Abstract
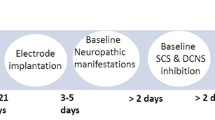
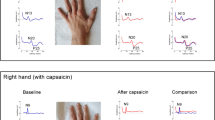
Previous studies from our laboratory showed that in the anesthetized cat, the intradermal injection of capsaicin in the hindpaw facilitated the intraspinal field potentials (IFPs) evoked by stimulation of the intermediate and high-threshold myelinated fibers in the posterior articular nerve (PAN). The capsaicin-induced facilitation was significantly reduced 3–4 h after the injection, despite the persistence of hindpaw inflammation. Although this effect was attributed to an incremented descending inhibition acting on the spinal pathways, it was not clear if it was set in operation once the capsaicin-induced effects exceeded a certain threshold, or if it was continuously operating to keep the increased neuronal activation within manageable limits. To evaluate the changes in descending inhibition, we now examined the effects of successive reversible spinal blocks on the amplitude of the PAN IFPs evoked at different times after the intradermal injection of capsaicin. We found that after capsaicin the PAN IFPs recorded in laminae III–V by activation of high-threshold nociceptive Aδ myelinated fibers increased gradually during successive reversible spinal blocks, while the IFPs evoked by intermediate and low threshold proprioceptive Aβ afferents were only slightly affected. It is concluded that during the development of the central sensitization produced by capsaicin, there is a gradual increase of descending inhibition that tends to limit the nociceptive-induced facilitation, mainly by acting on the neuronal populations receiving inputs from the capsaicin-activated afferents without significantly affecting the information on joint angle transmitted by the low threshold afferents.







Similar content being viewed by others
References
Basbaum AI, Bautista DM, Scherrer G, Julius D (2009) Cellular and molecular mechanisms of pain. Cell 139:267–284
Caterina MJ, Schumacher MA, Rosen TA, Levine JD, Julius D (1997) The capsaicin receptor: a heat-activated ion channel in the pain pathway. Nature 389:816–824
Cervero F, Plenderleith B (1985) C-fibre excitation and tonic descending inhibition of dorsal horn neurones in adult rats treated at birth with capsaicin. J Physiol 365:223–237
Cervero F, Schaible HG, Schmidt RF (1991) Tonic descending inhibition of spinal cord neurones driven by joint afferents in normal cats and in cats with an inflamed knee joint. Exp Brain Res 83:675–678
Cholewinski A, Burgess GM, Bevan S (1993) The role of calcium in capsaicin-induced desensitization in rat cultured dorsal root ganglion neurons. Neuroscience 55:1015–1023
Contreras-Hernández E, Chávez D, Hernández E, Velázquez E, Reyes P, Béjar J, Martín M, Cortés U, Glusman S, Rudomin P (2018) Supraspinal modulation of neuronal synchronization by nociceptive stimulation induces and enduring reorganization of dorsal horn neuronal connectivity. J Physiol 596:1747–1776
Docherty RJ, Robertson B, Bevan S (1991) Capsaicin causes prolonged inhibition of voltage-activated calcium currents in adult rat dorsal root ganglion neurons in culture. Neuroscience 40:513–521
Dougherty PM, Willis WD (1992) Enhanced responses of spinothalamic tract neurons to excitatory amino acids accompany capsaicin-induced sensitization in the monkey. J Neurosci 12:883–894
Eccles JC, Magni F, Willis WD (1962) Depolarization of central terminals of group I afferent fibres from muscle. J Physiol 160:62–93
Fields HL, Heinricher MM, Mason P (1991) Neurotransmitters in nociceptive modulatory circuits. Annu Rev Neurosci 14:219–245
