Abstract
Rationale
Minocycline, a tetracycline antibiotic, inhibits activation of microglia. In preclinical studies, minocycline prevented development of opioid tolerance and opioid-induced hyperalgesia (OIH). The goal of this study was to determine if minocycline changes pain threshold and tolerance in individuals with opioid use disorder who are maintained on agonist treatment.
Methods
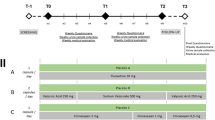
In this double-blind, randomized human laboratory study, 20 participants were randomized to either minocycline (200 mg/day) or placebo treatment for 15 days. The study had three test sessions (days 1, 8, and 15 of treatment) and one follow-up visit 1 week after the end of treatment. In each test session, participants were assessed on several subjective and cognitive measures, followed by assessment of pain sensitivity using the Cold Pressor Test (CPT). Daily surveys and cognitive measures using Ecological Momentary Assessment (EMA) were also collected four times a day on days 8 through 14 of treatment, and proinflammatory serum cytokines were assessed before and on the last day of treatment.
Results
Minocycline treatment did not change pain threshold or tolerance on the CPT. Similarly, minocycline did not change severity of pain, opioid craving, withdrawal, or serum cytokines. Minocycline treatment increased accuracy on a Go/No-Go task.
Conclusions
While these findings do not support minocycline’s effects on OIH, minocycline may have a potential use as a cognitive enhancer for individuals with opioid use disorder, a finding that warrants further systematic studies.
Similar content being viewed by others
References
Akgűn E, Lunzer MM, Portoghese P (2018) Combined glia inhibition and opioid receptor agonism afford highly potent analgesics without tolerance ACS chemical neuroscience
Arezoomandan R, Haghparast A (2015) Administration of the glial cell modulator, minocycline, in the nucleus accumbens attenuated the maintenance and reinstatement of morphine-seeking behavior. Can J Physiol Pharmacol 94:257–264
Arout CA, Edens E, Petrakis IL, Sofuoglu M (2015) Targeting opioid-induced hyperalgesia in clinical treatment: neurobiological considerations. CNS drugs 29:465–486
Bachtell RK, Jones JD, Heinzerling KG, Beardsley PM, Comer SD (2017) Glial and neuroinflammatory targets for treating substance use disorders. Drug Alcohol Depend 180:156–170
Baldacchino A, Armanyous M, Balfour D, Humphris G, Matthews K (2017) Neuropsychological functioning and chronic methadone use: a systematic review and meta-analysis. Neurosci Biobehav Rev 73:23–38
Chapman CR, Lipschitz DL, Angst MS, Chou R, Denisco RC, Donaldson GW, Fine PG, Foley KM, Gallagher RM, Gilson AM, Haddox JD, Horn SD, Inturrisi CE, Jick SS, Lipman AG, Loeser JD, Noble M, Porter L, Rowbotham MC, Schoelles KM, Turk DC, Volinn E, von Korff MR, Webster LR, Weisner CM (2010) Opioid pharmacotherapy for chronic non-cancer pain in the United States: a research guideline for developing an evidence-base. J Pain 11:807–829
Chu LF, Clark DJ, Angst MS (2006) Opioid tolerance and hyperalgesia in chronic pain patients after one month of oral morphine therapy: a preliminary prospective study. J Pain 7:43–48
Compton MA (1994) Cold-pressor pain tolerance in opiate and cocaine abusers: correlates of drug type and use status. J Pain Symptom Manag 9:462–473
Compton P, Kehoe P, Sinha K, Torrington MA, Ling W (2010) Gabapentin improves cold-pressor pain responses in methadone-maintained patients. Drug Alcohol Depend 109:213–219
Compton P, Canamar CP, Hillhouse M, Ling W (2012) Hyperalgesia in heroin dependent patients and the effects of opioid substitution therapy. J Pain 13:401–409
Cui Y, Liao XX, Liu W, Guo RX, Wu ZZ, Zhao CM, Chen PX, Feng JQ (2008) A novel role of minocycline: attenuating morphine antinociceptive tolerance by inhibition of p38 MAPK in the activated spinal microglia. Brain Behav Immun 22:114–123. https://doi.org/10.1016/j.bbi.2007.07.014
