Abstract
Background: Ultrasonography and fine-needle aspiration (FNA) are used to evaluate the breast and regional nodes in breast cancer patients. We sought to identify factors influencing the sensitivity of ultrasonography for detection of nodal metastasis.
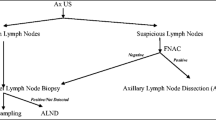
Methods: Patients with a clinically negative axilla who underwent axillary ultrasonography and sentinel lymph node biopsy were included.
Results: Of 208 patients, axillary ultrasonography was negative in 180 (86%) and suspicious or indeterminate in 28 (14%). FNA was performed in 22 patients whose findings were indeterminate or suspicious, and 3 were positive for malignancy. Final pathological examinations revealed positive nodes in 53 patients: 39 (22%) of 180 with negative ultrasonographic findings and 14 (50%) of 28 with indeterminate or suspicious ultrasonographic findings (P = .001). Excisional biopsy was more common for patients with indeterminate or suspicious findings on preoperative ultrasonography (P = .038). There were no significant differences in tumor size, histological features, size of nodal metastasis, or number of positive nodes between patients whose ultrasonography findings were negative and those whose findings were indeterminate or suspicious.
Conclusions: Ultrasonographically suggested nodal metastasis is associated with the finding of nodal disease on final pathological examination. No significant clinicopathologic criteria were found to impact sensitivity of ultrasonography; however, excisional biopsy for diagnosis may be a confounding variable in subsequent axillary ultrasonography.
Similar content being viewed by others
REFERENCES
Herrada J, Iyer RB, Atkinson EN, et al. Relative value of physical examination, mammography, and breast sonography in evaluating the size of the primary tumor and regional lymph node metastases in women receiving neoadjuvant chemotherapy for locally advanced breast carcinoma. Clin Cancer Res 1997;3:1565–9.
de Kanter AY, van Eijck CH, van Geel AN, et al. Multicentre study of ultrasonographically guided axillary node biopsy in patients with breast cancer. Br J Surg 1999;86:1459–62.
Albo D, Wayne JD, Hunt KK, et al. Anaphylactic reactions to isosulfan blue dye during sentinel lymph node biopsy for breast cancer. Am J Surg 2001;182:393–8.
Montgomery LL, Thorne AC, Van Zee KJ, et al. Isosulfan blue dye reactions during sentinel lymph node mapping for breast cancer. Anesth Analg 2002;95:385–8.
Vlastos G, Fornage BD, Mirza NQ, et al. The correlation of axillary ultrasonography with histologic breast cancer downstaging after induction chemotherapy. Am J Surg 2000;179:446–52.
de Freitas R Jr, Costa M, Schneider S, et al. Accuracy of ultrasound and clinical examination in the diagnosis of axillary lymph node metastasis in breast cancer. Eur J Surg Oncol 1991;17:240–4.
Bonnema J, van Geel AN, van Ooijen B, et al. Ultrasound-guided aspiration biopsy for detection of non-palpable axillary node metastasis in breast cancer patients: new diagnostic method. World J Surg 1997;21:270–4.
Motomura K, Inaji H, Komoike Y, et al. Gamma probe and ultrasonographically-guided fine needle aspiration biopsy of sentinel lymph nodes in breast cancer patients. Eur J Surg Oncol 2001;27:141–5.
Walsh J, Dixon J, Chetty U, Paterson D. Colour Doppler studies of axillary node metastasis in breast carcinoma. Clin Radiol 1994;49:189–91.
Yang W, Ahuja A, Tang A, et al. High resolution sonographic detection of axillary lymph node metastasis in breast cancer. J Ultrasound Med 1996;15:241–6.
Krishnamurthy R, Bedi D, Krishnamurthy S. Ultrasound of axillary lymph nodes: classification based on cortical morphology. Radiology 2001;221(P):646.
Motomura K, Inaji H, Komoike Y, et al. Intraoperative sentinel lymph node examination by imprint cytology and frozen sectioning during breast surgery. Br J Surg 2000;87:597–601.
Kane JM 3rd, Edge SB, Winston JS, et al. Intraoperative pathologic evaluation of a breast cancer sentinel lymph node biopsy as a determinant for synchronous axillary lymph node dissection. Ann Surg Oncol 2001;8:361–7.
Zurrida S, Mazzarol G, Galimberti V, et al. The problem of the accuracy of intraoperative examination of axillary sentinel nodes in breast cancer. Ann Surg Oncol 2001;8:817–20.
Chao C, Wong SL, Ackermann D, et al. Utility of intraoperative frozen section analysis of sentinel lymph nodes in breast cancer. Am J Surg 2001;182:609–15.
Dixon JM, Mamman U, Thomas J. Accuracy of intraoperative frozen-section analysis of axillary nodes. Edinburgh Breast Unit team. Br J Surg 1999;86:392–5.
Henry-Tillman RS, Korourian S, Rubio IT, et al. Intraoperative touch preparation for sentinel lymph node biopsy: a 4-year experience. Ann Surg Oncol 2002;9:333–9.
Sacre RA. Clinical evaluation of axillary lymph nodes compared to surgical and pathological findings. Eur J Surg Oncol 1986;12:169–73.
Pamilo M, Soiva M, Lavast EM. Real-time ultrasound, axillary mammography, and clinical examination in the detection of axillary lymph node metastases in breast cancer patients. J Ultrasound Med 1989;8:115–20.
Ohta M, Tokuda Y, Saitoh Y, et al. Comparative efficacy of positron emission tomography and ultrasonography in preoperative evaluation of axillary lymph node metastases in breast cancer. Breast Cancer 2000;7:99–103.
Murray AD, Staff RT, Redpath TW, et al. Dynamic contrast enhanced MRI of the axilla in women with breast cancer: comparison with pathology of excised nodes. Br J Radiol 2002;75:220–8.
Feu J, Tresserra F, Fabregas R, et al. Metastatic breast carcinoma in axillary lymph nodes: in vitro US detection. Radiology 1997;205:831–5.
Vaidya JS, Vyas JJ, Thakur MH, et al. Role of ultrasonography to detect axillary node involvement in operable breast cancer. Eur J Surg Oncol 1996;22:140–3.
Verbanck J, Vandewiele I, De Winter H, et al. Value of axillary ultrasonography and sonographically guided puncture of axillary nodes: a prospective study in 144 consecutive patients. J Clin Ultrasound 1997;25:53–6.
Krishnamurthy S, Sneige N, Bedi DG, et al. Role of ultrasound-guided fine-needle aspiration of indeterminate and suspicious axillary lymph nodes in the initial staging of breast carcinoma. Cancer 2002;95:982–8.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bedrosian, I., Bedi, D., Kuerer, H.M. et al. Impact of Clinicopathological Factors on Sensitivity of Axillary Ultrasonography in the Detection of Axillary Nodal Metastases in Patients With Breast Cancer. Ann Surg Oncol 10, 1025–1030 (2003). https://doi.org/10.1245/ASO.2003.12.017
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1245/ASO.2003.12.017