Franco-Cereceda A, Henke H, Lundberg JM, Petermann JB, Hökfelt T, Fischer JA (1987) Calcitonin gene-related peptide (CGRP) in capsaicin-sensitive substance P-immunoreactive sensory neurons in animals and man: distribution and release by capsaicin. Peptides 8:399–410
Globe D, Bayliss MS, Harrison DJ (2009) The impact of itch symptoms in psoriasis: results from physician interviews and patient focus groups. Health Qual Life Outcomes 7:62
Grundy D (2015) Principles and standards for reporting animal experiments in The Journal of Physiology and Experimental Physiology. J Physiol 593:2547–2549
Hayes AG, Tyers MB (1980) Effects of capsaicin on nociceptive heat, pressure and chemical thresholds and on substance P levels in the rat. Brain Res 189:561–564
Helliwell PS, Taylor WJ (2005) Classification and diagnostic criteria for psoriatic arthritis. Ann Rheum Dis 64:ii3–ii8
Ikoma A, Rukwied R, Ständer S, Steinhoff M, Miyachi Y, Schmelz M (2003) Neuronal sensitization for histamine-induced itch in lesional skin of patients with atopic dermatitis. Arch Dermatol 139:1455–1458
Ikoma A, Fartasch M, Heyer G, Miyachi Y, Handwerker H, Schmelz M (2004) Painful stimuli evoke itch in patients with chronic pruritus central sensitization for itch. Neurology 62:212–217
Jankowska E, Riddell JS, McCrea DA (1993) Primary afferent depolarization of myelinated fibres in the joint and interosseous nerves of the cat. J Physiol 466:115–131
Julius D, Basbaum AI (2001) Molecular mechanisms of nociception. Nature 413:203–210
Kilo S, Schmelz M, Koltzenburg M, Handwerker HO (1994) Different patterns of hyperalgesia induced by experimental inflammation in human skin. Brain 117:385–396
Koplas PA, Rosenburg RL, Oxford GS (1997) The role of calcium in the desensitization of capsaicin responses in rat dorsal root ganglion neurons. J Neurosci 17:3525–3537
Lafleur J, Zytnicki D, Horcholle-Bossavit G, Jami I (1992) Depolarization of Ib afferent axons in the cat spinal cord during homonymous muscle contraction. J Physiol 445:345–354
Laird JM, Cervero F (1990) Tonic descending influences on receptive-field properties of nociceptive dorsal horn neurons in sacral spinal cord of rat. J Neurophysiol 63:1022–1032
LaMotte RH, Shain CN, Simone DA, Tsai EF (1991) Neurogenic hyperalgesia: psychophysical studies of underlying mechanisms. J Neurophysiol 66:190–211
LaMotte RH, Lundberg LE, Torebjörk HE (1992) Pain, hyperalgesia and activity in nociceptive C units in humans after intradermal injection of capsaicin. J Physiol 448:749–764
Latremoliere A, Woolf CJ (2009) Central sensitization: a generator of pain hypersensitivity by central neuronal plarticity. Pain 10:895–926
Light AR, Kavookjian AM (1988) Morphology and ultrastructure of physiologically identified substantia gelatinosa (lamina II) neurons with axons that terminate in deeper dorsal horn laminae (III–IV). J Comp Neurol 267:172–189
Lin Q, Wu J, Willis WD (1999) Dorsal root reflexes and cutaneous neurogenic inflammation after intradermal injection of capsaicin in rats. J Neurophysiol 82:2602–2611
Lin Q, Zou X, Willis WD (2000) Aδ and C primary afferents convey dorsal root reflexes after intradermal injection of capsaicin in rats. J Neurophysiol 84:2695–2698
Lundberg JM, Franco-Cereceda A, Hua X, Hökfelt T, Fisher JA (1985) Co-existence of substance P and calcitonin gene-related peptide-like inmunoreactivities in sensory nerves in relation to cardiovascular and bronchoconstrictor effects of capsaicin. Eur J Pharmacol 108:315–319
Lynn B (1990) Capsaicin: actions on nociceptive C-fibres and therapeutic potential. Pain 41:61–69
