Abstract
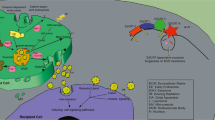
In the past decades, plenty of evidence has gathered pointing to the role of extracellular vesicles (EVs) secreted by irradiated cells in the development of radiation-induced non-targeted effects. EVs are complex natural structures composed of a phospholipid bilayer which are secreted by virtually all cells and carry bioactive molecules. They can travel certain distances in the body before being taken up by recipient cells. In this review we discuss the role and fate of EVs in tumor cells and highlight the importance of DNA specimens in EVs cargo in the context of radiotherapy. The effect of EVs depends on their cargo, which reflects physiological and pathological conditions of donor cell types, but also depends on the mode of EV uptake and mechanisms involved in the route of EV internalization. While the secretion and cargo of EVs from irradiated cells has been extensively studied in recent years, their uptake is much less understood. In this review, we will focus on recent knowledge regarding the EV uptake of cancer cells and the effect of radiation in this process.



Similar content being viewed by others
References
Vinod SK, Hau E (2020) Radiotherapy treatment for lung cancer: current status and future directions. Respirology 25(2):61–71. https://doi.org/10.1111/resp.13870
Shirvani SM, Huntzinger CJ, Melcher T, Olcott PD, Voronenko Y, Bartlett-Roberto J, Mazin S (2021) Biology-guided radiotherapy: redefining the role of radiotherapy in metastatic cancer. Br J Radiol 94:20200873. https://doi.org/10.1259/bjr.20200873
Jokar S, Marques IA, Khazaei S, Martins-Marques T, Girao H, Laranjo M, Botelho MF (2022) The footprint of exosomes in the radiation-induced bystander effects. Bioengineering. https://doi.org/10.3390/bioengineering9060243
Jabbari N, Karimipour M, Khaksar M, Akbariazar E, Heidarzadeh M, Mojarad B, Aftab H, Rahbarghazi R, Rezaie J (2020) Tumor-derived extracellular vesicles: insights into bystander effects of exosomes after irradiation. Lasers Med Sci 35:531–545. https://doi.org/10.1007/s10103-019-02880-8
Reynders K, Illidge T, Siva S, Chang JY, De Ruysscher D (2015) The abscopal effect of local radiotherapy: using immunotherapy to make a rare event clinically relevant. Cancer Treat Rev 41:503–510. https://doi.org/10.1016/j.ctrv.2015.03.011
Hargitai R, Kis D, Persa E, Szatmari T, Safrany G, Lumniczky K (2021) Oxidative stress and gene expression modifications mediated by extracellular vesicles: an in vivo study of the radiation-induced bystander effect. Antioxidants. https://doi.org/10.3390/antiox10020156
Kis D, Csordas IB, Persa E, Jezso B, Hargitai R, Szatmari T, Sandor N, Kis E, Balazs K, Safrany G et al (2022) Extracellular vesicles derived from bone marrow in an early stage of ionizing radiation damage are able to induce bystander responses in the bone marrow. Cells. https://doi.org/10.3390/cells11010155
Kis D, Persa E, Szatmari T, Antal L, Bota A, Csordas IB, Hargitai R, Jezso B, Kis E, Mihaly J et al (2020) The effect of ionising radiation on the phenotype of bone marrow-derived extracellular vesicles. Br J Radiol 93:20200319. https://doi.org/10.1259/bjr.20200319
Szatmari T, Kis D, Bogdandi EN, Benedek A, Bright S, Bowler D, Persa E, Kis E, Balogh A, Naszalyi LN et al (2017) Extracellular vesicles mediate radiation-induced systemic bystander signals in the bone marrow and spleen. Front Immunol 8:347. https://doi.org/10.3389/fimmu.2017.00347
Szatmari T, Persa E, Kis E, Benedek A, Hargitai R, Safrany G, Lumniczky K (2018) Extracellular vesicles mediate low dose ionizing radiation-induced immune and inflammatory responses in the blood. Int J Radiat Biol. https://doi.org/10.1080/09553002.2018.1450533
Mavragani IV, Nikitaki Z, Kalospyros SA, Georgakilas AG (2019) Ionizing radiation and complex DNA damage: from prediction to detection challenges and biological significance. Cancers. https://doi.org/10.3390/cancers11111789
Szatmari T, Hargitai R, Safrany G, Lumniczky K (2019) Extracellular vesicles in modifying the effects of ionizing radiation. Int J Mol Sci. https://doi.org/10.3390/ijms20225527
Jelonek K, Wojakowska A, Marczak L, Muer A, Tinhofer-Keilholz I, Lysek-Gladysinska M, Widlak P, Pietrowska M (2015) Ionizing radiation affects protein composition of exosomes secreted in vitro from head and neck squamous cell carcinoma. Acta Biochim Pol 62:265–272. https://doi.org/10.18388/abp.2015_970
Hurwitz MD, Kaur P, Nagaraja GM, Bausero MA, Manola J, Asea A (2010) Radiation therapy induces circulating serum Hsp72 in patients with prostate cancer. Radiother Oncol 95:350–358. https://doi.org/10.1016/j.radonc.2010.03.024
Mutschelknaus L, Azimzadeh O, Heider T, Winkler K, Vetter M, Kell R, Tapio S, Merl-Pham J, Huber SM, Edalat L et al (2017) Radiation alters the cargo of exosomes released from squamous head and neck cancer cells to promote migration of recipient cells. Sci Rep 7:12423. https://doi.org/10.1038/s41598-017-12403-6
Goliwas KF, Ashraf HM, Wood AM, Wang Y, Hough KP, Bodduluri S, Athar M, Berry JL, Ponnazhagan S, Thannickal VJ et al (2021) Extracellular vesicle mediated tumor-stromal crosstalk within an engineered lung cancer model. Front Oncol 11:654922. https://doi.org/10.3389/fonc.2021.654922
Naito Y, Yoshioka Y, Ochiya T (2022) Intercellular crosstalk between cancer cells and cancer-associated fibroblasts via extracellular vesicles. Cancer Cell Int 22:367. https://doi.org/10.1186/s12935-022-02784-8
Mutschelknaus L, Peters C, Winkler K, Yentrapalli R, Heider T, Atkinson MJ, Moertl S (2016) Exosomes derived from squamous head and neck cancer promote cell survival after ionizing radiation. PLoS ONE 11:e152213. https://doi.org/10.1371/journal.pone.0152213
Arscott WT, Tandle AT, Zhao S, Shabason JE, Gordon IK, Schlaff CD, Zhang G, Tofilon PJ, Camphausen KA (2013) Ionizing radiation and glioblastoma exosomes: implications in tumor biology and cell migration. Transl Oncol 6:638–648. https://doi.org/10.1593/tlo.13640
Payton C, Pang LY, Gray M, Argyle DJ (2021) Exosomes derived from radioresistant breast cancer cells promote therapeutic resistance in naive recipient cells. J Pers Med. https://doi.org/10.3390/jpm11121310
Milman N, Ginini L, Gil Z (2019) Exosomes and their role in tumorigenesis and anticancer drug resistance. Drug Resist Updat 45:1–12. https://doi.org/10.1016/j.drup.2019.07.003
Shao C, Stewart V, Folkard M, Michael BD, Prise KM (2003) Nitric oxide-mediated signaling in the bystander response of individually targeted glioma cells. Cancer Res 63:8437–8442
Baixauli F, Lopez-Otin C, Mittelbrunn M (2014) Exosomes and autophagy: coordinated mechanisms for the maintenance of cellular fitness. Front Immunol 5:403. https://doi.org/10.3389/fimmu.2014.00403
Takahashi A, Okada R, Nagao K, Kawamata Y, Hanyu A, Yoshimoto S, Takasugi M, Watanabe S, Kanemaki MT, Obuse C et al (2017) Exosomes maintain cellular homeostasis by excreting harmful DNA from cells. Nat Commun 8:15287. https://doi.org/10.1038/ncomms15287
Hood JL, Wickline SA (2012) A systematic approach to exosome-based translational nanomedicine. Wiley Interdiscip Rev Nanomed Nanobiotechnol 4:458–467. https://doi.org/10.1002/wnan.1174
Record M, Carayon K, Poirot M, Silvente-Poirot S (2014) Exosomes as new vesicular lipid transporters involved in cell-cell communication and various pathophysiologies. Biochim Biophys Acta 1841:108–120. https://doi.org/10.1016/j.bbalip.2013.10.004
