Abstract
Background
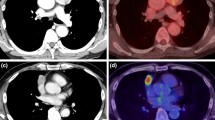
We investigated the role of 18F-fluorodeoxyglucose positron emission tomography-computed tomography (PET-CT) in predicting the effect of induction therapy in patients with thymic epithelial tumors.
Methods
Fourteen patients with thymic epithelial tumors who underwent PET-CT before and after induction therapy were retrospectively analyzed. The relationship between the change in the maximum standardized uptake value (SUVmax) in PET-CT, the response evaluation criteria in solid tumors and the pathologic response (Ef0, no necrosis of tumor cells; Ef1, some necrosis of tumor cells with more than one-third of viable tumor cells; Ef2, less than one-third of tumor cells were viable; and Ef3, no tumor cells were viable) was analyzed.
Results
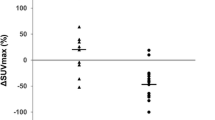
The study cohort consisted of 5 males and 9 females. Nine of the patients had thymoma, and 5 had thymic carcinoma. The induction therapy included chemotherapy in 9 cases, chemoradiation therapy in 4 cases and radiation therapy in 1 case. Among the 8 patients with a pathologic response of Ef0/1, 5 were clinically evaluated as having stable disease (SD), while 3 were found to have had a partial response (PR). The SUVmax was elevated in 2 cases, unchanged in 1 and decreased in 5. On the other hand, 3 of the 6 patients with a pathologic response of Ef2, 3 were classified as having SD, while the other 3 had a PR. The SUVmax decreased in all of the patients.
Conclusions
In comparison with CT, PET-CT seems to be useful for predicting the pathologic response to induction therapy in patients with thymic epithelial tumors.



Similar content being viewed by others
References
Masuda M, Kuwano H, Okumura M et al (2015) Thoracic and cardiovascular surgery in Japan during 2013: annual report by the Japanese Association for Thoracic Surgery. Gen Thorac Cardiovasc Surg 63:670–701
Fischer B, Lassen U, Mortensen J et al (2009) Preoperative staging of lung cancer with combined PET-CT. N Engl J Med 361:32–39
Liu J, Dong M, Sun X et al (2016) Prognostic value of 18F-FDG PET/CT in surgical non-small cell lung cancer: a meta-analysis. PLoS ONE 11:e0146195
Groheux D, Sanna A, Majdoub M et al (2015) Baseline tumor 18F-FDG uptake and modifications after 2 cycles of neoadjuvant chemotherapy are prognostic of outcome in ER +/HER2 − breast cancer. J Nucl Med 56:824–831
Kittaka H, Takahashi H, Ohigashi H et al (2013) Role of (18)F-fluorodeoxyglucose positron emission tomography/computed tomography in predicting the pathologic response to preoperative chemoradiation therapy in patients with resectable T3 pancreatic cancer. World J Surg 37:169–178. doi:10.1007/s00268-012-1775-x
Maffione AM, Marzola MC, Capirci C et al (2015) Value of 18F-FDG PET for predicting response to neoadjuvant therapy in rectal cancer: systematic review and meta-analysis. AJR Am Roentgenol 204:1261–1268
Cerfolio RJ, Bryant AS, Winokur TS et al (2004) Repeat FDG-PET after neoadjuvant therapy is a predictor of pathologic response in patients with non-small cell lung cancer. Ann Thorac Surg 78:1903–1909
Ozeki N, Kawaguchi K, Fukui T et al (2015) Which variables should be considered in patients with stage II and III non-small cell lung cancer after neoadjuvant therapy? Nagoya J Med Sci 77:475–480
Kukar M, Alnaji RM, Jabi F et al (2015) Role of repeat 18F-fluorodeoxyglucose positron emission tomography examination in predicting pathologic response following neoadjuvant chemoradiotherapy for esophageal adenocarcinoma. JAMA Surg 150:555–562
Cheng L, Tunairu N, Collins DJ et al (2015) Response evaluation in mesothelioma: beyond RECIST. Lung Cancer 90:433–441
Kaira K, Murakami H, Miura S et al (2011) 18F-FDG uptake on PET helps predict outcome and response after treatment in unresectable thymic epithelial tumors. Ann Nucl Med 25:247–253
Thomas A, Mena E, Kurdziel K et al (2013) 18F-fluorodeoxyglucose positron emission tomography in the management of patients with thymic epithelial tumors. Clin Cancer Res 19:1487–1493
Eisenhauer EA, Therasse P, Bogaerts J et al (2009) New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer 45:228–247
Masaoka A, Monden Y, Nakahara K et al (1981) Follow-up study of thymomas with special reference to their clinical stages. Cancer 48:2485–2492
Fukumoto K, Taniguchi T, Ishikawa Y et al (2012) The utility of [18F]-fluorodeoxyglucose positron emission tomography-computed tomography in thymic epithelial tumours. Eur J Cardiothorac Surg 42:e152–e156
Japan Lung Cancer Society (2003) General rule for clinical and pathological record of lung cancer, 7th edn. Kanehara, Tokyo, pp 175–177
Yokoi K, Matsuguma H, Nakahara R et al (2007) Multidisciplinary treatment for advanced invasive thymoma with cisplatin, doxorubicin, and methylprednisolone. J Thorac Oncol 2:73–78
Treglia G, Sadeghi R, Giovanella L et al (2014) Is 18F-FDG PET useful in predicting the WHO grade of malignancy in thymic epithelial tumors? A meta-analysis. Lung Cancer 86:5–13
Terzi A, Bertolaccini L, Rizzardi G et al (2011) Usefulness of 18F FDG PET/CT in the pre-treatment evaluation of thymic epithelial neoplasms. Lung Cancer 74:239–243
Shiono S, Abiko M, Okazaki T et al (2011) Positron emission tomography for predicting recurrence in stage I lung adenocarcinoma: standardized uptake value corrected by mean liver standardized uptake value. Eur J Cardiothorac Surg 40:1165–1169
Acknowledgements
We thank Hisashi Tateyama, MD, at the Department of Pathology, Clinical Laboratory, Kasugai Municipal Hospital, Kasugai, Japan, for providing the pathologic data.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest in association with the present study.
Rights and permissions
About this article
Cite this article
Fukumoto, K., Fukui, T., Okasaka, T. et al. The Role of 18F-fluorodeoxyglucose Positron Emission Tomography-Computed Tomography for Predicting Pathologic Response After Induction Therapy for Thymic Epithelial Tumors. World J Surg 41, 1828–1833 (2017). https://doi.org/10.1007/s00268-017-3938-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-017-3938-2