McIntyre AK, Proske U, Tracey DJ (1978) Afferent fibres from muscle receptors in the posterior nerve of the cat’s knee joint. Exp Brain Res 33:415–424
Murphy RM, Zemlan FP (1987) Differential effects of substance P on serotonin-modulated spinal nociceptive reflexes. Psychopharmacology 93:118–121
Oku R, Satoh M, Fujii N, Otaka A, Yajima H, Takagi H (1987) Calcitonin gene-related peptide promotes mechanical nociception by potentiating release of substance P from the spinal dorsal horn in rats. Brain Res 403:350–354
Omote K, Kawamata T, Kawamata M, Namiki A (1998) Formalin-induced nociception activates a monoaminergic descending inhibitory system. Brain Res 814:194–198
Park KM, Max MB, Robinovits E, Gracely RH, Bennett GJ (1995) Effects of intravenous ketamine, alfentanil, pinprick hyperalgesia, and allodynia produced by intradermal capsaicin in human subjects. Pain 63:163–172
Quevedo J, Eguibar JR, Jiménez I, Schmidt RF, Rudomin P (1993) Primary afferent depolarization of muscle afferents elicited by stimulation of joint afferents in cats with intact neuraxis and during reversible spinalization. J Neurophysiol 70:1899–1910
Quevedo J, Eguibar JR, Jiménez I, Rudomin P (1995) Raphe magnus and reticulospinal actions on primary afferent depolarization of group I muscle afferents in the cat. J Physiol 482:623–640
Ramírez-Morales A, Hernández E, Rudomín P (2011) During acute capsaicin skin inflammation, increased descending control induces unmasking of autogenetic pad in articular afferents. Abstr Soc Neurosci 804:13
Ramírez-Morales A, Hernández E, Rudomín P (2014) Intradermic capsaicin increases autogenic and heterogenic PAD in Aδ articular afferents as part of a control mechanism that regulates information flow in nociceptive afferents. Abstr Soc Neurosci 627:04
Ren K, Dubner R (1996) Enhanced descending modulation of nociception in rats with persistent hindpaw inflammation. J Neurophysiol 70:3025–3037
Ren K, Dubner R (2002) Descending modulation in persistent pain: an update. Pain 100:1–6
Ren Y, Zou X, Fang L, Lin Q (2005) Sympathetic modulation of activity in A sympathetic modulation of activity in Aδ- and C-primary nociceptive afferents after intradermal injection of capsaicin in rats. J Neurophysiol 93:365–377
Rudomin P, Hernández E (2008) Changes in synaptic effectiveness of myelinated joint afferents during capsaicin-induced inflammation of the footpad in the anesthetized cat. Exp Brain Res 187:71–84
Rudomin P, Lomelí J (2007) Patterns of primary afferent depolarization of segmental and ascending intraspinal collaterals of single joint afferents in the cat. Exp Brain Res 176:119–131
Rudomin P, Hernández E, Lomelí J (2007) Tonic and phasic differential GABAergic inhibition of synaptic actions of joint afferents in the cat. Exp Brain Res 176:98–118
Russell LC, Burchiel KJ (1984) Neurophysiological effects of capsaicin. Brain Res Rev 8:165–176
Sakurada T, Komatsu T, Moriyama T, Sasaki M, Sanai K, Orito T, Sakurada C, Sakurada S (2005) Effects of intraplantar injections of nocicpetin and its N-terminal fragments on nociceptive and desensitized responses induced by capsaicin in mice. Peptides 26:2505–2512
Schaible HG, Schmidt RF, Willis WD (1986) Responses of spinal cord neurones to stimulation of articular afferent fibres in the cat. J Physiol 372:575–593
Schaible HG, Schmidt RF, Willis WD (1987a) Convergent inputs from articular, cutaneous and muscle receptors onto ascending tract cells in the cat spinal cord. Exp Brain Res 66:479–488
