Abstract
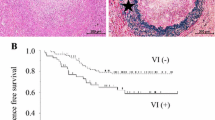
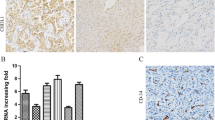
Tumor angiogenesis is important for the progression of cancer and is orchestrated by various factors associated with tumor vessels, tumor cells, and stromal cells. Angiogenic signaling in non-small cell lung cancer (NSCLC) needs to be further clarified, especially regarding existing and upcoming therapeutic approaches. Expression of CD34, CD105, Mel-CAM, VE-cadherin, D2-40, VEGF, VEGFR1, and VEGFR2 was assessed immunohistochemically on a cohort of 371 well documented, surgically resected NSCLC using a standardized tissue microarray platform. Extensive clinical data and a postoperative follow-up period of up to 18 years allowed us to assess clinicopathological correlations in detail. Microvasculature in NSCLC was significantly denser at the tumor periphery as compared to the tumor center. Squamous cell carcinomas (SCC) were associated with a notably lower microvessel density (MVD) than adenocarcinomas (ACA). CD105 was present at significantly higher levels on stromal cells of ACA as compared to SCC. Expression of VE-cadherin by tumor cells (6 % of cases, mainly ACA) as well as decreased MVD in the tumor centers was independently associated with poor prognosis in the entire cohort. Low MVD in SCC might be related to lower efficacy of and fatal bleeding during therapy with bevacizumab. In other NSCLC entities for which treatment with VEGF inhibitors is studied in clinical trials, the predictive value of MVD for therapy response merits to be prospectively examined. Our data suggest that patients with ACA may be candidates for therapies targeting CD105. VE-cadherin is another promising target for therapy, but its expression also provides independent prognostic information.


Similar content being viewed by others
References
Lima AB, Macedo LT, Sasse AD (2011) Addition of bevacizumab to chemotherapy in advanced non-small cell lung cancer: a systematic review and meta-analysis. PLoS One 6:e22681
American Cancer Society. Non-small cell lung cancer survival rates by stage. www.cancer.org/cancer/lungcancer-non-smallcell/detailedguide/non-small-cell-lung-cancer-survival-rates Date last updated: July 12, 2013. Date last accessed: October 2013
Langer CJ, Besse B, Gualberto A et al (2010) The evolving role of histology in the management of advanced non‐small‐cell lung cancer. J Clin Oncol 28:5311–5320
Folkman J (2007) Angiogenesis: an organizing principle for drug discovery? Nat Rev Drug Discov 6:273–286
Jain RK (2001) Normalizing tumor vasculature with anti-angiogenetic therapy. Nat Med 7:987–989
Ferrara N, Kerbel RS (2005) Angiogenesis as a therapeutic target. Nature 438:967–974
De Bock K, Mazzone M, Carmeliet P (2011) Antiangiogenic therapy, hypoxia, and metastasis: risky liaisons, or not? Nat Rev Clin Oncol l8:393–404
Carmeliet P, Jain NK (2000) Angiogenesis in cancer and other diseases. Nature 407:249–257
Carmeliet P (2005) VEGF as a key mediator of angiogenesis in cancer. Oncology 69:4–10
Hicklin DJ, Ellis LM (2005) Role of the vascular endothelial growth factor pathway in tumor growth and angiogenesis. J Clin Oncol 23:1011–1027
Carmeliet P, Jain RK (2011) Molecular mechanisms and clinical applications of angiogenesis. Nature 473:298–307
Wedge SR, Kendrew J, Hennequin LF et al (2005) A highly potent, orally bioavailable, vascular endothelial growth factor receptor-2 tyrosine kinase inhibitor for the treatment of cancer. Cancer Res 65:4389–4400
