Abstract
Background
The aim of the present study was to perform a systematic review and meta-analysis of cancer-specific outcomes after curative rectal cancer surgery comparing anastomotic leak (AL) with no leak.
Methods
PubMed, Medline and Embase databases were searched to identify studies comparing cancer-specific outcomes after rectal cancer surgery in patients with AL and without. A meta-analysis with a random-effects model was used to calculate pooled odds ratios (OR) and confidence intervals (CI) for each outcome measure.
Results
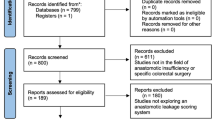
A total of 18 studies were included for meta-analysis, comprising a total of 18,039 patients after curative rectal resection (1764 AL, 16,275 without AL). The overall rate of AL was 9.8%. After AL and excluding 30-day mortality there was an increased risk of local recurrence (OR 1.50; CI 1.23, 1.82), worse overall survival (OR 0.69; CI 0.60–0.81), decreased disease free survival (OR 0.51; CI 0.36–0.73) and cancer specific survival (OR 0.71; CI 0.54–0.94). Distant recurrence (OR 1.10; CI 0.89–1.37) and overall recurrence (OR 1.33; CI 0.64–2.76) were not significantly different between the two groups.
Conclusions
AL may negatively impact cancer-specific outcomes after curative rectal cancer surgery and could be considered an independent negative prognostic factor.











Similar content being viewed by others
References
Rutter CM, Johnson EA, Feuer EJ et al (2013) Secular trends in colon and rectal cancer relative survival. J Natl Cancer Inst 105(23):1806–1813
Janjua Z, Moran B (2014) Rectal cancer-specialist practice, p(69) (ISBN: 978–0–7020–4965)
Folkesson J, Birgisson H, Pahlman L et al (2005) Swedish Rectal Cancer Trial: long lasting benefits from radiotherapy on survival and local recurrence rate. J Clin Oncol 23:5644–5650
Sauer R, Liersch T, Merkel S et al (2012) Preoperative versus postoperative chemoradiotherapy for locally advanced rectal cancer: results of the German CAO/ARO/AIO-94 randomized phase III trial after a median follow-up of 11 years. J Clin Oncol 30:1926–1933
van Gijn W, Marijnen CA, Nagtegaal ID et al (2011) Preoperative radiotherapy combined with total mesorectal excision for resectable rectal cancer: 12-year follow-up of the multicentre, randomised controlled TME trial. Lancet Oncol 12:575–582
Fisher B, Wolmark N, Rockette H et al (1988) Postoperative adjuvant chemotherapy or radiation therapy for rectal cancer: results from NSABP protocol R-01. J Natl Cancer Inst 80:21–29
Krook JE, Moertel CG, Gunderson LL et al (1991) Effective surgical adjuvant therapy for high-risk rectal carcinoma. N Engl J Med 324:709–715
Wolmark N, Rockette H, Fisher B et al (1993) The benefit of leucovorin-modulated fluorouracil as postoperative adjuvant therapy for primary colon cancer: results from National Surgical Adjuvant Breast and Bowel Project protocol C-03. J Clin Oncol 11:1879–1887
O’Connell MJ, Martenson JA, Wieand HS et al (1994) Improving adjuvant therapy for rectal cancer by combining protracted-infusion fluorouracil with radiation therapy after curative surgery. N Engl J Med 331:502–507
Hofheinz RD, Wenz F, Post S et al (2012) Chemoradiotherapy with capecitabine versus fluorouracil for locally advanced rectal cancer: a randomised, multicentre, non-inferiority, phase 3 trial. Lancet Oncol 13:579–588
Yothers G, O’Connell MJ, Allegra CJ et al (2011) Oxaliplatin as adjuvant therapy for colon cancer: updated results of NSABP C-07 trial, including survival and subset analyses. J Clin Oncol 29:3768–3774
André T, Boni C, Navarro M et al (2009) Improved overall survival with oxaliplatin, fluorouracil, and leucovorin as adjuvant treatment in stage II or III colon cancer in the MOSAIC trial. J Clin Oncol 27:3109–3116
Petersen SH, Harling H, Kirkeby LT et al (2012) Postoperative adjuvant chemotherapy in rectal cancer operated for cure. Cochrane Database Syst Rev 3:CD004078
Heald RJ, Husband EM, Ryall RD (1982) The mesorectum in rectal cancer surgery–the clue to pelvic recurrence? Br J Surg 69(10):613–616
