Abstract
Tissue engineering faces an intriguing challenge in creating biomaterials for cartilage repair. Within the category of biopolymeric scaffolds, hydrogels made from polysaccharides are particularly suitable for regenerating cartilage tissue. In this paper, a new formulation of biocompatible alginate-based hydrogel for joint cartilage regeneration was investigated. An alginate-dendrimer hydrogel obtained by covalently grafting alginate with polyamidoamine generation 5 dendrimer. 58S bioactive glass was synthesized through sol–gel procedures and was added to the hydrogel before cross-linking. The obtained hydrogel is an innovative system with sustained drug-releasing properties and improved mechanical behavior in comparison to the alginate matrix. For instance, the tensile and compressive modulus of the fabricated composite hydrogel increased from 0.035 to 0.072 MPa and 0.17 to 0.40 MPa respectively. Whereas the degradation ratio decreased from 0.26 to 0.09% by the addition of polyamidoamine and bioactive glass. The developed hydrogel also showed better properties in in-vitro studies such as swelling and degradation. MTT assay showed no toxicity and revealed the biocompatibility of prepared hydrogel. The MTT test, also performed better adhesion of cells by the addition of bioactive glass powder. The composite hydrogel loaded with tetracycline hydrochloride showed more sustained drug-release behavior and excellent antibacterial properties compared to bear alginate hydrogel. Therefore, the Alginate/polyamidoamine/bioactive glass hydrogel can couple the well-known bioactive properties of 58S bioactive glass with good biocompatibility of alginate-dendrimer hydrogels, opening new approaches in the field of tissue engineering.
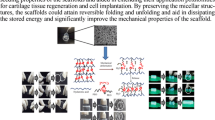
Graphical abstract











Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Tran HDN, Park KD, Ching YC et al (2020) A comprehensive review on polymeric hydrogel and its composite: matrices of choice for bone and cartilage tissue engineering. J Ind Eng Chem 89:58–82. https://doi.org/10.1016/j.jiec.2020.06.017
Gao X, Gao L, Groth T et al (2019) Fabrication and properties of an injectable sodium alginate/PRP composite hydrogel as a potential cell carrier for cartilage repair. J Biomed Mater Res Part A 107:2076–2087. https://doi.org/10.1002/jbm.a.36720
Zhang Z-Z, Jiang D, Ding J-X et al (2016) Role of scaffold mean pore size in meniscus regeneration. Acta Biomater 43:314–326. https://doi.org/10.1016/j.actbio.2016.07.050
Lima AC, Ferreira H, Reis RL, Neves NM (2019) Biodegradable polymers: an update on drug delivery in bone and cartilage diseases. Expert Opin Drug Deliv 16:795–813. https://doi.org/10.1080/17425247.2019.1635117
Cutcliffe HC, DeFrate LE (2020) Comparison of cartilage mechanical properties measured during creep and recovery. Sci Rep 10:1547. https://doi.org/10.1038/s41598-020-58220-2
Bilgen B, Jayasuriya CT, Owens BD (2018) Current concepts in meniscus tissue engineering and repair. Adv Healthc Mater 7:1701407. https://doi.org/10.1002/adhm.201701407
Ma X, Yang R, Wang P et al (2022) Bioinspired dual dynamic network hydrogels promote cartilage regeneration through regulating BMSC chondrogenic differentiation. Mater Today Chem 23:100648. https://doi.org/10.1016/j.mtchem.2021.100648
Asadi N, Alizadeh E, Salehi R et al (2018) Nanocomposite hydrogels for cartilage tissue engineering: a review. Artif Cells Nanomed Biotechnol 46:465–471. https://doi.org/10.1080/21691401.2017.1345924
Chuang E-Y, Chiang C-W, Wong P-C, Chen C-H (2018) Hydrogels for the application of articular cartilage tissue engineering: a review of hydrogels. Adv Mater Sci Eng 2018:1–13. https://doi.org/10.1155/2018/4368910