Wilhelm SM, Carter C, Tang L et al (2004) BAY 43-9006 exhibits broad spectrum oral antitumor activity and targets the RAF/MEK/ERK pathway and receptor tyrosine kinases involved in tumor progression and angiogenesis. Cancer Res 64:7099–7109
Kim KJ, Li B, Winer J et al (1993) Inhibition of vascular endothelial growth factor-induced angiogenesis suppresses tumour growth in vivo. Nature 362:841–844
Risau W (1997) Mechanisms of angiogenesis. Nature 386:671–674
Benouchan M, Colombo BM (2005) Anti-angiogenic strategies for cancer therapy. Int J Oncol 27:563–571
Hurwitz H, Fehrenbacher L, Novotny W et al (2004) Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N Engl J Med 350:2335–2342
Sandler A, Gray R, Perry MC et al (2006) Paclitaxel-carboplatin alone or with bevacizumab for non-small-cell lung cancer. N Engl J Med 355:2542–2550
Miller K, Wang M, Gralow J et al (2007) Paclitaxel plus bevacizumab versus paclitaxel alone for metastatic breast cancer. N Engl J Med 357:2666–2676
Karp JE, Gojo I, Pili R et al (2004) Targeting vascular endothelial growth factor for relapsed and refractory adult acute myelogenousleukemias: therapy with sequential 1-beta-d-arabinofuranosylcytosine, mitoxantrone, and bevacizumab. Clin Cancer Res 10:3577–3585
Escudier B, Eisen T, Stadler WM et al (2007) TARGET Study Group. Sorafenibin in advanced clear-cell renal-cell carcinoma. N Engl J Med 356:125–134
Hutson TEMRJ, Tomczak P et al (2007) Sunitinib versus interferon alfa in metastaticrenal-cell carcinoma. N Engl J Med 356:115–124
Ebos JM, Lee CR, Cruz-Munoz W et al (2009) Accelerated metastasis after short-term treatment with a potent inhibitor of tumor angiogenesis. Cancer Cell 15:232–239
Paez-Ribes M, Allen E, Hudock J et al (2009) Antiangiogenic therapy elicits malignant progression of tumors to increased local invasion and distant metastasis. Cancer Cell 15:220–231
Rugo HS, Herbst RS, Liu G et al (2005) Phase I trial of the oral antiangiogenesis agent AG-013736 in patients with advanced solid tumors: pharmacokinetic and clinical results. J Clin Oncol 23:5474–5483
Jenab-Wolcott J, Giantonio BJ (2009) Bevacizumab current indications and future development for management of solid tumors. Expert Opin Biol Ther 9:507–517
Crinò L, Dansin E, Garrido P et al (2010) Safety and efficacy of first-line bevacizumab-based therapy in advanced non-squamous non-small cell lung cancer (SAiL, MO19390): a phase 4 study. Lancet Oncol 11:733–740
Fishbach NA, Spigel D, Brahmer J et al (2009) Preliminary safety and effectiveness of bevacizumab (Bv)-based treatment in subpopulation of patients (pts) with non-small cell lung cancer (NSCLC) from the ARIES study: a bevacizumab treatment observational cohort study (OCS). J Clin Oncol 27:abstr. 8040
Johnson DH, Fehrenbacher L, Novotny WF et al (2004) Randomized phase II trial comparing bevacizumab plus carboplatin and paclitaxel with carboplatin and paclitaxel alone in previously untreated locally advanced or metastatic non-small cell lung cancer. J Clin Oncol 22:2184–2191
Kumar P, Fishbach NA, Brahmer JR et al (2010) Baseline (BL) radiographic characteristics and severe pulmonary hemorrhage (SPH) in bevacizumab ((BV).treated non-small cell lung cancer (NSCLC) patients (pt): results from ARIES, an observational cohort study (OCS). J Clin Oncol 28:abstr. 7619
LeighlNB ZP, Mezger J et al (2010) Efficacy and safety of bevacizumab-based therapy in elderly patients with advanced or recurrent non-squamous non-small cell lung cancer in the phase III BO17704 study (AVAIL). J Thorac Oncol 5:1970–1976
Reck M, Barlesi F, Crinò L et al (2012) Predicting and managing the risk of pulmonary hemorrhage in patients with NSCLC treated with bevacizumab: A consensus report from a panel of expert. Ann Oncol 23:1111–1120
