Abstract
The first appearance of SARS-CoV-2 is dated back to 2019. This new member of the coronavirus family has caused more than 5 million deaths worldwide up until the end of January 2022. At the moment, and after intensive vaccination programmes throughout the world, the pandemic is still active, whilst new mutations constantly appear. Researchers are working intensively to discover antiviral drugs to combat the severe cases in intensive care units, giving the overloaded hospital units a breather. Alongside various research projects focusing on developing small pharmaceutical molecules, a significant proportion of the research community has shifted towards paying attention to metal drugs. In this small review, we make brief reference to the use of metal drugs in therapeutics and provide some examples of metal drugs that are of extreme interest in the current pandemic. At the same time, we will also examine some of their promising mechanisms of action and possible effectiveness against COVID-19.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
General for COVID-19 and the pandemic
In December 2019, the outbreak of a new coronavirus, known as SARS-CoV-2, broke out in Wuhan (Santos 2020). This outbreak has turned into a pandemic, affecting most countries dealing with it (Bonotti and Zech 2021). Based on history, the most effective method of dealing with viral epidemic crises is vaccination (Taylor 2014). Many countries have had to speed up the licensing procedures for the circulation of vaccines to limit the spread of the virus. Up until the beginning of June 2021, 18 vaccines had been approved in at least one country worldwide for mass vaccination of the citizens (COVID-19 Vaccine Tracker 2021). Due to the intensive vaccination programmes, until mid-June 2021, about 22% of the world's population had received at least one dose of vaccine against SARS-CoV-2 (Coronavirus (COVID-19) Vaccinations - Statistics and Research 2021). Despite the rapid and massive vaccinations of the public, the pandemic is still active, and there remains a need to find a drug against COVID-19. The primary purpose of this drug will be to treat mainly those cases that relapse and end up in intensive care units with serious health risks. Vaccines offer protective coverage and have no efficacy in patients suffering from the disease (Weisblum et al. 2020). This effort would significantly relieve hospitals and better manage the pandemic itself. So far, only one drug, remdesivir, is approved for emergency use by the Food and Drug Administration (FDA) for this disease. At the same time, regarding the drug remdesivir, large-scale clinical trials in coronavirus patients have not been carried out so far (Commissioner 2021; Naveed et al. 2021). The pharmaceutical formulation, molnupiravir, which so far seems to be the first oral pharmaceutical formulation for the treatment of severe symptoms, has been tested in various clinical studies (COVID-19 First In Human Study to Evaluate Safety, Tolerability, and Pharmacokinetics of EIDD-2801 in Healthy Volunteers - Full-Text View - ClinicalTrials.gov [Internet] 2021; Safety 2021; Efficacy and Safety of Molnupiravir (MK-4482) in Non-Hospitalized Adult Participants With COVID-19 (MK-4482-002) - Full Text View - ClinicalTrials.gov [Internet]. 2021). This formulation has been approved by the United Kingdom (First oral antiviral for COVID-19, Lagevrio (molnupiravir), approved by MHRA [Internet]. 2021) whilst still under investigation by the FDA and European Medicines Agency (EMA) (FDA to Hold Advisory Committee Meeting to Discuss Merck and Ridgeback's EUA Application for COVID-19 Oral Treatment [Internet]. 2021; COVID-19: EMA starts rolling review of molnupiravir - European Medicines Agency [Internet]. 2021). Despite the publicity that molnupiravir has recently received, its effectiveness appears limited only in patients with early-stage COVID-19.
In contrast, in patients hospitalised with an advanced stage of the disease, its effectiveness is minimal and causes drawbacks for the research community (Singh et al. 2021). It is therefore apparent that there is an immediate need to find a new medicine to deal with the pandemic. The recent studies of Messori (Cirri et al. 2021), Bergamini (Paiva et al. 2020), (Karges and Cohen 2021) and (Paiva et al. 2020) have shown that metallodrugs may also be possible options for use against COVID-19. In this small review, we explore the potential usefulness of metallodrugs against SARS-CoV-2. At the same time, we will focus on their potential advantages over other organic molecules.
Target-disease association
Owing to the dangerousness of the situation, a large part of the scientific community is engaged in identifying and verifying possible molecular targets for the fight against SARS-CoV-2. Many candidate targets were proposed, and research continues in this direction (Prajapat et al. 2020). The study focuses on the RNA genotypic sequence of SARS-CoV-2 and has already been identified (GenBank: MN908947.3). By studying the virulent life cycle of the new coronavirus, some specific targets have emerged and are engaging in the possibility of their use as therapeutic targets. In its general set, the genome of the virus revealed 29,891 nucleotides which encode 9860 amino acids. As a result, four structural proteins and even 16 non-structural proteins have been characterised, which appear to have regulatory properties. Researchers identified at least three essential protein targets from the early stages of the research: (1) spike protein; (2) RNA-dependent-RNA-polymerase (RdRp); and (3) 3-chymotrypsin-like protein (3CL-PR) (Artese et al. 2020). At this stage, the structural verification of the characteristics of these proteins has begun to help target them better (Wrapp et al. 2020). More specifically, the spike protein is responsible for the virus's connectivity to the host cells of the human body. It achieves this by binding to angiotensin-converting enzyme 2 (ACE2) receptors via the S protein of the virus. This feature is common for both SARS-CoV-1 and SARS-CoV-2, demonstrating that the specific protein and the receptor are essential drug targets (Li et al. 2003; Yang et al. 2003; Lan et al. 2020; Krumm et al. 2021).
An excellent drug target is RdRp. RdRp is responsible for both replication of the virus RNA genome and removal of the RNA and is used to translate structural and auxiliary proteins at the 3′ end of the genome. With this polymerase inactive, the virus cannot reproduce and generate the necessary proteins (Gao et al. 2020; SARS-coronavirus replication is supported by a reticulovesicular network of modified endoplasmic reticulum 2021). Remdesivir can inhibit the activity of RNA polymerase, and relevant studies have shown the response to this formulation in the treatment of RNA coronavirus infections (Jordan et al. 2018; Pruijssers et al. 2020). RdRp inhibitors have been used several times, thus being amongst the most used drugs against viral RNA infections (Kumar et al. 2021; Favipiravir 2021). In turn, it shows how a particular inhibitor for SARS-CoV-2 polymerase could be a promising solution to the pandemic crisis. Owing to the high rate at which virus mutations occur, the design of an inhibitor of this polymerase must be carried out with extreme caution. It is confirmed that we have already observed a mutation of the RdRp protein of SARS-CoV-2, but it is not clear whether this mutation has influenced the targeting of this protein (Pachetti et al. 2020).
Following and based on the knowledge that we have so far regarding the characteristics of the coronavirus, another critical and promising protein target for the development of drugs against SARS-CoV-2 is the 3CLpro protease. This protease has a vital role in the virus's life cycle since it processes the two main viral polyproteins, pp1a and pp1ab (Kuzikov et al. 2021). 3CLpro proteolytically processes these polyproteins to create a series of non-structural proteins that appear essential for virus replication and transcription processes, including RdRp protein (Boras et al. 2020). Based on previous drug development that targets virus protease for human immunodeficiency virus (HIV) and hepatitis C virus, the result of a drug that selectively targets this SARS-Cov-2 protease is a desirable target for developing new pharmaceutical formulations (Brower et al. 2008).
