Abstract
Purpose
To evaluate robustness of a radiomics-based support vector machine (SVM) model for detection of visually occult PDA on pre-diagnostic CTs by simulating common variations in image acquisition and radiomics workflow using image perturbation methods.
Methods
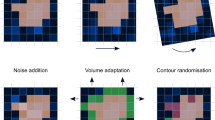
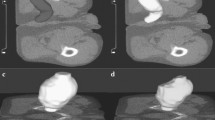
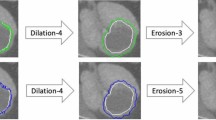
Eighteen algorithmically generated-perturbations, which simulated variations in image noise levels (σ, 2σ, 3σ, 5σ), image rotation [both CT image and the corresponding pancreas segmentation mask by 45° and 90° in axial plane], voxel resampling (isotropic and anisotropic), gray-level discretization [bin width (BW) 32 and 64)], and pancreas segmentation (sequential erosions by 3, 4, 6, and 8 pixels and dilations by 3, 4, and 6 pixels from the boundary), were introduced to the original (unperturbed) test subset (n = 128; 45 pre-diagnostic CTs, 83 control CTs with normal pancreas). Radiomic features were extracted from pancreas masks of these additional test subsets, and the model's performance was compared vis-a-vis the unperturbed test subset.
Results
The model correctly classified 43 out of 45 pre-diagnostic CTs and 75 out of 83 control CTs in the unperturbed test subset, achieving 92.2% accuracy and 0.98 AUC. Model's performance was unaffected by a three-fold increase in noise level except for sensitivity declining to 80% at 3σ (p = 0.02). Performance remained comparable vis-a-vis the unperturbed test subset despite variations in image rotation (p = 0.99), voxel resampling (p = 0.25–0.31), change in gray-level BW to 32 (p = 0.31–0.99), and erosions/dilations up to 4 pixels from the pancreas boundary (p = 0.12–0.34).
Conclusion
The model’s high performance for detection of visually occult PDA was robust within a broad range of clinically relevant variations in image acquisition and radiomics workflow.







Similar content being viewed by others
References
Singh DP, Sheedy S, Goenka AH, Wells M, Lee NJ, Barlow J, et al. (2020) Computerized tomography scan in pre-diagnostic pancreatic ductal adenocarcinoma: Stages of progression and potential benefits of early intervention: A retrospective study. Pancreatology 20(7):1495-501 https://doi.org/10.1016/j.pan.2020.07.410.
Chari ST, Kelly K, Hollingsworth MA, Thayer SP, Ahlquist DA, Andersen DK, et al. (2015) Early detection of sporadic pancreatic cancer: summative review. Pancreas 44(5):693-712 https://doi.org/10.1097/MPA.0000000000000368.
Chhoda A, Vodusek Z, Wattamwar K, Mukherjee E, Gunderson C, Grimshaw A, et al. (2022) Late-Stage Pancreatic Cancer Detected During High-Risk Individual Surveillance: A Systematic Review and Meta-Analysis. Gastroenterology 162(3):786-98 https://doi.org/10.1053/j.gastro.2021.11.021.
Klatte DCF, Boekestijn B, Onnekink AM, Dekker FW, van der Geest LG, Wasser M, et al. (2023) Surveillance for Pancreatic Cancer in High-Risk Individuals Leads to Improved Outcomes: A Propensity Score-Matched Analysis. Gastroenterology 164(7):1223-31 e4 https://doi.org/10.1053/j.gastro.2023.02.032.
Overbeek KA, Goggins MG, Dbouk M, Levink IJM, Koopmann BDM, Chuidian M, et al. (2022) Timeline of Development of Pancreatic Cancer and Implications for Successful Early Detection in High-Risk Individuals. Gastroenterology 162(3):772-85 e4 https://doi.org/10.1053/j.gastro.2021.10.014.
Kurita Y, Kuwahara T, Hara K, Mizuno N, Okuno N, Matsumoto S, et al. (2019) Diagnostic ability of artificial intelligence using deep learning analysis of cyst fluid in differentiating malignant from benign pancreatic cystic lesions. Sci Rep 9(1):6893 https://doi.org/10.1038/s41598-019-43314-3.
Kang J, Clarke SE, Abdolell M, Ramjeesingh R, Payne J, Costa AF (2021) The implications of missed or misinterpreted cases of pancreatic ductal adenocarcinoma on imaging: a multi-centered population-based study. Eur Radiol 31(1):212-21 https://doi.org/10.1007/s00330-020-07120-0.
