Abstract
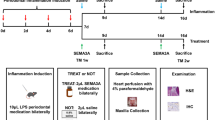
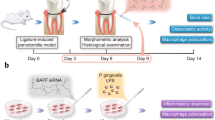
Periodontitis, characterized by progressive alveolar bone destruction, leads to the loss of attachment and stability of the affected teeth. Macrophages, especially the proinflammatory M1 subtype, are key in periodontitis pathogenesis, driving the disease's inflammatory and destructive processes. Despite existing insight into their involvement, comprehensive understanding of the underlying molecular mechanisms remains limited. TRPV1 is a non-selective cation channel protein and is known to regulate cellular function and homeostasis in macrophages. Our research objective was to investigate the impact of TRPV1 on the proinflammatory attributes of M1 macrophages in periodontal tissues, exploring potential mechanistic pathways. A mouse model of periodontitis was established using Porphyromonas gingivalis inoculation and ligature application around the maxillary second molar. Immunohistological analysis showed a significant reduction in macrophage TRPV1 expression in periodontitis-induced mice. Treatment with capsaicin, a TRPV1 agonist, was observed to effectively elevate TRPV1 expression in these macrophages. Furthermore, micro-computed tomography analysis revealed a marked decrease in alveolar bone resorption in the capsaicin -treated group, compared with vehicle and healthy control groups. Our in vitro findings show that capsaicin treatment successfully attenuated LPS-induced TNF-α and IL-6 production in macrophages, mediated through NRF2 activation, consequently reducing intracellular ROS levels. These findings suggest that TRPV1 agonists, through modulating M1 macrophage activity and up-regulating TRPV1, could be a novel therapeutic approach in periodontal disease management.








Similar content being viewed by others
Data Availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- H&E:
-
Haematoxylin/eosin
- TRAP:
-
Tartrate-resistant acid phosphatase
- CAP:
-
Capsaicin
- TRPV1:
-
Transient receptor potential vanilloid type1
- LPS:
-
Lipopolysaccharide;
- TNF-α:
-
Tumor necrosis factor-α
- IL-6:
-
Interleukin-6
- qRT-PCR:
-
Quantitative real-time polymerase chain reaction
- ROS:
-
Reactive Oxygen Species
- IFN-γ:
-
Interferon-γ;
- ANOVA:
-
One-way analysis of variance
- Micro-CT:
-
Micro–Computed Tomography
- 3D:
-
Three dimensional
- CEJ:
-
Cemento-enamel junction
- ABC:
-
Alveolar bone crest
- P. gingivalis :
-
Porphyromonas gingivalis
- DAPI, 4’:
-
6-Diamidino-2-phenylindole;
- NRF2:
-
Nuclear factor erythroid 2-related factor 2
- HO-1:
-
Heme oxygenase-1
- RANKL:
-
Receptor activator of nuclear factor-κB ligand
- Keap1:
-
Kelch-like ECH-associated protein 1
- SD:
-
Standard deviation
References
Papapanou, P.N., M. Sanz, N. Buduneli, T. Dietrich, M. Feres, D.H. Fine, et al. 2018. Periodontitis: consensus report of workgroup 2 of the 2017 world workshop on the classification of periodontal and peri-implant diseases and conditions. Journal of Periodontology 89 (Suppl 1): S173–S182.
Jepsen, S., J.G. Caton, J.M. Albandar, N.F. Bissada, P. Bouchard, P. Cortellini, et al. 2018. Periodontal manifestations of systemic diseases and developmental and acquired conditions: Consensus report of workgroup 3 of the 2017 World Workshop on the Classification of Periodontal and Peri-Implant Diseases and Conditions. Journal of Clinical Periodontology 45 (Suppl 20): S219–S229.
Darveau, R.P. 2010. Periodontitis: A polymicrobial disruption of host homeostasis. Nature Reviews Microbiology 8 (7): 481–490.
Iniesta, M., C. Chamorro, N. Ambrosio, M.J. Marín, M. Sanz, and D. Herrera. 2023. Subgingival microbiome in periodontal health, gingivitis and different stages of periodontitis. Journal of Clinical Periodontology 50 (7): 905–920.
