Abstract
Background
Although patellar instability can be treated with several surgical procedures, the appropriate surgical treatment for patellar instability with patella alta has not yet been investigated. The objective of this study is to find out whether three-dimensional transfer of the tibial tuberosity elicits good knee functionality with improved patella alta and prevents further patellar dislocation.
Methods
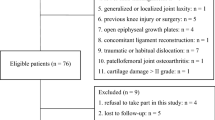
Twelve knees (10 patients) underwent surgery for patellar instability with patella alta from 2007 to 2011. The surgery performed was a three-dimensional transfer for the anteromedial distalization of the tibial tuberosity. Predisposing anatomical factors for patellar instability were evaluated preoperatively; femorotibial angle (FTA), patella alta (IS ratio), trochlear dysplasia (sulcus angle) and tilting angle (lateral tilt). The function of the knee was assessed before and after surgery by Lysholm and Kujala score.
Results
Before surgery, the IS ratio was 1.34 ± 0.13, lateral tilt was 22.4° ± 6.5°, and the sulcus angle was 151.7° ± 8.3°, indicating patella alta, laterality, and trochlear dysplasia. After surgery, the IS ratio and lateral tilt significantly improved to 0.95 ± 0.13, and 10.6° ± 3.4°, respectively. FTA and sulcus angle were not altered. Lysholm and Kujala score improved from 63.8 to 94.7 and 67.0 to 94.1 points, respectively. Most patients displayed good outcomes except for one patient who suffered re-dislocation by hitting their knee on the floor, 2.5 years after surgery.
Conclusion
Three-dimensional tibial tuberosity transfer was shown to correct the patella position and result in a good clinical outcome. This method is introduced as an alternative surgery for patellar instability with patella alta.



Similar content being viewed by others
References
Panni AS, Cerciello S, Maffulli N, Di Cesare M, Servien E, Neyret P. Patellar shape can be a predisposing factor in patellar instability. Knee Surg Sports Traumatol Arthrosc. 2011;19:663–70.
Ward SR, Terk MR, Powers CM. Patella alta: association with patellofemoral alignment and changes in contact area during weight-bearing. J Bone Joint Surg Am. 2007;89:1749–55.
Juliusson R, Markhede G. A modified Hauser procedure for recurrent dislocation of the patella. A long-term follow-up study with special reference to osteoarthritis. Arch Orthop Trauma Surg. 1984;103:42–6.
Laurin CA, Lévesque HP, Dussault R, Labelle H, Peides JP. The abnormal lateral patellofemoral angle: a diagnostic roentgenographic sign of recurrent patellar subluxation. J Bone Joint Surg Am. 1978;60:55–60.
Balcarek P, Jung K, Ammon J, Walde TA, Frosch S, Schüttrumpf JP, Stürmer KM, Frosch KH. Anatomy of lateral patellar instability: trochlear dysplasia and tibial tubercle–trochlear groove distance is more pronounced in women who dislocate the patella. Am J Sports Med. 2010;38:2320–7.
Servien E, Verdonk PC, Neyret P. Tibial tuberosity transfer for episodic patellar dislocation. Sports Med Arthrosc. 2007;15:61–7.
Monk AP, Doll HA, Gibbons CLMH, Ostlere S, Beard DJ, Gill HS, Murray DW. The patho-anatomy of patellofemoral subluxation. J Bone Joint Surg Br. 2011;93:1341–7.
Hauser EDW. Total tendon transplant for slipping patella: a new operation for recurrent dislocation of the patella. 1938. Clin Orthop Relat Res. 2006;452:7–16.
Cox JS. Evaluation of the Roux-Elmslie-Trillat procedure for knee extensor realignment. Am J Sports Med. 1982;10:303–10.
Fulkerson JP. Anteromedialization of the tibial tuberosity for patellofemoral malalignment. Clin Orthop Relat Res. 1983;177:176–81.
Endres S, Wilke A. A 10 year follow-up study after Roux-Elmslie-Trillat treatment for cases of patellar instability. BMC Musculoskelet Disord. 2011;12:48.
Akgün U, Nuran R, Karahan M. Modified Fulkerson osteotomy in recurrent patellofemoral dislocations. Acta Orthop Traumatol Turc. 2010;44:27–35.
Nakagawa K, Wada Y, Minamide M, Tsuchiya A, Moriya H. Deterioration of long-term clinical results after the Elmslie-Trillat procedure for dislocation of the patella. J Bone Joint Surg Br. 2002;84:861–4.
