Abstract
Introduction and hypothesis
It is commonly believed that pelvic organ prolapse (POP) is associated with cervical elongation. However, cervical lengths have not been formally compared between women with prolapse and those with normal support.
Methods
Cervix and uterine corpus lengths were measured on magnetic resonance images in a case-control study of 51 women with prolapse and 46 women with normal support determined by the Pelvic Organ Prolapse Quantification (POP-Q) examination. Group matching ensured similar demographics in both groups. Ranges for normal cervical lengths were determined from the values in the control group in order to evaluate for cervical elongation amongst women with prolapse.
Results
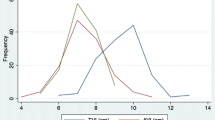
The cervix is 36.4 % (8.6 mm) longer in women with prolapse than in women with normal pelvic support (p < 0.001). Linear regression modeling suggests the feature most highly associated with cervical length is the degree of uterine descent (POP-Q point C). Approximately 40 % of women with prolapse have cervical elongation; 57 % of cervical elongation in prolapse can be explained by a logistic regression-based model including POP-Q point C, body mass index, and menopausal status.
Conclusions
Cervical elongation is found in one third of women with POP, with the extent of elongation increasing with greater degrees of uterine descent.


Similar content being viewed by others
References
Rogers RM, Richardson AC (2003) Clinical evaluation of pelvic support defects with anatomic correlations. In: Bent AE, Ostergard DR, Cundiff GW, Swift SE (eds) Ostergard's urogynecology and pelvic floor dysfunction. Lippincott Williams & Wilkins, Philadephia
Bump RC, Mattiasson A, Bo K, Brubaker LP, DeLancey JO, Klarskov P et al (1996) The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175:10–17
Trowbridge ER, Fultz NH, Patel DA, DeLancey JOL, Fenner DE (2008) Distribution of pelvic organ support measures in a population-based sample of middle-aged, community-dwelling African American and white women in southeastern Michigan. Am J Obstet Gynecol 198:548.e1–548.e6
Tumbarello JA, Hsu Y, Lewicky-Gaupp C, Rohrer S, DeLancey JO (2010) Do repetitive Valsalva maneuvers change maximum prolapse on dynamic MRI? Int Urogynecol J 21:1247–1251
Morgan DM, Umek W, Stein T, Hsu Y, Guire K, DeLancey JO (2007) Interrater reliability of assessing levator ani muscle defects with magnetic resonance images. Int Urogynecol J Pelvic Floor Dysfunct 18:773–778
Merz E, Miric-Tesanic D, Bahlmann F, Weber G, Wellek S (1996) Sonographic size of uterus and ovaries in pre- and postmenopausal women. Ultrasound Obstet Gynecol 7:38–42
Antovska SV (2008) A new modification of the POPQ system—its effectiveness in the diagnosis of supravaginal elongation of the uterine cervix in cases with genital prolapse. Bratisl Lek Listy 109:307–312
Ibeanu OA, Chesson RR, Sandquist D, Perez J, Santiago K, Nolan TE (2010) Hypertrophic cervical elongation: clinical and histological correlations. Int Urogynecol J 21:995–1000
Walters MD (2008) Uterovaginal prolapse in a woman desiring uterine preservation. Int Urogynecol J Pelvic Floor Dysfunct 19:1465, discussion 1465–70
Zucchi A, Lazzeri M, Porena M, Mearini L, Costantini E (2010) Uterus preservation in pelvic organ prolapse surgery. Nat Rev Urol 7:626–633
Rosen DM, Shukla A, Cario GM, Carlton MA, Chou D (2008) Is hysterectomy necessary for laparoscopic pelvic floor repair? A prospective study. J Minim Invasive Gynecol 15:729–734
Karram MM (2011) Vaginal hysterectomy. In: Baggish MS, Karram MM (eds) Atlas of pelvic anatomy and gynecologic surgery. Elsevier Saunders, St. Louis
Diwan A, Rardin CR, Kohli N (2004) Uterine preservation during surgery for uterovaginal prolapse: a review. Int Urogynecol J Pelvic Floor Dysfunct 15:286–292
Tamakawa M, Murakami G, Takashima K, Kato T, Hareyama M (2003) Fascial structures and autonomic nerves in the female pelvis: a study using macroscopic slices and their corresponding histology. Anat Sci Int 78:228–242
Umek WH, Morgan DM, Ashton-Miller JA, DeLancey JO (2004) Quantitative analysis of uterosacral ligament origin and insertion points by magnetic resonance imaging. Obstet Gynecol 103:447–451
Otcenasek M, Baca V, Krofta L, Feyereisl J (2008) Endopelvic fascia in women: shape and relation to parietal pelvic structures. Obstet Gynecol 111:622–630
Vu D, Haylen BT, Tse K, Farnsworth A (2010) Surgical anatomy of the uterosacral ligament. Int Urogynecol J 21:1123–1128
Campeau L, Gorbachinsky I, Badlani GH, Andersson KE (2011) Pelvic floor disorders: linking genetic risk factors to biochemical changes. BJU Int 108:1240–1247
Kerkhof MH, Hendriks L, Brölmann HA (2009) Changes in connective tissue in patients with pelvic organ prolapse—a review of the current literature. Int Urogynecol J Pelvic Floor Dysfunct 20:461–474
Bartoli JM, Moulin G, Delannoy L, Chagnaud C, Kasbarian M (1991) The normal uterus on magnetic resonance imaging and variations associated with the hormonal state. Surg Radiol Anat 13:213–220
Benacerraf BR, Shipp TD, Lyons JG, Bromley B (2010) Width of the normal uterine cavity in premenopausal women and effect of parity. Obstet Gynecol 116:305–310
Londero AP, Bertozzi S, Fruscalzo A, Driul L, Marchesoni D (2011) Ultrasonographic assessment of cervix size and its correlation with female characteristics, pregnancy, BMI, and other anthropometric features. Arch Gynecol Obstet 283:545–550
DeLancey JO, Morgan DM, Fenner DE, Kearney R, Guire K, Miller JM et al (2007) Comparison of levator ani muscle defects and function in women with and without pelvic organ prolapse. Obstet Gynecol 109:295–302
Dietz HP, Simpson JM (2008) Levator trauma is associated with pelvic organ prolapse. BJOG 115:979–984
Acknowledgments
We gratefully acknowledge funding support from NICHD through grant R01 HD 38665 and ORWH through grant P50 HD44406. We thank Mark D. Pearlman, M.D., for critical reading of the manuscript. Preliminary data from this study were presented as a poster at the American Urogynecologic Society 31st Annual Scientific Meeting in Long Beach, CA (September, 2010).
Conflicts of interest
J. O. L. DeLancey receives research support from American Medical Systems, Johnson & Johnson and Kimberly Clark. The authors have no other relevant disclosures.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Berger, M.B., Ramanah, R., Guire, K.E. et al. Is cervical elongation associated with pelvic organ prolapse?. Int Urogynecol J 23, 1095–1103 (2012). https://doi.org/10.1007/s00192-012-1747-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-012-1747-6