Abstract
Aim
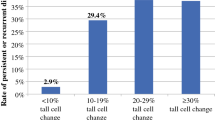
Tall cell variant (TCV) of papillary thyroid carcinoma (PTC) shows a poorer prognosis than conventional PTC. The World Health Organization (WHO) classification defines TCV as the tall cell component (TCC) in ≥50% of PTC lesions. We investigated whether and how the proportion of TCC affects the prognosis of patients with PTC with TCC.
Patients and methods
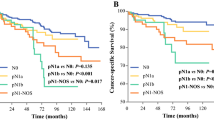
Seventy patients with TCC in ≥30% of their PTC lesions and 210 age- and gender-matched controls with no TCC who underwent locally curative surgery at Kuma Hospital (2006–2014) were enrolled. The 70 PTC patients were divided into two categories: TCC ≥50% (TCC-major, n = 19) and TCC 30–49% (TCC-minor, n = 51). We performed univariate and multivariate analyses of the relationships between disease-free survival (DFS) and variables including the TCC proportion in 276 patients who had no distant metastases at surgery (median follow-up 64 months).
Results
In the univariate analysis, TCC-major, TCC-minor, old age (≥65 years), clinical node metastasis, significant extrathyroid extension (Ex), and high Ki-67 labeling index (≥5%) significantly affected the DFS. In the multivariate analysis, TCC-major and Ex independently affected the DFS, but TCC-minor did not. In an analysis excluding TCC-major patients, TCC-minor was not an independent prognostic factor for DFS.
Conclusions
Studies or larger patient series with longer follow-ups are necessary, but we speculate that in PTC with TCC, TCC-major significantly and independently affects the DFS, whereas TCC-minor does not. Our findings indicate that the WHO definition of TCV is appropriate and that the prognostic impact of TCC-minor is limited.

Similar content being viewed by others
References
Machens A, Hoizhausen HJ, Lautenschlager C et al (2004) The tall-cell variant of papillary thyroid carcinoma: a multivariate analysis of clinical risk factors. Langenbecks Arch Surg 389:278–282
Michels JJ, Jacques M, Henry-Amar M et al (2007) Prevalence and prognostic significance of tall cell variant of papillary thyroid carcinoma. Hum Pathol 38:212–219
Ghossein RA, Leboeuf R, Patel KN et al (2007) Tall cell variant of papillary thyroid carcinoma without extrathyroid extension: biologic behavior and clinical implications. Thyroid 17:655–661
Morris LG, Shaha AR, Tuttle RM et al (2010) Tall-cell variant of papillary thyroid carcinoma: a matched-pair analysis of survival. Thyroid 20:153–158
Jalisi S, Ainsworth T, Lavalley M (2010) Prognostic outcomes of tall cell variant papillary thyroid cancer: a meta-analysis. J Thyroid Res 2010:325602
Regalbuto C, Malandreino P, Frasca F et al (2013) The tall cell variant of papillary thyroid carcinoma: clinical and pathological features and outcomes. J Endocrinol Investig 36:249–254
Dettmer MS, Schmitt A, Steinert H et al (2015) Tall cell papillary thyroid carcinoma: new diagnostic criteria and mutations in BRAF and TERT. Endocr Relat Cancer 22:419–429
Shi X, Liu R, Basolo F et al (2016) Differential clinicopathological risk and prognosis of major papillary thyroid cancer variants. J Clin Endocrinol Metab 101:264–274
DeLeillis RA, Lloyd RV, Heitz PU (eds) (2004) Pathology of tumours of endocrine organs. IARC Press, Lyon
Beninato T, Scognamiglio T, Rleiman DA et al (2013) Ten percent tall cells confer the aggressive features of the tall cell variant of papillary thyroid carcinoma. Surgery 154:1331–1336
Ito Y, Tomoda C, Uruno T et al (2006) Prognostic significance of extrathyroid extension of papillary thyroid carcinoma: massive but not minimal extension affects the relapse-free survival. World J Surg 30:780–786. doi:10.1007/s00268-005-0270-z
Uruno T, Miyauchi A, Shimizu K et al (2005) Usefulness of thyroglobulin measurement in fine-needle aspiration biopsy specimens for diagnosing cervical lymph node metastasis in patients with papillary thyroid cancer. World J Surg 29:483–485. doi:10.1007/s00268-004-7701-0
Ito Y, Hirokawa M, Fukushima M et al (2008) Prevalence and prognostic significance of poor differentiation and tall cell variant in Japan. World J Surg 32:1535–1543. doi:10.1007/s00268-007-9406-7
Ito Y, Kudo T, Kobayashi K et al (2012) Prognostic factors for recurrence of papillary thyroid carcinoma in the lymph nodes, lung, and bone: analysis of 5768 patients with average 10-year follow-up. World J Surg 36:1274–1278. doi:10.1007/s00268-012-1423-5
Ito Y, Miyauchi A, Kakudo K et al (2010) Prognostic significance of Ki-67 labeling index in papillary thyroid carcinoma. World J Surg 34:3015–3021. doi:10.1007/s00268-010-0746-3
Miyauchi A, Kudo T, Hirokawa M et al (2013) Ki-67 labeling index is a predictor of postoperative persistent disease and cancer growth and a prognostic indicator in papillary thyroid carcinoma. Eur Thyroid J 2:57–64
Ito Y, Miyauchi A, Kihara M et al (2014) Patient age is significantly related to the progression of papillary microcarcinoma of the thyroid under observation. Thyroid 24:27–34
Haugen BR, Alexander EK, Bible KC et al (2016) 2015 American Thyroid Association management guidelines for adult patients with thyroid nodules and differentiated thyroid cancer: the American Thyroid Association guidelines task force on thyroid nodules and differentiated thyroid cancer. Thyroid 26:1–133
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ito, Y., Hirokawa, M., Miyauchi, A. et al. Prognostic Significance of the Proportion of Tall Cell Components in Papillary Thyroid Carcinoma. World J Surg 41, 742–747 (2017). https://doi.org/10.1007/s00268-016-3784-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-016-3784-7