Gyorgy B, Szabo TG, Pasztoi M, Pal Z, Misjak P, Aradi B, Laszlo V, Pallinger E, Pap E, Kittel A et al (2011) Membrane vesicles, current state-of-the-art: emerging role of extracellular vesicles. Cell Mol Life Sci 68:2667–2688. https://doi.org/10.1007/s00018-011-0689-3
Raposo G, Stoorvogel W (2013) Extracellular vesicles: exosomes, microvesicles, and friends. J Cell Biol 200:373–383. https://doi.org/10.1083/jcb.201211138
Hurley JH, Boura E, Carlson LA, Rozycki B (2010) Membrane budding. Cell 143:875–887. https://doi.org/10.1016/j.cell.2010.11.030
Vlassov AV, Magdaleno S, Setterquist R, Conrad R (2012) Exosomes: current knowledge of their composition, biological functions, and diagnostic and therapeutic potentials. Biochim Biophys Acta 1820:940–948. https://doi.org/10.1016/j.bbagen.2012.03.017
Simons M, Raposo G (2009) Exosomes—vesicular carriers for intercellular communication. Curr Opin Cell Biol 21:575–581. https://doi.org/10.1016/j.ceb.2009.03.007
Thery C, Ostrowski M, Segura E (2009) Membrane vesicles as conveyors of immune responses. Nat Rev Immunol 9:581–593. https://doi.org/10.1038/nri2567
Zoller M (2009) Tetraspanins: push and pull in suppressing and promoting metastasis. Nat Rev Cancer 9:40–55. https://doi.org/10.1038/nrc2543
Mathivanan S, Ji H, Simpson RJ (2010) Exosomes: extracellular organelles important in intercellular communication. J Proteomics 73:1907–1920. https://doi.org/10.1016/j.jprot.2010.06.006
Jelonek K, Widlak P, Pietrowska M (2016) The influence of ionizing radiation on exosome composition, secretion and intercellular communication. Protein Pept Lett 23:656–663
Chargaff E, West R (1946) The biological significance of the thromboplastic protein of blood. J Biol Chem 166:189–197
Muralidharan-Chari V, Clancy JW, Sedgwick A, D’Souza-Schorey C (2010) Microvesicles: mediators of extracellular communication during cancer progression. J Cell Sci 123:1603–1611. https://doi.org/10.1242/jcs.064386
Ratajczak J, Wysoczynski M, Hayek F, Janowska-Wieczorek A, Ratajczak MZ (2006) Membrane-derived microvesicles: important and underappreciated mediators of cell-to-cell communication. Leukemia 20:1487–1495. https://doi.org/10.1038/sj.leu.2404296
Holmgren L, Szeles A, Rajnavolgyi E, Folkman J, Klein G, Ernberg I, Falk KI (1999) Horizontal transfer of DNA by the uptake of apoptotic bodies. Blood 93:3956–3963
Bergsmedh A, Szeles A, Henriksson M, Bratt A, Folkman MJ, Spetz AL, Holmgren L (2001) Horizontal transfer of oncogenes by uptake of apoptotic bodies. Proc Natl Acad Sci U S A 98:6407–6411. https://doi.org/10.1073/pnas.101129998
Karlsson M, Lundin S, Dahlgren U, Kahu H, Pettersson I, Telemo E (2001) “Tolerosomes” are produced by intestinal epithelial cells. Eur J Immunol 31:2892–2900
Teo MT, Landi D, Taylor CF, Elliott F, Vaslin L, Cox DG, Hall J, Landi S, Bishop DT, Kiltie AE (2012) The role of microRNA-binding site polymorphisms in DNA repair genes as risk factors for bladder cancer and breast cancer and their impact on radiotherapy outcomes. Carcinogenesis 33:581–586. https://doi.org/10.1093/carcin/bgr300
Marzesco AM, Janich P, Wilsch-Brauninger M, Dubreuil V, Langenfeld K, Corbeil D, Huttner WB (2005) Release of extracellular membrane particles carrying the stem cell marker prominin‑1 (CD133) from neural progenitors and other epithelial cells. J Cell Sci 118:2849–2858. https://doi.org/10.1242/jcs.02439
Di Daniele A, Antonucci Y, Campello S (2022) Migrasomes, new vescicles as Hansel and Gretel white pebbles? Biol Direct 17:8. https://doi.org/10.1186/s13062-022-00321-1
Ma L, Li Y, Peng J, Wu D, Zhao X, Cui Y, Chen L, Yan X, Du Y, Yu L (2015) Discovery of the migrasome, an organelle mediating release of cytoplasmic contents during cell migration. Cell Res 25:24–38. https://doi.org/10.1038/cr.2014.135
Meehan B, Rak J, Di Vizio D (2016) Oncosomes—large and small: what are they, where they came from? J Extracell Vesicles 5:33109. https://doi.org/10.3402/jev.v5.33109
Jaiswal R, Sedger LM (2019) Intercellular vesicular transfer by exosomes, microparticles and oncosomes—implications for cancer biology and treatments. Front Oncol 9:125. https://doi.org/10.3389/fonc.2019.00125
Al-Nedawi K, Meehan B, Micallef J, Lhotak V, May L, Guha A, Rak J (2008) Intercellular transfer of the oncogenic receptor EGFRvIII by microvesicles derived from tumour cells. Nat Cell Biol 10:619–624. https://doi.org/10.1038/ncb1725
Minciacchi VR, You S, Spinelli C, Morley S, Zandian M, Aspuria PJ, Cavallini L, Ciardiello C, Reis Sobreiro M, Morello M et al (2015) Large oncosomes contain distinct protein cargo and represent a separate functional class of tumor-derived extracellular vesicles. Oncotarget 6:11327–11341. https://doi.org/10.18632/oncotarget.3598
Di Vizio D, Morello M, Dudley AC, Schow PW, Adam RM, Morley S, Mulholland D, Rotinen M, Hager MH, Insabato L et al (2012) Large oncosomes in human prostate cancer tissues and in the circulation of mice with metastatic disease. Am J Pathol 181:1573–1584. https://doi.org/10.1016/j.ajpath.2012.07.030
Bobrie A, Colombo M, Raposo G, Thery C (2011) Exosome secretion: molecular mechanisms and roles in immune responses. Traffic 12:1659–1668. https://doi.org/10.1111/j.1600-0854.2011.01225.x
Witwer KW, Soekmadji C, Hill AF, Wauben MH, Buzas EI, Di Vizio D, Falcon-Perez JM, Gardiner C, Hochberg F, Kurochkin IV et al (2017) Updating the MISEV minimal requirements for extracellular vesicle studies: building bridges to reproducibility. J Extracell Vesicles 6:1396823. https://doi.org/10.1080/20013078.2017.1396823
Witwer KW, Goberdhan DC, O’Driscoll L, Thery C, Welsh JA, Blenkiron C, Buzas EI, Di Vizio D, Erdbrugger U, Falcon-Perez JM et al (2021) Updating MISEV: evolving the minimal requirements for studies of extracellular vesicles. J of Extracellular Vesicle 10:e12182. https://doi.org/10.1002/jev2.12182
Kwok ZH, Wang C, Jin Y (2021) Extracellular vesicle transportation and uptake by recipient cells: a critical process to regulate human diseases. Processes. https://doi.org/10.3390/pr9020273
Soekmadji C, Hill AF, Wauben MH, Buzas EI, Di Vizio D, Gardiner C, Lotvall J, Sahoo S, Witwer KW (2018) Towards mechanisms and standardization in extracellular vesicle and extracellular RNA studies: results of a worldwide survey. J of Extracellular Vesicle 7:1535745. https://doi.org/10.1080/20013078.2018.1535745
Hessvik NP, Llorente A (2018) Current knowledge on exosome biogenesis and release. Cell Mol Life Sci 75:193–208. https://doi.org/10.1007/s00018-017-2595-9
Beer L, Zimmermann M, Mitterbauer A, Ellinger A, Gruber F, Narzt MS, Zellner M, Gyongyosi M, Madlener S, Simader E et al (2015) Analysis of the secretome of apoptotic peripheral blood mononuclear cells: impact of released proteins and exosomes for tissue regeneration. Sci Rep 5:16662. https://doi.org/10.1038/srep16662
Lehmann BD, Paine MS, Brooks AM, McCubrey JA, Renegar RH, Wang R, Terrian DM (2008) Senescence-associated exosome release from human prostate cancer cells. Cancer Res 68:7864–7871. https://doi.org/10.1158/0008-5472.CAN-07-6538
Bhatta B, Luz I, Krueger C, Teo FX, Lane DP, Sabapathy K, Cooks T (2021) Cancer cells shuttle extracellular vesicles containing oncogenic mutant p53 proteins to the tumor microenvironment. Cancers. https://doi.org/10.3390/cancers13122985