Lamont, R.J., H. Koo, and G. Hajishengallis. 2018. The oral microbiota: Dynamic communities and host interactions. Nature Reviews Microbiology 16 (12): 745–759.
Eke, P.I., L. Wei, W.S. Borgnakke, G. Thornton-Evans, X. Zhang, H. Lu, et al. 2016. Periodontitis prevalence in adults ≥ 65 years of age, in the USA. Periodontology 2000 72 (1): 76–95.
Kassebaum, N.J., E. Bernabé, M. Dahiya, B. Bhandari, C.J. Murray, and W. Marcenes. 2014. Global burden of severe periodontitis in 1990–2010: A systematic review and meta-regression. Journal of Dental Research 93 (11): 1045–1053.
Marruganti, C., M. Romandini, C. Gaeta, E.F. Cagidiaco, N. Discepoli, S. Parrini, et al. 2023. Healthy lifestyles are associated with a better response to periodontal therapy: A prospective cohort study. Journal of Clinical Periodontology 50 (8): 1089–1100.
Elsadek, M.F., and M.F. Farahat. 2022. Effectiveness of photodynamic therapy as an adjunct to periodontal scaling for treating periodontitis in geriatric patients. European Review for Medical and Pharmacological Sciences 26 (6): 1832–1838.
Sälzer, S., C. Graetz, C.E. Dörfer, D.E. Slot, and F.A. Van der Weijden. 2020. Contemporary practices for mechanical oral hygiene to prevent periodontal disease. Periodontology 2000 84 (1): 35–44.
Slots, J. 2022. Concise evaluation and therapeutic guidelines for severe periodontitis: A public health perspective. Periodontology 2000 90 (1): 262–265.
Balta, M.G., E. Papathanasiou, I.J. Blix, and T.E. Van Dyke. 2021. Host Modulation and Treatment of Periodontal Disease. Journal of Dental Research 100 (8): 798–809.
Li, X., H. Wang, X. Yu, G. Saha, L. Kalafati, C. Ioannidis, et al. 2022. Maladaptive innate immune training of myelopoiesis links inflammatory comorbidities. Cell 185 (10): 1709–1727.
Carcuac, O., and T. Berglundh. 2014. Composition of human peri-implantitis and periodontitis lesions. Journal of Dental Research 93 (11): 1083–1088.
Liu, H., X. Wu, N. Gang, S. Wang, W. Deng, L. Zan, et al. 2015. Macrophage functional phenotype can be consecutively and reversibly shifted to adapt to microenvironmental changes. International Journal of Clinical and Experimental Medicine 8 (2): 3044–3053.
Gonzalez, O.A., S. Kirakodu, L. Nguyen, and J.L. Ebersole. 2023. Macrophage-related gingival transcriptomic patterns and microbiome alterations in experimental periodontitis in nonhuman primates. Journal of Periodontal Research 58 (6): 1148–1170.
Garaicoa-Pazmino, C., T. Fretwurst, C.H. Squarize, T. Berglundh, W.V. Giannobile, L. Larsson, et al. 2019. Characterization of macrophage polarization in periodontal disease. Journal of Clinical Periodontology 46 (8): 830–839.
Zhou, L.N., C.S. Bi, L.N. Gao, Y. An, F. Chen, and F.M. Chen. 2019. Macrophage polarization in human gingival tissue in response to periodontal disease. Oral Disease 25 (1): 265–273.
Huynh, N.C., V. Everts, P. Pavasant, and R.S. Ampornaramveth. 2017. Interleukin-1β induces human cementoblasts to support osteoclastogenesis. International Journal of Oral Science 9 (12): e5.
Cohen, M.R., and V.Y. Moiseenkova-Bell. 2014. Structure of thermally activated TRP channels. 2014. Current Topics in Membranes 74: 181–211.
Clapham, D.E. 2003. TRP channels as cellular sensors. Nature 426 (6966): 517–524.
Lv, Z., J. Han, J. Li, H. Guo, Y. Fei, Z. Sun, et al. 2022. Single cell RNA-seq analysis identifies ferroptotic chondrocyte cluster and reveals TRPV1 as an anti-ferroptotic target in osteoarthritis. eBioMedicine 84: 104258.