Tang C, Luo D, Yang H et al (2013) Expression of SHP2 and related markers in non-small cell lung cancer: a tissue microarray study of 80 cases. Appl Immunohistochem Mol Morphol 21:386–394
Bing Z, Jian-Ru Y, Yao-Quan J et al (2014) Evaluation of Angiogenesis in Non-small Cell Lung Carcinoma by CD34 Immunohistochemistry. Cell Biochem Biophys 70:327–331
Bremnes RM, Veve R, Gabrielson E et al (2002) High-throughput tissue microarray analysis used to evaluate biology and prognostic significance of the E-cadherin pathway in non–small-cell lung cancer. J Clin Oncol 10:2417–2428
Su CY, Li YS, Han Y et al (2014) Correlation between expression of cell adhesion molecules CD44 v6 and E-cadherin and lymphatic metastasis in non- small cell lung cancer. Asian Pac J Cancer Prev 15:2221–2224
Sterlacci W, Fiegl M, Hilbe W et al (2009) Clinical relevance of neuroendocrine differentiation in non-small cell lung cancer assessed by immunohistochemistry: a retrospective study on 405 surgically resected cases. Virchows Arch 455:125–132
Travis WD, Brambilla E, Noguchi M et al (2011) International association for the study of lung cancer/American thoracic society/European respiratory society international multidisciplinary classification of lung adenocarcinoma. J Thorac Oncol 6:244–285
Fiegl M, Hilbe W, Auberger J et al (2008) Twelve-year retrospective analysis of lung cancer‐ The TYROL Study: Dailyroutine in 1,424 patients (1995-2006). J Clin Oncol 26 :abstr. 19063
Kocher F, Hilbe W, Seeber A et al (2015) Longitudinal analysis of 2293 NSCLC patients: a comprehensive study of the TYROL registry. Lung Cancer 87:193–200
Tzankov A, Zlobec I, Went P et al (2010) Prognostic immune-phenotypic biomarker studies in diffuse large B cell lymphoma with special emphasis on rational determination of cut-off scores. Leuk Lymphoma 51:199–212
Sterlacci W, Savic S, Fiegl M et al (2014) Putative stem cell markers in non-small-cell lung cancer: a clinico-pathologic characterization. J Thorac Oncol 9:41–49
Sterlacci W, Savic S, Schmid T et al (2012) Tissue-sparing application of the newly proposed IASLC/ATS/ERS classification of adenocarcinoma of the lung shows practical diagnostic and prognostic impact. Am J Clin Pathol 137:946–956
Sterlacci W, Tzankov A, Veits L et al (2011) A comprehensive analysis of p16 expression, gene status, and promoter hypermethylation in surgically resected non-small cell lung carcinomas. J Thorac Oncol 6:1649–1657
Sterlacci W, Wolf D, Savic S et al (2012) High transforming growth factor β expression represents an important prognostic parameter for surgically resected non-small cell lung cancer. Hum Pathol 43:339–349
Sterlacci W, Tzankov A, Veits L et al (2011) The prognostic impact of sex on surgically resected non-small cell lung cancer depends on clinico-pathologic characteristics. Am J Clin Pathol 135:611–618
Sterlacci W, Fiegl M, Hilbe W et al (2010) Deregulation of p27 and cyclin D1/D3 control over mitosis is associated with unfavorable prognosis in non-small cell lung cancer, as determined in 405 operated patients. J Thorac Oncol 5:1325–1336
Nielsen JS, McNagny KM (2008) Novel functions of the CD34 family. J Cell Sci 121:3683–3692, Erratum in: J Cell Sci 2008;121:4145
Nassiri F, Cusimano MD, Scheithauer BW et al (2011) Endoglin (CD105): a review of its role in angiogenesis and tumor diagnosis, progression and therapy. Anticancer Res 31:2283–2290
Flanagan K, Fitzgerald K, Baker J et al (2012) Laminin-411 is a vascular ligand for MCAM and facilitates TH17 cell entry into the CNS. PLoS One 7:e40443
