation of mitochondrial fission. Antioxid Redox Signal 14(3):425–437
Fanaei SM et al (2023) The impact of metabolic syndrome on chronic kidney disease development. Insights from a big prospective study. Eur J Clin Invest 53(4):13945
Rubel D et al (2022) Anti-microRNA-21 therapy on top of ACE inhibition delays renal failure in alport syndrome mouse models. Cells 11(4):594
Vaduganathan M et al (2022) The global burden of cardiovascular diseases and risk: a compass for future health. J Am Coll Cardiol 80(25):2361–2371
Guembe MJ et al (2020) Risk for cardiovascular disease associated with metabolic syndrome and its components: a 13-year prospective study in the RIVANA cohort. Cardiovasc Diabetol 19(1):195
McCracken E, Monaghan M, Sreenivasan S (2018) Pathophysiology of the metabolic syndrome. Clin Dermatol 36(1):14–20
Santos RD et al (2015) Mipomersen preferentially reduces small low-density lipoprotein particle number in patients with hypercholesterolemia. J Clin Lipidol 9(2):201–209
Fogacci F et al (2019) Efficacy and safety of mipomersen: a systematic review and meta-analysis of randomized clinical trials. Drugs 79(7):751–766
Fogacci F et al (2020) Efficacy and safety of volanesorsen (ISIS 304801): the evidence from phase 2 and 3 clinical trials. Curr Atheroscler Rep 22(5):18
Bao X et al (2024) Targeting proprotein convertase subtilisin/kexin type 9 (PCSK9): from bench to bedside. Signal Transduct Target Ther 9(1):13
Boada C et al (2021) RNA therapeutics for cardiovascular disease. Curr Opin Cardiol 36(3):256–263
Aguilar-Salinas CA, Gomez-Diaz RA, Corral P (2022) New therapies for primary hyperlipidemia. J Clin Endocrinol Metab 107(5):1216–1224
Jones NR et al (2020) Diagnosis and management of hypertension in adults: NICE guideline update 2019. Br J Gen Pract 70(691):90–91
Huang SA et al (2020) Abstract 14387: dose-related reductions in blood pressure with a RNA interference (RNAi) therapeutic targeting angiotensinogen in hypertensive patients: interim results from a first-in-human phase 1 study of ALN-AGT01. Circulation. https://doi.org/10.1161/circ.142.suppl_3.14387
Gan LM et al (2019) Intradermal delivery of modified mRNA encoding VEGF-A in patients with type 2 diabetes. Nat Commun 10(1):871
Qureshi D et al (2024) Association between metabolic syndrome and risk of incident dementia in UK Biobank. Alzheimers Dement 20(1):447–458
Ezkurdia A, Ramirez MJ, Solas M (2023) Metabolic syndrome as a risk factor for Alzheimer’s disease: a focus on insulin resistance. Int J Mol Sci 24(5):4354
Craft S (2009) The role of metabolic disorders in Alzheimer disease and vascular dementia. Arch Neurol. https://doi.org/10.1001/archneurol.2009.27
Tasaki S et al (2022) Inferring protein expression changes from mRNA in Alzheimer’s dementia using deep neural networks. Nat Commun 13(1):655
Rofo F et al (2022) Blood-brain barrier penetrating neprilysin degrades monomeric amyloid-beta in a mouse model of Alzheimer’s disease. Alzheimers Res Ther 14(1):180
Teleanu DM et al (2018) Blood-brain delivery methods using nanotechnology. Pharmaceutics 10(4):269
Zhou Y et al (2020) Blood-brain barrier-penetrating siRNA nanomedicine for Alzheimer’s disease therapy. Sci Adv. https://doi.org/10.1126/sciadv.abc7031
Di Meco A, Pratico D (2016) MicroRNAs as therapeutic targets for Alzheimer’s disease. J Alzheimers Dis 53(2):367–372
Rinella ME et al (2023) A multi-society Delphi consensus statement on new fatty liver disease nomenclature. J Hepatol 78:1966
Powell EE, Wong VW, Rinella M (2021) Non-alcoholic fatty liver disease. Lancet 397(10290):2212–2224
De A et al (2023) Metabolic dysfunction-associated steatotic liver disease (MASLD) definition is better than MAFLD criteria for lean patients with NAFLD. J Hepatol. https://doi.org/10.1016/j.jhep.2023.07.031
Godoy-Matos AF, Silva Junior WS, Valerio CM (2020) NAFLD as a continuum: from obesity to metabolic syndrome and diabetes. Diabetol Metab Syndr 12:60
Zhu Y et al (2023) Therapeutic effects of microRNAs on nonalcoholic fatty liver disease (NAFLD) and nonalcoholic steatohepatitis (NASH): a systematic review and meta-analysis. Int J Mol Sci 24(11):9168