Of course, the number of candidate targets for the development of drugs to combat SARS-CoV-2 is substantial. The scientific community is constantly adding new targets that may be of significant interest in developing pharmaceutical molecules. Closing this section, we consider it essential to mention the example of the protein target NTPase/helicase (nsp13). NTPase is a critical protein in the SARS-CoV-2 replication-transcription complex that catalyses the separation of double oligonucleotides into single strands in a manner dependent on nucleotide triphosphate hydrolysis (Gil et al. 2020). Previous studies proposed this target by examining the effectiveness of bismuth complexes in targeting this protein (Karaküçük-İyidoğan et al. 2011; Nareetsile et al. 2020). Based on this, we will list some medicinal metal compounds used in the past. We will explore the possible advantages that such compounds may have in the treatment of viral infections and at the same time, we will consider the use of these formulations in the current pandemic.
Metal-based drugs
-
Some examples of metal-based drugs in modern therapeutics
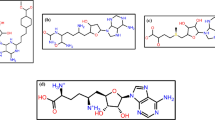
Metallodrugs, as a chemical class of pharmaceutical compounds, are not new in therapeutics. Since ancient times, there have been examples of such compounds in traditional therapeutics. An example is arsenic trioxide, used in Chinese medicine as an antiseptic agent and for the treatment of psoriasis and syphilis (Nagi et al. 2017). Other metals, such as gold and copper, treat syphilis in Chinese and Egyptian therapeutics (Pricker 1996; Norn et al. 2008; Sodhi and Paul 2019). More generally, metallodrugs, over time, have been found in many applications and used in various diseases, as summarised in Table 1.
Cisplatin is the best-known pharmaceutical compound in this category. This compound belongs chemically to the class of platinum compounds. Barnett Rosenberg first discovered it in 1960 (Padua et al. 1987) and therapeutically, it belongs to anti-cancer agents (Jungwirth et al. 2011). Cisplatin and its derivatives revolutionised modern therapeutics in many cancers. The characteristics of this compound have been studied extensively and have been very carefully mapped, both for its mechanism of action and its pharmacokinetic and pharmacodynamic characteristics (Franz and Metzler-Nolte 2019). Metallodrugs have many applications in modern therapeutics, e.g. as an anti-diabetic, anti-inflammatory, anti-manic (against mania), anti-parasitic (Navarro et al. 2010) and anti-hypertensive. At the same time, their use is constantly extended (Bharti and Singh 2009; Singh and Sharma 2018). Since the purpose of this small review is to explore the possible benefits of metallodrugs against the current pandemic of SARS-CoV-2, we will see some specific examples of pharmaceutical compounds based on metal ions against viral infections.
Several studies have examined possible metallodrug antiviral activity against HIV. The earliest study we found was done by controlling the possible interaction of complexes with surface proteins, gp120 and CD4, so as to explore the potential ability of complexes to inhibit the entry of the virus into the human cell (Clercq 1997). A more recent study by McGuire (McGuire et al. 2020) and his collaborators attempted to investigate the antiviral activity of copper complexes against the influenzas virus whilst controlling the likelihood of developing strain tolerance. The study showed promising results leaving room for further research of these metal complexes for antiviral activity. In 2010, Chang, Simmers and Knight released a review that was intended to present the antiviral and antimicrobial activity of cobalt complexes. The review as a whole showed the prospects of cobalt complexes for the development of antiviral drugs (Chang et al. 2010). More specifically, studies by Epstein and his collaborators show that a series of cobalt complexes, also known as CTC, show antiviral activity against herpes simplex virus type 1 (HSV-1), which causes herpetic epithelial keratitis (Asbell et al. 1998).
In contrast, later studies confirm their claim for efficacy against the virus (Schwartz et al. 2001). Moreover, this series of cobalt complexes, and especially CTC-96, has been tested for its effectiveness against adenovirus in vitro and in vivo on rabbit models showing positive results (Epstein et al. 2006). Studies have also been performed on potential antiviral platinum(II) and palladium(II) compounds. More specifically, in a study by Karaküçük-iyidoğan and his collaborators (Karaküçük-İyidoğan et al. 2011), conducted in 2011, a series of derivatives of platinum and palladium complexes were selected for possible antiviral potency. Studies were performed on several different strains of various viruses, such as HSV-1, HSV-2, RSV, H1N1, H3N2 and others. However, the researchers observed no characteristic antiviral activity for any of the variants of the compounds except one that showed activity against the human cytomegalovirus virus.
Researchers state the need for further studies on specific compounds and their analogues. In similar studies by Pelosi and his collaborators, two metal complexes (nickel, copper) of thiosemicarbazone were tested for their effectiveness against HIV-1 and HTLV retroviruses. The results showed that both complexes appeared effective against HIV-1, with the copper complex being effective, whilst neither of the two seemed to be effective against HTLV (Pelosi et al. 2010). With a brief review of the systematic literature, it appears that the study of metallodrugs for HIV candidate drugs remains quite promising. Many metals, such as vanadium, manganese, iron, copper, cobalt, nickel, zinc, ruthenium, platinum and gold are still good candidates for further development to combat this virus (Nareetsile et al. 2020). Generally, concerning the antiviral activity of medicinal compounds containing metals, the literature is limited. Some characteristic reports comment that this category of drugs will be helpful in the fight against viral infections, but no further studies have appeared to date.
Metallodrugs and COVID-19: is there so far any effort?
-
Auranofin hypothesis
Even though metallodrugs are constantly expanding their therapeutic usefulness, so far, no significant efforts to control their effectiveness against the current pandemic have been made. Despite that, the literature highlights some specific efforts of considerable interest. Marzo and Messori made the first attempt to include metal-based drugs in the fight against the pandemic. They proposed using the pharmaceutical compound, auranofin, for its possible action against SARS-CoV-2 (Marzo and Messori 2020). This proposal was made by the two researchers based on the general characteristics of the combination. Amongst other things, the researchers highlighted the excellent tolerance of the compound in the body, its low toxicity and its multi-targeting ability. An essential role in this choice was played because, based on previous studies, auranofin appears to show efficacy against HIV, a statement confirmed after pilot clinical trials (Diaz et al. 2019).
Furthermore, in their review, Sanarino and Shytaj concluded that auranofin is more effective than chloroquine in the treatment of HIV (Savarino and Shytaj 2015). Within a few months, the hypothesis of Marzo and Messori was significantly strengthened by two subsequent experimental studies. This time, the auranofin hypothesis results showed meaningful use of this organometallic compound. More specifically, a study on human cells showed that auranofin, at low micromolar concentrations, managed to suppress the virus by 95% after 48 h. It had significantly reduced the expression of cytokines in human cells (Rothan et al. 2020).
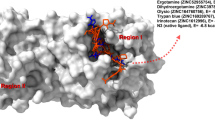
Furthermore, a study by Gil-Moles and her collaborators showed that auranofin could inhibit the interaction of the spike protein with the active centre of the enzyme, ACE2. As mentioned above, it is the leading portal of entry of the virus into the human cell. They also observed strong evidence of the compound's ability to inhibit the papain-like protein (PLpro) of SARS-CoV-1 and SARS-CoV-2, a crucial enzyme for virus replication. They reported that inhibition of this enzyme is the first experimentally confirmed inhibition of this target protein (Gil-Moles et al. 2020). Based on what was mentioned above, we suggest investigating auranofin further to verify its effectiveness against COVID-19.
-
Bismuth citrate hypothesis
Bismuth complexes are another class of promising metal complexes for their usefulness in the face of the current pandemic. This category has been studied to verify its effectiveness against SARS-CoV-1. In a 2007 study, researchers examined the ability of bismuth complexes to bind to the 100-residue cysteine-rich metal-binding domain of the SARS coronavirus (SCV) NTPase/helicase, enzymes that are essential for the life cycle of these viruses (Yang et al. 2007). Their study showed a significant ability of bismuth complexes to inhibit the enzymatic activity of SCV helicase, thus creating a later study of these complexes against SARS-CoV-2.