Havenga K, Enker WE, Norstein J et al (1999) Improved survival and local control after total mesorectal excision or D3 lymphadenectomy in the treatment of primary rectal cancer: an international analysis of 1411 patients. Eur J Surg Oncol 25:368–374
McDermott FD, Heeney A, Kelly ME, Steele RJ, Carlson GL, Winter DC (2015) Systematic review of preoperative, intraoperative and postoperative risk factors for colorectal anastomotic leaks. Br J Surg 102(5):462–479
Arezzo A, Migliore M, Chiaro P, REAL Score Collaborators et al (2019) The REAL (REctal Anastomotic Leak) score for prediction of anastomotic leak after rectal cancer surgery. Tech Coloproctol 23:649–663. https://doi.org/10.1007/s10151-019-02028-4
Rausa E1, Zappa MA2, Kelly ME et al (2019) A standardized use of intraoperative anastomotic testing in colorectal surgery in the new millennium: Is technology taking over? A systematic review and network meta-analysis. Tech Coloproctol 23(7):625–631. https://doi.org/10.1007/s10151-019-02034-6(epub 2019 Jul 13)
Bakker S, Grossmann I, Henneman D et al (2014) Risk factors for anastomotic leakage and leak-related mortality after colonic cancer surgery in a nationwide audit. Br J Surg 101(4):424–432
Mirnezami A, Mirnezami R, Chandrakumaran K et al (2011) Increased local recurrence and reduced survival from colorectal cancer following anastomotic leak: systematic review and meta-analysis. Ann Surg 253(5):890–899 (review)
Espín E, Ciga MA, Pera M et al (2015) Oncological outcome following anastomotic leak in rectal surgery. Br J Surg 102(4):416–422
Adelsdorfer C, Delgado S, Adelsdorfer W et al (2012) Influence of anastomotic leakage in the long term results of laparoscopic treatment of curative rectal cancer. Surg Endosc Other Interv Tech 26:S276
Bertelsen CA, Andreasen AH, Jorgensen T et al (2010) Anastomotic leakage after curative anterior resection for rectal cancer: short and long-term outcome. Colorectal Dis 12:e76–81
Branagan G, Finnis D (2005) Prognosis after anastomotic leakage in colorectal surgery. Dis Colon Rectum 48(5):1021–1026
Chang SC, Lin JK, Yang SH et al (2003) Long-term outcome of anastomosis leakage after curative resection for mid and low rectal cancer. Hepatogastroenterology 50(54):1898–1902
den Dulk M, Marijnen CA, Collette L et al (2009) Multicentre analysis of oncological and survival outcomes following anastomotic leakage after rectal cancer surgery. Br J Surg 96(9):1066–1075
Eberhardt JM, Kiran RP, Lavery IC (2009) The impact of leak and intra-abdominal abscess on cancer related outcomes after resection for colorectal cancer: a case control study. Dis Colon Rectum 52(3):380–386
Eriksen MT, Wibe A, Norstein J et al (2005) Anastomotic leakage following routine mesorectal excision for rectal cancer in a national cohort of patients. Colorectal Dis 7(1):51–57
Hai-Lin K, Pan C, Hui-Ming L et al (2015) The influence of anastomotic leakage of longterm survival after resection for cancer. Eur Surg Acta Chirugica Austriaca 47(S61):1682–8631
Jorgren F, Johansson R, Damber L (2011) Anastomotic leakage after surgery for rectal cancer: a risk factor for local recurrence, distant metastasis and reduced cancer-specific survival? Colorectal Dis 13(3):272–283 (1462–8910; 1463–1318)
Jung SH, Yu CS, Choi PW et al (2008) Risk factors and oncologic impact of anastomotic leakage after rectal cancer surgery. Dis Colon Rectum 51(6):902–908
Katoh H, Yamashita K, Wang G et al (2011) Anastomotic leakage contributes to the risk for systemic recurrence in stage II colorectal cancer. J Gastrointest Surg 15(1):120–129
Kulu Y, Tarantio I, Warschkow R et al (2015) Anastomotic leakage is associated with impaired overall and disease-free survival after curative rectal cancer resection: a propensity score analysis. Ann Surg Oncol 22(6):2059–2067
Lee WS, Yun SH, Roh YN et al (2008) Risk factors and clinical outcome for anastomotic leakage after total mesorectal excision for rectal cancer. World J Surg 32(6):1124–1129
Merkel S, Wang WY, Schmidt O et al (2001) Locoregional recurrence in patients with anastomotic leakage after anterior resection for rectal carcinoma. Colorectal Dis 3(3):154–160
