Abstract
Premature infants often develop serious clinical complications associated with respiratory failure and hyperoxic lung injury that includes lung inflammation and alterations in lung development. The goal of these studies is to test the hypothesis that there are differences in the course of lung injury in newborn mice exposed to 85% or >95% oxygen that provide models to address the differential effects of oxidation and inflammation. Our results indicate differences between the 85% and >95% O2 exposure groups by day 14 in weight gain and lung alveolarization. Inflammation, assessed by neutrophil counts, was observed in both hyperoxia groups by day 3 but was dramatically greater in the >95% O2-exposed groups by day 14 and associated with greater developmental deficits. Cytoplasmic phospholipase A2, cyclooxygenase-2, and 5-lipoxygenase levels were elevated but no patterns of differences were observed between exposure groups. Prostaglandins D2, E2, and F2α were increased in the tissues from mouse pups exposed to >95% O2 at 7 d indicating a differential expression of cyclooxygenase-2 products. Our data indicate that there are differences in the models of 85% or >95% O2 exposure and these differences may provide mechanistic insights into hyperoxic lung injury in an immature system.
Similar content being viewed by others
Main
The development of bronchopulmonary dysplasia (BPD), a form of chronic lung disease associated with prematurity, occurs in immature lungs on exposure to supplemental oxygen, mechanical ventilation, and inflammatory cell infiltration. The structural and biochemical changes that occur during exposure to hyperoxia are well-described in animal models (1–6).
Mice pups are born in the saccular stage of lung development and decreased alveolarization is a prevalent characteristic in mouse pups exposed to hyperoxia during the early postnatal period. Previous studies using 85% and >95% O2 exposures have reported disruption of key growth events and aberrant alveolarization that may lead to permanent deficits in lung growth (7–9) but comparative studies have not been reported. Neonatal mice often succumb to >95% O2 with robust inflammatory responses, whereas models using <90% O2 have demonstrated less inflammation and limited lethality (7). It is possible that the different outcomes in these types of studies are related to more exaggerated lung inflammation in newborn mice exposed to >95% oxygen than in newborn mice exposed to <90% oxygen, and our hypothesis is that the differences in lung inflammatory responses between these two models are related to differences in the formation of lipid inflammatory mediators.
The lung has large quantities of cellular membrane glycerophospholipids which contain esterified arachidonic acid and provide a source for the formation of biologically active arachidonic acid metabolites or eicosanoids (10). Phospholipases are responsible for cleavage of esterified fatty acids from membrane phospholipids. Cyclooxygenases (COX) form prostaglandins (PG) and thromboxanes (TBX), which have potent inflammatory and vasoconstrictive properties. Lipoxygenases (LO) produce hydroxyeicosatetraenoic acids (HETE) that may function as precursors for other biologically active lipid products or as ligands for receptors. 5-LO is specifically responsible for leukotriene (LT) formation and often associated with neutrophil chemotaxis (Fig. 1).
The goal of these studies is to test the hypothesis that differences in the course of injury in newborn mice exposed to 85% and >95% oxygen exist and provide distinctly different models to address developmental deficits associated with hyperoxic lung injury (85% O2) separate from the additive effects of inflammation and developmental deficits associated with >95% O2. Furthermore, these studies test the hypothesis that the differences observed between 85% and >95% O2 exposure are in part due to activation of pro-inflammatory lipid mediators. Careful temporal analyses of hyperoxia exposure in newborn pups may provide clues that lead to the design of new interventions for treatment in premature infants.
METHODS
Animal models.
Animal study protocols were approved by the IACUC at Columbus Children's Research Institute. Pups were randomized and equally distributed between two pregnant C3H/HeN dams delivering within 12 h. One dam and litter was placed in a Plexiglas chamber containing a 10 L/min flow of 85% or >95% (daily average 98%) O2 while the corresponding dam and litter was placed in room air (RA). Twenty-four hours of hyperoxia exposure was designated as day 1. On 1, 3, 7, or 14 d of life, the pups were euthanized by intraperitoneal injections of 200 mg/kg of sodium pentobarbital and the tissues harvested.
