Abstract
Background
Intercellular communication between macrophages and peritoneal mesothelial cells (PMCs) has been suggested as a key factor regulating peritonitis development. Here, we explored whether PPARγ (peroxisome proliferator-activated receptor gamma) can be packaged into macrophage exosomes to mediate intercellular communication and regulate peritonitis.
Methods
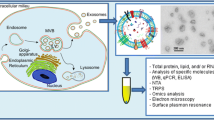
Macrophage exosomes were isolated by ultracentrifugation and identified by nanoparticle tracking analysis and transmission electron microscopy. Proteomic analysis of macrophage-derived exosomes was performed using mass spectrometry. Co-culture models of supernatants or exosomes with PMCs, as well as a mouse peritonitis model induced by lipopolysaccharide (LPS), were employed.
Results
In this study, using stable Raw264.7 cells overexpressing GFP-FLAG-PPARγ (OE-PPARγ), we found that PPARγ inhibited LPS-induced inflammatory responses in Raw264.7 cells and that PPARγ was incorporated into macrophage exosomes during this process. Overexpression of PPARγ mainly regulated the secretion of differentially expressed exosomal proteins involved in the biological processes of protein transport, lipid metabolic process, cell cycle, apoptotic process, DNA damage stimulus, as well as the KEGG pathway of salmonella infection. Using co-culture models and mouse peritonitis model, we showed that exosomes from Raw264.7 cells overexpressing PPARγ inhibited LPS-induced inflammation in co-cultured human PMCs and in mice through downregulating CD14 and TLR4, two key regulators of the salmonella infection pathway. Pretreatment of the PPARγ inhibitor GW9662 abolished the anti-inflammatory effect of exosomes from Raw264.7 OE-PPARγ cells on human PMCs.
Conclusions
These results suggested that overexpression of PPARγ largely altered the proteomic profile of macrophage exosomes and that exosomal PPARγ from macrophages acted as a regulator of intercellular communication to suppress LPS-induced inflammatory responses in vitro and in vivo via negatively regulating the CD14/TLR4 axis.







Similar content being viewed by others
Data availability
The datasets generated during the current study are available in the ProteomeXchange Consortium via the PRIDE partner repository with the identifier PXD039203 (http://www.proteomexchange.org/). All other data generated during this study are included in this published article and its supplementary information file.
Abbreviations
- CD14:
-
Cluster of differentiation 14
- CD63:
-
Cluster of differentiation 63
- FDR:
-
False discovery rate
- HE:
-
Hematoxylin–eosin
- IHC:
-
Immunohistochemistry
- IL-1β:
-
Interleukin 1β
- iNOS:
-
Inducible nitric oxide synthase
- KEGG:
-
Kyoto encyclopedia of genes and genomes
- LPS:
-
Lipopolysaccharide
- MS:
-
Mass spectrometry
- NTA:
-
Nanoparticle tracking analysis
- OE-PPARγ:
-
Overexpression of PPARγ
- OE-V:
-
Overexpression of vector
- PD:
-
Peritoneal dialysis
- PMCs:
-
Peritoneal mesothelial cells
- PPARγ:
-
Peroxisome proliferator-activated receptor gamma
- qRT-PCR:
-
Quantitative real-time PCR
- TEM:
-
Transmission electron microscopy
- TNF-α:
-
Tumor necrosis factor-alpha
- TLR4:
-
Toll-like receptor 4
References
Mehrotra R, Devuyst O, Davies SJ, Johnson DW. The current state of peritoneal dialysis. J Am Soc Nephrol. 2016;27:3238–52. https://doi.org/10.1681/ASN.2016010112.
Terri M, Trionfetti F, Montaldo C, Cordani M, Tripodi M, Lopez-Cabrera M, Strippoli R. Mechanisms of peritoneal fibrosis: focus on immune cells-peritoneal stroma interactions. Front Immunol. 2021;12: 607204. https://doi.org/10.3389/fimmu.2021.607204.
Nochaiwong S, et al. A clinical risk prediction tool for peritonitis-associated treatment failure in peritoneal dialysis patients. Sci Rep. 2018;8:14797. https://doi.org/10.1038/s41598-018-33196-2.
Mutsaers SE, Birnie K, Lansley S, Herrick SE, Lim CB, Prele CM. Mesothelial cells in tissue repair and fibrosis. Front Pharmacol. 2015;6:113. https://doi.org/10.3389/fphar.2015.00113.