Hampson WG, Hill P. Late results of transfer of the tibial tubercle for recurrent dislocation of the patella. J Bone Joint Surg Br. 1975;57:209–13.
Nomura E. Classification of lesions of the medial patello-femoral ligament in patellar dislocation. Int Orthop. 1999;23:260–3.
Nomura E, Inoue M, Kobayashi S. Long-term follow-up and knee osteoarthritis change after medial patellofemoral ligament reconstruction for recurrent patellar dislocation. Am J Sports Med. 2007;35:1851–8.
Ellera Gomes JL. Medial patellofemoral ligament reconstruction for recurrent dislocation of the patella: a preliminary report. YJARS. 1992;8:335–40.
Wagner D, Pfalzer F, Hingelbaum S, Huth J, Mauch F, Bauer G. The influence of risk factors on clinical outcomes following anatomical medial patellofemoral ligament (MPFL) reconstruction using the gracilis tendon. Knee Surg Sports Traumatol Arthrosc. (Published Online First: 27 April 2012).
Arendt EA, Moeller A, Agel J. Clinical outcomes of medial patellofemoral ligament repair in recurrent (chronic) lateral patella dislocations. Knee Surg Sports Traumatol Arthrosc. 2011;19:1909–14.
Insall J, Salvati E. Patella position in the normal knee joint. Radiology. 1971;101:101–4.
Luyckx T, Didden K, Vandenneucker H, Labey L, Innocenti B, Bellemans J. Is there a biomechanical explanation for anterior knee pain in patients with patella alta? Influence of patellar height on patellofemoral contact force, contact area and contact pressure. J Bone Joint Surg Br. 2009;91:344–50.
Redziniak DE, Diduch DR, Mihalko WM, Fulkerson JP, Novicoff WM, Sheibani-Rad S, Saleh KJ. Patellar instability. J Bone Joint Surg Am. 2009;91:2264–75.
Ahlbäck S, Mattsson S. Patella alta and gonarthrosis. Acta Radiol Diagn (Stockh). 1978;19:578–84.
Stefanik JJ, Zhu Y, Zumwalt AC, Gross KD, Clancy M, Lynch JA, Frey Law LA, Lewis CE, Roemer FW, Powers CM, Guermazi A, Felson DT. Association between patella alta and the prevalence and worsening of structural features of patellofemoral joint osteoarthritis: the multicenter osteoarthritis study. Arthritis Care Res (Hoboken). 2010;62:1258–65.
Merchant AC, Mercer RL, Jacobsen RH, Cool CR. Roentgenographic analysis of patellofemoral congruence. J Bone Joint Surg Am. 1974;56:1391–6.
Laurin CA, Dussault R, Lévesque HP. The tangential X-ray investigation of the patellofemoral joint: X-ray technique, diagnostic criteria and their interpretation. Clin Orthop Relat Res. 1979;144:16–26.
Kujala UM, Jaakkola LH, Koskinen SK, Taimela S, Hurme M, Nelimarkka O. Scoring of patellofemoral disorders. YJARS. 1993;9:159–63.
Bollier M, Fulkerson J, Cosgarea A, Tanaka M. Technical failure of medial patellofemoral ligament reconstruction. YJARS. 2011;27:1153–9.
Arendt EA. MPFL reconstruction for PF instability. The soft (tissue) approach. Orthop Traumatol Surg Res. 2009;95:97–100.
Barber FA, McGarry JE. Elmslie–Trillat procedure for the treatment of recurrent patellar instability. Arthrosc J Arthrosc Relat Surg. 2008;24:77–81.
Rillmann P, Dutly A, Kieser C, Berbig R. Modified Elmslie-Trillat procedure for instability of the patella. Knee Surg Sports Traumatol Arthrosc. 1998;6:31–5.
Tsuda E, Ishibashi Y, Yamamoto Y, Maeda S. Incidence and radiologic predictor of postoperative patellar instability after Fulkerson procedure of the tibial tuberosity for recurrent patellar dislocation. Knee Surg Sports Traumatol Arthrosc. 2012;20:2058–66.
Nietosvaara Y, Paukku R, Palmu S, Donell ST. Acute patellar dislocation in children and adolescents. Surgical technique. J Bone Joint Surg Am. 2009;91(Suppl 2 Pt 1):139–45.
Conflict of interest
The authors have no conflicts of interest in the authorship and publication of this contribution.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Otsuki, S., Nakajima, M., Oda, S. et al. Three-dimensional transfer of the tibial tuberosity for patellar instability with patella alta. J Orthop Sci 18, 437–442 (2013). https://doi.org/10.1007/s00776-013-0364-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00776-013-0364-7