Abstract
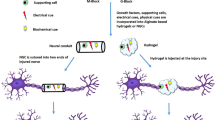
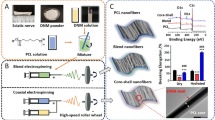
Artificial tissue engineering scaffolds can potentially provide support and guidance for the regrowth of severed axons following nerve injury. In this study, a hybrid biomaterial composed of alginate and hyaluronic acid (HA) was synthesized and characterized in terms of its suitability for covalent modification, biocompatibility for living Schwann cells and feasibility to construct three dimensional (3D) scaffolds. Carbodiimide mediated amide formation for the purpose of covalent crosslinking of the HA was carried out in the presence of calciumions that ionically crosslink alginate. Amide formation was found to be dependent on the concentrations of carbodiimide and calcium chloride. The double-crosslinked composite hydrogels display biocompatibility that is comparable to simple HA hydrogels, allowing for Schwann cell survival and growth. No significant difference was found between composite hydrogels made from different ratios of alginate and HA. A 3D BioPlotter™ rapid prototyping system was used to fabricate 3D scaffolds. The result indicated that combining HA with alginate facilitated the fabrication process and that 3D scaffolds with porous inner structure can be fabricated from the composite hydrogels, but not from HA alone. This information provides a basis for continuing in vitro and in vivo tests of the suitability of alginate/HA hydrogel as a biomaterial to create living cell scaffolds to support nerve regeneration.
Similar content being viewed by others
References
Causa F, Netti P A, Ambrosio L. A multi-functional scaffold for tissue regeneration: the need to engineer a tissue analogue. Biomaterials, 2007, 28(34): 5093–5099
Hollister S J. Porous scaffold design for tissue engineering. Nature Materials, 2005, 4(7): 518–524
Mondrinos M J, Dembzynski R, Lu L, et al. Porogen-based solid freeform fabrication of polycaprolactone-calcium phosphate scaffolds for tissue engineering. Biomaterials, 2006, 27(25): 4399–4408
Malda J, Woodfield T B, van der Vloodt F, et al. The effect of PEGT/PBT scaffold architecture on the composition of tissue engineered cartilage. Biomaterials, 2005, 26(1): 63–72
Burd D A R, Ritz M, Regauer S, et al. Hyaluronan and wound healing: a new perspective. British Journal of Plastic Surgery, 1991, 44(8): 579–584
Ozgenel G Y. Effects of hyaluronic acid on peripheral nerve scarring and regeneration in rats. Microsurgery, 2003, 23(6): 575–581
Lee H S, Kim J C. Effect of amniotic fluid in corneal sensitivity and nerve regeneration after excimer laser ablation. Cornea, 1996, 15(5): 517–524
Ikeda K, Yamauchi D, Osamura N, et al. Hyaluronic acid prevents peripheral nerve adhesion. British Journal of Plastic Surgery, 2003, 56(4): 342–347
Peattie R A, Nayate A P, Firpo M A, et al. Stimulation of in vivo angiogenesis by cytokine-loaded hyaluronic acid hydrogel implants. Biomaterials, 2004, 25(14): 2789–2798
Khaing Z Z, Milman B D, Vanscoy J E, et al. High molecular weight hyaluronic acid limits astrocyte activation and scar formation after spinal cord injury. Journal of Neural Engineering, 2011, 8(4): 046033
Struve J, Maher P C, Li Y Q, et al. Disruption of the hyaluronanbased extracellular matrix in spinal cord promotes astrocyte proliferation. Glia, 2005, 52(1): 16–24
Bourguignon L Y W, Peyrollier K, Gilad E, et al. Hyaluronan-CD44 interaction with neural Wiskott-Aldrich syndrome protein (N-WASP) promotes actin polymerization and ErbB2 activation leading to β-catenin nuclear translocation, transcriptional upregulation, and cell migration in ovarian tumor cells. The Journal of Biological Chemistry, 2007, 282(2): 1265–1280
Aruffo A, Stamenkovic I, Melnick M, et al. CD44 is the principal cell surface receptor for hyaluronate. Cell, 1990, 61(7): 1303–1313
Entwistle J, Hall C L, Turley E A. HA receptors: regulators of signalling to the cytoskeleton. Journal of Cellular Biochemistry, 1996, 61(4): 569–577
Hou S, Xu Q, Tian W, et al. The repair of brain lesion by implantation of hyaluronic acid hydrogels modified with laminin. Journal of Neuroscience Methods, 2005, 148(1): 60–70
Tian W M, Hou S P, Ma J, et al. Hyaluronic acid-poly-D-lysine-based three-dimensional hydrogel for traumatic brain injury. Tissue Engineering, 2005, 11(3–4): 513–525
