Abstract
Aims
To examine the relationships between type 2 diabetes (T2D) status, glycemic control, and T2D duration with magnetic resonance imaging (MRI)-derived neuroimaging measures in European Americans from the Diabetes Heart Study (DHS) Mind cohort.
Methods
Relationships were examined using marginal models with generalized estimating equations in 784 participants from 514 DHS Mind families. Fasting plasma glucose, glycated hemoglobin, and diabetes duration were analyzed in 682 participants with T2D. Models were adjusted for potential confounders, including age, sex, history of cardiovascular disease, smoking, educational attainment, and use of statins or blood pressure medications. Association was tested with gray and white matter volume, white matter lesion volume, gray matter cerebral blood flow, and white and gray matter fractional anisotropy and mean diffusivity.
Results
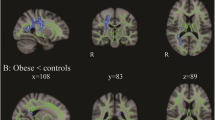
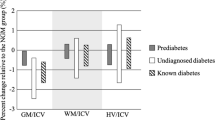
Adjusting for multiple comparisons, T2D status was associated with reduced white matter volume (p = 2.48 × 10−6) and reduced gray and white matter fractional anisotropy (p ≤ 0.001) in fully adjusted models, with a trend toward increased white matter lesion volume (p = 0.008) and increased gray and white matter mean diffusivity (p ≤ 0.031). Among T2D-affected participants, neither fasting glucose, glycated hemoglobin, nor diabetes duration were associated with the neuroimaging measures assessed (p > 0.05).
Conclusions
While T2D was significantly associated with MRI-derived neuroimaging measures, differences in glycemic control in T2D-affected individuals in the DHS Mind study do not appear to significantly contribute to variation in these measures. This supports the idea that the presence or absence of T2D, not fine gradations of glycemic control, may be more significantly associated with age-related changes in the brain.
Similar content being viewed by others
References
Lu F-P, Lin K-P, Kuo H-K (2009) Diabetes and the risk of multi-system aging phenotypes: a systematic review and meta-analysis. PLoS ONE 4(1):e4144. doi:10.1371/journal.pone.0004144
Reijmer Y, van den Berg E, Ruis C, Kappelle L, Biessels G (2010) Cognitive dysfunction in patients with type 2 diabetes. Diabetes/Metab Res Rev 26(7):507–519. doi:10.1002/dmrr.1112
Palta P, Schneider AL, Biessels GJ, Touradji P, Hill-Briggs F (2014) Magnitude of cognitive dysfunction in adults with type 2 diabetes: a meta-analysis of six cognitive domains and the most frequently reported neuropsychological tests within domains. J Int Neuropsychol Soc 20(3):278–291. doi:10.1017/s1355617713001483
Biessels GJ, Reijmer YD (2014) Brain changes underlying cognitive dysfunction in diabetes: what can we learn from MRI? Diabetes 63(7):2244–2252. doi:10.2337/db14-0348
Falvey C, Rosano C, Simonsick E et al (2013) Macro- and microstructural magnetic resonance imaging indices associated with diabetes among community-dwelling older adults. Diabetes Care 36(3):677–682. doi:10.2337/dc12-0814
Moran C, Phan T, Chen J et al (2013) Brain atrophy in type 2 diabetes: regional distribution and influence on cognition. Diabetes Care 36(12):4036–4042. doi:10.2337/dc13-0143
Cukierman-Yaffe T, Gerstein HC, Williamson JD et al (2009) Relationship between baseline glycemic control and cognitive function in individuals with type 2 diabetes and other cardiovascular risk factors: the action to control cardiovascular risk in diabetes-memory in diabetes (ACCORD-MIND) trial. Diabetes Care 32(2):221–226. doi:10.2337/dc08-1153
Geijselaers SL, Sep SJ, Stehouwer CD, Biessels GJ (2014) Glucose regulation, cognition, and brain MRI in type 2 diabetes: a systematic review. Lancet Diabetes Endocrinol. doi:10.1016/s2213-8587(14)70148-2
Yaffe K, Blackwell T, Whitmer R, Krueger K, Barrett-Connor E (2006) Glycosylated hemoglobin level and development of mild cognitive impairment or dementia in older women. J Nutr Health Aging 10(4):292–295
van Elderen S, de Roos A, de Craen A et al (2010) Progression of brain atrophy and cognitive decline in diabetes mellitus: a 3-year follow-up. Neurology 75(11):997–1002. doi:10.1212/WNL.0b013e3181f25f06
Bryan RN, Bilello M, Davatzikos C et al (2014) Effect of diabetes on brain structure: the action to control cardiovascular risk in diabetes MR imaging baseline data. Radiology 272(1):210–216. doi:10.1148/radiol.14131494
Weinstein G, Maillard P, Himali JJ et al (2015) Glucose indices are associated with cognitive and structural brain measures in young adults. Neurology 84(23):2329–2337. doi:10.1212/wnl.0000000000001655
Bowden D, Cox A, Freedman B et al (2010) Review of the Diabetes Heart Study (DHS) family of studies: a comprehensively examined sample for genetic and epidemiological studies of type 2 diabetes and its complications. Rev Diabetic Stud RDS 7(3):188–201. doi:10.1900/rds.2010.7.188