Kang JD, Clarke SE, Costa AF (2021) Factors associated with missed and misinterpreted cases of pancreatic ductal adenocarcinoma. Eur Radiol 31(4):2422-32 https://doi.org/10.1007/s00330-020-07307-5.
Dewitt J, Devereaux BM, Lehman GA, Sherman S, Imperiale TF (2006) Comparison of endoscopic ultrasound and computed tomography for the preoperative evaluation of pancreatic cancer: a systematic review. Clin Gastroenterol Hepatol 4(6):717-25; quiz 664 https://doi.org/10.1016/j.cgh.2006.02.020.
Toshima F, Watanabe R, Inoue D, Yoneda N, Yamamoto T, Sasahira N, et al. (2021) CT Abnormalities of the Pancreas Associated With the Subsequent Diagnosis of Clinical Stage I Pancreatic Ductal Adenocarcinoma More Than 1 Year Later: A Case-Control Study. AJR Am J Roentgenol:1-12 https://doi.org/10.2214/AJR.21.26014.
Mukherjee S, Patra A, Khasawneh H, Korfiatis P, Rajamohan N, Suman G, et al. (2022) Radiomics-based Machine-learning models can detect pancreatic cancer on prediagnostic computed tomography scans at a substantial lead time before clinical diagnosis. Gastroenterology 163(5):1435-46 e3 https://doi.org/10.1053/j.gastro.2022.06.066.
Zwanenburg A, Leger S, Agolli L, Pilz K, Troost EGC, Richter C, et al. (2019) Assessing robustness of radiomic features by image perturbation. Sci Rep 9(1):614 https://doi.org/10.1038/s41598-018-36938-4.
Zhao B (2021) Understanding Sources of Variation to Improve the Reproducibility of Radiomics. Front Oncol 11:633176 https://doi.org/10.3389/fonc.2021.633176.
Mackin D, Fave X, Zhang L, Fried D, Yang J, Taylor B, et al. (2015) Measuring Computed Tomography Scanner Variability of Radiomics Features. Invest Radiol 50(11):757-65 https://doi.org/10.1097/RLI.0000000000000180.
Yip SS, Aerts HJ (2016) Applications and limitations of radiomics. Phys Med Biol 61(13):R150-66 https://doi.org/10.1088/0031-9155/61/13/R150.
Tixier F, Hatt M, Le Rest CC, Le Pogam A, Corcos L, Visvikis D (2012) Reproducibility of tumor uptake heterogeneity characterization through textural feature analysis in 18F-FDG PET. J Nucl Med 53(5):693-700 https://doi.org/10.2967/jnumed.111.099127.
Leijenaar RT, Carvalho S, Velazquez ER, van Elmpt WJ, Parmar C, Hoekstra OS, et al. (2013) Stability of FDG-PET Radiomics features: an integrated analysis of test-retest and inter- observer variability. Acta Oncol 52(7):1391-7 https://doi.org/10.3109/0284186X.2013.812798.
Teng X, Zhang J, Zwanenburg A, Sun J, Huang Y, Lam S, et al. (2022) Building reliable radiomic models using image perturbation. Sci Rep 12(1):10035 https://doi.org/10.1038/s41598-022-14178-x.
van Griethuysen JJM, Fedorov A, Parmar C, Hosny A, Aucoin N, Narayan V, et al. (2017) Computational Radiomics System to Decode the Radiographic Phenotype. Cancer Res 77(21):e104-e7 https://doi.org/10.1158/0008-5472.CAN-17-0339.
Tibshirani R (1997) The lasso method for variable selection in the Cox model. Stat Med 16(4):385-95 https://doi.org/10.1002/(sici)1097-0258(19970228)16:4<385::aid-sim380>3.0.co;2-3.
DeLong ER, DeLong DM, Clarke-Pearson DL (1988) Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics 44(3):837-45
Qureshi TA, Gaddam S, Wachsman AM, Wang L, Azab L, Asadpour V, et al. (2022) Predicting pancreatic ductal adenocarcinoma using artificial intelligence analysis of pre- diagnostic computed tomography images. Cancer Biomark 33(2):211-7 https://doi.org/10.3233/CBM-210273.
Oliver JA, Budzevich M, Hunt D, Moros EG, Latifi K, Dilling TJ, et al. (2017) Sensitivity of Image Features to Noise in Conventional and Respiratory-Gated PET/CT Images of Lung Cancer: Uncorrelated Noise Effects. Technol Cancer Res Treat 16(5):595-608 https://doi.org/10.1177/1533034616661852.