Curtin CM, Kenney D, Suarez P, Hentz VR, Hernandez-Boussard T, Mackey S, Carroll IR (2017) A double-blind placebo randomized controlled trial of minocycline to reduce pain after carpal tunnel and trigger finger release. J Hand Surg 42:166–174. https://doi.org/10.1016/j.jhsa.2016.12.011
Darcq E, Kieffer BL (2018) Opioid receptors: drivers to addiction? Nat Rev Neurosci 19(8):499–514. https://doi.org/10.1038/s41583-018-0028-x
Doverty M, White JM, Somogyi AA, Bochner F, Ali R, Ling W (2001) Hyperalgesic responses in methadone maintenance patients. Pain 90:91–96
Garland EL, Brown SM, Howard MO (2016) Thought suppression as a mediator of the association between depressed mood and prescription opioid craving among chronic pain patients. J Behav Med 39:128–138
Handelsman L, Cochrane KJ, Aronson MJ, Ness R, Rubinstein KJ, Kanof PD (1987) Two new rating scales for opiate withdrawal. Am J Drug Alcohol Abuse 13:293–308
Hou Y, Xie G, Liu X, Li G, Jia C, Xu J, Wang B (2016) Minocycline protects against lipopolysaccharide-induced cognitive impairment in mice. Psychopharmacology 233:905–916
Hutchinson MR, Northcutt AL, Chao LW, Kearney JJ, Zhang Y, Berkelhammer DL, Loram LC, Rozeske RR, Bland ST, Maier SF, Gleeson TT, Watkins LR (2008) Minocycline suppresses morphine-induced respiratory depression, suppresses morphine-induced reward, and enhances systemic morphine-induced analgesia. Brain Behav Immun 22:1248–1256
Hutchinson MR et al (2010) Evidence that opioids may have toll-like receptor 4 and MD-2 effects. Brain, Behav Immun 24:83–95
Jin W-J, Feng S-W, Feng Z, Lu S-M, Qi T, Qian Y-N (2014) Minocycline improves postoperative cognitive impairment in aged mice by inhibiting astrocytic activation. Neuroreport 25:1–6
Kato TA, Watabe M, Tsuboi S, Ishikawa K, Hashiya K, Monji A, Utsumi H, Kanba S (2012) Minocycline modulates human social decision-making: possible impact of microglia on personality-oriented social behaviors. PLoS One 7:e40461
Keller S, Bann CM, Dodd SL, Schein J, Mendoza TR, Cleeland CS (2004) Validity of the brief pain inventory for use in documenting the outcomes of patients with noncancer pain. Clin J Pain 20:309–318
Koltzenburg M, Pokorny R, Gasser UE, Richarz U (2006) Differential sensitivity of three experimental pain models in detecting the analgesic effects of transdermal fentanyl and buprenorphine. Pain 126:165–174. https://doi.org/10.1016/j.pain.2006.06.028
Li Q (2012) Antagonists of toll like receptor 4 maybe a new strategy to counteract opioid-induced hyperalgesia and opioid tolerance. Med Hypotheses 79:754–756
Martel MO, Finan PH, McHugh RK, Issa M, Edwards RR, Jamison RN, Wasan AD (2016) Day-to-day pain symptoms are only weakly associated with opioid craving among patients with chronic pain prescribed opioid therapy. Drug Alcohol Depend 162:130–136
McNair D, Lorr M, Droppleman L (1992) POMS Manual–Profile of Mood Questionnaire San Diego: Edits
Melzack R (1987) The short-form McGill pain questionnaire. Pain 30:191–197
Mika J, Osikowicz M, Makuch W, Przewlocka B (2007) Minocycline and pentoxifylline attenuate allodynia and hyperalgesia and potentiate the effects of morphine in rat and mouse models of neuropathic pain. Eur J Pharmacol 560:142–149
Pocock JM, Kettenmann H (2007) Neurotransmitter receptors on microglia. Trends Neurosci 30:527–535. https://doi.org/10.1016/j.tins.2007.07.007
Rezapour T, DeVito EE, Sofuoglu M, Ekhtiari H (2016) Perspectives on neurocognitive rehabilitation as an adjunct treatment for addictive disorders: from cognitive improvement to relapse prevention. In: Progress in brain research, vol 224. Elsevier, pp 345–369
Ricardo Buenaventura M, Rajive Adlaka M, Nalini Sehgal M (2008) Opioid complications and side effects. Pain Phys 11:S105–S120
Robertson IH, Manly T, Andrade J, Baddeley BT, Yiend J (1997) Oops!': performance correlates of everyday attentional failures in traumatic brain injured and normal subjects. Neuropsychologia 35:747–758
