Abstract
Summary
We evaluated mortality in a cohort of hip fracture patients and implemented a risk prediction score named ASAgeCoGeCC with excellent discrimination. It allowed to separate patients in 3 different risk groups with distinct mortality rates. Recognition of the heterogeneity of patients with femoral fractures may have relevant implications for their management.
Introduction
Usage of risk prediction models to estimate postoperative mortality risk for hip fracture patients represents a useful tool to give insight in the prognosis and assist in clinical decision-making. The aim of this study was to identify a predictive model able to determine the possible presence of distinct subgroups of hip fracture patients by risk classes in the mid-term.
Methods
Three hundred twenty-three hip fracture patients were evaluated, and mortality rates at 30 days, 1, 2, and 4 years were calculated. A multivariate logistic regression analysis using mortality 4 years after fracture as a dependent variable found ASA score, age, cognitive status, gender, and Charlson Comorbidities Index (CCI) as significant risk factors. Using these items, a score named ASAgeCoGeCC was implemented and compared with CCI and Nottingham Hip Fracture Score (NHFS) by a receiver operating characteristic (ROC) curve.
Results
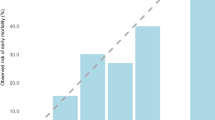
The area under the ROC curve for ASAgeCoGeCC was always greater than that of CCI and NHFS and ranged between 0.804 and 0.820 suggesting an excellent discrimination. The ASAgeCoGeCC logistic model showed also a good calibration. Patients were divided in 3 groups: a low risk group, an intermediate risk group with an odds ratio for 4-year mortality of 5.6 (95% CI 2.9–10.6), and a high risk group with an odds ratio 21.6 (95% CI 10.6–44).
Conclusion
The ASAgeCoGeCC Score is a predictive tool for mortality after hip fracture with good calibration and excellent discrimination properties. It is the first scoring system stratifying hip fracture patients’ mortality at 4 years from fracture.



Similar content being viewed by others
References
Svedbom A, Hernlund E, Ivergård M, Compston J, Cooper C, Stenmark J, McCloskey EV, Jönsson B, Kanis JA (2013) Osteoporosis in the European Union: a compendium of country-specific reports. Arch Osteoporos 8:137. https://doi.org/10.1007/s11657-013-0137-0
Gjertsen JE, Dybvik E, Furnes O, Fevang JM, Havelin LI, Matre K, Engesæter LB (2017) Improved outcome after hip fracture surgery in Norway. Acta Orthop 88:505–511. https://doi.org/10.1080/17453674.2017.1344456
Karres J, Heesakkers NA, Ultee JM, Vrouenraets BC (2015) Predicting 30-day mortality following hip fracture surgery: evaluation of six risk prediction models. Injury 46:371–377. https://doi.org/10.1016/j.injury.2014.11.004
Marufu TC, Mannings A, Moppett IK (2015) Risk scoring models for predicting peri-operative morbidity and mortality in people with fragility hip fractures: qualitative systematic review. Injury 46:2325–2334. https://doi.org/10.1016/j.injury.2015.10.025
Burgos E, Gómez-Arnau JI, Díez R, Muñoz L, Fernández-Guisasola J, Garcia del Valle S (2008) Predictive value of six risk scores for outcome after surgical repair of hip fracture in elderly patients. Acta Anaesthesiol Scand 52:125–131. https://doi.org/10.1111/j.1399-6576.2007.01473.x
Hu F, Jiang C, Shen J, Tang P, Wang Y (2012) Preoperative predictors for mortality following hip fracture surgery: a systematic review and meta-analysis. Injury 43:676–685. https://doi.org/10.1016/j.injury.2011.05.017
Smith T, Pelpola K, Ball M, Ong A, Myint PK (2014) Pre-operative indicators for mortality following hip fracture surgery: a systematic review and meta-analysis. Age Ageing 43:464–471. https://doi.org/10.1093/ageing/afu065
Haentjens P, Magaziner J, Colón-Emeric CS, Vanderschueren D, Milisen K, Velkeniers B, Boonen S (2010) Meta-analysis: excess mortality after hip fracture among older women and men. Ann Intern Med 152:380–390. https://doi.org/10.7326/0003-4819-152-6-201003160-00008
Mellner C, Hedström M, Hommel A, Sköldenberg O, Eisler T, Mukka S (2020) The Sernbo score as a predictor of 1-year mortality after hip fracture: a registry study on 55,716 patients. Eur J Trauma Emerg Surg. https://doi.org/10.1007/s00068-020-01375-4, https://doi.org/10.1007/s00068-020-01375-4
Folstein MF, Folstein SE, McHugh PR (1975) Mini-mental state. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12:189–198. https://doi.org/10.1016/0022-3956(75)90026-6