Yang F, Zhao J, Koshut WJ et al (2020) A synthetic hydrogel composite with the mechanical behavior and durability of cartilage. Adv Funct Mater 30:2003451. https://doi.org/10.1002/adfm.202003451
Bertuola M, Aráoz B, Gilabert U et al (2021) Gelatin–alginate–hyaluronic acid inks for 3D printing: effects of bioglass addition on printability, rheology and scaffold tensile modulus. J Mater Sci 56:15327–15343. https://doi.org/10.1007/s10853-021-06250-0
Zhang M, Zhao X (2020) Alginate hydrogel dressings for advanced wound management. Int J Biol Macromol 162:1414–1428. https://doi.org/10.1016/j.ijbiomac.2020.07.311
García-García P, Reyes R, Pérez-Herrero E et al (2020) Alginate-hydrogel versus alginate-solid system efficacy in bone regeneration in osteoporosis. Mater Sci Eng C 115:111009. https://doi.org/10.1016/j.msec.2020.111009
Chen Z, Lv Y (2022) Gelatin/sodium alginate composite hydrogel with dynamic matrix stiffening ability for bone regeneration. Compos Part B Eng 243:110162. https://doi.org/10.1016/j.compositesb.2022.110162
Liu W, Madry H, Cucchiarini M (2022) Application of alginate hydrogels for next-generation articular cartilage regeneration. Int J Mol Sci 23:1147. https://doi.org/10.3390/ijms23031147
Gorroñogoitia I, Urtaza U, Zubiarrain-Laserna A et al (2022) A study of the printability of alginate-based bioinks by 3D bioprinting for articular cartilage tissue engineering. Polymers 14:354. https://doi.org/10.3390/polym14020354
Farokhi M, Jonidi Shariatzadeh F, Solouk A, Mirzadeh H (2020) Alginate based scaffolds for cartilage tissue engineering: a review. Int J Polym Mater Polym Biomater 69:230–247. https://doi.org/10.1080/00914037.2018.1562924
Calori IR, Braga G, de Jesus P, da CC, et al (2020) Polymer scaffolds as drug delivery systems. Eur Polym J 129:109621. https://doi.org/10.1016/j.eurpolymj.2020.109621
Moshaverinia A, Xu X, Chen C et al (2013) Dental mesenchymal stem cells encapsulated in an alginate hydrogel co-delivery microencapsulation system for cartilage regeneration. Acta Biomater 9:9343–9350. https://doi.org/10.1016/j.actbio.2013.07.023
El-Houssiny AS, Ward AA, Mostafa DM et al (2016) Drug–polymer interaction between glucosamine sulfate and alginate nanoparticles: FTIR, DSC and dielectric spectroscopy studies. Adv Nat Sci Nanosci Nanotechnol 7:025014. https://doi.org/10.1088/2043-6262/7/2/025014
Mathew M, Rad MA, Mata JP et al (2022) Hyperbranched polymers tune the physicochemical, mechanical, and biomedical properties of alginate hydrogels. Mater Today Chem 23:100656. https://doi.org/10.1016/j.mtchem.2021.100656
Malik N, Wiwattanapatapee R, Klopsch R et al (2000) Dendrimers. J Control Release 65:133–148. https://doi.org/10.1016/S0168-3659(99)00246-1
Matai I, Gopinath P (2016) Chemically cross-linked hybrid nanogels of alginate and PAMAM dendrimers as efficient anticancer drug delivery vehicles. ACS Biomater Sci Eng 2:213–223. https://doi.org/10.1021/acsbiomaterials.5b00392
Staehlke S, Lehnfeld J, Schneider A et al (2019) Terminal chemical functions of polyamidoamine dendrimer surfaces and its impact on bone cell growth. Mater Sci Eng C 101:190–203. https://doi.org/10.1016/j.msec.2019.03.073
Patil S, Nune K, Misra R (2018) Alginate/poly(amidoamine) injectable hybrid hydrogel for cell delivery. J Biomater Appl 33:295–314. https://doi.org/10.1177/0885328218790211
Rahaman MN, Day DE, Sonny Bal B et al (2011) Bioactive glass in tissue engineering. Acta Biomater 7:2355–2373. https://doi.org/10.1016/j.actbio.2011.03.016
Chevalier J, Gremillard L (2009) Ceramics for medical applications: a picture for the next 20 years. J Eur Ceram Soc 29:1245–1255. https://doi.org/10.1016/j.jeurceramsoc.2008.08.025
