Abstract
Purpose
To determine whether an additional arterial phase (AP) leads to a change in the grade of splenic injury according to the 2018 revision of the AAST Organ Injury Scale, which has incorporated vascular injuries into the grading system and also to study its impact on management.
Methods
In this retrospective study, 527 patients who sustained blunt abdominal trauma and had underwent dual-phase CT (AP and portal venous phase (PVP)) from December 2014 to October 2016 (23 months) were included. Two experienced radiologists independently graded the splenic injury according to the revised system in 2 blinded ways (AP + PVP and PVP alone). Receiver operator characteristic (ROC) curves were generated for grade of injury on both the phases for all splenic interventions.
Results
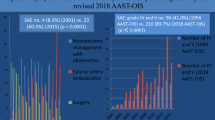
Splenic injuries were detected in 154 patients, and splenic vascular injuries were detected in 52 of them. Of these, 22 vascular injuries were detected only on the AP, leading to a change in the grade of injury according to the new system in 18 patients. The AUC for ROC curves was generated for the grade of injury on AP + PVP vs. PVP alone for angioembolization (0.80 vs. 0.71, p value 0.002), and all splenic interventions (0.89 vs. 0.83, p value 0.003) showed higher AUC for AP + PVP.
Conclusion
Addition of AP leads to a significant change in the grading of splenic injuries according to the revised grading system due to increased detection of vascular injuries. Accurate classification of splenic injuries using additional AP would lead to better triage of patients for splenic interventions or conservative management.


Similar content being viewed by others
Abbreviations
- AAST:
-
American Association for the Surgery of Trauma
- AE:
-
Active extravasation of contrast
- AP:
-
Arterial phase
- AUC:
-
Area under the curve
- CVI:
-
Contained vascular injury
- DSA:
-
Digital subtraction angiography
- OIS:
-
Organ Injury Scale
- PVP:
-
Portal venous phase
- ROC:
-
Receiver operator characteristic
References
Zarzaur BL, Kozar R, Myers JG, Claridge JA, Scalea TM, Neideen TA, Maung AA, Alarcon L, Corcos A, Kerwin A, Coimbra R (2015) The splenic injury outcomes trial: an American Association for the Surgery of Trauma multi-institutional study. J Trauma Acute Care Surg 79(3):335–342. https://doi.org/10.1097/TA.0000000000000782
D’Huyvetter C (2000) The trauma disease. J Trauma Nurs 7(1):5–12
Gad MA, Saber A, Farrag S, Shams ME, Ellabban GM (2012) Incidence, patterns, and factors predicting mortality of abdominal injuries in trauma patients. N Am J Med Sci 4(3):129–134. https://doi.org/10.4103/1947-2714.93889
Brillantino A, Iacobellis F, Robustelli U, Villamaina E, Maglione F, Colletti O, de Palma M, Paladino F, Noschese G (2015) Non operative management of blunt splenic trauma: a prospective evaluation of a standardized treatment protocol. Eur J Trauma Emerg Surg Published online September 28:593–598. https://doi.org/10.1007/s00068-015-0575-z
Chastang L, Bège T, Prudhomme M, Simonnet AC, Herrero A, Guillon F, Bono D, Nini E, Buisson T, Carbonnel G, Passebois L, Vacher C, le Moine MC (2015) Is non-operative management of severe blunt splenic injury safer than embolization or surgery? Results from a French prospective multicenter study. J Visc Surg 152(2):85–91. https://doi.org/10.1016/j.jviscsurg.2015.01.003
Watson GA, Hoffman MK, Peitzman AB (2015) Nonoperative management of blunt splenic injury: what is new? Eur J Trauma Emerg Surg 41(3):219–228. https://doi.org/10.1007/s00068-015-0520-1
Moore EE, Shackford SR, Pachter HL et al (1989) Organ injury scaling: spleen, liver, and kidney. J Trauma 29(12):1664–1666
Moore EE, Cogbill TH, Jurkovich GJ, Shackford SR, Malangoni MA, Champion HR (1995) Organ injury scaling: spleen and liver (1994 revision). J Trauma 38(3):323–324. https://doi.org/10.1097/00005373-199503000-00001
Kozar RA, Crandall M, Shanmuganathan K, Zarzaur BL, Coburn M, Cribari C, Kaups K, Schuster K, Tominaga GT, AAST Patient Assessment Committee (2018) Organ injury scaling 2018 update: spleen, liver, and kidney. J Trauma Acute Care Surg 85(6):1119–1122. https://doi.org/10.1097/TA.0000000000002058
Hinzpeter R, Boehm T, Boll D, Constantin C, del Grande F, Fretz V, Leschka S, Ohletz T, Brönnimann M, Schmidt S, Treumann T, Poletti PA, Alkadhi H (2016) Imaging algorithms and CT protocols in trauma patients: survey of Swiss emergency centers. Eur Radiol Published online September 5:1922–1928. https://doi.org/10.1007/s00330-016-4574-1