Tian WM, Zhang C L, Hou S P, et al. Hyaluronic acid hydrogel as Nogo-66 receptor antibody delivery system for the repairing of injured rat brain: in vitro. Journal of Controlled Release, 2005, 102(1): 13–22
Wei Y-T, He Y, Xu C-L, et al. Hyaluronic acid hydrogel modified with nogo-66 receptor antibody and poly-L-lysine to promote axon regrowth after spinal cord injury. Journal of Biomedical Materials Research Part B: Applied Biomaterials, 2010, 95B(1): 110–117
Perets A, Baruch Y, Weisbuch F, et al. Enhancing the vascularization of three-dimensional porous alginate scaffolds by incorporating controlled release basic fibroblast growth factor microspheres. Journal of Biomedical Materials Research Part A, 2003, 65A(4): 489–497
Tobias C A, Dhoot N O, Wheatley M A, et al. Grafting of encapsulated BDNF-producing fibroblasts into the injured spinal cord without immune suppression in adult rats. Journal of Neurotrauma, 2001, 18(3): 287–301
Suzuki K, Suzuki Y, Ohnishi K, et al. Regeneration of transected spinal cord in young adult rats using freeze-dried alginate gel. Neuroreport, 1999, 10(14): 2891–2894
Suzuki Y, Kitaura M, Wu S, et al. Electrophysiological and horseradish peroxidase-tracing studies of nerve regeneration through alginate-filled gap in adult rat spinal cord. Neuroscience Letters, 2002, 318(3): 121–124
Prang P, Muller R, Eljaouhari A, et al. The promotion of oriented axonal regrowth in the injured spinal cord by alginate-based anisotropic capillary hydrogels. Biomaterials, 2006, 27(19): 3560–3569
Khalil S, Nam J, Sun W. Multi-nozzle deposition for construction of 3D biopolymer tissue scaffolds. Rapid Prototyping Journal, 2005, 11(1): 9–17
Haug A, Larsen B, Samuelsson B, et al. The solubility of alginate at low pH. Acta Chemica Scandinavica, 1963, 17(6): 1653–1662
Nakajima N, Ikada Y. Mechanism of amide formation by carbodiimide for bioconjugation in aqueous media. Bioconjugate Chemistry, 1995, 6(1): 123–130
Danishefsky I, Siskovic E. Conversion of carboxyl groups of mucopolysaccharides into amides of amino acid esters. Carbohydrate Research, 1971, 16(1): 199–205
LeRoux M A, Guilak F, Setton L A. Compressive and shear properties of alginate gel: effects of sodium ions and alginate concentration. Journal of Biomedical Materials Research, 1999, 47(1): 46–53
Rowley J A, Madlambayan G, Mooney D J. Alginate hydrogels as synthetic extracellular matrix materials. Biomaterials, 1999, 20(1): 45–53
Pouyani T, Prestwich G D. Functionalized derivatives of hyaluronic acid oligosaccharides: drug carriers and novel biomaterials. Bioconjugate Chemistry, 1994, 5(4): 339–347
Suri S, Schmidt C E. Cell-laden hydrogel constructs of hyaluronic acid, collagen, and laminin for neural tissue engineering. Tissue Engineering Part A, 2010, 16(5): 1703–1716
Campbell W W. Evaluation and management of peripheral nerve injury. Clinical Neurophysiology, 2008, 119(9): 1951–1965
Papastefanaki F, Chen J, Lavdas A A, et al. Grafts of Schwann cells engineered to express PSA-NCAM promote functional recovery after spinal cord injury. Brain, 2007, 130(8): 2159–2174
Hill C E, Moon L D, Wood P M, et al. Labeled Schwann cell transplantation: cell loss, host Schwann cell replacement, and strategies to enhance survival. Glia, 2006, 53(3): 338–343
Oudega M, Xu X M. Schwann cell transplantation for repair of the adult spinal cord. Journal of Neurotrauma, 2006, 23(3–4): 453–467
Goto E, Mukozawa M, Mori H, et al. A rolled sheet of collagen gel with cultured Schwann cells: model of nerve conduit to enhance neurite growth. Journal of Bioscience and Bioengineering, 2010, 109(5): 512–518
Deng L X, Hu J, Liu N, et al. GDNF modifies reactive astrogliosis allowing robust axonal regeneration through Schwann cell-seeded guidance channels after spinal cord injury. Experimental Neurology, 2011, 229(2): 238–250
Sherman L, Skroch-Angel P, Moll J, et al. Schwann cell tumors express characteristic patterns of CD44 splice variants. Journal of Neuro-Oncology, 1995, 26(3): 171–184
Maharjan A S, Pilling D, Gomer R H. High and low molecular weight hyaluronic acid differentially regulate human fibrocyte differentiation. PLoS ONE, 2011, 6(10): e26078–e26087
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wang, MD., Zhai, P., Schreyer, D.J. et al. Novel crosslinked alginate/hyaluronic acid hydrogels for nerve tissue engineering. Front. Mater. Sci. 7, 269–284 (2013). https://doi.org/10.1007/s11706-013-0211-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11706-013-0211-y