Utech S, Boccaccini AR (2016) A review of hydrogel-based composites for biomedical applications: enhancement of hydrogel properties by addition of rigid inorganic fillers. J Mater Sci 51:271–310. https://doi.org/10.1007/s10853-015-9382-5
Kargozar S, Hamzehlou S, Baino F (2019) Can bioactive glasses be useful to accelerate the healing of epithelial tissues? Mater Sci Eng C 97:1009–1020. https://doi.org/10.1016/j.msec.2019.01.028
Sonatkar J, Kandasubramanian B (2021) Bioactive glass with biocompatible polymers for bone applications. Eur Polym J 160:110801. https://doi.org/10.1016/j.eurpolymj.2021.110801
Miguez-Pacheco V, de Ligny D, Schmidt J et al (2018) Development and characterization of niobium-releasing silicate bioactive glasses for tissue engineering applications. J Eur Ceram Soc 38:871–876. https://doi.org/10.1016/j.jeurceramsoc.2017.07.028
Balasubramanian P, Büttner T, Miguez Pacheco V, Boccaccini AR (2018) Boron-containing bioactive glasses in bone and soft tissue engineering. J Eur Ceram Soc 38:855–869. https://doi.org/10.1016/j.jeurceramsoc.2017.11.001
Shahrbabak MSN, Sharifianjazi F, Rahban D, Salimi A (2019) A comparative investigation on bioactivity and antibacterial properties of sol-gel derived 58S bioactive glass substituted by Ag and Zn. Silicon 11:2741–2751. https://doi.org/10.1007/s12633-018-0063-2
Sepulveda P, Jones JR, Hench LL (2002) In vitro dissolution of melt-derived 45S5 and sol-gel derived 58S bioactive glasses. J Biomed Mater Res 61:301–311. https://doi.org/10.1002/jbm.10207
Meng J, Boschetto F, Yagi S et al (2022) Melt-electrowritten poly(L-lactic acid)- and bioglass-reinforced biomimetic hydrogel for bone regeneration. Mater Des 219:110781. https://doi.org/10.1016/j.matdes.2022.110781
Zhang X, Li Y, Ma Z et al (2021) Modulating degradation of sodium alginate/bioglass hydrogel for improving tissue infiltration and promoting wound healing. Bioact Mater 6:3692–3704. https://doi.org/10.1016/j.bioactmat.2021.03.038
Vukajlovic D, Parker J, Bretcanu O, Novakovic K (2019) Chitosan based polymer/bioglass composites for tissue engineering applications. Mater Sci Eng C 96:955–967. https://doi.org/10.1016/j.msec.2018.12.026
Lin B, Hu H, Deng Z et al (2020) Novel bioactive glass cross-linked PVA hydrogel with enhanced chondrogenesis properties and application in mice chondrocytes for cartilage repair. J Non Cryst Solids 529:119594. https://doi.org/10.1016/j.jnoncrysol.2019.119594
Sánchez-Aguinagalde O, Lejardi A, Meaurio E et al (2021) Novel hydrogels of chitosan and poly(vinyl alcohol) reinforced with inorganic particles of bioactive glass. Polym Basel 13:691. https://doi.org/10.3390/polym13050691
Zhou L, Fan L, Zhang F-M et al (2021) Hybrid gelatin/oxidized chondroitin sulfate hydrogels incorporating bioactive glass nanoparticles with enhanced mechanical properties, mineralization, and osteogenic differentiation. Bioact Mater 6:890–904. https://doi.org/10.1016/j.bioactmat.2020.09.012
Srinivasan S, Jayasree R, Chennazhi KP et al (2012) Biocompatible alginate/nano bioactive glass ceramic composite scaffolds for periodontal tissue regeneration. Carbohydr Polym 87:274–283. https://doi.org/10.1016/j.carbpol.2011.07.058
Clare A, Jones JR (2012) Bio-glasses: an introduction. Wiley, Hoboken, pp 179–202
Moghanian A, Firoozi S, Tahriri M (2017) Synthesis and in vitro studies of sol-gel derived lithium substituted 58S bioactive glass. Ceram Int 43(15):12835–12843
Jones JR (2015) Reprint of: review of bioactive glass: from hench to hybrids. Acta Biomater 23:S53–S82. https://doi.org/10.1016/j.actbio.2015.07.019
Schulz A, Katsen-Globa A, Huber EJ et al (2018) Poly(amidoamine)-alginate hydrogels: directing the behavior of mesenchymal stem cells with charged hydrogel surfaces. J Mater Sci Mater Med 29:105. https://doi.org/10.1007/s10856-018-6113-x