Taylor DD, Gercel-Taylor C (2005) Tumour-derived exosomes and their role in cancer-associated T‑cell signalling defects. Br J Cancer 92:305–311. https://doi.org/10.1038/sj.bjc.6602316
Kalluri R (2016) The biology and function of exosomes in cancer. J Clin Invest 126:1208–1215. https://doi.org/10.1172/JCI81135
Moller A, Lobb RJ (2020) The evolving translational potential of small extracellular vesicles in cancer. Nat Rev Cancer 20:697–709. https://doi.org/10.1038/s41568-020-00299-w
Ortiz A (2021) Extracellular vesicles in cancer progression. Semin Cancer Biol 76:139–142. https://doi.org/10.1016/j.semcancer.2021.05.032
Peinado H, Lavotshkin S, Lyden D (2011) The secreted factors responsible for pre-metastatic niche formation: old sayings and new thoughts. Semin Cancer Biol 21:139–146. https://doi.org/10.1016/j.semcancer.2011.01.002
Fong MY, Zhou W, Liu L, Alontaga AY, Chandra M, Ashby J, Chow A, O’Connor ST, Li S, Chin AR et al (2015) Breast-cancer-secreted miR-122 reprograms glucose metabolism in premetastatic niche to promote metastasis. Nat Cell Biol 17:183–194. https://doi.org/10.1038/ncb3094
Peinado H, Aleckovic M, Lavotshkin S, Matei I, Costa-Silva B, Moreno-Bueno G, Hergueta-Redondo M, Williams C, Garcia-Santos G, Ghajar C et al (2012) Melanoma exosomes educate bone marrow progenitor cells toward a pro-metastatic phenotype through MET. Nat Med 18:883–891. https://doi.org/10.1038/nm.2753
Li J, Yuan H, Xu H, Zhao H, Xiong N (2020) Hypoxic cancer-secreted exosomal miR-182-5p promotes glioblastoma angiogenesis by targeting Kruppel-like factor 2 and 4. Mol Cancer Res 18:1218–1231. https://doi.org/10.1158/1541-7786.MCR-19-0725
King HW, Michael MZ, Gleadle JM (2012) Hypoxic enhancement of exosome release by breast cancer cells. BMC Cancer 12:421. https://doi.org/10.1186/1471-2407-12-421
Matsuura Y, Wada H, Eguchi H, Gotoh K, Kobayashi S, Kinoshita M, Kubo M, Hayashi K, Iwagami Y, Yamada D et al (2019) Exosomal miR-155 derived from hepatocellular carcinoma cells under hypoxia promotes angiogenesis in endothelial cells. Dig Dis Sci 64:792–802. https://doi.org/10.1007/s10620-018-5380-1
Patton MC, Zubair H, Khan MA, Singh S, Singh AP (2020) Hypoxia alters the release and size distribution of extracellular vesicles in pancreatic cancer cells to support their adaptive survival. J Cell Biochem 121:828–839. https://doi.org/10.1002/jcb.29328
Xia X, Wang S, Ni B, Xing S, Cao H, Zhang Z, Yu F, Zhao E, Zhao G (2020) Hypoxic gastric cancer-derived exosomes promote progression and metastasis via MiR-301a-3p/PHD3/HIF-1alpha positive feedback loop. Oncogene 39:6231–6244. https://doi.org/10.1038/s41388-020-01425-6
Ren R, Sun H, Ma C, Liu J, Wang H (2019) Colon cancer cells secrete exosomes to promote self-proliferation by shortening mitosis duration and activation of STAT3 in a hypoxic environment. Cell Biosci 9:62. https://doi.org/10.1186/s13578-019-0325-8
Ramteke A, Ting H, Agarwal C, Mateen S, Somasagara R, Hussain A, Graner M, Frederick B, Agarwal R, Deep G (2015) Exosomes secreted under hypoxia enhance invasiveness and stemness of prostate cancer cells by targeting adherens junction molecules. Mol Carcinog 54:554–565. https://doi.org/10.1002/mc.22124
Thakur A, Qiu G, Xu C, Han X, Yang T, Ng SP, Chan KWY, Wu CML, Lee Y (2020) Label-free sensing of exosomal MCT1 and CD147 for tracking metabolic reprogramming and malignant progression in glioma. Sci Adv 6:eaaz6119. https://doi.org/10.1126/sciadv.aaz6119
He G, Peng X, Wei S, Yang S, Li X, Huang M, Tang S, Jin H, Liu J, Zhang S et al (2022) Exosomes in the hypoxic TME: from release, uptake and biofunctions to clinical applications. Mol Cancer 21:19. https://doi.org/10.1186/s12943-021-01440-5
Jung KO, Jo H, Yu JH, Gambhir SS, Pratx G (2018) Development and MPI tracking of novel hypoxia-targeted theranostic exosomes. Biomaterials 177:139–148. https://doi.org/10.1016/j.biomaterials.2018.05.048
Parolini I, Federici C, Raggi C, Lugini L, Palleschi S, De Milito A, Coscia C, Iessi E, Logozzi M, Molinari A et al (2009) Microenvironmental pH is a key factor for exosome traffic in tumor cells. J Biol Chem 284:34211–34222. https://doi.org/10.1074/jbc.M109.041152
Luciani F, Spada M, De Milito A, Molinari A, Rivoltini L, Montinaro A, Marra M, Lugini L, Logozzi M, Lozupone F et al (2004) Effect of proton pump inhibitor pretreatment on resistance of solid tumors to cytotoxic drugs. J Natl Cancer Inst 96:1702–1713. https://doi.org/10.1093/jnci/djh305
Fuentes P, Sese M, Guijarro PJ, Emperador M, Sanchez-Redondo S, Peinado H, Hummer S, Ramon YCS (2020) ITGB3-mediated uptake of small extracellular vesicles facilitates intercellular communication in breast cancer cells. Nat Commun 11:4261. https://doi.org/10.1038/s41467-020-18081-9
Kelemen A, Carmi I, Oszvald A, Lorincz P, Petovari G, Tolgyes T, Dede K, Bursics A, Buzas EI, Wiener Z (2021) IFITM1 expression determines extracellular vesicle uptake in colorectal cancer. Cell Mol Life Sci 78:7009–7024. https://doi.org/10.1007/s00018-021-03949-w
Toda Y, Takata K, Nakagawa Y, Kawakami H, Fujioka S, Kobayashi K, Hattori Y, Kitamura Y, Akaji K, Ashihara E (2015) Effective internalization of U251-MG-secreted exosomes into cancer cells and characterization of their lipid components. Biochem Biophys Res Commun 456:768–773. https://doi.org/10.1016/j.bbrc.2014.12.015
Hazan-Halevy I, Rosenblum D, Weinstein S, Bairey O, Raanani P, Peer D (2015) Cell-specific uptake of mantle cell lymphoma-derived exosomes by malignant and non-malignant B‑lymphocytes. Cancer Lett 364:59–69. https://doi.org/10.1016/j.canlet.2015.04.026
Linxweiler J, Kolbinger A, Himbert D, Zeuschner P, Saar M, Stockle M, Junker K (2021) Organ-specific uptake of extracellular vesicles secreted by urological cancer cells. Cancers. https://doi.org/10.3390/cancers13194937
Escrevente C, Keller S, Altevogt P, Costa J (2011) Interaction and uptake of exosomes by ovarian cancer cells. BMC Cancer 11:108. https://doi.org/10.1186/1471-2407-11-108
Xi XM, Xia SJ, Lu R (2021) Drug loading techniques for exosome-based drug delivery systems. Pharmazie 76:61–67. https://doi.org/10.1691/ph.2021.0128
Saari H, Lazaro-Ibanez E, Viitala T, Vuorimaa-Laukkanen E, Siljander P, Yliperttula M (2015) Microvesicle- and exosome-mediated drug delivery enhances the cytotoxicity of paclitaxel in autologous prostate cancer cells. J Control Release 220:727–737. https://doi.org/10.1016/j.jconrel.2015.09.031
Kim MS, Haney MJ, Zhao Y, Yuan D, Deygen I, Klyachko NL, Kabanov AV, Batrakova EV (2018) Engineering macrophage-derived exosomes for targeted paclitaxel delivery to pulmonary metastases: in vitro and in vivo evaluations. Nanomedicine 14:195–204. https://doi.org/10.1016/j.nano.2017.09.011
Al Faruque H, Choi ES, Kim JH, Kim E (2022) Enhanced effect of autologous EVs delivering paclitaxel in pancreatic cancer. J Control Release 347:330–346. https://doi.org/10.1016/j.jconrel.2022.05.012
Tian Y, Li S, Song J, Ji T, Zhu M, Anderson GJ, Wei J, Nie G (2014) A doxorubicin delivery platform using engineered natural membrane vesicle exosomes for targeted tumor therapy. Biomaterials 35:2383–2390. https://doi.org/10.1016/j.biomaterials.2013.11.083
Gehrmann U, Naslund TI, Hiltbrunner S, Larssen P, Gabrielsson S (2014) Harnessing the exosome-induced immune response for cancer immunotherapy. Semin Cancer Biol 28:58–67. https://doi.org/10.1016/j.semcancer.2014.05.003