Morphometric and digital image analysis.
Morphometric analyses were performed as described by Park et al. (8). The following parameters were determined: number of complete terminal airways per field of view; average terminal airway area; and average terminal airway perimeter using Image J, version 1.37 software (National Institutes of Health, http://rsbweb.nih.gov/ij). Manual measurements are made from the numbers of secondary crests per image and the septal thicknesses. Septal thickness was assessed by linear measurements of the septum at a 90° angle, using at least five random measurements per field, and five fields per slide (animal).
Immunohistochemistry for neutrophil quantification.
Neutrophil counts were performed on paraffin embedded, anti-neutrophil stained mouse tissues. The primary antibody was rat anti-mouse neutrophils (Serotec, Kingston, UK) at a dilution of 1:2500 and secondary antibody was rabbit anti-rat, mouse adsorbed (vector, catalog BA-4001) at a dilution of 1:200. The slides were then counterstained with Richard Allen hematoxylin.
Western blots.
Frozen lung tissues were homogenized and proteins (25–50 μg) were separated by 12% sodium dodecyl sulfate-polyacrylamide gel electrophoresis (Invitrogen, Carlsbad, CA) and transferred to polyvinylidene difluoride membranes. Membranes were probed with antibodies to cytoplasmic phospholipase A2 (cPLA2; rabbit anti-mouse, 1:1000, Cell Signaling, Danvers, MA), COX-2 (rabbit anti-mouse, 1:200, Abcam, Cambridge, MA), or 5-LO (mouse monoclonal, 1:1000, BD Bioscience, San Jose, CA) and the appropriate secondary antibody, anti-rabbit (1:10,000, BioRad, Hercules, CA) or anti-mouse (1:15,000, BioRad). Blots were assessed with ECL detection and expression levels were quantitated by densitometry using Image Quant software, version 5.0 (Molecular Dynamics). The density of the band for the protein of interest was normalized to the density of β-actin protein (mouse monoclonal 1:5,000, Abcam; goat anti-mouse, 1:15,000, BioRad).
LC/MS/MS lipid analysis.
Lung tissues were homogenized and each sample was spiked with an internal standard solution (deuterated standards from each lipid group) then extracted using the Bligh-Dyer technique. Eicosanoids were analyzed by LC/MS/MS on an Applied Biosystems 4000 QTrap equipped with a Shimadzu high performance liquid chromatography. Separation was achieved using a Zorbax SB-C18 column, a flow rate of 0.3 mL/min, and a gradient of 8.3 mM acetic acid, pH 5.7 (mobile phase A), and acetonitrile:2-propanol (50:50) (mobile phase B) as follows: 3 min hold at 15% B, 10 min linear to 55% B, 15 min linear to 80% B. The samples are analyzed in negative ionization mode using multiple reaction monitoring. Individual calibration curves are generated for each group of analytes, and sample concentrations are calculated using isotope dilution corrections.
Statistics.
Data collected from analyses was analyzed by two-way ANOVA with time and exposure as independent variables. Individual differences were detected using modified t tests post hoc with p < 0.05 as significant. All analyses were performed with SPSS windows version 15.0 (Chicago, IL).
RESULTS
Mouse pups exposed to 85% or >95% O2 grew more slowly (Fig. 2) and exhibited less lung alveolarization (Fig. 3A and B) than did their respective RA exposed littermates. By day 7, pups in both hyperoxia-exposed groups weighed less than the pups in the RA control group and but by day 14 the weights of the mice in the 85% O2-exposed group were greater than the >95% O2-exposed group but still less than the RA controls. Those pups exposed to 85% O2 exhibited a lag in growth in the 1–7 d period but grew at the same rate as the RA-exposed animals during the 7–14 d period. Those pups exposed to >95% O2 did not demonstrate an early growth delay (days 1–3) but a growth delay was obvious at 7 and 14 d. No mortality was observed at 14 d.