In a survey by Yuan and his collaborators (Yuan et al. 2020), the efficacy of a bismuth complex (ranitidine bismuth citrate) for the suppression of COVID-19 was investigated both in vitro and in vivo. The studies showed efficacy in both cell cultures and animal models. Specifically, the researchers stressed that this complex has low toxicity and protection against SARS-CoV-2 in cell cultures with high selectivity. In animal models using Syrian hamsters, this compound dramatically reduces the replication of the virus, leading to a decrease in the viral load on these animals’ respiratory systems. The researchers also pointed out that the in vitro studies showed a strong ability of the complex to inhibit the processes of viral helicases, confirming the previously existing studies on the importance of this enzyme as a pharmaceutical target (Frick 2003), and also the ability of bismuth complexes to target this enzyme successfully. The efficacy of these complexes has not been examined in clinical trials. Still, a case study published in the American Journal of Gastroenterology showed a possible improvement of a patient in whom Crohn’s disease had worsened due to confirmed SARS-CoV-2 infection (Wolf et al. 2020). His treating physicians administered bismuth subsalicylate 525 mg orally, 2–4 times per day. This therapeutic approach improved the patient's condition over 6 days, leading to decreased diarrhoea, cough, increased appetite, energy and symptoms that the patient had after being infected by the virus.
In Table 2, we can see some of the main antiviral metal-based structures.
Investigating metallodrugs as candidates against COVID-19
-
Studying the action mechanism of antiviral metallodrugs and their advantages in treating SARS-CoV-2
Metallodrugs have an important place in modern therapeutics. However, these molecules’ various action mechanisms are known only recently. At this point, we will explore some examples of the multiple mechanisms of actions of pharmaceutical molecules having antimicrobial and possible antiviral activity. Metal-based drugs can be divided into several categories based on their mechanism of action. In a review published in January 2020 (Boros et al. 2020), researchers attempted to group metallodrugs in this way, giving a clear view of the various mechanisms. At this point, we will only refer to those mechanisms that may, based on our judgment, have a relevant application for the current pandemic.
The first mechanism is the covalent connection of metallodrugs to biological targets (Riccardi et al. 2018). It is presented by the well-known anti-cancer drug, cisplatin, and the anti-rheumatic, auranofin. These two pharmaceutical molecules exhibit activity through the covalent bonds of their biological targets, causing stereochemical changes. This is followed by the inhibition of their biological processes (Fuertes et al. 2003). In the case of auranofin, the molecule's primary mechanism of action is its interference with oxidoreductive pathways of cell death. Auranofin's action mechanism includes the inhibition of the redox enzymes of thioredoxin (Harbut et al. 2015), the induction of endoplasmic reticulum (ER) stress (May et al. 2018), as well as the activation of the unfolded protein response (UPR). Thioredoxin has the role of transferring electrons to the enzymes involved in protecting the cell by oxidative stress. The proposed inhibitory effect of auranofin is based on the displacement of the ligands of the gold complex and the formation of a covalent bond to the molecule with cysteine residues of the active centre of thioredoxin reductase (Roder and Thomson 2015). By inhibiting these enzymes, auranofin leads the cell to a state of apoptosis. Still based on its action as an anti-rheumatic drug, auranofin exhibits anti-inflammatory activity by reducing the production of the cytokines, leading to the stimulation of cellular immunity (Walz et al. 1983).
Regarding the usefulness of such a mechanism of action against viral infections, both ER oxidative stress and UPR activation contribute to the virulent cycle of coronavirus (Fung and Liu 2014). Based on relevant research, it was observed that cells infected with viruses of this family could exhibit overexpression of the spike protein. Additionally, other viral proteins increase UPR activation levels (Siu et al. 2014). Thus, inhibition of thioredoxin reductase and other redox enzymes may disrupt the protein synthesis of SARS-CoV-2 (Rothan and Kumar 2019). Considering the anti-inflammatory activity of auranofin, we have observed the interest in it as a pharmaceutical molecule against COVID-19. It is now well-known from systematic observation how SARS-CoV-2 infection leads to acute inflammation of the respiratory system and a cytokine storm (Mehta et al. 2020) with overexpression of interleukin-6 (IL-6). As reported in a study by Nam-Hoon Kim and his colleagues, auranofin blocks IL-6 signalling by inhibiting the phosphorylation of both JAK1 and STAT3 (Kim et al. 2007). The main objective of such a drug is to treat severe cases of infection that end up in intensive care units. The inhibition of the inflammatory state in these patients would be potentially life-saving and significantly reduce the likelihood of their death from the virus. These drugs' double activity makes them an excellent choice for further study for their action against COVID-19, shifting the scientific community to searching for additional metallodrugs with similar action mechanisms.
The second mechanism of action of metallodrugs against viral infections and possibly against SARS-CoV-2 is that of redox-active metal centres. Several metals or metal ions can be in various oxidative states. Their different oxidation states can affect the kinetics of their substituents whilst also affecting chemical and biological processes in the environment (Carter 1995; Nencioni et al. 2011). From studies conducted in the past, we know that, along with other intracellular factors that affect the life cycle of viruses, the oxidation state is also an important factor (Khomich et al. 2018). As we know, viruses are intracellular parasites and have various mechanisms to exploit and to disrupt the cell's interior for their benefit. They create favourable conditions to carry out their functions more efficiently (Mahalingam et al. 2002). Thus, the viruses, in the state of infection, alter the redox balance towards the oxidative state (Gullberg et al. 2015). In the case of viruses of the respiratory system, it has been observed that they can cause oxidative stress due to overproduction of reactive oxygen species (ROS) and, at the same time, they significantly reduce glutathione which is the central antioxidant system in the cells. These conditions, which are created by the increase in ROS and the reduction of the glutathione system, are highly favourable to the replication pathways of the virus (Chen et al. 2020). The overproduction of ROS against infection conditions is due to NOX oxidase’s activity, consisting of 7 members, with the most important, NOX 2, playing a vital role in viral replication. Additionally, its absence leads to a lower duration and severity of respiratory infections (Vlahos et al. 2011). Another member of the NOX family, NOX4, looks even more attractive as a target.
The NOX4 isoform is overexpressed after infection in lung epithelial cells and generates ROS (Amatore et al. 2015). ROS production from NOX4 is modulated by ACE2, the primary receptor used by coronaviruses as an entrance to the cell (Meng et al. 2015). ROS production, in turn, activates protein kinases (MAPKs) and promotes nuclear extraction of the filial ribonucleoprotein leading to viral replication (Nencioni et al. 2009). As a result of this, studies have been conducted and have stated that there is a correlation between the overexpression of ROS and NOX2 in SARS-CoV-2. Damiano and her colleagues propose a possible therapeutic approach for the current pandemic through the reduction of oxidative stress in cells, which can lead to a reduction in the number of worsening patients with COVID-19 and, at the same time, protect high-risk patients (Damiano et al. 2020). Up to this point and based on the research we conducted, we have not identified any specific example of a metal-based drug that has been examined for its effectiveness in viral infections which has this particular mechanism. Thus, based on the importance of redox state for the life cycle of viruses, the investigation and the possible use of metallodrugs can affect the oxidoreductive state of cells and their properties and is likely to be a logical continuation in combatting COVID-19.