Farokhi M, Solouk A, Mirzadeh H et al (2023) An injectable enzymatically crosslinked and mechanically tunable silk fibroin/chondroitin sulfate chondro-inductive hydrogel. Macromol Mater Eng 308:2200503. https://doi.org/10.1002/mame.202200503
Sani M, Hosseinie R, Latifi M et al (2022) Engineered artificial articular cartilage made of decellularized extracellular matrix by mechanical and IGF-1 stimulation. Biomater Adv 139:213019. https://doi.org/10.1016/j.bioadv.2022.213019
Gu P, Li B, Wu B et al (2020) Controlled hydration, transition, and drug release realized by adjusting layer thickness in alginate-Ca2+/poly( N -isopropylacrylamide) Interpenetrating polymeric network hydrogels on cotton fabrics. ACS Biomater Sci Eng 6:5051–5060. https://doi.org/10.1021/acsbiomaterials.0c00756
Petrova VA, Elokhovskiy VY, Raik SV et al (2019) Alginate gel reinforcement with chitin nanowhiskers modulates rheological properties and drug release profile. Biomolecules 9:291. https://doi.org/10.3390/biom9070291
Naghizadeh Z, Karkhaneh A, Nokhbatolfoghahaei H et al (2021) Cartilage regeneration with dual-drug-releasing injectable hydrogel/microparticle system: in vitro and in vivo study. J Cell Physiol 236:2194–2204. https://doi.org/10.1002/jcp.30006
Chen H, Xing X, Tan H et al (2017) Covalently antibacterial alginate-chitosan hydrogel dressing integrated gelatin microspheres containing tetracycline hydrochloride for wound healing. Mater Sci Eng C 70:287–295. https://doi.org/10.1016/j.msec.2016.08.086
Hafezi Moghaddam R, Dadfarnia S, Shabani AMH et al (2019) Electron beam irradiation synthesis of porous and non-porous pectin based hydrogels for a tetracycline drug delivery system. Mater Sci Eng C 102:391–404. https://doi.org/10.1016/j.msec.2019.04.071
Kaviani A, Pircheraghi G, Bagheri R, Goharpey F (2023) Polyelectrolyte complexes between chitosan and quince seed gum: a rheological, structural, and multiple dye adsorption study. J Polym Environ 31:852–869. https://doi.org/10.1007/s10924-022-02634-8
Costa VC, Costa HS, Vasconcelos WL et al (2007) Preparation of hybrid biomaterials for bone tissue engineering. Mater Res 10:21–26. https://doi.org/10.1590/S1516-14392007000100006
Saqaei M, Fathi M, Edris H, Mortazavi V (2015) Preparation and biocompatibility evaluation of bioactive glass–forsterite nanocomposite powder for oral bone defects treatment applications. Mater Sci Eng C 56:409–416. https://doi.org/10.1016/j.msec.2015.07.002
Li X, Cho B, Martin R et al (2019) Nanofiber-hydrogel composite–mediated angiogenesis for soft tissue reconstruction. Sci Transl Med 11:eaau6210. https://doi.org/10.1126/scitranslmed.aau6210
Yacob N, Hashim K (2014) Morphological effect on swelling behavior of hydrogel. 153–159
de Nunes R, M, Girão VCC, Cunha PLR, et al (2021) Decreased sulfate content and zeta potential distinguish glycosaminoglycans of the extracellular matrix of osteoarthritis cartilage. Front Med 8:612370. https://doi.org/10.3389/fmed.2021.612370
Xu HHK, Simon CG (2005) Fast setting calcium phosphate–chitosan scaffold: mechanical properties and biocompatibility. Biomaterials 26:1337–1348. https://doi.org/10.1016/j.biomaterials.2004.04.043
Gaharwar AK, Rivera C, Wu C-J et al (2013) Photocrosslinked nanocomposite hydrogels from PEG and silica nanospheres: structural, mechanical and cell adhesion characteristics. Mater Sci Eng C 33:1800–1807. https://doi.org/10.1016/j.msec.2012.12.099
Kumar BYS, Isloor AM, Kumar GCM et al (2019) Nanohydroxyapatite reinforced chitosan composite hydrogel with tunable mechanical and biological properties for cartilage regeneration. Sci Rep 9:15957. https://doi.org/10.1038/s41598-019-52042-7
Mortier C, Costa DCS, Oliveira MB et al (2022) Advanced hydrogels based on natural macromolecules: chemical routes to achieve mechanical versatility. Mater Today Chem 26:101222. https://doi.org/10.1016/j.mtchem.2022.101222
