Abstract
Introduction and hypothesis
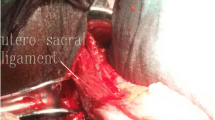
This study aims to elucidate and expand current knowledge of the uterosacral ligament (USL) from a surgical viewpoint.
Methods
Studies were performed on 12 unembalmed cadaveric pelves and five formalin-fixed pelves.
Results
The USL, 12–14-cm long, can be subdivided into three sections: (1) distal (2–3 cm), intermediate (5 cm), and proximal (5–6 cm). The thick (5–20 mm) distal section, attached to cervix and upper vagina, is confluent laterally with the cardinal ligament. The proximal section is diffuse in attachment and generally thinner. The relatively unattached intermediate section is wide, and thick, well defined when placed under tension, more than 2 cm from the ureter and suitable for surgical use. The strength of the USL is perhaps derived not only from the ligament itself, but also from the addition of extraperitoneal connective tissue.
Conclusions
The USL can be subdivided into three sections according to thickness and attachments with the intermediate section suitable for surgical use, particularly for vaginal vault support.






Similar content being viewed by others
References
Miller N (1927) A new method of correcting complete inversion of the vagina: with or without complete prolapse: report of 2 cases. Surg Gynecol Obstet 44:550–555
McCall ML (1957) Posterior culdoplasty: surgical correction of enterocoele during vaginal hysterectomy; a preliminary report. Obstet Gynecol 10:595–602
Jenkins VR 2nd (1997) Uterosacral ligament fixation for vaginal vault suspension in uterine and vaginal vault prolapse. Am J Obstet Gynecol 177:1337–1343
Barber MD, Visco AG, Weidner AC, Amundsen CL, Bump RC (2000) Bilateral uterosacral ligament vaginal vault suspension with site-specific endopelvic fascia defect repair for treatment of pelvic organ prolapse. Am J Obstet Gynecol 183:1402–1410
Shull BL, Bachofen C, Coates KW, Kuehl TJ (2000) A transvaginal approach to repair of apical and other associated sites of pelvic organ prolapse with uterosacral ligaments. Am J Obstet Gynecol 183:1365–1373
Karram M, Goldwasser S, Kleeman S, Steele A, Vassallo B, Walsh P (2001) High uterosacral vaginal vault suspension with fascial reconstruction for vaginal repair of enterocoele and vaginal vault prolapse. Am J Obstet Gynecol 185:1339–1343
Amundsen CL, Flynn BJ, Webster GD (2003) Anatomical correction of vaginal vault prolapse by uterosacral ligament fixation in women who also require a pubovaginal sling. J Urol 169:1770–1774
Silva WA, Pauls RN, Segal JL, Rooney CM, Kleeman SD, Karram MM (2006) Uterosacral ligament vault suspension: five-year outcomes. Obstet Gynecol 108:255–263
Park AJ, Ridgeway B, Gustilo-Ashby AM, Paraiso MFR, Walters MD, Barber MD (2008) Efficacy of a standardized technique of trans-vaginal entry into the peritoneal cavity for post-hysterectomy vaginal vault suspension. Int Urogynecol J 19:1393–1398
Dwyer PL, Fatton B (2008) Bilateral extraperitoneal uterosacral suspension: a new approach to correct posthysterectomy vaginal vault prolapse. Int Urogynecol J 19:283–292
Fatton B, Dwyer PL, Achtari C, Tan PK (2009) Bilateral extraperitoneal uterosacral vaginal vault suspension: a 2 year follow-up longitudinal case series of 123 patients. Int Urogynecol J 20(4):427–434
Haylen BT, Yang V, Vu D, Tse K (2009) Midline uterosacral suspension anterior colporrhaphy combo (MUSSACC): preliminary report. Int Urogynecol J (in press)