Shi X, Cheng Q, Hou T, Han M, Smbatyan G, Lang JE, Epstein AL, Lenz HJ, Zhang Y (2020) Genetically engineered cell-derived nanoparticles for targeted breast cancer immunotherapy. Mol Ther 28:536–547. https://doi.org/10.1016/j.ymthe.2019.11.020
Ruiss R, Jochum S, Mocikat R, Hammerschmidt W, Zeidler R (2011) EBV-gp350 confers B‑cell tropism to tailored exosomes and is a neo-antigen in normal and malignant B cells—a new option for the treatment of B‑CLL. PLoS One 6:e25294. https://doi.org/10.1371/journal.pone.0025294
Dellar ER, Hill C, Melling GE, Carter DRF, Baena-Lopez L (2022) Unpacking extracellular vesicles: RNA cargo loading and function. J Extracell Biol. https://doi.org/10.1002/jex2.40
Thakur BK, Zhang H, Becker A, Matei I, Huang Y, Costa-Silva B, Zheng Y, Hoshino A, Brazier H, Xiang J et al (2014) Double-stranded DNA in exosomes: a novel biomarker in cancer detection. Cell Res 24:766–769. https://doi.org/10.1038/cr.2014.44
Abramowicz A, Widlak P, Pietrowska M (2019) Different types of cellular stress affect the proteome composition of small extracellular vesicles: a mini review. Proteomes. https://doi.org/10.3390/proteomes7020023
Pizzinat N, Ong-Meang V, Bourgailh-Tortosa F, Blanzat M, Perquis L, Cussac D, Parini A, Poinsot V (2020) Extracellular vesicles of MSCs and cardiomyoblasts are vehicles for lipid mediators. Biochimie 178:69–80. https://doi.org/10.1016/j.biochi.2020.07.013
He C, Li L, Wang L, Meng W, Hao Y, Zhu G (2021) Exosome-mediated cellular crosstalk within the tumor microenvironment upon irradiation. Cancer Biol Med 18:21–33. https://doi.org/10.20892/j.issn.2095-3941.2020.0150
Mittelbrunn M, Gutierrez-Vazquez C, Villarroya-Beltri C, Gonzalez S, Sanchez-Cabo F, Gonzalez MA, Bernad A, Sanchez-Madrid F (2011) Unidirectional transfer of microRNA-loaded exosomes from T cells to antigen-presenting cells. Nat Commun 2:282. https://doi.org/10.1038/ncomms1285
Valadi H, Ekstrom K, Bossios A, Sjostrand M, Lee JJ, Lotvall JO (2007) Exosome-mediated transfer of mRNAs and microRNAs is a novel mechanism of genetic exchange between cells. Nat Cell Biol 9:654–659. https://doi.org/10.1038/ncb1596
Teng Y, Ren Y, Hu X, Mu J, Samykutty A, Zhuang X, Deng Z, Kumar A, Zhang L, Merchant ML et al (2017) MVP-mediated exosomal sorting of miR-193a promotes colon cancer progression. Nat Commun 8:14448. https://doi.org/10.1038/ncomms14448
Santangelo L, Giurato G, Cicchini C, Montaldo C, Mancone C, Tarallo R, Battistelli C, Alonzi T, Weisz A, Tripodi M (2016) The RNA-binding protein SYNCRIP is a component of the hepatocyte exosomal machinery controlling microRNA sorting. Cell Rep 17:799–808. https://doi.org/10.1016/j.celrep.2016.09.031
Villarroya-Beltri C, Gutiérrez-Vázquez C, Sánchez-Cabo F, Pérez-Hernández D, Vázquez J, Martin-Cofreces N, Martinez-Herrera DJ, Pascual-Montano A, Mittelbrunn M, Sánchez-Madrid F (2013) Sumoylated hnRNPA2B1 controls the sorting of miRNAs into exosomes through binding to specific motifs. Nat Commun 4:2980. https://doi.org/10.1038/ncomms3980
McKenzie AJ, Hoshino D, Hong NH, Cha DJ, Franklin JL, Coffey RJ, Patton JG, Weaver AM (2016) KRAS-MEK signaling controls Ago2 sorting into exosomes. Cell Rep 15:978–987. https://doi.org/10.1016/j.celrep.2016.03.085
Lu P, Li H, Li N, Singh RN, Bishop CE, Chen X, Lu B (2017) MEX3C interacts with adaptor-related protein complex 2 and involves in miR-451a exosomal sorting. PLoS ONE 12:e185992. https://doi.org/10.1371/journal.pone.0185992
Lin F, Zeng Z, Song Y, Li L, Wu Z, Zhang X, Li Z, Ke X, Hu X (2019) YBX‑1 mediated sorting of miR-133 into hypoxia/reoxygenation-induced EPC-derived exosomes to increase fibroblast angiogenesis and MEndoT. Stem Cell Res Ther 10:263. https://doi.org/10.1186/s13287-019-1377-8
Martins-Marques T, Costa MC, Catarino S, Simoes I, Aasen T, Enguita FJ, Girao H (2022) Cx43-mediated sorting of miRNAs into extracellular vesicles. EMBO Rep 23:e54312. https://doi.org/10.15252/embr.202154312
Lee H, Li C, Zhang Y, Zhang D, Otterbein LE, Jin Y (2019) Caveolin‑1 selectively regulates microRNA sorting into microvesicles after noxious stimuli. J Exp Med 216:2202–2220. https://doi.org/10.1084/jem.20182313
Si Y, Liu F, Wang D, Fang C, Tang X, Guo B, Shi Z, Dong Z, Guo D, Yue J et al (2021) Exosomal transfer of miR-185 is controlled by hnRNPA2B1 and impairs re-endothelialization after vascular injury. Front Cell Dev Biol 9:619444. https://doi.org/10.3389/fcell.2021.619444
Li C, Qin F, Wang W, Ni Y, Gao M, Guo M, Sun G (2021) hnRNPA2B1-mediated extracellular vesicles sorting of miR-122-5p potentially promotes lung cancer progression. Int J Mol Sci. https://doi.org/10.3390/ijms222312866
Kosaka N, Iguchi H, Hagiwara K, Yoshioka Y, Takeshita F, Ochiya T (2013) Neutral sphingomyelinase 2 (nSMase2)-dependent exosomal transfer of angiogenic microRNAs regulate cancer cell metastasis. J Biol Chem 288:10849–10859. https://doi.org/10.1074/jbc.M112.446831
Squadrito ML, Baer C, Burdet F, Maderna C, Gilfillan GD, Lyle R, Ibberson M, De Palma M (2014) Endogenous RNAs modulate microRNA sorting to exosomes and transfer to acceptor cells. Cell Rep 8:1432–1446. https://doi.org/10.1016/j.celrep.2014.07.035
Montecalvo A, Larregina AT, Shufesky WJ, Stolz DB, Sullivan ML, Karlsson JM, Baty CJ, Gibson GA, Erdos G, Wang Z et al (2012) Mechanism of transfer of functional microRNAs between mouse dendritic cells via exosomes. Blood 119:756–766. https://doi.org/10.1182/blood-2011-02-338004
Yentrapalli R, Merl-Pham J, Azimzadeh O, Mutschelknaus L, Peters C, Hauck SM, Atkinson MJ, Tapio S, Moertl S (2017) Quantitative changes in the protein and miRNA cargo of plasma exosome-like vesicles after exposure to ionizing radiation. Int J Radiat Biol 93:569–580. https://doi.org/10.1080/09553002.2017.1294772
Abramowicz A, Wojakowska A, Marczak L, Lysek-Gladysinska M, Smolarz M, Story MD, Polanska J, Widlak P, Pietrowska M (2019) Ionizing radiation affects the composition of the proteome of extracellular vesicles released by head-and-neck cancer cells in vitro. J Radiat Res 60:289–297. https://doi.org/10.1093/jrr/rrz001
Malla B, Aebersold DM, Dal Pra A (2018) Protocol for serum exosomal miRNAs analysis in prostate cancer patients treated with radiotherapy. J Transl Med 16:223. https://doi.org/10.1186/s12967-018-1592-6
An M, Lohse I, Tan Z, Zhu J, Wu J, Kurapati H, Morgan MA, Lawrence TS, Cuneo KC, Lubman DM (2017) Quantitative proteomic analysis of serum exosomes from patients with locally advanced pancreatic cancer undergoing chemoradiotherapy. J Proteome Res 16:1763–1772. https://doi.org/10.1021/acs.jproteome.7b00024
Yu Q, Li P, Weng M, Wu S, Zhang Y, Chen X, Zhang Q, Shen G, Ding X, Fu S (2018) Nano-vesicles are a potential tool to monitor therapeutic efficacy of carbon Ion radiotherapy in prostate cancer. J Biomed Nanotechnol 14:168–178. https://doi.org/10.1166/jbn.2018.2503
Kulkarni S, Koller A, Mani KM, Wen R, Alfieri A, Saha S, Wang J, Patel P, Bandeira N, Guha C et al (2016) Identifying urinary and serum exosome biomarkers for radiation exposure using a data dependent acquisition and SWATH-MS combined workflow. Int J Radiat Oncol Biol Phys 96:566–577. https://doi.org/10.1016/j.ijrobp.2016.06.008
Trajkovic K, Hsu C, Chiantia S, Rajendran L, Wenzel D, Wieland F, Schwille P, Brugger B, Simons M (2008) Ceramide triggers budding of exosome vesicles into multivesicular endosomes. Science 319:1244–1247. https://doi.org/10.1126/science.1153124