Wilm B, Munoz-Chapuli R. The role of WT1 in embryonic development and normal organ homeostasis. Methods Mol Biol. 2016;1467:23–39. https://doi.org/10.1007/978-1-4939-4023-3_3.
Yung S, Chan TM. Pathophysiological changes to the peritoneal membrane during PD-related peritonitis: the role of mesothelial cells. Mediat Inflamm. 2012;2012: 484167. https://doi.org/10.1155/2012/484167.
Topley N, Mackenzie RK, Williams JD. Macrophages and mesothelial cells in bacterial peritonitis. Immunobiology. 1996;195:563–73. https://doi.org/10.1016/S0171-2985(96)80022-2.
Langston PK, et al. Glycerol phosphate shuttle enzyme GPD2 regulates macrophage inflammatory responses. Nat Immunol. 2019;20:1186–95. https://doi.org/10.1038/s41590-019-0453-7.
He C, Zheng S, Luo Y, Wang B. Exosome theranostics: biology and translational medicine. Theranostics. 2018;8:237–55. https://doi.org/10.7150/thno.21945.
Kalluri R, LeBleu VS. The biology, function, and biomedical applications of exosomes. Science. 2020. https://doi.org/10.1126/science.aau6977.
Zhang X, Yuan X, Shi H, Wu L, Qian H, Xu W. Exosomes in cancer: small particle, big player. J Hematol Oncol. 2015;8:83. https://doi.org/10.1186/s13045-015-0181-x.
Simpson RJ, Lim JW, Moritz RL, Mathivanan S. Exosomes: proteomic insights and diagnostic potential. Expert Rev Proteomics. 2009;6:267–83. https://doi.org/10.1586/epr.09.17.
Carvalho MV, Goncalves-de-Albuquerque CF, Silva AR. PPAR gamma: from definition to molecular targets and therapy of lung diseases. Int J Mol Sci. 2021. https://doi.org/10.3390/ijms22020805.
Montaigne D, Butruille L, Staels B. PPAR control of metabolism and cardiovascular functions. Nat Rev Cardiol. 2021;18:809–23. https://doi.org/10.1038/s41569-021-00569-6.
Vallee A, Lecarpentier Y. Crosstalk between peroxisome proliferator-activated receptor gamma and the canonical WNT/beta-catenin pathway in chronic inflammation and oxidative stress during carcinogenesis. Front Immunol. 2018;9:745. https://doi.org/10.3389/fimmu.2018.00745.
Li Z, Feng J, Yang S, Meng P, Li J, Li H, Gao X, Zhang Y. Lipopolysaccharide-induced inflammation in human peritoneal mesothelial cells is controlled by ERK1/2-CDK5-PPARgamma axis. Ann Transl Med. 2021;9:850. https://doi.org/10.21037/atm-21-1623.
Jiang C, Ting AT, Seed B. PPAR-gamma agonists inhibit production of monocyte inflammatory cytokines. Nature. 1998;391:82–6. https://doi.org/10.1038/34184.
Brunmeir R, Xu F. Functional regulation of PPARs through post-translational modifications. Int J Mol Sci. 2018. https://doi.org/10.3390/ijms19061738.
Pascual G, et al. A SUMOylation-dependent pathway mediates transrepression of inflammatory response genes by PPAR-gamma. Nature. 2005;437:759–63. https://doi.org/10.1038/nature03988.
Hernandez-Quiles M, Broekema MF, Kalkhoven E. PPARgamma in metabolism, immunity, and cancer: unified and diverse mechanisms of action. Front Endocrinol (Lausanne). 2021;12: 624112. https://doi.org/10.3389/fendo.2021.624112.
Ho MM, Manughian-Peter A, Spivia WR, Taylor A, Fraser DA. Macrophage molecular signaling and inflammatory responses during ingestion of atherogenic lipoproteins are modulated by complement protein C1q. Atherosclerosis. 2016;253:38–46. https://doi.org/10.1016/j.atherosclerosis.2016.08.019.
Ran L, et al. Cx3cr1 deficiency in mice attenuates hepatic granuloma formation during acute schistosomiasis by enhancing the M2-type polarization of macrophages. Dis Model Mech. 2015;8:691–700. https://doi.org/10.1242/dmm.018242.