Ptok H, Marusch F, Meyer F et al (2007) Impact of anastomotic leakage on oncological outcome after rectal cancer resection. Br J Surg 94(12):1548–1554
Smith JD, Paty PB, Weiser MR et al (2013) Anastomotic leak following low anterior resection in stage IV rectal cancer is associated with poor survival. Ann Surg Oncol 20(8):2641–2646
Steele R, Quirke P, Grieve R et al (2012) Long term outcome after anastomotic leak and the impact of short course pre-operative radiotherapy-date from the MRC CR07 trial. Colorectal Dis 14(25):1462–8910
Wang S, Liu J, Wang S, Zhao H, Ge S, Wang W (2017) Adverse effects of anastomotic leakage on local recurrence and survival after curative anterior resection for rectal cancer: a systematic review and meta-analysis. World J Surg 41(1):277–284
Umpleby HC, Fermor B, Symes MO, Williamson RC (1984) Viability of exfoliated colorectal carcinoma cells. Br J Surg 71:659–663
Slanetz CA Jr (1984) The effect of inadvertent intraoperative perforation on survival and recurrence in colorectal cancer. Dis Colon Rectum 27:792–797
Alonso S, Pascual M, Salvans S, Mayol X, Mojal S, Gil MJ, Grande L, Pera M (2015) Postoperative intra-abdominal infection and colorectal cancer recurrence: a prospective matched cohort study of inflammatory and angiogenic responses as mechanisms involved in this association. Eur J Surg Oncol 41(2):208–214
Salvans S, Mayol X, Alonso S, Messeguer R, Pascual M, Mojal S, Grande L, Pera M (2014) Postoperative peritoneal infection enhances migration and invasion capacities of tumor cells in vitro: an insight into the association between anastomotic leak and recurrence after surgery for colorectal cancer. Ann Surg 260(5):939–943
Des Guetz G, Nicolas P, Perret GY, Morere JF, Uzzan B (2010) Does delaying adjuvant chemotherapy after curative surgery for colorectal cancer impair survival? A meta-analysis. Eur J Cancer 46(6):1049–1055
Amato A, Pescatori M, Butti A (1991) Local recurrence following abdominoperineal excision and anterior resection for rectal carcinoma. Dis Colon Rectum 34:317–332
Fujita S, Teramoto T, Watanabe M et al (1993) Anastomotic leakage after colorectal surgery: a risk factor for recurrence and poor prognosis. Jpn J Clin Oncol 23:299–302
Pakkastie TE, Luukonen PE, Jarvinen HJ (1995) Anterior resection controls cancer of the rectum as well as abdominoperineal excision. Eur J Surg 161:833–839
Bell SW, Walker KG, Rickard MJFX et al (2003) Anastomotic leakage after curative anterior resection results in a higher prevalence of local recurrence. Br J Surg 90:1261–1266
Law WL, Choi HK, Lee YM et al (2007) Anastomotic leakage is associated with poor long term outcome in patients after curative colorectal resection for malignancy. J Gastrointest Surg 11:8–15
Ha W et al (2017) Oncologic impact of anastomotic leakage following colorectal cancer surgery: a systematic review and meta-analysis. Ann Surg Oncol 24(11):3289–3299
Funding
No source of funding for declaration.
Author information
Authors and Affiliations
Contributions
AK and PWW conception and design of study, acquisition of data, analysis and interpretation of data, drafting article, final approval. VC, SZ and SK drafting article, final approval. HPP acquisition of data, analysis and interpretation of data, drafting article, final approval.
Corresponding author
Ethics declarations
Conflict of interest
The authors deny any conflict of interest.
Ethical approval
The study does not contain any human participants and does not require ethical approval.
Informed consent
For this type of study formal consent is not required.
Data sharing statement
No additional data are available.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Karim, A., Cubas, V., Zaman, S. et al. Anastomotic leak and cancer-specific outcomes after curative rectal cancer surgery: a systematic review and meta-analysis. Tech Coloproctol 24, 513–525 (2020). https://doi.org/10.1007/s10151-020-02153-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10151-020-02153-5