Abstract
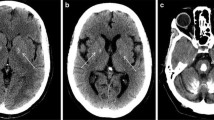
Familial idiopathic basal ganglia calcification (FIBGC), also known as “Fahr’s disease,” is a neuropsychiatric disorder with motor and cognitive symptoms. It is characterized pathologically by bilateral calcification most commonly in the basal ganglia and also in other brain regions such as the thalamus and cerebellum. A recent report by Wang et al. (2012) discovered multiple families with FIBGC carrying mutations in the SLC20A2 gene, encoding the inorganic phosphate transporter PiT-2, which segregated in an autosomal dominant pattern. To understand further the role of SLC20A2 in FIBGC brain pathology, here we described the gene expression pattern across the whole brain for SLC20A2, using the Allen Institute Human Brain Atlas database. Microarray analysis provided evidence that the neuroanatomical pattern of expression for SLC20A2 is highest in the regions most commonly affected in FIBGC. Neuroanatomical regions that demonstrated high correlation or anti-correlation with SLC20A2 expression also showed a molecular network with potential to explain the limited neuroanatomical distribution of calcifications in IBGC. Lastly, these co-expression networks suggest additional further candidate genes for FIBGC.
Similar content being viewed by others
References
Allen Institute for Brain Science (2009). Allen Human Brain Atlas. Allen Institute for Brain Science, Seattle, WA. Available from: http://www.brain-map.org. Accessed 5 Oct 2012
Bourassa CV, Meijer IA, Merner ND et al (2012) VAMP1 mutation causes dominant hereditary spastic ataxia in Newfoundland families. Am J Hum Genet 91(3):548–552
Collins JF, Bai L, Guichan FK (2004) The SLC20 family of proteins: dual functions as sodium-phosphate cotransporters and viral receptors. Pflügers Arch 447:647–652
Dahlin A, Royall J, Hohmann JG, Wang J (2009) Expression profiling of the solute carrier gene family in the mouse brain. J Pharmacol Exp Ther 329:558–570
Gregório SP, Sallet PC, Do KA, Lin E, Gattaz WF, Dias-Neto E (2009) Polymorphisms in genes involved in neurodevelopment may be associated with altered brain morphology in schizophrenia: preliminary evidence. Psychiatry Res 165(1–2):1–9
Kavanaugh MP, Kabat D (1996) Identification and characterization of a widely expressed phosphate transporter/retrovirus receptor family. Kidney Int 49:959–963
Kudo LC, Parfenova L, Vi N et al (2010) Integrative gene–tissue microarray-based approach for identification of human disease biomarkers: application to amyotrophic lateral sclerosis. Hum Mol Genet 16:3233–3253
Lagrue E, Abe H, Lavanya M et al (2010) Regional characterization of energy metabolism in the brain of normal and MPTP-intoxicated mice using new markers of glucose and phosphate transport. J Biomed Sci 17:91
Nakazawa K, Zsiros V, Jiang Z et al (2011) GABAergic interneuron origin of schizophrenia pathophysiology. Neuropharmacology 62(3):1574–1583
Nunes F, Shen Y, Niida Y et al (2005) Inactivation patterns of NF2 and DAL-1/4.1B (EPB41L3) in sporadic meningioma. Cancer Genet. Cytogenet 162(2):135–139
Oliveira JRM (2011) Managing idiopathic basal ganglia calcification (“Fahr’s disease”), 1st edn. Nova Publishing, New York
Philibert C, Bouillot S, Huber P, Faury G (2012) Protocadherin-12 deficiency leads to modifications in the structure and function of arteries in mice. Pathol Biol (Paris) 60(1):34–40
Sobrido MJ, Hopfer S, Geschwind DH (2007) Familial idiopathic basal ganglia calcification. GeneReviews [Internet]. University of Washington, Seattle, WA
Virkki LV, Biber J, Murer H, Forster IC (2007) Phosphate transporters: a tale of two solute carrier families. Am J Physiol Renal Physiol 293:F643–F654
Wang C, Li Y, Shi L et al (2012) Mutations in SLC20A2 link familial idiopathic basal ganglia calcification with phosphate homeostasis. Nat Genet 44:254–256
Note
In March, 2013, after this article was accepted, the Allen Human Brain Atlas added a new normalization to their array data analysis (http://help.brain-map.org/display/humanbrain/Documentation). After repeating our study, based at the new normalization, we found some differences from our first analysis, for the correlates (PCDH12, RHOBTB2, SLC16A5, NEHF, VAMP1. MMEL1, EPB41L3, IDH3G, FLJ43860, CD55, TTC39A) and anti-correlates (GABRA4, RIN1, KCTD1, GABRA2, KCNH3, RGS20, ITPKA, FAM171B, DPF1, ACRN1). Several genes are present in both lists and even some of the new genes listed share similar molecular pathways with the previous ones listed. This actually increases the number of candidates to be explored in familial basal ganglia calcification.
Acknowledgments
JRMO received specific training for the Allen Institute of Brain Science Atlas during the 1st Molecular Neuroanatomy Course provided by the AIBS and the Okinawa Institute of Science and Technology. This study received support from the John Simon Guggenheim Memorial Foundation, Conselho Nacional de Pesquisa, Tecnologia e Inovação (CNPq). We are indebted to Mark Ziats, from NIH, for a great review and nice inputs to this manuscript.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
Heat map of probes corresponding to the genes whose expression profile shows greater correlation and anticorrelation compared to SLC20A2. We used data from two donors, marked in orange and blue on the top line. Immediately below, we grouped similar neuroanatomical structures to better visualize the correlation between expression profiles. The regions of basal nuclei, thalamus, and cerebellum are highlighted. GP, globus pallidus; Cd, caudate nucleus; Pu, putamen; TH, thalamus; Dt, dentate nucleus. Available from: http://www.brain-map.org. This is an edited version. ©2012 Allen Institute for Brain Science. Allen Brain Atlas [Internet] (PNG 2.15 MB)
Rights and permissions
About this article
Cite this article
da Silva, R.J.G., Pereira, I.C.L. & Oliveira, J.R.M. Analysis of Gene Expression Pattern and Neuroanatomical Correlates for SLC20A2 (PiT-2) Shows a Molecular Network with Potential Impact in Idiopathic Basal Ganglia Calcification (“Fahr’s Disease”). J Mol Neurosci 50, 280–283 (2013). https://doi.org/10.1007/s12031-013-0001-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12031-013-0001-0