The third and final mechanism covered in this manuscript is the synthesis of photodynamic therapy (PDT) and photoactivated metal drugs. Metal complexes as a whole are excellent candidates for such treatments due to their specific properties (McKenzie et al. 2019). Such ideal properties are the abilities of some metals to absorb light in the visible spectrum whilst also exhibiting high diatomic absorptions of two photons in the near infra-red region. Unlike other molecules, the metals promote spin–orbit coupling that allows the triplet state that leads to the production of simple oxygen. Finally, another vital feature of metal-containing compounds in PDT therapy is their general photostability. We know that the most remarkable application of this class of drugs concerns mainly anti-cancer treatments (Photodynamic therapy in cancer treatment - an updated review 2021). However, a part of this category of medicines involves treating viral infections (Wiehe et al. 2019). The sensitivity of viruses to photodynamic processes was first reported in 1928 by Schultz and Krueger, and in 1933, by Perdrau and Thedd (Perdrau and Todd 1933); however, there was no interest in the field until several decades later. The first clinical application of PDT against viral infections occurred in the early seventies, targeting the herpes genitalis virus (Dai et al. 2009). Since then, this method has been studied for its effectiveness in several target viruses such as HPV, HIV, cytomegalovirus and others (Ichimura et al. 2003; Tardivo et al. 2006). Following relevant studies, enveloped viruses are more sensitive to PDT than those without one. Since SARS-CoV-2 is an enveloped virus, it may be a promising pharmaceutical approach (Käsermann and Kempf 1997; Bianchi et al. 2020).
The principle of this method is based on the activation of photosensitisers (PS) which have a light responding property and lead to the production of ROS. To activate a PS it must first absorb radiation at a specific wavelength. When the PS reaches its activation state by electron transfer, which lasts only for a few nanoseconds, it goes into the triple state. This state constitutes the last stage before entering one of the two photochemical pathways through ROS production. ROS production is significant as it leads to oxidative stress causing damage both to biomolecular structures (nucleic acids) and microbial systems. The method is fundamental because PS are not toxic molecules and only present toxicity at the target site after exposure to radiation of a specific wavelength (Allison and Moghissi 2013; Hamblin 2016). Many PS are used in various diseases, whilst others are developed (Lan et al. 2019). A summary of the action mechanisms of the metal compounds can be found in Fig. 1.
Regarding the usefulness of this technique for combatting COVID-19 infection, it should be noted that, based on our knowledge, there is no clinical study that examines the effectiveness of the method for the new coronavirus. However, we have identified critical in vitro studies that show the method’s possible effectiveness (Svyatchenko et al. 2021; Wu et al. 2021). In contrast, its potential efficacy against other coronaviruses, such as MERS-CoV, has been tested (Keil et al. 2016). Based on the structural features of SARS-CoV-2, we can assume that PDT can significantly affect the structural proteins of the virus through the production of ROS, resulting in its inactivation. Based on previous studies conducted to examine the effectiveness of the method for the treatment of coronavirus infections, it has been shown that photochemical inactivators, such as riboflavin, curcumin and various chlorophyll derivatives, are effective in suppressing viruses of this family (Ruane et al. 2004).
This approach is of interest, not only mechanistically, but also in administration. Since SARS-CoV-2 attacks epithelial cells of the nasal cavity and oropharyngeal membrane, one possible approach to administration is through nebulisation and the use of a catheter for the light supply (Blanco et al. 2017; Kassab et al. 2019). The combination of this technique may be of significant interest for the adjunctive treatment of COVID-19 as Dias mentioned in his recommendations, published in 2020 (Dias et al. 2020). Despite the specificity of the method and its limited use against viral infections, we were happy to identify that a significant number of researchers recommend this therapeutic approach against SARS-CoV-2 (Moghissi et al. 2020). No research effort has been recognised, however, that combines PDT with the use of metal-containing PS. The result is the exceptional properties of metals in such treatments (Josefsen and Boyle 2008). So, given both its particular mechanism of action and the original methods of administration that can be applied for PDT therapy, we can propose the development of new PS metal compounds for the development of protocols targeting the new coronavirus (Kipshidze et al. 2020; Tariq et al. 2021).
We should mention that despite the absence of specific examples of metal drugs in the fight against viral infections through the mechanisms discussed above, interest in studying such medicinal compounds is essential. In general, viruses appear to have a significant sensitivity to these mechanisms. So far, commonly used pharmaceutical molecules in the fight against viral infections have the disadvantage of being vulnerable to potential mutations of their viral targets (Irwin et al. 2016). In the case of SARS-CoV-2, the virus's increased mutation rate means that the design of conventional antiviral drugs is quite risky. From time to time, the virus may alter its protein targets leading to the non-efficacy of these drugs (Ivan Lozada et al. 2020). On the other hand, through the proposed mechanisms of action, metal-based drugs do not seem to act through their interaction with a specific molecular target of the virus. Their activity lies in the virus's general environment, an advantage that makes them less vulnerable to various mutations of the virus and, therefore, a better pharmaceutical approach.
Conclusion
The current pandemic proved to be a more significant challenge than the predictions. Despite severe restrictions and rigid controls, the situation got out of the government's control, and the next step is crucial for the future. Vaccination movements are progressing at a breakneck pace without limiting the pandemic on their own. The discovery and distribution of a pharmaceutical formulation to combat SARS-CoV-2 are imperative. The metal-based drugs, with their properties and various mechanisms of action, may present an ideal perspective for further study. Up to this time, there have been several research efforts but not a clinical survey involving metal drugs. It is, therefore, our strong suggestion to further study metal-based drugs for their utilisation against the current pandemic and to promote them in clinical trials.
References
A Safety, Tolerability, and Efficacy of Molnupiravir (EIDD-2801) to Eliminate Infectious Virus Detection in Persons With COVID-19 - Full-Text View - ClinicalTrials.gov [Internet]. Clinicaltrials.gov. 2021. https://clinicaltrials.gov/ct2/show/NCT04405570?term=Molnupiravir&draw=2&rank=6. Accessed 24 Nov 2021
Allison RR, Moghissi K (2013) Photodynamic therapy (PDT): PDT mechanisms. Clin Endosc 46(1):24–29. https://doi.org/10.5946/ce.2013.46.1.24
Amatore D, Sgarbanti R, Aquilano K, Baldelli S, Limongi D, Civitelli L, Nencioni L, Garcia E, Cirilo MR, Palamara AT (2015) Influenza virus replication in lung epithelial cells depends on redox-sensitive pathways activated by NOX4-derived ROS. Cell Microbiol 17(1):131–145. https://doi.org/10.1111/cmi.12343
Artese A, Svicher V, Costa G, Salpini R, Di Maio VC, Alkhatib M, Ambrosio FA, Santoro MM, Assaraf YG, Alcaro S, Ceccherini-Silberstein F (2020) Current status of antivirals and druggable targets of SARS-CoV-2 and other human pathogenic coronaviruses. Drug Resist Update 53:100721. https://doi.org/10.1016/j.drup.2020.100721
Asbell PA, Epstein SP, Wallace JA, Epstein D, Stewart CC, Burger RM (1998) Efficacy of cobalt chelates in the rabbit eye model for epithelial herpetic keratitis. Cornea 17(5):550–557. https://doi.org/10.1097/00003226-199809000-00014
Bharti S, Singh S (2009) Metal-based drugs: current use and future potential. Der Pharmacia Lett 1
Bianchi M, Benvenuto D, Giovanetti M, Angeletti S, Ciccozzi M, Pascarella S (2020) Sars-CoV-2 envelope and membrane proteins: structural differences linked to virus characteristics? Biomed Res Int 2020:e4389089. https://doi.org/10.1155/2020/4389089
Blanco KC, Inada NM, Carbinatto FM, Giusti AL, Bagnato VS (2017) Treatment of recurrent pharyngotonsillitis by photodynamic therapy. Photodiagn Photodyn Ther 18:138–139. https://doi.org/10.1016/j.pdpdt.2017.01.187
Bonotti M, Zech ST (2021) The human, economic, social, and political costs of COVID-19. Recovering Civility During COVID-19. https://doi.org/10.1007/978-981-33-6706-7_1.