Suman G, Patra A, Mukherjee S, Korffiatis P, Goenka AH (2022) Radiomics for Detection of Pancreas Adenocarcinoma on CT Scans: Impact of Biliary Stents. Radiol Imaging Cancer 4(1):e210081 https://doi.org/10.1148/rycan.210081.
Huang K, Rhee DJ, Ger R, Layman R, Yang J, Cardenas CE, et al. (2021) Impact of slice thickness, pixel size, and CT dose on the performance of automatic contouring algorithms. J Appl Clin Med Phys 22(5):168-74 https://doi.org/10.1002/acm2.13207.
van Timmeren JE, Cester D, Tanadini-Lang S, Alkadhi H, Baessler B (2020) Radiomics in medical imaging-"how-to" guide and critical reflection. Insights Imaging 11(1):91 https://doi.org/10.1186/s13244-020-00887-2.
Haarburger C, Muller-Franzes G, Weninger L, Kuhl C, Truhn D, Merhof D (2020) Radiomics feature reproducibility under inter-rater variability in segmentations of CT images. Sci Rep 10(1):12688 https://doi.org/10.1038/s41598-020-69534-6.
Wright DE, Mukherjee S, Patra A, Khasawneh H, Korfiatis P, Suman G, et al. (2022) Radiomics-based machine learning (ML) classifier for detection of type 2 diabetes on standard- of-care abdomen CTs: a proof-of-concept study. Abdom Radiol (NY) 47(11):3806-16 https://doi.org/10.1007/s00261-022-03668-1.
Panda A, Korfiatis P, Suman G, Garg SK, Polley EC, Singh DP, et al. (2021) Two-stage deep learning model for fully automated pancreas segmentation on computed tomography: Comparison with intra-reader and inter-reader reliability at full and reduced radiation dose on an external dataset. Med Phys 48(5):2468-81 https://doi.org/10.1002/mp.14782.
Khasawneh H, Patra A, Rajamohan N, Suman G, Klug J, Majumder S, et al. (2022) Volumetric Pancreas Segmentation on Computed Tomography: Accuracy and Efficiency of a Convolutional Neural Network Versus Manual Segmentation in 3D Slicer in the Context of Interreader Variability of Expert Radiologists. J Comput Assist Tomogr 46(6):841-7 https://doi.org/10.1097/RCT.0000000000001374.
Korfiatis P, Suman G, Patnam NG, Trivedi KH, Karbhari A, Mukherjee S, et al. (2023) Automated Artificial Intelligence Model Trained on a Large Data Set Can Detect Pancreas Cancer on Diagnostic Computed Tomography Scans As Well As Visually Occult Preinvasive Cancer on Prediagnostic Computed Tomography Scans. Gastroenterology https://doi.org/10.1053/j.gastro.2023.08.034.
Teng X, Zhang J, Ma Z, Zhang Y, Lam S, Li W, et al. (2022) Improving radiomic model reliability using robust features from perturbations for head-and-neck carcinoma. Front Oncol 12:974467 https://doi.org/10.3389/fonc.2022.974467.
Chari ST, Maitra A, Matrisian LM, Shrader EE, Wu BU, Kambadakone A, et al. (2022) Early Detection Initiative: A randomized controlled trial of algorithm-based screening in patients with new onset hyperglycemia and diabetes for early detection of pancreatic ductal adenocarcinoma. Contemp Clin Trials 113:106659 https://doi.org/10.1016/j.cct.2021.106659.
Funding
Dr. Goenka acknowledges grants from non-profit entities such as the Champions for Hope Pancreatic Cancer Research Program of the Funk Zitiello Foundation, the Centene Charitable Foundation, and the Advance the Practice Award from the Department of Radiology, Mayo Clinic, Rochester, Minnesota. Unrelated to this work (Dr. Goenka): CA190188, Department of Defense (DoD), Office of the Congressionally Directed Medical Research Programs (CDMRP); R01CA256969, National Cancer Institute (NCI) of the National Institutes of Health (NIH); R01CA272628- 01, National Cancer Institute (NCI) of the National Institutes of Health (NIH); Institutional research grant from Sofie Biosciences and Clovis Oncology; Advisory Board (ad hoc), BlueStar Genomics; Consultant, Bayer Healthcare, LLC; Consultant, Candel Therapeutics; Consultant, UWorld.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interest
Authors have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mukherjee, S., Korfiatis, P., Patnam, N.G. et al. Assessing the robustness of a machine-learning model for early detection of pancreatic adenocarcinoma (PDA): evaluating resilience to variations in image acquisition and radiomics workflow using image perturbation methods. Abdom Radiol 49, 964–974 (2024). https://doi.org/10.1007/s00261-023-04127-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-023-04127-1