Kahlert C, Melo SA, Protopopov A, Tang J, Seth S, Koch M, Zhang J, Weitz J, Chin L, Futreal A et al (2014) Identification of double-stranded genomic DNA spanning all chromosomes with mutated KRAS and p53 DNA in the serum exosomes of patients with pancreatic cancer. J Biol Chem 289:3869–3875. https://doi.org/10.1074/jbc.C113.532267
Waldenström A, Gennebäck N, Hellman U, Ronquist G (2012) Cardiomyocyte microvesicles contain DNA/RNA and convey biological messages to target cells. PLoS One 7:e34653. https://doi.org/10.1371/journal.pone.0034653
Guescini M, Genedani S, Stocchi V, Agnati LF (2010) Astrocytes and glioblastoma cells release exosomes carrying mtDNA. J Neural Transm 117:1–4. https://doi.org/10.1007/s00702-009-0288-8
Balaj L, Lessard R, Dai L, Cho YJ, Pomeroy SL, Breakefield XO, Skog J (2011) Tumour microvesicles contain retrotransposon elements and amplified oncogene sequences. Nat Commun 2:180. https://doi.org/10.1038/ncomms1180
Cambier L, Stachelek K, Triska M, Jubran R, Huang M, Li W, Zhang J, Li J, Cobrinik D (2021) Extracellular vesicle-associated repetitive element DNAs as candidate osteosarcoma biomarkers. Sci Rep 11:94. https://doi.org/10.1038/s41598-020-77398-z
Vagner T, Spinelli C, Minciacchi VR, Balaj L, Zandian M, Conley A, Zijlstra A, Freeman MR, Demichelis F, De S et al (2018) Large extracellular vesicles carry most of the tumour DNA circulating in prostate cancer patient plasma. J Extracell Vesicles 7:1505403. https://doi.org/10.1080/20013078.2018.1505403
Yokoi A, Villar-Prados A, Oliphint PA, Zhang J, Song X, De Hoff P, Morey R, Liu J, Roszik J, Clise-Dwyer K et al (2019) Mechanisms of nuclear content loading to exosomes. Sci Adv 5:eaax8849. https://doi.org/10.1126/sciadv.aax8849
Torralba D, Baixauli F, Villarroya-Beltri C, Fernández-Delgado I, Latorre-Pellicer A, Acín-Pérez R, Martín-Cófreces NB, Jaso-Tamame Á et al (2018) Priming of dendritic cells by DNA-containing extracellular vesicles from activated T cells through antigen-driven contacts. Nat Commun 9:2658. https://doi.org/10.1038/s41467-018-05077-9
Miranda KC, Bond DT, McKee M, Skog J, Păunescu TG, Da Silva N, Brown D, Russo LM (2010) Nucleic acids within urinary exosomes/microvesicles are potential biomarkers for renal disease. Kidney Int 78:191–199. https://doi.org/10.1038/ki.2010.106
Fischer S, Cornils K, Speiseder T, Badbaran A, Reimer R, Indenbirken D, Grundhoff A, Brunswig-Spickenheier B, Alawi M, Lange C (2016) Indication of horizontal DNA gene transfer by extracellular vesicles. PLoS ONE 11:e163665. https://doi.org/10.1371/journal.pone.0163665
Németh A, Orgovan N, Sódar BW, Osteikoetxea X, Pálóczi K, Szabó-Taylor K, Vukman KV, Kittel Á, Turiák L, Wiener Z et al (2017) Antibiotic-induced release of small extracellular vesicles (exosomes) with surface-associated DNA. Sci Rep 7:8202. https://doi.org/10.1038/s41598-017-08392-1
Sisirak V, Sally B, D’Agati V, Martinez-Ortiz W, Özçakar ZB, David J, Rashidfarrokhi A, Yeste A, Panea C, Chida AS et al (2016) Digestion of chromatin in apoptotic cell microparticles prevents autoimmunity. Cell 166:88–101. https://doi.org/10.1016/j.cell.2016.05.034
Sedej I, Štalekar M, Tušek Žnidarič M, Goričar K, Kojc N, Kogovšek P, Dolžan V, Arnol M, Lenassi M (2022) Extracellular vesicle-bound DNA in urine is indicative of kidney allograft injury. J Extracell Vesicles 11:e12268. https://doi.org/10.1002/jev2.12268
Tutanov O, Shtam T, Grigor’eva A, Tupikin A, Tsentalovich Y, Tamkovich S (2022) Blood plasma exosomes contain circulating DNA in their crown. Diagnostics. https://doi.org/10.3390/diagnostics12040854
Jeon H, Lee J, Lee S, Kang SK, Park SJ, Yoo SM, Lee MS (2019) Extracellular vesicles from KSHV-infected cells stimulate antiviral immune response through mitochondrial DNA. Front Immunol 10:876. https://doi.org/10.3389/fimmu.2019.00876
Branzk N, Lubojemska A, Hardison SE, Wang Q, Gutierrez MG, Brown GD, Papayannopoulos V (2014) Neutrophils sense microbe size and selectively release neutrophil extracellular traps in response to large pathogens. Nat Immunol 15:1017–1025. https://doi.org/10.1038/ni.2987
Yousefi S, Gold JA, Andina N, Lee JJ, Kelly AM, Kozlowski E, Schmid I, Straumann A, Reichenbach J, Gleich GJ et al (2008) Catapult-like release of mitochondrial DNA by eosinophils contributes to antibacterial defense. Nat Med 14:949–953. https://doi.org/10.1038/nm.1855
Wang Z, Hill S, Luther JM, Hachey DL, Schey KL (2012) Proteomic analysis of urine exosomes by multidimensional protein identification technology (MudPIT). Proteomics 12:329–338. https://doi.org/10.1002/pmic.201100477
Silvers CR, Miyamoto H, Messing EM, Netto GJ, Lee YF (2017) Characterization of urinary extracellular vesicle proteins in muscle-invasive bladder cancer. Oncotarget 8:91199–91208. https://doi.org/10.18632/oncotarget.20043
Lázaro-Ibáñez E, Lässer C, Shelke GV, Crescitelli R, Jang SC, Cvjetkovic A, García-Rodríguez A, Lötvall J (2019) DNA analysis of low- and high-density fractions defines heterogeneous subpopulations of small extracellular vesicles based on their DNA cargo and topology. J Extracell Vesicles 8:1656993. https://doi.org/10.1080/20013078.2019.1656993
Liu H, Tian Y, Xue C, Niu Q, Chen C, Yan X (2022) Analysis of extracellular vesicle DNA at the single-vesicle level by nano-flow cytometry. J Extracell Vesicles 11:e12206. https://doi.org/10.1002/jev2.12206
Erdal E, Haider S, Rehwinkel J, Harris AL, McHugh PJ (2017) A prosurvival DNA damage-induced cytoplasmic interferon response is mediated by end resection factors and is limited by Trex1. Genes Dev 31:353–369. https://doi.org/10.1101/gad.289769.116
Luzhna L, Kathiria P, Kovalchuk O (2013) Micronuclei in genotoxicity assessment: from genetics to epigenetics and beyond. Front Genet 4:131. https://doi.org/10.3389/fgene.2013.00131
Mahaney BL, Meek K, Lees-Miller SP (2009) Repair of ionizing radiation-induced DNA double-strand breaks by non-homologous end-joining. Biochem J 417:639–650. https://doi.org/10.1042/bj20080413
Harding SM, Benci JL, Irianto J, Discher DE, Minn AJ, Greenberg RA (2017) Mitotic progression following DNA damage enables pattern recognition within micronuclei. Nature 548:466–470. https://doi.org/10.1038/nature23470
Jonathan EC, Bernhard EJ, McKenna WG (1999) How does radiation kill cells? Curr Opin Chem Biol 3:77–83. https://doi.org/10.1016/s1367-5931(99)80014-3
Kobayashi D, Oike T, Murata K, Irie D, Hirota Y, Sato H, Shibata A, Ohno T (2020) Induction of micronuclei in cervical cancer treated with radiotherapy. J Pers Med. https://doi.org/10.3390/jpm10030110
Hintzsche H, Polat B, Schewe V, Djuzenova CS, Pfreundner L, Flentje M, Stopper H (2012) Micronucleus formation kinetics in buccal mucosa cells of head and neck cancer patients undergoing radiotherapy. Toxicol Lett 212:33–37. https://doi.org/10.1016/j.toxlet.2012.04.020
Driessens G, Harsan L, Robaye B, Waroquier D, Browaeys P, Giannakopoulos X, Velu T, Bruyns C (2003) Micronuclei to detect in vivo chemotherapy damage in a p53 mutated solid tumour. Br J Cancer 89:727–729. https://doi.org/10.1038/sj.bjc.6601163
Hatch EM, Fischer AH, Deerinck TJ, Hetzer MW (2013) Catastrophic nuclear envelope collapse in cancer cell micronuclei. Cell 154:47–60. https://doi.org/10.1016/j.cell.2013.06.007
Dou Z, Xu C, Donahue G, Shimi T, Pan JA, Zhu J, Ivanov A, Capell BC, Drake AM, Shah PP et al (2015) Autophagy mediates degradation of nuclear lamina. Nature 527:105–109. https://doi.org/10.1038/nature15548