Hugenschmidt C, Hsu F-C, Hayasaka S et al (2013) The influence of subclinical cardiovascular disease and related risk factors on cognition in type 2 diabetes mellitus: the DHS-Mind study. J Diabetes Complications 27(5):422–428. doi:10.1016/j.jdiacomp.2013.04.004
Cox AJ, Hugenschmidt CE, Raffield LM et al (2014) Heritability and genetic association analysis of cognition in the Diabetes Heart Study. Neurobiol Aging 35(8):1953–1958. doi:10.1016/j.neurobiolaging.2014.03.005
Raffield LM, Cox AJ, Hugenschmidt CE et al (2015) Heritability and genetic association analysis of neuroimaging measures in the Diabetes Heart Study. Neurobiol Aging 36(3):1602–1615. doi:10.1016/j.neurobiolaging.2014.11.008
Hsu FC, Raffield LM, Hugenschmidt CE et al (2015) Relationships between cognitive performance, neuroimaging and vascular disease: the DHS-MIND Study. Neuroepidemiology 45(1):1–11. doi:10.1159/000435775
Jenkinson M, Beckmann C, Behrens T, Woolrich M, Smith S (2012) Fsl. Neuroimage 62(2):782–790. doi:10.1016/j.neuroimage.2011.09.015
Maldjian JA, Laurienti PJ, Burdette JH, Kraft RA (2008) Clinical implementation of spin-tag perfusion magnetic resonance imaging. J Comput Assist Tomogr 32(3):403–406. doi:10.1097/RCT.0b013e31816b650b
Schmidt P, Gaser C, Arsic M et al (2012) An automated tool for detection of FLAIR-hyperintense white-matter lesions in multiple sclerosis. Neuroimage 59(4):3774–3783. doi:10.1016/j.neuroimage.2011.11.032
Maldjian J, Whitlow C, Saha B et al (2013) Automated white matter total lesion volume segmentation in diabetes. AJNR Am J Neuroradiol 34(12):2265–2270. doi:10.3174/ajnr.A3590
van Harten B, de Leeuw F-E, Weinstein H, Scheltens P, Biessels G (2006) Brain imaging in patients with diabetes: a systematic review. Diabetes Care 29(11):2539–2548. doi:10.2337/dc06-1637
de Leeuw FE, de Groot JC, Oudkerk M et al (2002) Hypertension and cerebral white matter lesions in a prospective cohort study. Brain 125(Pt 4):765–772. doi:10.1093/brain/125.4.765
Longstreth WT Jr, Arnold AM, Beauchamp NJ Jr et al (2005) Incidence, manifestations, and predictors of worsening white matter on serial cranial magnetic resonance imaging in the elderly: the Cardiovascular Health Study. Stroke 36(1):56–61. doi:10.1161/01.str.0000149625.99732.69
Biessels GJ, Strachan MW, Visseren FL, Kappelle LJ, Whitmer RA (2014) Dementia and cognitive decline in type 2 diabetes and prediabetic stages: towards targeted interventions. Lancet Diabetes Endocrinol 2(3):246–255. doi:10.1016/s2213-8587(13)70088-3
Schmidt R, Launer L, Nilsson L-G et al (2004) Magnetic resonance imaging of the brain in diabetes: the Cardiovascular Determinants of Dementia (CASCADE) Study. Diabetes 53(3):687–692. doi:10.2337/diabetes.53.3.687
Geerlings M, Appelman A, Vincken K et al (2010) Brain volumes and cerebrovascular lesions on MRI in patients with atherosclerotic disease: the SMART-MR Study. Atherosclerosis 210(1):130–136. doi:10.1016/j.atherosclerosis.2009.10.039
Vidal JS, Sigurdsson S, Jonsdottir MK et al (2010) Coronary artery calcium, brain function and structure: the AGES-Reykjavik Study. Stroke 41(5):891–897. doi:10.1161/strokeaha.110.579581
Debette S, Beiser A, Hoffmann U et al (2010) Visceral fat is associated with lower brain volume in healthy middle-aged adults. Ann Neurol 68(2):136–144. doi:10.1002/ana.22062
Verstynen T, Weinstein A, Erickson K, Sheu L, Marsland A, Gianaro P (2013) Competing physiological pathways link individual differences in weight and abdominal adiposity to white matter microstructure. NeuroImage 79:129–137. doi:10.1016/j.neuroimage.2013.04.075
He XS, Wang ZX, Zhu YZ et al (2015) Hyperactivation of working memory-related brain circuits in newly diagnosed middle-aged type 2 diabetics. Acta Diabetol 52(1):133–142. doi:10.1007/s00592-014-0618-7
Acknowledgments
The authors thank the other investigators, the staff, and the Diabetes Heart Study participants for their valuable contributions.
Funding
This study was supported in part by the National Institutes of Health through R01 HL67348, R01 HL092301, R01 NS058700 (to DWB), R01 NS075107 (to BIF, JAM), F32 DK083214-01 (to CEH), and F31 AG044879 (to LMR).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors report no conflicts of interest.
Human and animal rights statement
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Managed by Antonio Secchi.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Raffield, L.M., Cox, A.J., Freedman, B.I. et al. Analysis of the relationships between type 2 diabetes status, glycemic control, and neuroimaging measures in the Diabetes Heart Study Mind. Acta Diabetol 53, 439–447 (2016). https://doi.org/10.1007/s00592-015-0815-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-015-0815-z