Samour MS, Nagi SS, Shortland PJ, Mahns DA (2017) Minocycline prevents muscular pain hypersensitivity and cutaneous allodynia produced by repeated intramuscular injections of hypertonic saline in healthy human participants. J Pain 18:994–1005. https://doi.org/10.1016/j.jpain.2017.03.009
Smith AM, Dragunow M (2014) The human side of microglia. Trends Neurosci 37:125–135
Sofuoglu M, Waters AJ, Mooney M, O'malley SS (2009) Minocycline reduced craving for cigarettes but did not affect smoking or intravenous nicotine responses in humans. Pharmacol Biochem Behav 92:135–140
Sofuoglu M, Mooney M, Kosten T, Waters A, Hashimoto K (2011) Minocycline attenuates subjective rewarding effects of dextroamphetamine in humans. Psychopharmacology 213:61–68
Sofuoglu M, DeVito EE, Waters AJ, Carroll KM (2013) Cognitive enhancement as a treatment for drug addictions. Neuropharmacology 64:452–463
Stone AA, Shiffman S (1994) Ecological momentary assessment (EMA) in behavorial medicine Annals of Behavioral Medicine
Thorndike EL (1919) A standardized group examination of intelligence independent of language. J Appl Psychol 3(13):13–32
Trang T, Al-Hasani R, Salvemini D, Salter MW, Gutstein H, Cahill CM (2015) Pain and poppies: the good, the bad, and the ugly of opioid analgesics. J Neurosci 35:13879–13888
Vanelderen P, van Zundert J, Kozicz T, Puylaert M, de Vooght P, Mestrum R, Heylen R, Roubos E, Vissers K (2015) Effect of minocycline on lumbar radicular neuropathic pain: a randomized, placebo-controlled, double-blind clinical trial with amitriptyline as a comparator. Anesthesiology 122:399–406. https://doi.org/10.1097/aln.0000000000000508
Wadhwa M, Prabhakar A, Ray K, Roy K, Kumari P, Jha PK, Kishore K, Kumar S, Panjwani U (2017) Inhibiting the microglia activation improves the spatial memory and adult neurogenesis in rat hippocampus during 48 h of sleep deprivation. J Neuroinflammation 14:222
Watabe M, Kato TA, Monji A, Horikawa H, Kanba S (2012) Does minocycline, an antibiotic with inhibitory effects on microglial activation, sharpen a sense of trust in social interaction? Psychopharmacology 220:551–557
Watkins LR, Hutchinson MR, Rice KC, Maier SF (2009) The "toll" of opioid-induced glial activation: improving the clinical efficacy of opioids by targeting glia. Trends Pharmacol Sci 30:581–591. https://doi.org/10.1016/j.tips.2009.08.002
Zhang X, Wang J, Yu T, Du D, Jiang W (2015) Minocycline can delay the development of morphine tolerance, but cannot reverse existing tolerance in the maintenance period of neuropathic pain in rats. Clin Exp Pharmacol Physiol 42:94–101
Zhang L, Zheng H, Wu R, Zhu F, Kosten TR, Zhang XY, Zhao J (2018) Minocycline adjunctive treatment to risperidone for negative symptoms in schizophrenia: association with pro-inflammatory cytokine levels. Prog Neuro-Psychopharmacol Biol Psychiatry 85:69–76. https://doi.org/10.1016/j.pnpbp.2018.04.004
Acknowledgments
This study was conducted during Dr. Arout’s postdoctoral fellowship at Yale University School of Medicine (NIDA T32 DA007238; Principal Investigator: I. L. Petrakis) and was supported by the VA New England Mental Illness Research, Education and Clinical Center (MIRECC). We would like to thank Dr. Lesley Devine of Yale University School of Medicine for executing the serum cytokine analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that there is no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article belongs to a Special Issue on Neuroimmune Signaling in Psychiatric Disease
Electronic supplementary material
ESM 1
(DOCX 20 kb)
Rights and permissions
About this article
Cite this article
Arout, C.A., Waters, A.J., MacLean, R.R. et al. Minocycline does not affect experimental pain or addiction-related outcomes in opioid maintained patients. Psychopharmacology 236, 2857–2866 (2019). https://doi.org/10.1007/s00213-018-5146-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00213-018-5146-7