Schaible H, Schmidt RF, Willis WD (1987b) Enhancement of the responses of ascending tract cells in the cat spinal cord by acute inflammation of the knee joint. Exp Brain Res 66:489–499
Schaible HG, Jarrott B, Hope PJ, Duggan AW (1990) Release of immunoreactive substance P in the cat spinal cord during development of acute arthritis in cat’s knee: a study with antibody bearing microprobes. Brain Res 529:214–223
Schaible HG, Neugebauer V, Cervero F, Schmidt RF (1991) Changes in tonic descending inhibition of spinal neurons with articular input during the development of acute arthritis in the cat. J Neurophysiol 66:1021–1032
Schaible HG, Hope PJ, Lang CW, Duggan AW (1992) Calcitonin gene-related peptide causes intraspinal spreading of substance P released by peripheral stimulation. Eur J Neurosci 4:750–757
Seki K, Perlmutter SI, Fetz EE (2003) Sensory input to primate spinal cord is presynaptically inhibited during voluntary movement. Nature Neurosci 6:1309–1316
Simone DA, Baumann TK, LaMotte RH (1989) Dose-dependent pain and mechanical hyperalgesia in humans after intradermal injection of capsaicin. Pain 38:99–107
Simone DA, Sorkin LS, Oh U, Chung JM, Owens C, LaMotte RH, Willis WD (1991) Neurogenic hyperalgesia: central neural correlates in responses of spinothalamic tract neurons. J Neurophysiol 66:228–246
Sluka KA (1997) Blockade of calcium channels can prevent the onset of secondary hyperalgesia and allodynia induced by intradermal injection of capsaicin in rats. Pain 71:157–164
Sorkin LS, McAdoo DJ (1993) Amino acids and serotonin are released into the lumbar spinal cord of the anesthetized cat following intradermal capsaicin injections. Brain Res 607:89–98
Szolcsányi J (2004) Forty years in capsaicin research for sensory pharmacology and physiology. Neuropeptides 38:377–384
Todd AJ (2010) Neuronal circuitry for pain processing in the dorsal horn. Nat Rev Neurosci 11:823–836
Torebjörk HE, Lundberg LE, LaMotte RH (1992) Central changes in processing of mechanoreceptive input in capsaicin-induced secondary hyperalgesia in humans. J Physiol 448(765–7):80
Vanegas H, Schaible HG (2004) Descending control of persistent pain: inhibitory or facilitatory? Brain Res Rev 46:295–309
Wall PD, Werman R (1976) The physiology and anatomy of long ranging afferent fibres within the spinal cord. J Physiol 255:321–334
Wang J, Ren Y, Zou X, Fang L, Willis WD, Lin Q (2004) Sympathetic influence on capsaicin-evoked enhancement of dorsal root reflexes in rats. J Neurophysiol 92:2017–2026
Willis WD (2002) Long-term potenitiation in spinothalamic neurons. Brain Res Rev 40:202–214
Winter J, Bevan S, Campbell EA (1995) Capsaicin and pain mechanisms. Br J Anaesth 75:157–168
Woolf JC (1995) Somatic pain—pathogenesis and prevention. Br J Anaesth 75:169–176
Woolf JC (2011) Central sensitization: implications for the diagnosis and treatment of pain. Pain 152:S2–S15
Acknowledgements
We would like to thank Dr. S. Glusman for his comments to an earlier version of this paper, to C. León for technical assistance and to E. Rosales for her excellent secretarial support.
Funding
This work was partly supported CONACyT Grants 50900 and 255548. AR was holder of a CONACyT fellowship for doctoral studies.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ramírez-Morales, A., Hernández, E. & Rudomin, P. Descending inhibition selectively counteracts the capsaicin-induced facilitation of dorsal horn neurons activated by joint nociceptive afferents. Exp Brain Res 237, 1629–1641 (2019). https://doi.org/10.1007/s00221-019-05535-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00221-019-05535-w