Effects of 85% (▴) or >95% O2 (•) or room air (▪) on body weight in newborn mice. Pups were treated as described in Methods. Results are reported as mean ± SD. Data were assessed by two-way ANOVA, with modified t test post hoc. An effect of day, an exposure, and an interaction were noted, p < 0.05, n = 5–32. *difference between RA and O2-exposed animals on the same day, §different from day 1 same treatment, ¶difference between 85% and >95% O2 same day.
A, Histology of mouse pup lung tissues exposed to 85% or >95% O2, or RA. Pups were treated as described in Methods section and fixed lung tissues were stained with H&E using standard procedures (100×). No differences were noted at days 1 and 3 (not shown) but by days 7 or 14, changes in lung structure were evident and quantitative assessments of the changes are demonstrated in Figure 2. B, Morphometric analyses of lung tissue samples obtained from mouse pups exposed to 85% (Δ) or >95% O2 (•) or RA (▪). Number of air spaces (1), number of secondary crests (2), airspace area (3), airspace perimeters (4), and septal thicknesses (5) were measured. Each data point represents tissues taken from three individual animals and at least five fields per slide were measured and averaged. Data were expressed as mean ± SD and assessed by two-way ANOVA with modified t test post hoc. An effect of exposure and an interaction were identified in number of alveoli, alveolar area, and alveolar perimeter, an effect of day, exposure, and an interaction were identified in number of alveolar crests and septal thickness. *difference between RA and O2-exposed animals on the same day, §different from day 1 same treatment, ¶difference between 85% and >95% O2 same day.
Histologic analyses of lung tissue sections obtained from pups exposed to 85%, >95%, and RA indicated decreased alveolarization at 7 and 14 d in pups exposed to hyperoxia (Fig. 3A). Morphometric measurements of the histologic sections demonstrated specific deficits in lung growth in the pups exposed to hyperoxia (Fig. 3B). In the RA controls, the number of terminal airspaces or alveoli (Fig. 3B1) and secondary crests (Fig. 3B2) increased, whereas terminal airspace area (Fig. 3B3), perimeter (Fig. 3B4), and septal thickness (Fig. 3B5) decreased through the first 14 d of life. Both hyperoxia-exposed groups had larger terminal airspace area and fewer secondary crests by 3 d of exposure and lower terminal airspace number and larger perimeters by 7 d than the corresponding RA group. Differences in analyzed morphometric perimeters of pup tissues exposed to 85% and >95% O2 became evident between 7 and 14 d with the 85% exposure group demonstrating more secondary crests and less alveolar area and smaller perimeters by 14 d. Septal thickness was greater in the 85% O2-exposed pups at all times than in the RA controls. Septal thickness decreased in the RA animals from day 7–14. Pups exposed to >95% O2 had septal thickness similar to RA controls until day 14 when septal thickness was significantly greater in >95% O2-exposed group than in RA group.
As an assessment of inflammation, lung sections were stained with an antineutrophil antibody and number of neutrophils per high power field was counted. At day 3 and 7, there were more neutrophils in the lungs of the pups exposed to 85% or >95% O2 than in the lungs of pups that remained in RA. By day 14 there were no changes in the number of neutrophils between the RA and the 85% O2 groups, but those pups exposed to >95% O2 had substantially higher numbers of neutrophils present in their lung tissues (Fig. 4).
Neutrophil accumulation in lung tissues of mice pups exposed 85% (▴) or >95% O2 (•), or RA (▪). Pups were treated as described in Methods section and fixed lung tissues were stained with anti-neutrophil antibodies. Four high power fields were counted for each section and three animals per treatment group. Graphs indicate mean ± SD. Data were analyzed by two-way ANOVA with modified t test post hoc. An effect of day and exposure and an interaction were observed. *difference between RA and O2-exposed animals on the same day, §different from day 1 same treatment, ¶difference between 85% and >95% O2 same day.