Zhao M, Bian YY, Yang LL, Chen YQ, Wang YJ, Ma YT, Pei YQ, Li WL, Zeng L. HuoXueTongFu formula alleviates intraperitoneal adhesion by regulating macrophage polarization and the SOCS/JAK2/STAT/PPAR-gamma signalling pathway. Mediators Inflamm. 2019;2019:1769374. https://doi.org/10.1155/2019/1769374.
Zhang YF, Zou XL, Wu J, Yu XQ, Yang X. Rosiglitazone, a peroxisome proliferator-activated receptor (PPAR)-gamma agonist, attenuates inflammation via NF-kappaB inhibition in lipopolysaccharide-induced peritonitis. Inflammation. 2015;38:2105–15. https://doi.org/10.1007/s10753-015-0193-2.
Zhang Y, Feng J, Wang Q, Zhao S, Xu J, Li H. PPAR-gamma agonist rosiglitazone ameliorates peritoneal deterioration in peritoneal dialysis rats with LPS-induced peritonitis through up-regulation of AQP-1 and ZO-1. 2018. Biosci Rep. https://doi.org/10.1042/BSR20180009.
Looze C, et al. Proteomic profiling of human plasma exosomes identifies PPARgamma as an exosome-associated protein. Biochem Biophys Res Commun. 2009;378:433–8. https://doi.org/10.1016/j.bbrc.2008.11.050.
Gao X, et al. ZSWIM1 promotes the proliferation and metastasis of lung adenocarcinoma cells through the STK38/MEKK2/ERK1/2 axis. J Proteome Res. 2022. https://doi.org/10.1021/acs.jproteome.2c00412.
Zhang HT, et al. TRIM21-regulated Annexin A2 plasma membrane trafficking facilitates osteosarcoma cell differentiation through the TFEB-mediated autophagy. Cell Death Dis. 2021;12:21. https://doi.org/10.1038/s41419-020-03364-2.
Gao X, et al. hnRNPK inhibits GSK3beta Ser9 phosphorylation, thereby stabilizing c-FLIP and contributes to TRAIL resistance in H1299 lung adenocarcinoma cells. Sci Rep. 2016;6:22999. https://doi.org/10.1038/srep22999.
Zeng QZ, Liu WT, Lu JL, Liu XH, Zhang YF, Liu LX, Gao XJ. YWHAZ binds to TRIM21 but is not involved in TRIM21-stimulated osteosarcoma cell proliferation. Biomed Environ Sci. 2018;31:186–96. https://doi.org/10.3967/bes2018.024.
Feng J, Lu M, Li W, Li J, Meng P, Li Z, Gao X, Zhang Y. PPARgamma alleviates peritoneal fibrosis progression along with promoting GLUT1 expression and suppressing peritoneal mesothelial cell proliferation. Mol Cell Biochem. 2022;477:1959–71. https://doi.org/10.1007/s11010-022-04419-y.
Miao J, et al. Wnt/beta-catenin/RAS signaling mediates age-related renal fibrosis and is associated with mitochondrial dysfunction. Aging Cell. 2019;18: e13004. https://doi.org/10.1111/acel.13004.
Simons M, Raposo G. Exosomes–vesicular carriers for intercellular communication. Curr Opin Cell Biol. 2009;21:575–81. https://doi.org/10.1016/j.ceb.2009.03.007.
Lee SM, Son KN, Shah D, Ali M, Balasubramaniam A, Shukla D, Aakalu VK. Histatin-1 attenuates LPS-induced inflammatory signaling in RAW264.7 macrophages. Int J Mol Sci. 2021. https://doi.org/10.3390/ijms22157856.
Wang G, et al. Proteomic profiling of LPS-induced macrophage-derived exosomes indicates their involvement in acute liver injury. Proteomics. 2019;19: e1800274. https://doi.org/10.1002/pmic.201800274.
Hui WW, Hercik K, Belsare S, Alugubelly N, Clapp B, Rinaldi C, Edelmann MJ. Salmonella enterica serovar Typhimurium alters the extracellular proteome of macrophages and leads to the production of proinflammatory exosomes. Infect Immun. 2018. https://doi.org/10.1128/IAI.00386-17.
Wang JJ, Chen C, Xie PF, Pan Y, Tan YH, Tang LJ. Proteomic analysis and immune properties of exosomes released by macrophages infected with Mycobacterium avium. Microbes Infect. 2014;16:283–91. https://doi.org/10.1016/j.micinf.2013.12.001.