Yenilmez B et al (2022) An RNAi therapeutic targeting hepatic DGAT2 in a genetically obese mouse model of nonalcoholic steatohepatitis. Mol Ther 30(3):1329–1342
Konings M et al (2022) Investigating microRNAs to explain the link between cholesterol metabolism and NAFLD in humans: a systematic review. Nutrients 14(23):4946
Xu Y et al (2015) A metabolic stress-inducible miR-34a-HNF4alpha pathway regulates lipid and lipoprotein metabolism. Nat Commun 6:7466
Loyer X et al (2016) Liver microRNA-21 is overexpressed in non-alcoholic steatohepatitis and contributes to the disease in experimental models by inhibiting PPARalpha expression. Gut 65(11):1882–1894
Christian P, Su Q (2014) MicroRNA regulation of mitochondrial and ER stress signaling pathways: implications for lipoprotein metabolism in metabolic syndrome. Am J Physiol Endocrinol Metab 307(9):E729–E737
Harlid S, Myte R, Van Guelpen B (2017) The metabolic syndrome, inflammation, and colorectal cancer risk: an evaluation of large panels of plasma protein markers using repeated. Prediagnostic Samples Mediators Inflamm 2017:4803156
Liu T et al (2022) The combination of metabolic syndrome and inflammation increased the risk of colorectal cancer. Inflamm Res 71(7–8):899–909
Jin EH et al (2022) Association between metabolic syndrome and the risk of colorectal cancer diagnosed before age 50 years according to tumor location. Gastroenterology 163(3):637–648
Chung KC et al (2022) Association between metabolic syndrome and colorectal cancer incidence and all-cause mortality: a hospital-based observational study. BMC Gastroenterol 22(1):453
Sung H et al (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71(3):209–249
Liu J, Guo B (2020) RNA-based therapeutics for colorectal cancer: Updates and future directions. Pharmacol Res 152:104550
Siegel RL et al (2017) Colorectal cancer statistics, 2017. CA Cancer J Clin 67(3):177–193
Peng HX et al (2015) Role of B7–H4 siRNA in proliferation, migration, and invasion of LOVO colorectal carcinoma cell line. Biomed Res Int 2015:326981
Baumer S et al (2015) Antibody-mediated delivery of anti-KRAS-siRNA in vivo overcomes therapy resistance in colon cancer. Clin Cancer Res 21(6):1383–1394
Sadreddini S et al (2017) Chitosan nanoparticles as a dual drug/siRNA delivery system for treatment of colorectal cancer. Immunol Lett 181:79–86
Lin YX et al (2020) RNA nanotechnology-mediated cancer immunotherapy. Theranostics 10(1):281–299
Tao YJ et al (2015) Antisense oligonucleotides against microRNA-21 reduced the proliferation and migration of human colon carcinoma cells. Cancer Cell Int 15:77
Grandl G, Wolfrum C (2018) Hemostasis, endothelial stress, inflammation, and the metabolic syndrome. Semin Immunopathol 40(2):215–224
Konstantinides S et al (2001) Leptin-dependent platelet aggregation and arterial thrombosis suggests a mechanism for atherothrombotic disease in obesity. J Clin Invest 108(10):1533–1540
Cesari M, Pahor M, Incalzi RA (2010) Plasminogen activator inhibitor-1 (PAI-1): a key factor linking fibrinolysis and age-related subclinical and clinical conditions. Cardiovasc Ther 28(5):72–91
De Pablo-Moreno JA et al (2022) The vascular endothelium and coagulation: homeostasis, disease, and treatment, with a focus on the Von Willebrand factor and factors VIII and V. Int J Mol Sci 23(15):8283
Weng Y et al (2019) RNAi therapeutic and its innovative biotechnological evolution. Biotechnol Adv 37(5):801–825
Boyce S, Rangarajan S (2023) RNAi for the treatment of people with hemophilia: current evidence and patient selection. J Blood Med 14:317–327
Sehgal A et al (2015) An RNAi therapeutic targeting antithrombin to rebalance the coagulation system and promote hemostasis in hemophilia. Nat Med 21(5):492–497
de Laat-Kremers RMW et al (2021) Tailoring the effect of antithrombin-targeting therapy in haemophilia A using in silico thrombin generation. Sci Rep 11(1):15572
Szatmary P et al (2022) Acute pancreatitis: diagnosis and treatment. Drugs 82(12):1251–1276
Nieto-Vazquez I et al (2008) Insulin resistance associated to obesity: the link TNF-alpha. Arch Physiol Biochem 114(3):183–194