Ivanov A, Pawlikowski J, Manoharan I, van Tuyn J, Nelson DM, Rai TS, Shah PP, Hewitt G, Korolchuk VI, Passos JF et al (2013) Lysosome-mediated processing of chromatin in senescence. J Cell Biol 202:129–143. https://doi.org/10.1083/jcb.201212110
Vizioli MG, Liu T, Miller KN, Robertson NA, Gilroy K, Lagnado AB, Perez-Garcia A, Kiourtis C, Dasgupta N, Lei X et al (2020) Mitochondria-to-nucleus retrograde signaling drives formation of cytoplasmic chromatin and inflammation in senescence. Genes Dev 34:428–445. https://doi.org/10.1101/gad.331272.119
Glück S, Guey B, Gulen MF, Wolter K, Kang TW, Schmacke NA, Bridgeman A, Rehwinkel J, Zender L, Ablasser A (2017) Innate immune sensing of cytosolic chromatin fragments through cGAS promotes senescence. Nat Cell Biol 19:1061–1070. https://doi.org/10.1038/ncb3586
Borghesan M, Fafian-Labora J, Eleftheriadou O, Carpintero-Fernandez P, Paez-Ribes M, Vizcay-Barrena G, Swisa A, Kolodkin-Gal D, Ximenez-Embun P, Lowe R et al (2019) Small extracellular vesicles are key regulators of non-cell autonomous intercellular communication in senescence via the interferon protein IFITM3. Cell Rep 27:3956–3971.e6. https://doi.org/10.1016/j.celrep.2019.05.095
Abdul-Aziz AM, Sun Y, Hellmich C, Marlein CR, Mistry J, Forde E, Piddock RE, Shafat MS, Morfakis A, Mehta T et al (2019) Acute myeloid leukemia induces protumoral p16INK4a-driven senescence in the bone marrow microenvironment. Blood 133:446–456. https://doi.org/10.1182/blood-2018-04-845420
Jeon HY, Kim JK, Ham SW, Oh SY, Kim J, Park JB, Lee JY, Kim SC, Kim H (2016) Irradiation induces glioblastoma cell senescence and senescence-associated secretory phenotype. Tumour Biol 37:5857–5867. https://doi.org/10.1007/s13277-015-4439-2
Joyner DE, Bastar JD, Randall RL (2006) Doxorubicin induces cell senescence preferentially over apoptosis in the FU-SY‑1 synovial sarcoma cell line. J Orthop Res 24:1163–1169. https://doi.org/10.1002/jor.20169
Hitomi K, Okada R, Loo TM, Miyata K, Nakamura AJ, Takahashi A (2020) DNA damage regulates senescence-associated extracellular vesicle release via the ceramide pathway to prevent excessive inflammatory responses. Int J Mol Sci. https://doi.org/10.3390/ijms21103720
Soleimani R, Heytens E, Darzynkiewicz Z, Oktay K (2011) Mechanisms of chemotherapy-induced human ovarian aging: double strand DNA breaks and microvascular compromise. Aging 3:782–793. https://doi.org/10.18632/aging.100363
Riley JS, Quarato G, Cloix C, Lopez J, O’Prey J, Pearson M, Chapman J, Sesaki H, Carlin LM, Passos JF et al (2018) Mitochondrial inner membrane permeabilisation enables mtDNA release during apoptosis. EMBO J. https://doi.org/10.15252/embj.201899238
McArthur K, Whitehead LW, Heddleston JM, Li L, Padman BS, Oorschot V, Geoghegan ND, Chappaz S, Davidson S, San Chin H et al (2018) BAK/BAX macropores facilitate mitochondrial herniation and mtDNA efflux during apoptosis. Science. https://doi.org/10.1126/science.aao6047
Ichim G, Lopez J, Ahmed SU, Muthalagu N, Giampazolias E, Delgado ME, Haller M, Riley JS, Mason SM, Athineos D et al (2015) Limited mitochondrial permeabilization causes DNA damage and genomic instability in the absence of cell death. Mol Cell 57:860–872. https://doi.org/10.1016/j.molcel.2015.01.018
Kim J, Gupta R, Blanco LP, Yang S, Shteinfer-Kuzmine A, Wang K, Zhu J, Yoon HE, Wang X, Kerkhofs M et al (2019) VDAC oligomers form mitochondrial pores to release mtDNA fragments and promote lupus-like disease. Science 366:1531–1536. https://doi.org/10.1126/science.aav4011
García N, García JJ, Correa F, Chávez E (2005) The permeability transition pore as a pathway for the release of mitochondrial DNA. Proc Natl Sci Counc Repub China B 76:2873–2880. https://doi.org/10.1016/j.lfs.2004.12.012
Kam WW, Banati RB (2013) Effects of ionizing radiation on mitochondria. Free Radic Biol Med 65:607–619. https://doi.org/10.1016/j.freeradbiomed.2013.07.024
Averbeck D, Rodriguez-Lafrasse C (2021) Role of mitochondria in radiation responses: epigenetic, metabolic, and signaling impacts. Int J Mol Sci. https://doi.org/10.3390/ijms222011047
Pérez-Treviño P, Velásquez M, García N (2020) Mechanisms of mitochondrial DNA escape and its relationship with different metabolic diseases. Biochim Biophys Acta Mol Basis Dis 1866:165761. https://doi.org/10.1016/j.bbadis.2020.165761
Jeppesen DK, Fenix AM, Franklin JL, Higginbotham JN, Zhang Q, Zimmerman LJ, Liebler DC, Ping J, Liu Q, Evans R et al (2019) Reassessment of exosome composition. Cell 177:428–445.e18. https://doi.org/10.1016/j.cell.2019.02.029
Castellanos-Rizaldos E, Zhang X, Tadigotla VR, Grimm DG, Karlovich C, Raez LE, Skog JK (2019) Exosome-based detection of activating and resistance EGFR mutations from plasma of non-small cell lung cancer patients. Oncotarget 10:2911–2920. https://doi.org/10.18632/oncotarget.26885
Yang S, Che SP, Kurywchak P, Tavormina JL, Gansmo LB, Correa de Sampaio P, Tachezy M, Bockhorn M, Gebauer F, Haltom AR et al (2017) Detection of mutant KRAS and TP53 DNA in circulating exosomes from healthy individuals and patients with pancreatic cancer. Cancer Biol Ther 18:158–165. https://doi.org/10.1080/15384047.2017.1281499
Bernard V, Kim DU, San Lucas FA, Castillo J, Allenson K, Mulu FC, Stephens BM, Huang J, Semaan A, Guerrero PA et al (2019) Circulating nucleic acids are associated with outcomes of patients with pancreatic cancer. Gastroenterology 156:108–118.e4. https://doi.org/10.1053/j.gastro.2018.09.022
Allenson K, Castillo J, San Lucas FA, Scelo G, Kim DU, Bernard V, Davis G, Kumar T, Katz M, Overman MJ et al (2017) High prevalence of mutant KRAS in circulating exosome-derived DNA from early-stage pancreatic cancer patients. Ann Oncol 28:741–747. https://doi.org/10.1093/annonc/mdx004
Elzanowska J, Semira C, Costa-Silva B (2021) DNA in extracellular vesicles: biological and clinical aspects. Mol Oncol 15:1701–1714. https://doi.org/10.1002/1878-0261.12777
McKelvey KJ, Powell KL, Ashton AW, Morris JM, McCracken SA (2015) Exosomes: mechanisms of uptake. J Circ Biomark 4:7. https://doi.org/10.5772/61186
Zech D, Rana S, Buchler MW, Zoller M (2012) Tumor-exosomes and leukocyte activation: an ambivalent crosstalk. Cell Commun Signal 10:37. https://doi.org/10.1186/1478-811X-10-37
Horibe S, Tanahashi T, Kawauchi S, Murakami Y, Rikitake Y (2018) Mechanism of recipient cell-dependent differences in exosome uptake. BMC Cancer 18:47. https://doi.org/10.1186/s12885-017-3958-1
Rana S, Yue S, Stadel D, Zoller M (2012) Toward tailored exosomes: the exosomal tetraspanin web contributes to target cell selection. Int J Biochem Cell Biol 44:1574–1584. https://doi.org/10.1016/j.biocel.2012.06.018
Hemler ME (2003) Tetraspanin proteins mediate cellular penetration, invasion, and fusion events and define a novel type of membrane microdomain. Annu Rev Cell Dev Biol 19:397–422. https://doi.org/10.1146/annurev.cellbio.19.111301.153609
Hoshino A, Costa-Silva B, Shen TL, Rodrigues G, Hashimoto A, Tesic Mark M, Molina H, Kohsaka S, Di Giannatale A, Ceder S et al (2015) Tumour exosome integrins determine organotropic metastasis. Nature 527:329–335. https://doi.org/10.1038/nature15756
Rogasevskaia T, Coorssen JR (2006) Sphingomyelin-enriched microdomains define the efficiency of native Ca(2+)-triggered membrane fusion. J Cell Sci 119:2688–2694. https://doi.org/10.1242/jcs.03007