Corada M, Liao F, Lindgren M et al (2001) Monoclonal antibodies directed to different regions of vascular endothelial cadherin extracellular domain affect adhesion and clustering of the protein and modulate endothelial permeability. Blood 97:1679–1684
Kalof AN, Cooper K (2009) D2–40 immunohistochemistry–so far! Adv Anat Pathol 16:62–64
Camp RL, Charette LA, Rimm DL (2000) Validation of tissue microarray technology in breast carcinoma. Lab Invest 80:1943–1949
Welter M, Rieger H (2010) Physical determinants of vascular network remodeling during tumor growth. Eur Phys J E Soft Matter 33:149–163
Escorcia FE, Henke E, McDevitt MR et al (2010) Selective killing of tumor neovasculature paradoxically improves chemotherapy delivery to tumors. Cancer Res 70:9277–9286
Tanaka F, Otake Y, Yanagihara K et al (2001) Evaluation of angiogenesis in non-small cell lung cancer: comparison between anti-CD34 antibody and anti-CD105 antibody. Clin Cancer Res 7:3410–3415
Zhang C, Liu Y, Guo S et al (2014) Different biomarkers in non-small cell lung cancer in blood vessel invasion. Cell Biochem Biophys 70:777–784
Rosen LS, Hurwitz HI, Wong MK et al (2012) A phase I first-in-human study of TRC105 (Anti-Endoglin Antibody) in patients with advanced cancer. Clin Cancer Res 18:4820–4829
Rosen LS, Gordon MS, Robert F et al (2014) Endoglin for targeted cancer treatment. Curr Oncol Rep 16:365
Mineo TC, Ambrogi V, Baldi A et al (2004) Prognostic impact of VEGF, CD31, CD34, and CD105 expression and tumour vessel invasion after radical surgery for IB-IIA non-small cell lung cancer. J Clin Pathol 57:591–597
DonnemT A-SS, Al-Shibli K et al (2007) Inverse prognostic impact of angiogenic marker expression in tumor cells versus stromal cells in non-small cell lung cancer. Clin Cancer Res 13:6649–6657
Labelle M, Schnittler HJ, Aust DE et al (2008) Vascular endothelial cadherin promotes breast cancer progression via transforming growth factor beta signaling. Cancer Res 68:1388–1397
Hendrix MJ, Seftor EA, Meltzer PS et al (2001) Expression and functional significance of VE-cadherin in aggressive human melanoma cells: role in vasculogenic mimicry. Proc Natl Acad Sci USA 98:8018–8023
Oka S, Uramoto H, Chikaishi Y et al (2012) The expression of CD146 predicts a poor overall survival in patients with adenocarcinoma of the lung. Anticancer Res 32:861–864
Kadota K, Huang CL, Liu D et al (2010) The clinical significance of the tumor cell D2-40 immunoreactivity in non-small cell lung cancer. Lung Cancer 70:88–93
May C, Doody JF, Abdullah R et al (2005) Identification of a transiently exposed VE-cadherin epitope that allows for specific targeting of an antibody to the tumor neovasculature. Blood 105:4337–4344
Penack O, Henke E, Suh D et al (2010) Inhibition of neovascularization to simultaneously ameliorate graft-vs-host disease and decrease tumor growth. J Natl Cancer Inst 102:894–908
Conflict of interest
The authors declare that they have no conflict of interest.
Sources of funding
The authors declare that they have not received sources of funding.
Author information
Authors and Affiliations
Corresponding author
Additional information
William Sterlacci and AlexandarTzankov shared senior authorship.
Rights and permissions
About this article
Cite this article
Pomme, G., Augustin, F., Fiegl, M. et al. Detailed assessment of microvasculature markers in non-small cell lung cancer reveals potentially clinically relevant characteristics. Virchows Arch 467, 55–66 (2015). https://doi.org/10.1007/s00428-015-1767-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00428-015-1767-y