Shen Z et al (2021) Metabolic syndrome components and acute pancreatitis: a case-control study in China. BMC Gastroenterol 21(1):17
Guo YY et al (2019) Hypertriglyceridemia-induced acute pancreatitis: progress on disease mechanisms and treatment modalities. Discov Med 27(147):101–109
Zhou W et al (2022) New challenges for microRNAs in acute pancreatitis: progress and treatment. J Transl Med 20(1):192
Shen Y et al (2021) miR-9 alleviated the inflammatory response and apoptosis in caerulein-induced acute pancreatitis by regulating FGF10 and the NF-kappaB signaling pathway. Exp Ther Med 22(2):795
Wang Q, Liu S, Han Z (2020) miR-339-3p regulated acute pancreatitis induced by caerulein through targeting TNF receptor-associated factor 3 in AR42J cells. Open Life Sci 15(1):912–922
Patel HR et al (2023) The role of MicroRNAs in pancreatitis development and progression. Int J Mol Sci 24(2):1057
Goodwin D et al (2014) Evaluation of miR-216a and miR-217 as potential biomarkers of acute pancreatic injury in rats and mice. Biomarkers 19(6):517–529
Zhang XX et al (2017) Circulating microRNA 216 as a marker for the early identification of severe acute pancreatitis. Am J Med Sci 353(2):178–186
Sun Y et al (2013) MiR-150-5p inhibits the proliferation and promoted apoptosis of pancreatic cancer cells. Zhonghua Bing Li Xue Za Zhi 42(7):460–464
Elendu C et al (2023) Comprehensive review of current management guidelines of chronic kidney disease. Medicine 102(23):e33984
Feng X et al (2023) Secular trends of epidemiologic patterns of chronic kidney disease over three decades: an updated analysis of the global burden of disease study 2019. BMJ Open 13(3):e064540
Sun F, Tao Q, Zhan S (2010) Metabolic syndrome and the development of chronic kidney disease among 118 924 non-diabetic Taiwanese in a retrospective cohort. Nephrology 15(1):84–92
Ruan X, Guan Y (2009) Metabolic syndrome and chronic kidney disease. J Diabetes 1(4):236–245
Bondue T et al (2023) The potential of RNA-based therapy for kidney diseases. Pediatr Nephrol 38(2):327–344
Guo J et al (2019) Dysregulated expression of microRNA-21 and disease-related genes in human patients and in a mouse model of alport syndrome. Hum Gene Ther 30(7):865–881
Shimizu H et al (2010) siRNA-based therapy ameliorates glomerulonephritis. J Am Soc Nephrol 21(4):622–633
Williams RM, Jaimes EA, Heller DA (2016) Nanomedicines for kidney diseases. Kidney Int 90(4):740–745
Gao S et al (2014) Megalin-mediated specific uptake of chitosan/siRNA nanoparticles in mouse kidney proximal tubule epithelial cells enables AQP1 gene silencing. Theranostics 4(10):1039–1051
Asgeirsdottir SA et al (2008) Inhibition of proinflammatory genes in anti-GBM glomerulonephritis by targeted dexamethasone-loaded AbEsel liposomes. Am J Physiol Renal Physiol 294(3):F554–F561
Zuckerman JE et al (2012) Polycation-siRNA nanoparticles can disassemble at the kidney glomerular basement membrane. Proc Natl Acad Sci U S A 109(8):3137–3142
Zuckerman JE et al (2015) siRNA delivery to the glomerular mesangium using polycationic cyclodextrin nanoparticles containing siRNA. Nucleic Acid Ther 25(2):53–64
Benjafield AV et al (2019) Estimation of the global prevalence and burden of obstructive sleep apnoea: a literature-based analysis. Lancet Respir Med 7(8):687–698
Kim DH et al (2021) The relationship between metabolic syndrome and obstructive sleep apnea syndrome: a nationwide population-based study. Sci Rep 11(1):8751
Li K, Chen ZT, Qin YW (2019) Expression profiles of microRNA related to atherosclerosis in patients with OSA. Lin Chung Er Bi Yan Hou Tou Jing Wai Ke Za Zhi 33(4):304–309
Gottlieb DJ, Punjabi NM (2020) Diagnosis and management of obstructive sleep apnea: a review. JAMA 323(14):1389–1400
Li K et al (2018) MiR-664a-3p expression in patients with obstructive sleep apnea: A potential marker of atherosclerosis. Medicine 97(6):e9813
Santamaria-Martos F et al (2019) Circulating microRNA profile as a potential biomarker for obstructive sleep apnea diagnosis. Sci Rep 9(1):13456
Khurana S et al (2020) In-silico investigations of selective miRNA-gene targets and their validation studies in obstructive sleep apnea (OSA) patient cohorts. Comput Biol Chem 87:107264