Boras B, Jones RM, Anson BJ, Arenson D, Aschenbrenner L, Bakowski MA, Beutler N, Binder J, Chen E, Eng H, Hammond J, Hoffman R, Kadar EP, Kania R, Kimoto E, Kirkpatrick MG, Lanyon L, Lendy EK, Lillis JR, Luthra SA, Ma C, Noell S, Obach RS, Brien MNO, O’Connor R, Ogilvie K, Owen D, Pettersson M, Reese MR, Rogers TF, Rossulek MI, Sathish JG, Steppan C, Ticehurst M, Updyke LW, Zhu Y, Wang J, Chatterjee AK, Mesecar AD, Anderson AS, Allerton C (2020) Discovery of a novel inhibitor of coronavirus 3CL protease as a clinical candidate for the potential treatment of COVID-19. BioRxiv. https://doi.org/10.1101/2020.09.12.293498
Boros E, Dyson PJ, Gasser G (2020) Classification of metal-based drugs according to their mechanisms of action. Chem 6(1):41–60. https://doi.org/10.1016/j.chempr.2019.10.013
Brower ET, Bacha UM, Kawasaki Y, Freire E (2008) Inhibition of HIV-2 protease by HIV-1 protease inhibitors in clinical use. Chem Biol Drug Des 71(4):298–305. https://doi.org/10.1111/j.1747-0285.2008.00647.x
COVID-19: EMA starts rolling review of molnupiravir - European Medicines Agency [Internet]. European Medicines Agency. 2021. https://www.ema.europa.eu/en/news/covid-19-ema-starts-rolling-review-molnupiravir. Accessed 24 Nov 2021
COVID-19 Vaccine Tracker. https://vac-lshtm.shinyapps.io/ncov_vaccine_landscape/. Accessed 24 June 2021
COVID-19 First In Human Study to Evaluate Safety, Tolerability, and Pharmacokinetics of EIDD-2801 in Healthy Volunteers - Full-Text View - ClinicalTrials.gov [Internet]. Clinicaltrials.gov. 2021. https://clinicaltrials.gov/ct2/show/NCT04392219?term=Molnupiravir&draw=2&rank=5. Accessed 24 Nov 2021
Carter DE Oxidation-reduction reactions of metal ions. 3
Chang EL, Simmers C, Knight DA (2010) Cobalt complexes as antiviral and antibacterial agents. Pharmaceuticals 3(6):1711–1728. https://doi.org/10.3390/ph3061711
Chen K-K, Minakuchi M, Wuputra K, Ku C-C, Pan J-B, Kuo K-K, Lin Y-C, Saito S, Lin C-S, Yokoyama KK (2020) Redox control in the pathophysiology of influenza virus infection. BMC Microbiol 20(1):214. https://doi.org/10.1186/s12866-020-01890-9
Cirri D, Pratesi A, Marzo T, Messori L (2021) Metallo therapeutics for COVID-19. Exploiting metal-based compounds for the discovery of new antiviral drugs. Exp Opin Drug Discovery 16(1):39–46. https://doi.org/10.1080/17460441.2020.1819236
De Clercq E (1997) Antiviral metal complexes. Met-Based Drugs 4(3):173–192. https://doi.org/10.1155/MBD.1997.173
dos Santos WG (2020) Natural history of COVID-19 and current knowledge on treatment therapeutic options. Biomed Pharmacother 129:110493. https://doi.org/10.1016/j.biopha.2020.110493
Commissioner O. of the. FDA Approves First Treatment for COVID-19. https://www.fda.gov/news-events/press-announcements/fda-approves-first-treatment-covid-19. Accessed 24 June 2021
Coronavirus (COVID-19) Vaccinations - Statistics and Research. https://ourworldindata.org/covid-vaccinations. Accessed 24 June 2021
Dai T, Huang Y-Y, Hamblin MR (2009) Photodynamic therapy for localized infections – State of the Art. Photodiagnosis Photodyn Ther 6(3–4):170–188. https://doi.org/10.1016/j.pdpdt.2009.10.008
Damiano S, Sozio C, La Rosa G, Santillo M (2020) NOX-dependent signaling dysregulation in severe COVID-19: clues to effective treatments. Front Cell Infect Microbiol 10:608435. https://doi.org/10.3389/fcimb.2020.608435
Dias LD, Blanco KC, Bagnato VS (2020) COVID-19: beyond the virus. The use of photodynamic therapy for the treatment of infections in the respiratory tract. Photodiagnosis Photodyn Ther 31:101804. https://doi.org/10.1016/j.pdpdt.2020.101804
Diaz RS, Shytaj IL, Giron LB, Obermaier B, Della Libera E, Galinskas J, Dias D, Hunter J, Janini M, Gossen G, Ferreira PA, Sucupira MC, Maricato J, Fackler O, Lusic M, Savarino A (2019) Potential impact of the antirheumatic agent auranofin on proviral HIV-1 DNA in individuals under intensified antiretroviral therapy: results from a randomised clinical trial. Int J Antimicrobial Agents 54(5):592–600. https://doi.org/10.1016/j.ijantimicag.2019.08.001
Efficacy and Safety of Molnupiravir (MK-4482) in Non-Hospitalized Adult Participants With COVID-19 (MK-4482-002) - Full Text View - ClinicalTrials.gov [Internet]. Clinicaltrials.gov. 2021. https://clinicaltrials.gov/ct2/show/NCT04575597?term=Molnupiravir&draw=2&rank=2. Accessed 24 Nov 2021
Epstein SP, Pashinsky YY, Gershon D, Winicov I, Srivilasa C, Kristic KJ, Asbell PA (2006) Efficacy of topical cobalt chelate CTC-96 against adenovirus in a cell culture model and adenovirus keratoconjunctivitis in a rabbit model. BMC Ophthalmol 6:22. https://doi.org/10.1186/1471-2415-6-22
FDA to Hold Advisory Committee Meeting to Discuss Merck and Ridgeback's EUA Application for COVID-19 Oral Treatment [Internet]. U.S. Food and Drug Administration. 2021. https://www.fda.gov/news-events/press-announcements/fda-hold-advisory-committee-meeting-discuss-merck-and-ridgebacks-eua-application-covid-19-oral. Accessed 24 Nov 2021
Favipiravir (T-705), A Broad-Spectrum Inhibitor of Viral RNA Polymerase. https://www.jstage.jst.go.jp/article/pjab/93/7/93_PJA9307B-02/_article/-char/ja/. Accessed 26 June 2021
First oral antiviral for COVID-19, Lagevrio (molnupiravir), approved by MHRA [Internet]. GOV.UK. 2021. Available from: https://www.gov.uk/government/news/first-oral-antiviral-for-covid-19-lagevrio-molnupiravir-approved-by-mhra. Accessed 24 Nov 2021
Franz KJ, Metzler-Nolte N (2019) Introduction: metals in medicine. Chem Rev 119(2):727–729. https://doi.org/10.1021/acs.chemrev.8b00685
Frick DN (2003) Helicases as antiviral drug targets. Drug News Perspect 16(6):355–362
Fuertes MA, Castilla J, Alonso C, Pérez JM (2003) Cisplatin biochemical mechanism of action: from cytotoxicity to induction of cell death through interconnections between apoptotic and necrotic pathways. Curr Med Chem 10(3):257–266. https://doi.org/10.2174/0929867033368484
Fung TS, Liu DX (2014) Coronavirus infection, ER stress, apoptosis, and innate immunity. Front Microbiol 5:296. https://doi.org/10.3389/fmicb.2014.00296
Gao Y, Yan L, Huang Y, Liu F, Zhao Y, Cao L, Wang T, Sun Q, Ming Z, Zhang L, Ge J, Zheng L, Zhang Y, Wang H, Zhu Y, Zhu C, Hu T, Hua T, Zhang B, Yang X, Li J, Yang H, Liu Z, Xu W, Guddat LW, Wang Q, Lou Z, Rao Z (2020) Structure of the RNA-dependent RNA polymerase from COVID-19 virus. Science 368(6492):779–782. https://doi.org/10.1126/science.abb7498
Gil C, Ginex T, Maestro I, Nozal V, Barrado-Gil L, Cuesta-Geijo M et al (2020) COVID-19: drug targets and potential treatments. J Med Chem 63(21):12359–12386