Bouhlel MA, et al. PPARgamma activation primes human monocytes into alternative M2 macrophages with anti-inflammatory properties. Cell Metab. 2007;6:137–43. https://doi.org/10.1016/j.cmet.2007.06.010.
Wu MM, Wang QM, Huang BY, Mai CT, Wang CL, Wang TT, Zhang XJ. Dioscin ameliorates murine ulcerative colitis by regulating macrophage polarization. Pharmacol Res. 2021;172: 105796. https://doi.org/10.1016/j.phrs.2021.105796.
Zhou JP, Yang XN, Song Y, Zhou F, Liu JJ, Hu YQ, Chen LG. Rosiglitazone alleviates lipopolysaccharide-induced inflammation in RAW264.7 cells via inhibition of NF-kappaB and in a PPARgamma-dependent manner. Exp Ther Med. 2021;22:743. https://doi.org/10.3892/etm.2021.10175.
Ciesielska A, Matyjek M, Kwiatkowska K. TLR4 and CD14 trafficking and its influence on LPS-induced pro-inflammatory signaling. Cell Mol Life Sci. 2021;78:1233–61. https://doi.org/10.1007/s00018-020-03656-y.
Plociennikowska A, Hromada-Judycka A, Dembinska J, Roszczenko P, Ciesielska A, Kwiatkowska K. Contribution of CD14 and TLR4 to changes of the PI(4,5)P2 level in LPS-stimulated cells. J Leukoc Biol. 2016;100:1363–73. https://doi.org/10.1189/jlb.2VMA1215-577R.
Wensink AC, Kemp V, Fermie J, Garcia Laorden MI, van der Poll T, Hack CE, Bovenschen N. Granzyme K synergistically potentiates LPS-induced cytokine responses in human monocytes. Proc Natl Acad Sci USA. 2014;111:5974–9. https://doi.org/10.1073/pnas.1317347111.
Ryu JK, et al. Reconstruction of LPS transfer cascade reveals structural determinants within LBP, CD14, and TLR4-MD2 for efficient LPS recognition and transfer. Immunity. 2017;46:38–50. https://doi.org/10.1016/j.immuni.2016.11.007.
Gioannini TL, Teghanemt A, Zhang D, Levis EN, Weiss JP. Monomeric endotoxin:protein complexes are essential for TLR4-dependent cell activation. J Endotoxin Res. 2005;11:117–23. https://doi.org/10.1179/096805105X35198.
Schappe MS, et al. Chanzyme TRPM7 mediates the Ca(2+) influx essential for lipopolysaccharide-induced toll-like receptor 4 endocytosis and macrophage activation. Immunity. 2018;48:59-74 e5. https://doi.org/10.1016/j.immuni.2017.11.026.
Kagan JC, Su T, Horng T, Chow A, Akira S, Medzhitov R. TRAM couples endocytosis of toll-like receptor 4 to the induction of interferon-beta. Nat Immunol. 2008;9:361–8. https://doi.org/10.1038/ni1569.
Funding
This work was supported by National Natural Science Foundation of China (81800675; 81860143; 82200758), Medical Scientific Research Foundation of Guangdong Province of China (A2021251), Guangdong Basic and Applied Basic Research Foundation (2023A1515011221; 2023A1515010248), China Postdoctoral Science Foundation (2018M633085), Guangzhou Science and Technology Project (202201010034). Open project supported by the Key Laboratory of tumor molecular biology of the Ministry of education of Jinan University (202203).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. MM and ML contributed to the execution of most experiments and data analysis. JF, XZ, PM, LC and XL contributed to the performance of the rest experiments. MM, LL, XG and YZ wrote the first draft of the manuscript. XZ, LL, XG and YZ contributed to the conception and design of the experiment, data analysis, drafted the manuscript and approved the final version to be published.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethical approval
All animal procedures were approved by the Experimental Animal Ethics Committee of Jinan University, Guangzhou, China (approval number: 100041).
Additional information
Responsible Editor: L Li.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
11_2023_1765_MOESM2_ESM.xlsx
Supplementary file2Table S1. Differentially secreted proteins of exosomes from the indicated groups identified in this study (XLSX 463 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Meng, M., Lu, M., Feng, J. et al. Exosomal PPARγ derived from macrophages suppresses LPS-induced peritonitis by negative regulation of CD14/TLR4 axis. Inflamm. Res. 72, 1567–1581 (2023). https://doi.org/10.1007/s00011-023-01765-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-023-01765-5