Becker CD, Spring P, Glättli A, Schweizer W (1994) Blunt splenic trauma in adults: can CT findings be used to determine the need for surgery? AJR Am J Roentgenol 162(2):343–347. https://doi.org/10.2214/ajr.162.2.8310923
Uyeda JW, LeBedis CA, Penn DR, Soto JA, Anderson SW (2014) Active hemorrhage and vascular injuries in splenic trauma: utility of the arterial phase in multidetector CT. Radiology. 270(1):99–106. https://doi.org/10.1148/radiol.13121242
Boscak AR, Shanmuganathan K, Mirvis SE, Fleiter TR, Miller LA, Sliker CW, Steenburg SD, Alexander M (2013) Optimizing trauma multidetector CT protocol for blunt splenic injury: need for arterial and portal venous phase scans. Radiology. 268(1):79–88. https://doi.org/10.1148/radiol.13121370
Melikian R, Goldberg S, Strife BJ, Halvorsen RA (2016) Comparison of MDCT protocols in trauma patients with suspected splenic injury: superior results with protocol that includes arterial and portal venous phase imaging. Diagn Interv Radiol 22(5):395–399. https://doi.org/10.5152/dir.2016.15232
Anderson SW, Soto JA, Lucey BC, Burke PA, Hirsch EF, Rhea JT (2008) Blunt trauma: feasibility and clinical utility of pelvic CT angiography performed with 64-detector row CT. Radiology. 246(2):410–419. https://doi.org/10.1148/radiol.2462070082
Kirkpatrick AW, Ball CG, D’Amours SK, Zygun D (2008) Acute resuscitation of the unstable adult trauma patient: bedside diagnosis and therapy. Can J Surg 51(1):57–69 Accessed Sept 16, 2019. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2386316/
Renzulli P, Gross T, Schnüriger B, Schoepfer AM, Inderbitzin D, Exadaktylos AK, Hoppe H, Candinas D (2010) Management of blunt injuries to the spleen. Br J Surg 97(11):1696–1703. https://doi.org/10.1002/bjs.7203
Marmery H, Shanmuganathan K, Mirvis SE, Richard H III, Sliker C, Miller LA, Haan JM, Witlus D, Scalea TM (2008) Correlation of multidetector CT findings with splenic arteriography and surgery: prospective study in 392 patients. J Am Coll Surg 206(4):685–693. https://doi.org/10.1016/j.jamcollsurg.2007.11.024
Hamilton JD, Kumaravel M, Censullo ML, Cohen AM, Kievlan DS, West OC (2008) Multidetector CT evaluation of active extravasation in blunt abdominal and pelvic trauma patients. Radiographics. 28(6):1603–1616. https://doi.org/10.1148/rg.286085522
Anderson SW, Varghese JC, Lucey BC, Burke PA, Hirsch EF, Soto JA (2007) Blunt splenic trauma: delayed-phase CT for differentiation of active hemorrhage from contained vascular injury in patients. Radiology. 243(1):88–95. https://doi.org/10.1148/radiol.2431060376
DeLong ER, DeLong DM, Clarke-Pearson DL (1988) Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics. 44(3):837–845
Atluri S, Richard HM, Shanmuganathan K (2011) Optimizing multidetector CT for visualization of splenic vascular injury. Validation by splenic arteriography in blunt abdominal trauma patients. Emerg Radiol 18(4):307–312. https://doi.org/10.1007/s10140-011-0961-8
Shanmuganathan K, Mirvis SE, Reaney SM (1995) Pictorial review: CT appearances of contrast medium extravasations associated with injury sustained from blunt abdominal trauma. Clin Radiol 50(3):182–187
Bae KT (2010) Intravenous contrast medium administration and scan timing at CT: considerations and approaches. Radiology. 256(1):32–61. https://doi.org/10.1148/radiol.10090908
Soto JA, Anderson SW (2012) Multidetector CT of blunt abdominal trauma. Radiology. 265(3):678–693. https://doi.org/10.1148/radiol.12120354
Rosenkrantz AB (2017) Genitourinary imaging, an issue of radiologic clinics of North America, E-Book. Elsevier Health Sciences
Donnelly LF, Foss JN, Frush DP, Bisset GS (1999) Heterogeneous splenic enhancement patterns on spiral CT images in children: minimizing misinterpretation. Radiology. 210(2):493–497. https://doi.org/10.1148/radiology.210.2.r99fe16493
Acknowledgments
We would like to acknowledge the contribution of Dr. Kathirkamanathan Shanmuganathan (deceased), professor, Diagnostic Radiology, University of Maryland School of Medicine, for his help in conceptualization of the paper and in editing the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This study was approved by the Institutional Review Board (ref no. IESC/T-421), and the requirement for informed consent was waived.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hemachandran, N., Gamanagatti, S., Sharma, R. et al. Revised AAST scale for splenic injury (2018): does addition of arterial phase on CT have an impact on the grade?. Emerg Radiol 28, 47–54 (2021). https://doi.org/10.1007/s10140-020-01823-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10140-020-01823-z