Nezhad-Mokhtari P, Ghorbani M, Roshangar L, Soleimani Rad J (2019) A review on the construction of hydrogel scaffolds by various chemically techniques for tissue engineering. Eur Polym J 117:64–76. https://doi.org/10.1016/j.eurpolymj.2019.05.004
Iviglia G, Cassinelli C, Torre E et al (2016) Novel bioceramic-reinforced hydrogel for alveolar bone regeneration. Acta Biomater 44:97–109. https://doi.org/10.1016/j.actbio.2016.08.012
Faghihi S, Gheysour M, Karimi A, Salarian R (2014) Fabrication and mechanical characterization of graphene oxide-reinforced poly (acrylic acid)/gelatin composite hydrogels. J Appl Phys 115:083513. https://doi.org/10.1063/1.4864153
Abedini AA, Pircheraghi G, Kaviani A (2023) The role of calcium crosslinking and glycerol plasticizing on the physical and mechanical properties of superabsorbent. J Polym Res 30:20. https://doi.org/10.1007/s10965-022-03397-5
Jang J, Seol Y-J, Kim HJ et al (2014) Effects of alginate hydrogel cross-linking density on mechanical and biological behaviors for tissue engineering. J Mech Behav Biomed Mater 37:69–77. https://doi.org/10.1016/j.jmbbm.2014.05.004
Jiang Y-Y, Zhu Y-J, Li H et al (2017) Preparation and enhanced mechanical properties of hybrid hydrogels comprising ultralong hydroxyapatite nanowires and sodium alginate. J Colloid Interface Sci 497:266–275. https://doi.org/10.1016/j.jcis.2017.03.032
Jeon O, Bouhadir KH, Mansour JM, Alsberg E (2009) Photocrosslinked alginate hydrogels with tunable biodegradation rates and mechanical properties. Biomaterials 30:2724–2734. https://doi.org/10.1016/j.biomaterials.2009.01.034
Di S, Liu X, Liu D et al (2016) A multifunctional porous scaffold with capacities of minimally invasive implantation, self-fitting and drug delivery. Mater Today Chem 1:52–62. https://doi.org/10.1016/j.mtchem.2016.11.004
Cheng Y, Lu J, Liu S et al (2014) The preparation, characterization and evaluation of regenerated cellulose/collagen composite hydrogel films. Carbohydr Polym 107:57–64. https://doi.org/10.1016/j.carbpol.2014.02.034
Mikael PE, Kim HS, Nukavarapu SP (2018) Hybrid extracellular matrix design for cartilage-mediated bone regeneration. J Biomed Mater Res Part B Appl Biomater 106:300–309. https://doi.org/10.1002/jbm.b.33842
He X, Zeng L, Cheng X et al (2021) Shape memory composite hydrogel based on sodium alginate dual crosslinked network with carboxymethyl cellulose. Eur Polym J 156:110592. https://doi.org/10.1016/j.eurpolymj.2021.110592
Mansoorianfar M, Shahin K, Mirström MM, Li D (2021) Cellulose-reinforced bioglass composite as flexible bioactive bandage to enhance bone healing. Ceram Int 47:416–423. https://doi.org/10.1016/j.ceramint.2020.08.148
Zhang H, Xiong Y, Dong L et al (2021) Microstructural, mechanical properties and strengthening mechanism of DLP produced β-tricalcium phosphate scaffolds by incorporation of MgO/ZnO/58S bioglass. Ceram Int 47:25863–25874. https://doi.org/10.1016/j.ceramint.2021.05.317
Farag MM (2023) Recent trends on biomaterials for tissue regeneration applications: review. J Mater Sci 58:527–558. https://doi.org/10.1007/s10853-022-08102-x
Keshavarz M, Alizadeh P (2021) On the role of alginate coating on the mechanical and biological properties of 58S bioactive glass scaffolds. Int J Biol Macromol 167:947–961. https://doi.org/10.1016/j.ijbiomac.2020.11.051
Liu H, Yazici H, Ergun C et al (2008) An in vitro evaluation of the Ca/P ratio for the cytocompatibility of nano-to-micron particulate calcium phosphates for bone regeneration. Acta Biomater 4:1472–1479. https://doi.org/10.1016/j.actbio.2008.02.025