He J, Ren W, Wang W, Han W, Jiang L, Zhang D, Guo M (2022) Exosomal targeting and its potential clinical application. Drug Deliv and Transl Res 12:2385–2402. https://doi.org/10.1007/s13346-021-01087-1
Saunderson SC, Dunn AC, Crocker PR, McLellan AD (2014) CD169 mediates the capture of exosomes in spleen and lymph node. Blood 123:208–216. https://doi.org/10.1182/blood-2013-03-489732
Christianson HC, Svensson KJ, van Kuppevelt TH, Li JP, Belting M (2013) Cancer cell exosomes depend on cell-surface heparan sulfate proteoglycans for their internalization and functional activity. Proc Natl Acad Sci U S A 110:17380–17385. https://doi.org/10.1073/pnas.1304266110
Purushothaman A, Bandari SK, Chandrashekar DS, Jones RJ, Lee HC, Weber DM, Orlowski RZ (2017) Chondroitin sulfate proteoglycan serglycin influences protein cargo loading and functions of tumor-derived exosomes. Oncotarget 8:73723–73732. https://doi.org/10.18632/oncotarget.20564
Purushothaman A, Bandari SK, Liu J, Mobley JA, Brown EE, Sanderson RD (2016) Fibronectin on the surface of myeloma cell-derived exosomes mediates exosome-cell interactions. J Biol Chem 291:1652–1663. https://doi.org/10.1074/jbc.M115.686295
Lima LG, Ham S, Shin H, Chai EPZ, Lek ESH, Lobb RJ, Muller AF, Mathivanan S, Yeo B, Choi Y et al (2021) Tumor microenvironmental cytokines bound to cancer exosomes determine uptake by cytokine receptor-expressing cells and biodistribution. Nat Commun 12:3543. https://doi.org/10.1038/s41467-021-23946-8
Berditchevski F, Odintsova E (1999) Characterization of integrin-tetraspanin adhesion complexes: role of tetraspanins in integrin signaling. J Cell Biol 146:477–492
Nazarenko I, Rana S, Baumann A, McAlear J, Hellwig A, Trendelenburg M, Lochnit G, Preissner KT, Zoller M (2010) Cell surface tetraspanin Tspan8 contributes to molecular pathways of exosome-induced endothelial cell activation. Cancer Res 70:1668–1678. https://doi.org/10.1158/0008-5472.CAN-09-2470
Mulcahy LA, Pink RC, Carter DR (2014) Routes and mechanisms of extracellular vesicle uptake. J of Extracellular Vesicle. https://doi.org/10.3402/jev.v3.24641
Tian T, Zhu YL, Zhou YY, Liang GF, Wang YY, Hu FH, Xiao ZD (2014) Exosome uptake through clathrin-mediated endocytosis and macropinocytosis and mediating miR-21 delivery. J Biol Chem 289:22258–22267. https://doi.org/10.1074/jbc.M114.588046
Feng D, Zhao WL, Ye YY, Bai XC, Liu RQ, Chang LF, Zhou Q, Sui SF (2010) Cellular internalization of exosomes occurs through phagocytosis. Traffic 11:675–687. https://doi.org/10.1111/j.1600-0854.2010.01041.x
Fitzner D, Schnaars M, van Rossum D, Krishnamoorthy G, Dibaj P, Bakhti M, Regen T, Hanisch UK, Simons M (2011) Selective transfer of exosomes from oligodendrocytes to microglia by macropinocytosis. J Cell Sci 124:447–458. https://doi.org/10.1242/jcs.074088
Taylor MJ, Perrais D, Merrifield CJ (2011) A high precision survey of the molecular dynamics of mammalian clathrin-mediated endocytosis. PLoS Biol 9:e1000604. https://doi.org/10.1371/journal.pbio.1000604
Giangreco G, Malabarba MG, Sigismund S (2021) Specialised endocytic proteins regulate diverse internalisation mechanisms and signalling outputs in physiology and cancer. Biol Cell 113:165–182. https://doi.org/10.1111/boc.202000129
Kovtun O, Dickson VK, Kelly BT, Owen DJ, Briggs JAG (2020) Architecture of the AP2/clathrin coat on the membranes of clathrin-coated vesicles. Sci Adv 6:eaba8381. https://doi.org/10.1126/sciadv.aba8381
Kirchhausen T (2000) Clathrin. Annu Rev Biochem 69:699–727. https://doi.org/10.1146/annurev.biochem.69.1.699
McMahon HT, Boucrot E (2011) Molecular mechanism and physiological functions of clathrin-mediated endocytosis. Nat Rev Mol Cell Biol 12:517–533. https://doi.org/10.1038/nrm3151
Cronqvist T, Erlandsson L, Tannetta D, Hansson SR (2020) Placental syncytiotrophoblast extracellular vesicles enter primary endothelial cells through clathrin-mediated endocytosis. Placenta 100:133–141. https://doi.org/10.1016/j.placenta.2020.07.006
Cheung KL, Jarrett R, Subramaniam S, Salimi M, Gutowska-Owsiak D, Chen YL, Hardman C, Xue L, Cerundolo V, Ogg G (2016) Psoriatic T cells recognize neolipid antigens generated by mast cell phospholipase delivered by exosomes and presented by CD1a. J Exp Med 213:2399–2412. https://doi.org/10.1084/jem.20160258
Popena I, Abols A, Saulite L, Pleiko K, Zandberga E, Jekabsons K, Endzelins E, Llorente A, Line A, Riekstina U (2018) Effect of colorectal cancer-derived extracellular vesicles on the immunophenotype and cytokine secretion profile of monocytes and macrophages. Cell Commun Signal 16:17. https://doi.org/10.1186/s12964-018-0229-y
Ginini L, Billan S, Fridman E, Gil Z (2022) Insight into extracellular vesicle-cell communication: from cell recognition to intracellular fate. Cells. https://doi.org/10.3390/cells11091375
Koumangoye RB, Sakwe AM, Goodwin JS, Patel T, Ochieng J (2011) Detachment of breast tumor cells induces rapid secretion of exosomes which subsequently mediate cellular adhesion and spreading. PLoS One 6:e24234. https://doi.org/10.1371/journal.pone.0024234
Svensson KJ, Christianson HC, Wittrup A, Bourseau-Guilmain E, Lindqvist E, Svensson LM, Morgelin M, Belting M (2013) Exosome uptake depends on ERK1/2-heat shock protein 27 signaling and lipid Raft-mediated endocytosis negatively regulated by caveolin‑1. J Biol Chem 288:17713–17724. https://doi.org/10.1074/jbc.M112.445403
Khan I, Steeg PS (2021) Endocytosis: a pivotal pathway for regulating metastasis. Br J Cancer 124:66–75. https://doi.org/10.1038/s41416-020-01179-8
Furmanik M, Chatrou M, van Gorp R, Akbulut A, Willems B, Schmidt H, van Eys G, Bochaton-Piallat ML, Proudfoot D, Biessen E et al (2020) Reactive oxygen-forming Nox5 links vascular smooth muscle cell phenotypic switching and extracellular vesicle-mediated vascular calcification. Circ Res 127:911–927. https://doi.org/10.1161/CIRCRESAHA.119.316159
Ahram M, Sameni M, Qiu RG, Linebaugh B, Kirn D, Sloane BF (2000) Rac1-induced endocytosis is associated with intracellular proteolysis during migration through a three-dimensional matrix. Exp Cell Res 260:292–303. https://doi.org/10.1006/excr.2000.5031
Kerr MC, Teasdale RD (2009) Defining macropinocytosis. Traffic 10:364–371. https://doi.org/10.1111/j.1600-0854.2009.00878.x
Costa Verdera H, Gitz-Francois JJ, Schiffelers RM, Vader P (2017) Cellular uptake of extracellular vesicles is mediated by clathrin-independent endocytosis and macropinocytosis. J Control Release 266:100–108. https://doi.org/10.1016/j.jconrel.2017.09.019
Wang Z, Zhu H, Shi H, Zhao H, Gao R, Weng X, Liu R, Li X, Zou Y, Hu K et al (2019) Exosomes derived from M1 macrophages aggravate neointimal hyperplasia following carotid artery injuries in mice through miR-222/CDKN1B/CDKN1C pathway. Cell Death Dis 10:422. https://doi.org/10.1038/s41419-019-1667-1
Nakase I, Kobayashi NB, Takatani-Nakase T, Yoshida T (2015) Active macropinocytosis induction by stimulation of epidermal growth factor receptor and oncogenic Ras expression potentiates cellular uptake efficacy of exosomes. Sci Rep 5:10300. https://doi.org/10.1038/srep10300
Li YX, Pang HB (2021) Macropinocytosis as a cell entry route for peptide-functionalized and bystander nanoparticles. J Control Release 329:1222–1230. https://doi.org/10.1016/j.jconrel.2020.10.049
Desrochers LM, Bordeleau F, Reinhart-King CA, Cerione RA, Antonyak MA (2016) Microvesicles provide a mechanism for intercellular communication by embryonic stem cells during embryo implantation. Nat Commun 7:11958. https://doi.org/10.1038/ncomms11958