Dmitrzak-Węglarz, M., J. Rybakowski, A. Szczepankiewicz, P. Kapelski, M. Lesicka, E. Jabłońska, et al. 2023. Identification of shared disease marker genes and underlying mechanisms between major depression and rheumatoid arthritis. Journal of Psychiatric Research 168: 22–29.
Li, T., S. Jiang, Y. Zhang, J. Luo, M. Li, H. Ke, et al. 2023. Nanoparticle-mediated TRPV1 channel blockade amplifies cancer thermo-immunotherapy via heat shock factor 1 modulation. Nature Communication 14 (1): 2498.
Chen, C.C., C.H. Ke, C.H. Wu, H.F. Lee, Y. Chao, M.C. Tsai, et al. 2024. Transient receptor potential vanilloid 1 inhibition reduces brain damage by suppressing neuronal apoptosis after intracerebral hemorrhage. Brain Pathology 2: e13244.
Lucius, A., S. Chhatwal, M. Valtink, P.S. Reinach, A. Li, U. Pleyer, et al. 2023. L-Carnitine Suppresses Transient Receptor Potential Vanilloid Type 1 Activation in Human Corneal Epithelial Cells. International Journal of Molecular Science 24 (14): 11815.
Dohnalová, L., P. Lundgren, J.R.E. Carty, N. Goldstein, S.L. Wenski, P. Nanudorn, et al. 2022. A microbiome-dependent gut-brain pathway regulates motivation for exercise. Nature 612 (7941): 739–747.
Yan, S., L. Miao, Y. Lu, and L. Wang. 2019. Sirtuin 1 inhibits TNF-α-mediated osteoclastogenesis of bone marrow-derived macrophages through both ROS generation and TRPV1 activation. Molecular and Cellular Biochemistry 455 (1–2): 135–145.
Limberg, M.M., D. Wiebe, N. Gray, T. Weihrauch, A.U. Bräuer, A.E. Kremer, et al. 2024. Functional expression of TRPV1 in human peripheral blood basophils and its regulation in atopic dermatitis. Allergy 79 (1): 225–228.
Bertin, S., Y. Aoki-Nonaka, P.R. de Jong, L.L. Nohara, H. Xu, S.R. Stanwood, et al. 2014. The ion channel TRPV1 regulates the activation and proinflammatory properties of CD4+ T cells. Nature Immunology 15 (11): 1055–1063.
Tortora, C., A. Di Paola, M. Creoli, et al. 2022. Effects of CB2 and TRPV1 Stimulation on Osteoclast Overactivity Induced by Iron in Pediatric Inflammatory Bowel Disease. Inflammatory Bowel Diseases 28 (8): 1244–1253.
Takahashi, N., Y. Matsuda, K. Sato, P.R. de Jong, S. Bertin, K. Tabeta, et al. 2016. Neuronal TRPV1 activation regulates alveolar bone resorption by suppressing osteoclastogenesis via CGRP. Scientific Report 6: 29294.
Kim, Y.G., M.O. Kim, S.H. Kim, H.J. Kim, N.K. Pokhrel, J.H. Lee, et al. 2020. 6-Shogaol, an active ingredient of ginger, inhibits osteoclastogenesis and alveolar bone resorption in ligature-induced periodontitis in mice. Journal of Periodontology 91 (6): 809–818.
Yoshimoto, T., M. Kittaka, A.A.P. Doan, R. Urata, M. Prideaux, R.E. Rojas, et al. 2022. Osteocytes directly regulate osteolysis via MYD88 signaling in bacterial bone infection. Nature Communications 13 (1): 6648.
Zhang, L., W. Lu, C. Lu, Y. Guo, X. Chen, J. Chen, et al. 2022. Beneficial effect of capsaicin via TRPV4/EDH signals on mesenteric arterioles of normal and colitis mice. Journal of Advanced Research 39: 291–303.
Xin, L., F. Zhou, C. Zhang, W. Zhong, S. Xu, X. Jing, et al. 2022. Four-Octyl itaconate ameliorates periodontal destruction via Nrf2-dependent antioxidant system. International Journal of Oral Science 14 (1): 27.