He L et al (2020) miR-126a-3p targets HIF-1alpha and alleviates obstructive sleep apnea syndrome with hypertension. Hum Cell 33(4):1036–1045
Sanchez-de-la-Torre M et al (2015) Precision medicine in patients with resistant hypertension and obstructive sleep apnea: blood pressure response to continuous positive airway pressure treatment. J Am Coll Cardiol 66(9):1023–1032
Chen YC et al (2020) miR-21–5p under-expression in patients with obstructive sleep apnea modulates intermittent hypoxia with re-oxygenation-induced-cell apoptosis and cytotoxicity by targeting pro-inflammatory TNF-alpha-TLR4 signaling. Int J Mol Sci 21(3):999
Zhang Z et al (2019) Overexpressed long noncoding RNA CPS1-IT alleviates pulmonary arterial hypertension in obstructive sleep apnea by reducing interleukin-1beta expression via HIF1 transcriptional activity. J Cell Physiol 234(11):19715–19727
Liu Y et al (2023) Role of precision medicine in obstructive sleep apnoea. BMJ Med 2(1):e000218
Xu Y et al (2021) Inhaled RNA therapeutics for obstructive airway diseases: recent advances and future prospects. Pharmaceutics 13(2):177
Sadeghi HM et al (2022) Polycystic ovary syndrome: a comprehensive review of pathogenesis, management, and drug repurposing. Int J Mol Sci 23(2):583
Azziz R (2018) Polycystic ovary syndrome. Obstet Gynecol 132(2):321–336
Chen W, Pang Y (2021) Metabolic syndrome and PCOS: pathogenesis and the role of metabolites. Metabolites 11(12):869
Tamaddon M, Azimzadeh M, Tavangar SM (2022) microRNAs and long non-coding RNAs as biomarkers for polycystic ovary syndrome. J Cell Mol Med 26(3):654–670
Che X et al (2020) PCOS serum-derived exosomal miR-27a-5p stimulates endometrial cancer cells migration and invasion. J Mol Endocrinol 64(1):1–12
Deswal R, Dang AS (2020) Dissecting the role of micro-RNAs as a diagnostic marker for polycystic ovary syndrome: a systematic review and meta-analysis. Fertil Steril 113(3):661–669
Huang X et al (2020) Depletion of exosomal circLDLR in follicle fluid derepresses miR-1294 function and inhibits estradiol production via CYP19A1 in polycystic ovary syndrome. Aging 12(15):15414–15435
Li L et al (2021) Long non-coding RNA H19 regulates proliferation of ovarian granulosa cells via STAT3 in polycystic ovarian syndrome. Arch Med Sci 17(3):785–791
Tiemann K, Rossi JJ (2009) RNAi-based therapeutics-current status, challenges and prospects. EMBO Mol Med 1(3):142–151
Kang H et al (2023) Small interfering RNA (siRNA)-based therapeutic applications against viruses: principles, potential, and challenges. J Biomed Sci 30(1):88
Jackson AL et al (2006) Widespread siRNA “off-target” transcript silencing mediated by seed region sequence complementarity. RNA 12(7):1179–1187
Kanasty RL et al (2012) Action and reaction: the biological response to siRNA and its delivery vehicles. Mol Ther 20(3):513–524
Tafer H et al (2008) The impact of target site accessibility on the design of effective siRNAs. Nat Biotechnol 26(5):578–583
Lu ZJ, Mathews DH (2008) OligoWalk: an online siRNA design tool utilizing hybridization thermodynamics. Nucleic Acids Res 36:W104–W108
Reynolds A et al (2004) Rational siRNA design for RNA interference. Nat Biotechnol 22(3):326–330
Hu B et al (2020) Therapeutic siRNA: state of the art. Signal Transduct Target Ther 5(1):101
Funding
Authors have no funding to declare.
Author information
Authors and Affiliations
Contributions
Conceptualization of topic and coordination of reading, writing, and editing: HH; Reading, writing, and editing of the original draft: All authors; Critical revision of the manuscript: HH, SB, MS, MB; Figures and tables: HH, SB, MS; Final approval of manuscript: HH, MB.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Conflicts of interest
Authors have no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Huang, H.Y.R., Badar, S., Said, M. et al. The advent of RNA-based therapeutics for metabolic syndrome and associated conditions: a comprehensive review of the literature. Mol Biol Rep 51, 493 (2024). https://doi.org/10.1007/s11033-024-09457-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11033-024-09457-x