Gil-Moles M, Basu U, Büssing R, Hoffmeister H, Türck S, Varchmin A, Ott I (2020) Gold metallodrugs to target coronavirus proteins: inhibitory effects on the spike-ACE2 interaction and PLpro protease activity by auranofin and gold organometallics. Chem 26(66):15140–15144. https://doi.org/10.1002/chem.202004112
Gullberg RC, Jordan Steel J, Moon SL, Soltani E, Geiss BJ (2015) Oxidative stress influences positive strand RNA virus genome synthesis and capping. Virology 475:219–229. https://doi.org/10.1016/j.virol.2014.10.037
Hamblin MR (2016) Antimicrobial photodynamic inactivation: a bright new technique to kill resistant microbes. Curr Opin Microbiol 33:67–73. https://doi.org/10.1016/j.mib.2016.06.008
Harbut MB, Vilchèze C, Luo X, Hensler ME, Guo H, Yang B, Chatterjee AK, Nizet V, Jacobs WR, Schultz PG, Wang F (2015) Auranofin exerts broad-spectrum bactericidal activities by targeting thiol-redox homeostasis. Proc Natl Acad Sci USA 112(14):4453–4458. https://doi.org/10.1073/pnas.1504022112
Ichimura H, Yamaguchi S, Kojima A, Tanaka T, Niiya K, Takemori M, Hasegawa K, Nishimura R (2003) Eradication and reinfection of human papillomavirus after photodynamic therapy for cervical intraepithelial Neoplasia. Int J Clin Oncol 8(5):322–325. https://doi.org/10.1007/s10147-003-0354-4
Irwin K, Renzetti N, Kowalik T, Jensen J (2016) Antiviral drug resistance as an adaptive process. Virus Evol 2(1):vew014
Ivan Lozada M, Daniela Torres L, Maria Bolaño R, Luis Moscote S (2020) High mutation rate in SARS-CoV-2: will it hit us the same way forever? J Infect Dis Epidemiol 6(6)
Jordan PC, Stevens SK, Deval J (2018) Nucleosides for the treatment of respiratory RNA virus infections. Antivir Chem Chemother 26:2040206618764483. https://doi.org/10.1177/2040206618764483
Josefsen LB, Boyle RW (2008) Photodynamic therapy and the development of metal-based photosensitisers. Met-Based Drugs 2008:e276109. https://doi.org/10.1155/2008/276109
Jungwirth U, Kowal CR, Keppler BK, Hartinger CG, Berger W, Heffeter P (2011) Anticancer activity of metal complexes: involvement of redox processes. Antioxid Redox Signal 15(4):1085–1127. https://doi.org/10.1089/ars.2010.3663
Karaküçük-İyidoğan A, Taşdemir D, Oruç-Emre EE, Balzarini J (2011) Novel platinum(ii) and palladium(ii) complexes of thiosemicarbazones derived from 5-substitutedthiophene-2-carboxaldehydes and their antiviral and cytotoxic activities. Eur J Med Chem 46(11):5616–5624. https://doi.org/10.1016/j.ejmech.2011.09.031
Karges J, Cohen SM (2021) Metal complexes as antiviral agents for SARS-CoV-2. ChemBioChem. https://doi.org/10.1002/cbic.202100186
Kassab G, Gerald MC, Inada NM, Achilles AE, Guerra VG, Bagnato VS (2019) Nebulization as a tool for photosensitizer delivery to the respiratory tract. J Biophotonics 12(4):e201800189. https://doi.org/10.1002/jbio.201800189
Keil SD, Bowen R, Marschner S (2016) Inactivation of middle east respiratory syndrome coronavirus (MERS-CoV) in plasma products using a riboflavin-based and ultraviolet light-based photochemical treatment. Transfusion 56(12):2948–2952. https://doi.org/10.1111/trf.13860
Khomich OA, Kochetkov SN, Bartosch B, Ivanov AV (2018) Redox biology of respiratory viral infections. Viruses 10(8):392. https://doi.org/10.3390/v10080392
Kim N-H, Lee M-Y, Park S-J, Choi J-S, Oh M-K, Kim I-S (2007) Auranofin blocks interleukin-6 signalling by inhibiting phosphorylation of JAK1 and STAT3. Immunology 122(4):607–614. https://doi.org/10.1111/j.1365-2567.2007.02679.x
Kipshidze N, Yeo N, Kipshidze N (2020) Photodynamic therapy for COVID-19. Nat Photonics 14(11):651–652. https://doi.org/10.1038/s41566-020-00703-9
Krumm ZA, Lloyd GM, Francis CP, Nasif LH, Mitchell DA, Golde TE, Giasson BI, Xia Y (2021) Precision therapeutic targets for COVID-19. Virol J 18(1):66. https://doi.org/10.1186/s12985-021-01526-y
Kumar R, Mishra S, Shreya; Maurya, S. K, (2021) Recent advances in the discovery of potent RNA-dependent RNA-polymerase (RdRp) inhibitors targeting viruses. RSC Med Chem 12(3):306–320. https://doi.org/10.1039/D0MD00318B
Kuzikov M, Costanzi E, Reinshagen J, Esposito F, Vangeel L, Wolf M, Ellinger B, Claussen C, Geisslinger G, Corona A, Iaconis D, Talarico C, Manelfi C, Cannalire R, Rossetti G, Gossen J, Albani S, Musiani F, Herzog K, Ye Y, Giabbai B, Demitri N, Jochmans D, Jonghe SD, Rymenants J, Summa V, Tramontano E, Beccari AR, Leyssen P, Storici P, Neyts J, Gribbon P, Zaliani A (2021) Identification of inhibitors of SARS-CoV-2 3CLpro enzymatic activity using a small molecule in vitro repurposing screen. ACS Pharmacol Transl Sci 4(3):1096–1110. https://doi.org/10.1021/acsptsci.0c00216
Käsermann F, Kempf C (1997) Photodynamic inactivation of enveloped viruses by buckminsterfullerene. Antiviral Res 34(1):65–70. https://doi.org/10.1016/s0166-3542(96)01207-7
Lan J, Ge J, Yu J, Shan S, Zhou H, Fan S, Zhang Q, Shi X, Wang Q, Zhang L, Wang X (2020) Structure of the SARS-CoV-2 spike receptor-binding domain bound to the ACE2 receptor. Nature 581(7807):215–220. https://doi.org/10.1038/s41586-020-2180-5
Lan M, Zhao S, Liu W, Lee C-S, Zhang W, Wang P (2019) Photosensitizers for photodynamic therapy. Adv Healthc Mater 8(13):e1900132. https://doi.org/10.1002/adhm.201900132
Li W, Moore MJ, Vasilieva N, Sui J, Wong SK, Berne MA, Somasundaran M, Sullivan JL, Luzuriaga K, Greenough TC, Choe H, Farzan M (2003) Angiotensin-converting enzyme 2 is a functional receptor for the SARS coronavirus. Nature 426(6965):450–454. https://doi.org/10.1038/nature02145
Mahalingam S, Meanger J, Foster PS, Lidbury BA (2002) The viral manipulation of the host cellular and immune environments to enhance propagation and survival: a focus on RNA viruses. J Leukoc Biol 72(3):429–439
Marzo T, Messori L (2020) A role for metal-based drugs in fighting COVID-19 infection? The case of auranofin. ACS Med Chem Lett 11(6):1067–1068. https://doi.org/10.1021/acsmedchemlett.0c00190
May HC, Yu J-J, Guentzel MN, Chambers JP, Cap AP, Arulanandam BP (2018) Repurposing auranofin, ebselen, and PX-12 as antimicrobial agents targeting the thioredoxin system. Front Microbiol 9:336. https://doi.org/10.3389/fmicb.2018.00336
McGuire L, Hogge J, Hintze A, Liddle N, Nelson N, Pollock J, Brown A, Facer S, Walker S, Lynch J, Harrison RG, Busath DD (2020) Copper Complexes as Influenza Antivirals: Reduced Zebrafish Toxicity. In: Marius Avramescu S, Akhtar K, Fierascu I, Bahadar Khan S, Ali FM, Asiri A (eds) Engineered Nanomaterials - Health and Safety, IntechOpen. https://doi.org/10.5772/intechopen.88786.