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383. https://doi.org/10.1016/0021-9681(87)90171-8
Charlson M, Szatrowski TP, Peterson J, Gold J (1994) Validation of a combined comorbidity index. J Clin Epidemiol 47:1245–1251. https://doi.org/10.1016/0895-4356(94)90129-5
Maxwell MJ, Moran CG, Moppett IK (2008) Development and validation of a preoperative scoring system to predict 30 day mortality in patients undergoing hip fracture surgery. Br J Anaesth 101:511–517. https://doi.org/10.1093/bja/aen236
Regione Lombardia (2019) Sistema Informativo Socio Sanitario. http://www.siss.regione.lombardia.it. Accessed 29 january 2021
Hanley JA, McNeil BJ (1982) The meaning and use of the area under a receiver operating characteristic (ROC) curve. Radiology 143:29–36. https://doi.org/10.1148/radiology.143.1.7063747
Youden WJ (1950) Index for rating diagnostic tests. Cancer 3:32–35
Lemeshow S, Hosmer DW Jr (1982) A review of goodness of fit statistics for use in the development of logistic regression models. Am J Epidemiol 115:92–106. https://doi.org/10.1093/oxfordjournals.aje.a113284
Trevisan C, Gallinari G, Klumpp R, Menon A, Compagnoni R (2019) Year to year comparison of 2000-2015 in hip fracture management: same survival rate despite older and more fragile patients. Aging Clin Exp Res 31:1097–1103. https://doi.org/10.1007/s40520-018-1047-1
Neuhaus V, King J, Hageman MG, Ring DC (2013) Charlson comorbidity indices and in-hospital deaths in patients with hip fractures. Clin Orthop Relat Res 471:1712–1719. https://doi.org/10.1007/s11999-012-2705-9
Toson B, Harvey LA, Close JC (2015) The ICD-10 Charlson Comorbidity Index predicted mortality but not resource utilization following hip fracture. J Clin Epidemiol 68:44–51. https://doi.org/10.1016/j.jclinepi.2014.09.017
Cher EWL, Allen JC, Howe TS, Koh JSB (2019) Comorbidity as the dominant predictor of mortality after hip fracture surgeries. Osteoporos Int 30:2477–2483. https://doi.org/10.1007/s00198-019-05139-8
Khan MA, Hossain FS, Ahmed I, Muthukumar N, Mohsen A (2013) Predictors of early mortality after hip fracture surgery. Int Orthop 37:2119–2124. https://doi.org/10.1007/s00264-013-2068-1
Barceló M, Torres OH, Mascaró J, Casademont J (2021) Hip fracture and mortality: study of specific causes of death and risk factors. Arch Osteoporos 16:15. https://doi.org/10.1007/s11657-020-00873-7
Roberts KC, Brox WT, Jevsevar DS, Sevarino K (2015) Management of hip fractures in the elderly. J Am Acad Orthop Surg 23:131–137. https://doi.org/10.5435/JAAOS-D-14-00432
Bliemel C, Sielski R, Doering B, Dodel R, Balzer-Geldsetzer M, Ruchholtz S, Buecking B (2016) Pre-fracture quality of life predicts 1-year survival in elderly patients with hip fracture-development of a new scoring system. Osteoporos Int 27:1979–1987. https://doi.org/10.1007/s00198-015-3472-8
Yin P, Lv H, Zhang L, Long A, Zhang L, Tang P (2016) Combination of red cell distribution width and American Society of Anesthesiologists score for hip fracture mortality prediction. Osteoporos Int 27:2077–2087. https://doi.org/10.1007/s00198-015-3357-x
Mellner C, Eisler T, Börsbo J, Brodén C, Morberg P, Mukka S (2017) The Sernbo score predicts 1-year mortality after displaced femoral neck fractures treated with a hip arthroplasty. Acta Orthop 88:402–406. https://doi.org/10.1080/17453674.2017.1318628
Khosla S, Cauley JA, Compston J, Kiel DP, Rosen C, Saag KG, Shane E (2017) Addressing the crisis in the treatment of osteoporosis: a path forward. J Bone Miner Res 32:424–430. https://doi.org/10.1002/jbmr.3074
Solomon DH, Johnston SS, Boytsov NN, McMorrow D, Lane JM, Krohn KD (2014) Osteoporosis medication use after hip fracture in U.S. patients between 2002 and 2011. J Bone Miner Res 29:1929–1937. https://doi.org/10.1002/jbmr.2202
Hurtado I, García-Sempere A, Peiró S, Rodríguez-Bernal C, Sanfélix-Genovés J, Sanfélix-Gimeno G (2020) Trends and geographical variability in osteoporosis treatment after hip fracture: a multilevel analysis of 30,965 patients in the region of Valencia, Spain. J Bone Miner Res 35:1660–1667. https://doi.org/10.1002/jbmr.4028
Sale JEM, Yang A, Elliot-Gibson V, Jain R, Sujic R, Linton D, Weldon J, Frankel L, Bogoch E (2021) Patients 80 + have similar medication initiation rates to those aged 50-79 in Ontario FLS. Osteoporos Int. https://doi.org/10.1007/s00198-020-05796-0