Rocton N, Oudadesse H, Lefeuvre B et al (2020) Fine analysis of interaction mechanism of bioactive glass surface after soaking in SBF solution: AFM and ICP-OES investigations. Appl Surf Sci 505:144076. https://doi.org/10.1016/j.apsusc.2019.144076
Montalbano G, Molino G, Fiorilli S, Vitale-Brovarone C (2020) Synthesis and incorporation of rod-like nano-hydroxyapatite into type I collagen matrix: a hybrid formulation for 3D printing of bone scaffolds. J Eur Ceram Soc 40:3689–3697. https://doi.org/10.1016/j.jeurceramsoc.2020.02.018
Juhasz JA, Best SM (2012) Bioactive ceramics: processing, structures and properties. J Mater Sci 47:610–624. https://doi.org/10.1007/s10853-011-6063-x
Abou-Okeil A, Aly AA, Amr A, Soliman AAF (2019) Biocompatible hydrogel for cartilage repair with adjustable properties. Polym Adv Technol 30:2026–2033. https://doi.org/10.1002/pat.4635
Abedi-Gaballu F, Dehghan G, Ghaffari M et al (2018) PAMAM dendrimers as efficient drug and gene delivery nanosystems for cancer therapy. Appl Mater Today 12:177–190. https://doi.org/10.1016/j.apmt.2018.05.002
Kheraldine H, Rachid O, Habib AM et al (2021) Emerging innate biological properties of nano-drug delivery systems: a focus on PAMAM dendrimers and their clinical potential. Adv Drug Deliv Rev 178:113908. https://doi.org/10.1016/j.addr.2021.113908
Fana M, Gallien J, Srinageshwar B et al (2020) PAMAM dendrimer nanomolecules utilized as drug delivery systems for potential treatment of glioblastoma: a systematic review. Int J Nanomed 15:2789–2808. https://doi.org/10.2147/IJN.S243155
Najafi F, Pashaei-Sarnaghi R, Salami-Kalajahi M, Roghani-Mamaqani H (2021) Application of poly(amidoamine) dendrimer as transfer agent to synthesize poly(amidoamine)-b-poly(methyl acrylate) amphiphilc block copolymers: self-assembly in aqueous media and drug delivery. J Drug Deliv Sci Technol 64:102626. https://doi.org/10.1016/j.jddst.2021.102626
Goodarzi K, Jonidi Shariatzadeh F, Solouk A et al (2020) Injectable drug loaded gelatin based scaffolds as minimally invasive approach for drug delivery system: CNC/PAMAM nanoparticles. Eur Polym J 139:109992. https://doi.org/10.1016/j.eurpolymj.2020.109992
Xu Q, Huang W, Jiang L et al (2013) KGM and PMAA based pH-sensitive interpenetrating polymer network hydrogel for controlled drug release. Carbohydr Polym 97:565–570. https://doi.org/10.1016/j.carbpol.2013.05.007
Li J, Mooney DJ (2016) Designing hydrogels for controlled drug delivery. Nat Rev Mater 1:16071. https://doi.org/10.1038/natrevmats.2016.71
Bruschi M (2015) Strategies to modify the drug release from pharmaceutical systems. Woodhead, Sawston, pp 37–89
Acknowledgement
The authors thank the Department of Materials Science and Engineering, Tarbiat Modares University of Tehran and Dr. Reza Poursalehi for providing the facility to carry out the work.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conceptualization. FMZ: Material preparation, Methodology, Data collection and statistical Analysis, Writing-original draft. PA: Methodology, Data analysis, Supervision, Validation, and Writing—review and Editing the manuscript. GK: Material preparation, Data collection and Analysis, Editing the manuscript. AK: Methodology, Data analysis, Validation, Writing—review and Editing the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disklose.
Ethical approval
Not applicable.
Additional information
Handling Editor: Andréa de Camargo.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Motesadi Zarandi, F., Alizadeh, P., Kohoolat, G. et al. Novel multifunctional bioactive glass incorporated alginate/poly(amidoamine) hydrogels with controlled drug release for cartilage tissue regeneration. J Mater Sci 59, 1550–1569 (2024). https://doi.org/10.1007/s10853-023-09275-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10853-023-09275-9