McKenzie LK, Bryant HE, Weinstein JA (2019) Transition metal complexes as photosensitisers in one- and two-photon photodynamic therapy. Coord Chem Rev 379:2–29. https://doi.org/10.1016/j.ccr.2018.03.020
Mehta P, McAuley DF, Brown M, Sanchez E, Tattersall RS, Manson JJ (2020) COVID-19: consider cytokine storm syndromes and immunosuppression. Lancet 395(10229):1033–1034. https://doi.org/10.1016/S0140-6736(20)30628-0
Meng Y, Li T, Zhou G-S, Chen Y, Yu C-H, Pang M-X, Li W, Li Y, Zhang W-Y, Li X (2015) The angiotensin-converting enzyme 2/angiotensin (1–7)/Mas axis protects against lung fibroblast migration and lung fibrosis by inhibiting the NOX4-derived ROS-mediated RhoA/Rho kinase pathway. Antioxid Redox Signal 22(3):241–258. https://doi.org/10.1089/ars.2013.5818
Moghissi K, Dixon K, Gibbins S (2020) Does PDT have potential in treating COVID 19 patients? Photodiagn Photodyn Ther 31:101889. https://doi.org/10.1016/j.pdpdt.2020.101889
Nagi U, Mhlongo N, Soliman ME (2017) Metal complexes in cancer therapy—an update from drug design perspective. DDDT 11:599–616. https://doi.org/10.2147/DDDT.S119488
Nareetsile F, Ndlovu S, Matshwele JTP, Ngaski M (2020) Transition metal complexes with HIV/AIDS inhibitory properties 21
Navarro M, Gabbiani C, Messori L, Gambino D (2010) Metal-based drugs for malaria, trypanosomiasis, and leishmaniasis: recent achievements and perspectives. Drug Discovery Today 15(23):1070–1078. https://doi.org/10.1016/j.drudis.2010.10.005
Naveed M, Uddin S, Khan MK, Khan Z (2021) Remdesivir for the treatment of COVID-19: a need for combined in vivo and in vitro studies to evaluate the efficacy. J Pharm Pract 34(3):343–346. https://doi.org/10.1177/0897190021997001
Nencioni L, De Chiara G, Sgarbanti R, Amatore D, Aquilano K, Marcocci ME, Serafino A, Torcia M, Cozzolino F, Ciriolo MR, Garaci E, Palamara AT (2009) Bcl-2 expression and P38MAPK activity in cells infected with influenza a virus: impact on virally induced apoptosis and viral replication. J Biol Chem 284(23):16004–16015. https://doi.org/10.1074/jbc.M900146200
Nencioni L, Sgarbanti R, Amatore D, Checconi P, Celestino I, Limongi D, Anticoli S, Palamara AT, Garaci E (2011) Intracellular redox signaling as therapeutic target for novel antiviral strategy. Curr Pharm Des 17(35):3898–3904. https://doi.org/10.2174/138161211798357728
Norn S, Permin H, Kruse E, Kruse PR (2008) Mercury-a significant agent in the history of medicine and alchemy. Dan Medicinhist Arbog 36:21–40
Pachetti M, Marini B, Benedetti F, Giudici F, Mauro E, Storici P, Masciovecchio C, Angeletti S, Ciccozzi M, Gallo RC, Zella D, Ippodrino R (2020) Emerging SARS-CoV-2 mutation hot spots include a novel RNA-dependent-RNA polymerase variant. J Translational Med 18(1):179. https://doi.org/10.1186/s12967-020-02344-6
de Paiva REF, Marçal Neto A, Santos IA, Jardim ACG, Corbi PP, Bergamini FRG (2020) What is holding back the development of antiviral metallodrugs? A literature overview and implications for SARS-CoV-2 therapeutics and future viral outbreaks. Dalton Trans 49(45):16004–16033. https://doi.org/10.1039/D0DT02478C
Pelosi G, Bisceglie F, Bignami F, Ronzi P, Schiavone P, Re MC, Casoli C, Pilotti E (2010) Antiretroviral activity of thiosemicarbazone metal complexes. J Med Chem 53(24):8765–8769. https://doi.org/10.1021/jm1007616
Perdrau JR, Todd C (1933) The photodynamic action of methylene blue on bacteriophage. Proceedings of the Royal Society of London Series B Containing Papers of a Biological Character 112(777):277–287. https://doi.org/10.1098/rspb.1933.0010
Photodynamic therapy in cancer treatment - an updated review https://jcmtjournal.com/article/view/3026. Accessed 25 July 2021
Platinum and other metal coordination compounds in cancer chemotherapy: proceedings of the fifth international symposium on platinum and other metal coordination compounds in cancer chemotherapy Abano, Padua, Italy — June 29–July 2, 1987, In: M. Nicolini (ed), Developments in Oncology; Springer US, 1988. https://doi.org/10.1007/978-1-4613-1717-3.