Mangione KK, Lopopolo RB, Neff NP, Craik RL, Palombaro KM (2008) Interventions used by physical therapists in home care for people after hip fracture. Phys Ther 88:199–210. https://doi.org/10.2522/ptj.20070023
Singh NA, Quine S, Clemson LM, Williams EJ, Williamson DA, Stavrinos TM, Grady JN, Perry TJ, Lloyd BD, Smith EU, Singh MA (2012) Effects of high-intensity progressive resistance training and targeted multidisciplinary treatment of frailty on mortality and nursing home admissions after hip fracture: a randomized controlled trial. J Am Med Dir Assoc 13:24–30. https://doi.org/10.1016/j.jamda.2011.08.005
Lewis PM (2016) Waddell JP (2016) When is the ideal time to operate on a patient with a fracture of the hip? : a review of the available literature. Bone Joint J 98-B:1573–1581. https://doi.org/10.1302/0301-620X.98B12.BJJ-2016-0362.R2
Öztürk B, Johnsen SP, Röck ND, Pedersen L, Pedersen AB (2019) Impact of comorbidity on the association between surgery delay and mortality in hip fracture patients: a Danish nationwide cohort study. Injury 50:424–431. https://doi.org/10.1016/j.injury.2018.12.03
Trevisan C, Gallinari G, Carbone A, Klumpp R (2021) Fifteen years change in acute management of hip fracture patients: 1-year mortality calls for improvements. Injury 20:S0020-1383(21)00060-7. https://doi.org/10.1016/j.injury.2021.01.025
Mundi S, Pindiprolu B, Simunovic N, Bhandari M (2014) Similar mortality rates in hip fracture patients over the past 31 years. Acta Orthop 85:54–59. https://doi.org/10.3109/17453674.2013.878831
Karampampa K, Ahlbom A, Michaëlsson K, Andersson T, Drefahl S, Modig K (2015) Declining incidence trends for hip fractures have not been accompanied by improvements in lifetime risk or post-fracture survival--a nationwide study of the Swedish population 60 years and older. Bone 78:55–61. https://doi.org/10.1016/j.bone.2015.04.032
Kristensen MT, Kehlet H (2018) The basic mobility status upon acute hospital discharge is an independent risk factor for mortality up to 5 years after hip fracture surgery: survival rates of 444 pre-fracture ambulatory patients evaluated with the Cumulated Ambulation Score. Acta Orthop 89:47–52. https://doi.org/10.1080/17453674.2017.1382038
Tran T, Bliuc D, Pham HM, van Geel T, Adachi JD, Berger C, van den Bergh J, Eisman JA, Geusens P, Goltzman D, Hanley DA, Josse RG, Kaiser SM, Kovacs CS, Langsetmo L, Prior JC, Nguyen TV, Center JR, CaMos Research Group (2020) A risk assessment tool for predicting fragility fractures and mortality in the elderly. J Bone Miner Res 35:1923–1934. https://doi.org/10.1002/jbmr.4100
Bohl DD, Shen MR, Hannon CP, Fillingham YA, Darrith B, Valle CJD (2017) Serum albumin predicts survival and postoperative course following surgery for geriatric hip fracture. J Bone Joint Surg Am 99:2110–2118. https://doi.org/10.2106/JBJS.16.01620
Kim BG, Lee YK, Park HP, Sohn HM, Oh AY, Jeon YT, Koo KH (2016) C-reactive protein is an independent predictor for 1-year mortality in elderly patients undergoing hip fracture surgery: a retrospective analysis. Medicine (Baltimore) 95:e5152. https://doi.org/10.1097/MD.0000000000005152
Chong E, Ho E, Baldevarona-Llego J, Chan M, Wu L, Tay L, Ding YY, Lim WS (2018) Frailty in hospitalized older adults: comparing different frailty measures in predicting short- and long-term patient outcomes. J Am Med Dir Assoc 19:450–457.e3. https://doi.org/10.1016/j.jamda.2017.10.006
Narula S, Lawless A, D'Alessandro P, Jones CW, Yates P, Seymour H (2020) Clinical Frailty Scale is a good predictor of mortality after proximal femur fracture: a cohort study of 30-day and one-year mortality. Bone Jt Open 1:443–449. https://doi.org/10.1302/2633-1462.18.BJO-2020-0089.R1
Pizzonia M, Giannotti C, Carmisciano L, Signori A, Rosa G, Santolini F, Caffa I, Montecucco F, Nencioni A, Monacelli F (2020) Frailty assessment, hip fracture and long-term clinical outcomes in older adults. Eur J Clin Invest 51:e13445. https://doi.org/10.1111/eci.13445
Availability of data and material
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Trevisan, C., Gallinari, G., Carbone, A. et al. Efficiently stratifying mid-term death risk in femoral fractures in the elderly: introducing the ASAgeCoGeCC Score. Osteoporos Int 32, 2023–2031 (2021). https://doi.org/10.1007/s00198-021-05932-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-021-05932-4