Yang, M., Z. Shen, X. Zhang, Z. Song, Y. Zhang, Z. Lin, et al. 2023. Ferroptosis of macrophages facilitates bone loss in apical periodontitis via NRF2/FSP1/ROS pathway. Free Radical Biology and Medicine 208: 334–347.
Fontana, F., M. Marzagalli, M. Raimondi, V. Zuco, N. Zaffaroni, and P. Limonta. 2021. δ-Tocotrienol sensitizes and re-sensitizes ovarian cancer cells to cisplatin via induction of G1 phase cell cycle arrest and ROS/MAPK-mediated apoptosis. Cell Proliferation 54 (11): e13111.
Sczepanik, F.S.C., M.L. Grossi, M. Casati, M. Goldberg, M. Glogauer, N. Fine, et al. 2020. Periodontitis is an inflammatory disease of oxidative stress: We should treat it that way. Periodontology 2000 84 (1): 45–68.
Weiss-Sadan, T., M. Ge, M. Hayashi, M. Gohar, C.H. Yao, A. de Groot, et al. 2023. NRF2 activation induces NADH-reductive stress, providing a metabolic vulnerability in lung cancer. Cell Metabolism 35 (3): 487–503.
Hajishengallis, G. 2015. Periodontitis: From microbial immune subversion to systemic inflammation. Nature Reviews Immunology 15 (1): 30–44.
Han, Y., Y. Huang, P. Gao, Q. Yang, L. Jia, Y. Zheng, et al. 2022. Leptin Aggravates Periodontitis by Promoting M1 Polarization via NLRP3. Journal of Dental Research 101 (6): 675–685.
Horwood, N.J. 2016. Macrophage Polarization and Bone Formation: A review. Clinical Reviews in Allergy and Immunology 51 (1): 79–86.
Champagne, C.M., J. Takebe, S. Offenbacher, and L.F. Cooper. 2002. Macrophage cell lines produce osteoinductive signals that include bone morphogenetic protein-2. Bone 30 (1): 26–31.
Sun, X., K. Li, M. Hase, R. Zha, Y. Feng, B.Y. Li, and H. Yokota. 2022. Suppression of breast cancer-associated bone loss with osteoblast proteomes via Hsp90ab1/moesin-mediated inhibition of TGFβ/FN1/CD44 signaling. Theranostics 12 (2): 929–943.
Lu, L.Y., F. Loi, K. Nathan, T.H. Lin, J. Pajarinen, E. Gibon, et al. 2017. Pro-inflammatory M1 macrophages promote Osteogenesis by mesenchymal stem cells via the COX-2-prostaglandin E2 pathway. Journal of Orthopaedic Research 35 (11): 2378–2385.
Wang, C., Q. Zhao, C. Chen, J. Li, J. Zhang, S. Qu, et al. 2023. CD301b+ macrophage: The new booster for activating bone regeneration in periodontitis treatment. International Journal of Oral Science 15 (1): 19.
Wu, Q., X. Zhou, D. Huang, Y. Ji, and F. Kang. 2017. IL-6 enhances osteocyte-mediated osteoclastogenesis by promoting JAK2 and RANKL activity in vitro. Cellular Physiology and Biochemistry 41 (4): 1360–1369.
Kimura, S., A. Nagai, T. Onitsuka, T. Koga, T. Fujiwara, H. Kaya, et al. 2000. Induction of experimental periodontitis in mice with Porphyromonas gingivalis-adhered ligatures. Journal of Periodontology 71 (7): 1167–1173.
Nagasaki, A., K. Nagasaki, B.D. Kear, W.D. Tadesse, V. Thumbigere-Math, J.L. Millán, et al. 2021. Delivery of alkaline phosphatase promotes periodontal regeneration in mice. Journal of Dental Research 100 (9): 993–1001.
Jin, S.S., D.Q. He, Y. Wang, T. Zhang, H.J. Yu, Z.X. Li, et al. 2020. Mechanical force modulates periodontal ligament stem cell characteristics during bone remodelling via TRPV4. Cell Proliferation 53 (10): e12912.
Liu, K., X. Gao, C. Hu, Y. Gui, S. Gui, Q. Ni, et al. 2022. Capsaicin ameliorates diabetic retinopathy by inhibiting poldip2-induced oxidative stress. Redox Biology 56: 102460.