Buller JL, Thompson JR, Cundiff GW, Sullivan LK, Schön Ybarra MAS, Bent AE (2001) Uterosacral ligament: description of anatomic relationships to optimize surgical safety. Obstet Gynecol 97(6):873–879
Blaisdell FE (1917) The anatomy of the sacro-uterine ligaments. Anat Rec 12:1–42
Campbell R (1950) The anatomy and histology of the sacrouterine ligaments. Am J Obstet Gynecol 59:1–12
Umek WH, Morgan DM, Ashton-Miller JA, DeLancey JOL (2004) Quantitative analysis of uterosacral ligament origin and insertion points by magnetic resonance imaging. Obstet Gynecol 103(3):447–451
Ramanah R, Parratte B, Arbez-Gindre F, Maillet R, Riethmuller D (2008) The uterosacral complex: ligament or neurovascular pathway? Anatomical and histological study of fetuses and adults. Int Urogynecol J 19:1565–1570
Butler-Manuel SA, Buttery LDK, Polak JM, A’Hern RA, Barton DJP (2008) Autonomic nerve trauma at radical hysterectomy: the nerve content and subtypes within the superficial and deep uterosacral ligaments. Reprod Sci 1:91–96
Siddique SA, Gutman RE, Schön Ybarra MA, Rojas F, Handa VL (2006) Relationship of the uterosacral ligament to the sacral plexus and to the pudendal nerve. Int Urogynecol J 17:642–645
Ercoli A, Delmas V, Fanfani F, Gadonneix P, Ceccaroni M, Fagotti A, Mancuso S, Scambia G (2005) Terminologia Anatomica versus unofficial descriptions and nomenclature of the fasciae and ligaments of the female pelvis: a dissection-based comparative study. Am J Obstet Gynecol 193:1565–1573
Yabuki Y, Sasaki H, Hatakeyama N, Murakami G (2005) Discrepancies between classic anatomy and modern gynecologic surgery on pelvic connective tissue structure: harmonisation of those concepts by collaborative cadaver dissection. Am J Obstet Gynecol 193:7–15
DeCherney AH, Nathan L, Goodwin TM, Laufer N (2006) Current obstetrics and gynecologic diagnosis and treatment, 10th edn. McGraw-Hill Medical, New York, p 46
Otcenasek M, Baca V, Ladislaw K, Jaroslaw F (2008) Endopelvic fascia in women. Obstet Gynecol 111:620–630
Cole EE, Leu PB, Gomelsky A, Revelo P, Shappell H, Scarpero HM, Dmochowski RR (2006) Histopathological evaluation of the uterosacral ligament: is this a dependable structure for pelvic reconstruction? BJU Int 97(2):345–348
Butler-Manuel SA, Buttery LDK, A’Hern RP, Polak JM, Barton DPJ (2000) Pelvic nerve plexus trauma at radical hysterectomy and simple hysterectomy. Cancer 89(4):834–841
Tong XK, Huo RJ (1991) The anatomical basis and prevention of neurogenic voiding dysfunction following radical hysterectomy. Surg Radiol Anat 13(2):145–148
Maas CP, Trimbos JB, DeRuiter MC, van de Velde CJH, Kenter GG (2003) Nerve sparing radical hysterectomy: latest developments and historical perspective. Crit Rev Oncol Hematol 48:271–279
Trimbos JB, Maas CP, DeRuiter MC, Peters AAW, Kenter GG (2001) A nerve-sparing radical hysterectomy: guidelines and feasibility in western patients. Int J Gynecol Cancer 11:180–186
Wieslander CK, Roshanravan SM, Wai CY et al (2007) Uterosacral ligament suspension sutures: anatomic relations in unembalmed female cadavers. Am J Obstet Gynecol 197:672e1–672e6
Fritsch H, Lienemann A, Brenner E, Ludwikowski B (2004) Clinical anatomy of the pelvic floor. Adv Anat Embryo Cell Biol 175(III–IX):1–64
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vu, D., Haylen, B.T., Tse, K. et al. Surgical anatomy of the uterosacral ligament. Int Urogynecol J 21, 1123–1128 (2010). https://doi.org/10.1007/s00192-010-1147-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-010-1147-8