Prajapat M, Sarma P, Shekhar N, Avti P, Sinha S, Kaur H, Kumar S, Bhattacharyya A, Kumar H, Bansal S, Medhi B (2020) Drug targets for coronavirus: a systematic review. Indian J Pharmacol 52(1):56–65. https://doi.org/10.4103/ijp.IJP_115_20
Pricker SP (1996) Medical uses of gold compounds: past, present, and future. Gold Bull 29(2):53–60. https://doi.org/10.1007/BF03215464
Pruijssers AJ, George AS, Schäfer A, Leist SR, Gralinksi LE, Dinnon KH, Yount BL, Agostini ML, Stevens LJ, Chappell JD, Lu X, Hughes TM, Gully K, Martinez DR, Brown AJ, Graham RL, Perry JK, Du Pont V, Pitts J, Ma B, Babusis D, Murakami E, Feng JY, Bilello JP, Porter DP, Cihlar T, Baric RS, Denison MR, Sheahan TP (2020) Remdesivir inhibits SARS-CoV-2 in human lung cells and chimeric SARS-CoV expressing the SARS-CoV-2 RNA polymerase in mice. Cell Rep 32(3):107940. https://doi.org/10.1016/j.celrep.2020.107940
Riccardi L, Genna V, De Vivo M (2018) Metal–ligand interactions in drug design. Nat Rev Chem 2(7):100–112. https://doi.org/10.1038/s41570-018-0018-6
Roder C, Thomson MJ (2015) Auranofin: repurposing an old drug for a golden new age. Drugs R D 15(1):13–20. https://doi.org/10.1007/s40268-015-0083-y
Rothan HA, Kumar M (2019) Role of endoplasmic reticulum-associated proteins in flavivirus replication and assembly complexes. Pathogens 8(3):148. https://doi.org/10.3390/pathogens8030148
Rothan HA, Stone S, Natekar J, Kumari P, Arora K, Kumar M (2020) The FDA-approved gold drug auranofin inhibits novel coronavirus (SARS-COV-2) replication and attenuates inflammation in human cells. Virology 547:7–11. https://doi.org/10.1016/j.virol.2020.05.002
Ruane PH, Edrich R, Gampp D, Keil SD, Leonard RL, Goodrich RP (2004) Photochemical inactivation of selected viruses and bacteria in platelet concentrates using riboflavin and light. Transfusion 44(6):877–885. https://doi.org/10.1111/j.1537-2995.2004.03355.x
SARS-coronavirus replication is supported by a reticulovesicular network of modified endoplasmic reticulum. https://journals.plos.org/plosbiology/article?id=https://doi.org/10.1371/journal.pbio.0060226. Accessed 26 June 2021
Savarino A, Shytaj IL (2015) Chloroquine and beyond: exploring antirheumatic drugs to reduce immune hyperactivation in HIV/AIDS. Retrovirology 12(1):51. https://doi.org/10.1186/s12977-015-0178-0
Schwartz JA, Lium EK, Silverstein SJ (2001) Herpes simplex virus type 1 entry is inhibited by the cobalt chelate complex CTC-96. J Virol 75(9):4117–4128. https://doi.org/10.1128/JVI.75.9.4117-4128.2001
Singh A, Singh A, Singh R, Misra A (2021) Molnupiravir in COVID-19: a systematic literature review. Diabetes Metab Syndr 15(6):102329
Singh R, Sharma B (2018) Metal-based therapy in traditional and modern medicine systems. In: Rai M, Ingle AP, Medici S (eds), Biomedical applications of metals. Springer International Publishing: Cham, pp 195–211. https://doi.org/10.1007/978-3-319-74814-6_9.
Siu K-L, Chan C-P, Kok K-H, Woo PC-Y, Jin D-Y (2014) Comparative analysis of the activation of unfolded protein response by spike proteins of severe acute respiratory syndrome coronavirus and human coronavirus HKU1. Cell Biosci 4:3. https://doi.org/10.1186/2045-3701-4-3
Sodhi RK, Paul S (2019) Metal complexes in medicine: an overview and update from drug design perspective. CTOIJ 14(1):1–8
Svyatchenko VA, Nikonov SD, Mayorov AP, Gelfond ML, Loktev VB (2021) Antiviral photodynamic therapy: inactivation and inhibition of SARS-CoV-2 in vitro using methylene blue and radachlorin. Photodiagnosis Photodyn Ther 33:102112. https://doi.org/10.1016/j.pdpdt.2020.102112
Tardivo JP, Giglio AD, Paschoal LH, Baptista MS (2006) New Photodynamic therapy protocol to treat AIDS-related kaposi’s sarcoma. Photomed Laser Surg 24(4):528–531. https://doi.org/10.1089/pho.2006.24.528
Tariq R, Khalid UA, Kanwal S, Adnan F, Qasim M (2021) Photodynamic therapy: a rational approach toward COVID-19 management. J Expl Res Pharmacol 6(2):44–52
Taylor MW (2014) Vaccines against viral infections. Viruses and Man. https://doi.org/10.1007/978-3-319-07758-1_19
Vlahos R, Sambas J, Bozinovski S, Broughton BRS, Drummond GR, Selemidis S (2011) Inhibition of NOX2 oxidase activity ameliorates influenza A virus-induced lung inflammation. PLoS Pathog 7(2):e1001271. https://doi.org/10.1371/journal.ppat.1001271
Walz DT, DiMartino MJ, Griswold DE, Intoccia AP, Flanagan TL (1983) Biologic actions and pharmacokinetic studies of auranofin. Am J Med 75(6A):90–108. https://doi.org/10.1016/0002-9343(83)90481-3
Weisblum Y, Schmidt F, Zhang F, DaSilva J, Poston D, Lorenzi JC, Muecksch F, Rutkowska M, Hoffmann H-H, Michailidis E, Gaebler C, Agudelo M, Cho A, Wang Z, Gazumyan A, Cipolla M, Luchsinger L, Hillyer CD, Caskey M, Robbiani DF, Rice CM, Nussenzweig MC, Hatziioannou T, Bieniasz PD (2020) Escape from neutralizing antibodies by SARS-CoV-2 spike protein variants. Elife 9:e61312. https://doi.org/10.7554/eLife.61312
Wiehe A, O’Brien JM, Senge MO (2019) Trends and targets in antiviral phototherapy. Photochem Photobiol Sci 18(11):2565–2612. https://doi.org/10.1039/C9PP00211A
Wolf DC, Wolf CH, Rubin DT (2020) Temporal improvement of a COVID-19-Positive Crohn's disease patient treated with bismuth subsalicylate. Am J Gastroenterol https://doi.org/10.14309/ajg.0000000000000725
Wrapp D, Wang N, Corbett KS, Goldsmith JA, Hsieh C-L, Abiona O, Graham BS, McLellan JS (2020) Cryo-EM structure of the 2019-NCoV spike in the prefusion conformation. Science 367(6483):1260–1263. https://doi.org/10.1126/science.abb2507
Wu M-Y, Gu M, Leung J-K, Li X, Yuan Y, Shen C, Wang L, Zhao E, Chen S. A membrane-targeting photosensitizer with aggregation-induced emission characteristics for highly efficient photodynamic combat of human coronaviruses. Small https://doi.org/10.1002/smll.202101770.
Yang N, Tanner JA, Zheng B-J, Watt RM, He M-L, Lu L-Y, Jiang J-Q, Shum K-T, Lin Y-P, Wong K-L, Lin MCM, Kung H-F, Sun H, Huang J-D (2007) Bismuth complexes inhibit the SARS coronavirus. Angew Chem Int Ed 46(34):6464–6468. https://doi.org/10.1002/anie.200701021
Yang H, Yang M, Ding Y, Liu Y, Lou Z, Zhou Z, Sun L, Mo L, Ye S, Pang H, Gao GF, Anand K, Bartlam M, Hilgenfeld R, Rao Z (2003) The crystal structures of severe acute respiratory syndrome virus main protease and its complex with an inhibitor. Proc Natl Acad Sci USA 100(23):13190–13195. https://doi.org/10.1073/pnas.1835675100
Yuan S, Wang R, Chan JF-W, Zhang AJ, Cheng T, Chik KK-H, Ye Z-W, Wang S, Lee AC-Y, Jin L, Li H, Jin D-Y, Yuen K-Y, Sun H (2020) Metallodrug ranitidine bismuth citrate suppresses SARS-CoV-2 replication and relieves virus-associated pneumonia in Syrian hamsters. Nat Microbiol 5(11):1439–1448. https://doi.org/10.1038/s41564-020-00802-x
Acknowledgements
None.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no known competing financial interests or personal relationships that could have influenced the work reported in this paper.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ioannou, K., Vlasiou, M.C. Metal-based complexes against SARS-CoV-2. Biometals 35, 639–652 (2022). https://doi.org/10.1007/s10534-022-00386-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10534-022-00386-5