Yin, C., B. Liu, P. Wang, X. Li, Y. Li, X. Zheng, et al. 2020. Eucalyptol alleviates inflammation and pain responses in a mouse model of gout arthritis. British Journal of Pharmacology 177 (9): 2042–2057.
Xu, X., Y. Li, Z. Yang, and Z. Zhou. 2022. Transient receptor potential vanilloid type-1 regulates periodontal disease damage via the PI3K/AKT signaling pathway. Iranian Journal of Basic Medical Sciences 25 (5): 635–642.
Yamaguchi, T., Y. Yamamoto, K. Egashira, A. Sato, Y. Kondo, S. Saiki, et al. 2023. Oxidative stress inhibits endotoxin tolerance and may affect periodontitis. Journal of Dental Research 102 (3): 331–339.
Chen, K., P. Qiu, Y. Yuan, L. Zheng, J. He, C. Wang, et al. 2019. Pseurotin a inhibits osteoclastogenesis and prevents ovariectomized-induced bone loss by suppressing reactive oxygen species. Theranostics 9 (6): 1634–1650.
Weng, Y., H. Wang, L. Li, Y. Feng, S. Xu, and Z. Wang. 2021. Trem2 mediated Syk-dependent ROS amplification is essential for osteoclastogenesis in periodontitis microenvironment. Redox Biology 40: 101849.
Deng, Z., J. Lim, Q. Wang, K. Purtell, S. Wu, G.M. Palomo, et al. 2020. ALS-FTLD-linked mutations of SQSTM1/p62 disrupt selective autophagy and NFE2L2/NRF2 anti-oxidative stress pathway. Autophagy 16 (5): 917–931.
Shen, K., Y. Jia, X. Wang, J. Zhang, K. Liu, J. Wang, et al. 2021. Exosomes from adipose-derived stem cells alleviate the inflammation and oxidative stress via regulating Nrf2/HO-1 axis in macrophages. Free Radical Biology and Medicine 165: 54-66.
Hung, S.Y., J.L. Chen, Y.K. Tu, H.Y. Tsai, P.H. Lu, I.M. Jou, et al. 2024. Isoliquiritigenin inhibits apoptosis and ameliorates oxidative stress in rheumatoid arthritis chondrocytes through the Nrf2/HO-1-mediated pathway. Biomedicine & Pharmacotherapy 170: 116006.
Funding
This work was supported by National Science Foundation of China (Grant No. 82170939, 82100995), International Cooperation Project of Science and Technology in Guangdong Province (Grant No. 2023A0505050158), Guangdong Basic and Applied Basic Research Foundation (Grant No. 2023A1515010327), Natural Science Foundation of Guangdong Province (Grant No. 2023A1515012257), Science and Technology Projects in Guangzhou (Grant No. SL2023A04J01702), Natural Science Foundation of Guangdong Province (Grant No. 2021A1515010876).
Author information
Authors and Affiliations
Contributions
Yiyang Li contributed to conception, design, data acquisition, analysis, interpretation, drafted and critically revised the manuscript; Lingling Chen, Zhengmei Lin contributed to conception, design, interpretation and critically revised the manuscript; Xiaotong Guo, Peimeng Zhan, Shuheng Huang, Jiayao Chen contributed to data acquisition, analysis and interpretation; Yujie Zhou, Wentao Jiang contributed to design and data acquisition. All authors gave final approval and agree to be accountable for all aspects of the work.
Corresponding authors
Ethics declarations
Ethics Approval
This study was approved by the Institutional Animal Care and Use Committee, Sun Yat-Sen University.
Competing Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
10753_2024_2024_MOESM1_ESM.tif
Supplementary file1 Fig. 1 The toxic effect of capsaicin on macrophages in 24 h conducted by cell counting Kit-8. ***p < 0.001; ****p < 0.0001; ns, no significant. Data represents mean ± SD performed in triplicate. (TIF 209 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, Y., Guo, X., Zhan, P. et al. TRPV1 Regulates Proinflammatory Properties of M1 Macrophages in Periodontitis Via NRF2. Inflammation (2024). https://doi.org/10.1007/s10753-024-02024-3
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10753-024-02024-3