Mathieu M, Martin-Jaular L, Lavieu G, Thery C (2019) Specificities of secretion and uptake of exosomes and other extracellular vesicles for cell-to-cell communication. Nat Cell Biol 21:9–17. https://doi.org/10.1038/s41556-018-0250-9
Hazawa M, Tomiyama K, Saotome-Nakamura A, Obara C, Yasuda T, Gotoh T, Tanaka I, Yakumaru H, Ishihara H, Tajima K (2014) Radiation increases the cellular uptake of exosomes through CD29/CD81 complex formation. Biochem Biophys Res Commun 446:1165–1171. https://doi.org/10.1016/j.bbrc.2014.03.067
Mrowczynski OD, Madhankumar AB, Sundstrom JM, Zhao Y, Kawasawa YI, Slagle-Webb B, Mau C, Payne RA, Rizk EB, Zacharia BE et al (2018) Exosomes impact survival to radiation exposure in cell line models of nervous system cancer. Oncotarget 9:36083–36101. https://doi.org/10.18632/oncotarget.26300
Tu C, Du Z, Zhang H, Feng Y, Qi Y, Zheng Y, Liu J, Wang J (2021) Endocytic pathway inhibition attenuates extracellular vesicle-induced reduction of chemosensitivity to bortezomib in multiple myeloma cells. Theranostics 11:2364–2380. https://doi.org/10.7150/thno.47996
Tsai WC, Hsu CC, Pang JH, Lin MS, Chen YH, Liang FC (2012) Low-level laser irradiation stimulates tenocyte migration with up-regulation of dynamin II expression. PLoS One 7:e38235. https://doi.org/10.1371/journal.pone.0038235
Qian J, Yang J, Dragovic AF, Abu-Isa E, Lawrence TS, Zhang M (2005) Ionizing radiation-induced adenovirus infection is mediated by dynamin 2. Cancer Res 65:5493–5497. https://doi.org/10.1158/0008-5472.CAN-04-4526
Tortolici F, Vumbaca S, Incocciati B, Dayal R, Aquilano K, Giovanetti A, Rufini S (2021) Ionizing radiation-induced extracellular vesicle release promotes AKT-associated survival response in SH-SY5Y neuroblastoma cells. Cells. https://doi.org/10.3390/cells10010107
Tomas A, Futter CE, Eden ER (2014) EGF receptor trafficking: consequences for signaling and cancer. Trends Cell Biol 24:26–34. https://doi.org/10.1016/j.tcb.2013.11.002
Zhang Y, Yu S, Zhuang L, Zheng Z, Chao T, Fu Q (2012) Caveolin‑1 is involved in radiation-induced ERBB2 nuclear transport in breast cancer cells. J Huazhong Univ Sci Technol Med Sci 32:888–892. https://doi.org/10.1007/s11596-012-1053-z
Zhu H, Yue J, Pan Z, Wu H, Cheng Y, Lu H, Ren X, Yao M, Shen Z, Yang JM (2010) Involvement of caveolin‑1 in repair of DNA damage through both homologous recombination and non-homologous end joining. PLoS One 5:e12055. https://doi.org/10.1371/journal.pone.0012055
Cordes N, Frick S, Brunner TB, Pilarsky C, Grutzmann R, Sipos B, Kloppel G, McKenna WG, Bernhard EJ (2007) Human pancreatic tumor cells are sensitized to ionizing radiation by knockdown of caveolin‑1. Oncogene 26:6851–6862. https://doi.org/10.1038/sj.onc.1210498
Qian M, Wang S, Guo X, Wang J, Zhang Z, Qiu W, Gao X, Chen Z, Xu J, Zhao R et al (2020) Hypoxic glioma-derived exosomes deliver microRNA-1246 to induce M2 macrophage polarization by targeting TERF2IP via the STAT3 and NF-kappaB pathways. Oncogene 39:428–442. https://doi.org/10.1038/s41388-019-0996-y
Baselet B, Azimzadeh O, Erbeldinger N, Bakshi MV, Dettmering T, Janssen A, Ktitareva S, Lowe DJ, Michaux A, Quintens R et al (2017) Differential impact of single-dose Fe Ion and X‑ray irradiation on endothelial cell transcriptomic and proteomic responses. Front Pharmacol 8:570. https://doi.org/10.3389/fphar.2017.00570
Nakaoka A, Nakahana M, Inubushi S, Akasaka H, Salah M, Fujita Y, Kubota H, Hassan M, Nishikawa R, Mukumoto N et al (2021) Exosome-mediated radiosensitizing effect on neighboring cancer cells via increase in intracellular levels of reactive oxygen species. Oncol Rep. https://doi.org/10.3892/or.2021.7964
Wang WL, Huang WC (2016) Rac1 is a potential target to circumvent radioresistance. J Thorac Dis 8:E1475–E1477. https://doi.org/10.21037/jtd.2016.11.79
Rathinam R, Berrier A, Alahari SK (2011) Role of Rho GTPases and their regulators in cancer progression. Front Biosci 16:2561–2571. https://doi.org/10.2741/3872
Hein AL, Post CM, Sheinin YM, Lakshmanan I, Natarajan A, Enke CA, Batra SK, Ouellette MM, Yan Y (2016) RAC1 GTPase promotes the survival of breast cancer cells in response to hyper-fractionated radiation treatment. Oncogene 35:6319–6329. https://doi.org/10.1038/onc.2016.163
Yan Y, Hein AL, Etekpo A, Burchett KM, Lin C, Enke CA, Batra SK, Cowan KH, Ouellette MM (2014) Inhibition of RAC1 GTPase sensitizes pancreatic cancer cells to gamma-irradiation. Oncotarget 5:10251–10270. https://doi.org/10.18632/oncotarget.2500
Yan Y, Greer PM, Cao PT, Kolb RH, Cowan KH (2012) RAC1 GTPase plays an important role in gamma-irradiation induced G2/M checkpoint activation. Breast Cancer Res 14:R60. https://doi.org/10.1186/bcr3164
Hamalukic M, Huelsenbeck J, Schad A, Wirtz S, Kaina B, Fritz G (2011) Rac1-regulated endothelial radiation response stimulates extravasation and metastasis that can be blocked by HMG-CoA reductase inhibitors. PLoS One 6:e26413. https://doi.org/10.1371/journal.pone.0026413
Faissal Ouenzar MJH, Weinfeld M (2016) Shuttling towards a predictive assay for radiotherapy. Transl Cancer Res. https://doi.org/10.21037/tcr.2016.10.61
Lim DS, Kirsch DG, Canman CE, Ahn JH, Ziv Y, Newman LS, Darnell RB, Shiloh Y, Kastan MB (1998) ATM binds to beta-adaptin in cytoplasmic vesicles. Proc Natl Acad Sci U S A 95:10146–10151. https://doi.org/10.1073/pnas.95.17.10146
Sundqvist T, Liu SM (1993) Hydrogen peroxide stimulates endocytosis in cultured bovine aortic endothelial cells. Acta Physiol Scand 149:127–131. https://doi.org/10.1111/j.1748-1716.1993.tb09604.x
Liu SM, Sundqvist T (1995) Effects of hydrogen peroxide and phorbol myristate acetate on endothelial transport and F‑actin distribution. Exp Cell Res 217:1–7. https://doi.org/10.1006/excr.1995.1056
Khan EM, Heidinger JM, Levy M, Lisanti MP, Ravid T, Goldkorn T (2006) Epidermal growth factor receptor exposed to oxidative stress undergoes Src- and caveolin-1-dependent perinuclear trafficking. J Biol Chem 281:14486–14493. https://doi.org/10.1074/jbc.M509332200
Lerner N, Chen I, Schreiber-Avissar S, Beit-Yannai E (2020) Extracellular vesicles mediate anti-oxidative response-in vitro study in the ocular drainage system. Int J Mol Sci. https://doi.org/10.3390/ijms21176105
Funding
This work was supported by Euratom Research and Training Programme 2021–2025, grant agreement number 101061037.
Author information
Authors and Affiliations
Contributions
LK and TSz had the idea for the article; TSz, KB, and IBCs performed the literature search of different parts of the manuscript and drafted the work; GS and KL revised the manuscript critically. All authors approved the version to be published and agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
T. Szatmári, K. Balázs, I.B. Csordás, G. Sáfrány, and K. Lumniczky declare that they have no competing interests.
Additional information
The authors Katalin Balázs and Ilona Barbara Csordás contributed equally to the manuscript.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Szatmári, T., Balázs, K., Csordás, I.B. et al. Effect of radiotherapy on the DNA cargo and cellular uptake mechanisms of extracellular vesicles. Strahlenther Onkol 199, 1191–1213 (2023). https://doi.org/10.1007/s00066-023-02098-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-023-02098-2