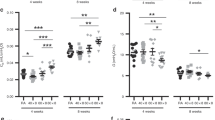
cPLA2 protein levels were not different among groups for days 1 and 3 but were greater in lung tissues after 7 d exposure to 85% or >95% O2 than in RA controls (Fig. 5). Interestingly, the higher levels of cPLA2 protein were maintained through 14 d in the >95% O2-exposed pup tissues but the levels of cPLA2 in the 85% O2-exposed pup tissues were less than the >95% O2-exposed tissues and not different from RA at 14 d.
cPLA2 levels in lung tissues of mouse pups exposed to 85% (□) or >95% O2 (▪), or RA (□). Pups were treated as described in Methods section and proteins were quantitated by Western blot. cPLA2 band intensity was normalized to β-actin, and the ratios were analyzed by two-way ANOVA with modified t test post hoc. Graphs indicate mean ± SD, n = 5–18. An effect of exposure and an interaction were observed. *difference between RA and O2-exposed animals on the same day, §different from day 1 same treatment, ¶difference between 85% and >95% O2 same day.
COX-2 levels were similar in all treatment groups at days 1 and 3 but COX-2 levels were greater in lung tissues of mouse pups exposed to 85% or >95% O2 for 7 or 14 d than in the corresponding RA controls (Fig. 6). The hyperoxia-induced increases in COX-2 levels were equivalent in both 85% and 95% O2-exposed pup tissues.
COX-2 levels in lung tissues of mouse pups exposed to 85% (□) or >95% O2 (▪), or RA (□). Pups were treated as described in Methods section and proteins were quantitated by Western blot. COX-2 band intensity was normalized to β-actin, and the ratios were analyzed by two-way ANOVA with modified t test post hoc. Graphs indicate mean ± SD, n = 5–18. An effect of exposure and an effect of day were observed. *difference between RA and O2-exposed animals on the same day, §different from day 1 same treatment, ¶difference between 85% and >95% O2 same day.
Similar to COX-2, 5-LO levels were not different among groups at days 1 and 3. However, at day 7, the 5-LO levels of tissues from pups exposed to 85% O2 were similar to control levels but the levels in the lung tissues of >95% O2-exposed pups were greater than RA controls or the 85% O2 groups (Fig. 7). By day 14, lung tissues from both O2-exposed groups indicated substantially greater 5-LO levels than the RA day 14 group.
5-LO levels in lung tissues of mouse pups exposed to 85% (□) or >95% O2 (▪), or RA (□). Pups were treated as described in Methods section and proteins were quantitated by Western blot. 5-LO band intensity was normalized to β-actin, and the ratios were analyzed by two-way ANOVA with modified t test post hoc. Graphs indicate mean ± SD, n = 5–18. An effect of exposure, an effect of day, and an interaction between day and exposure were observed. *difference between RA and O2-exposed animals on the same day, §different from day 1 same treatment, ¶difference between 85% and >95% O2 same day.
Metabolites of the COX-2 pathways, PGD2, PGE2, PGF2α, and TBXB2 were measured as evidence of COX-2 enzymatic activity (Table 1). At days 1 and 3 there was a trend toward higher levels of COX-2 metabolites in the 85% O2-exposed pup tissues than in RA or >95% O2 tissues, but this trend was not significant in most cases. However, a robust elevation was observed at 7 d in the tissues obtained from pups exposed to >95% O2 that was not observed in the 85% O2-exposed group. At 14 d, the PGD2 levels were elevated in both the 85% O2 and the >95% O2 groups. Interestingly, the elevated levels of PGE2 and PGF2α did not persist in the lungs of pup exposed to 85% or >95% O2 for 14 d of exposure. On the other hand, TBXB2 demonstrated a modest developmental increase and a slight elevation above control levels at day 7 in the >95% O2-exposed group.
In spite of increases in 5-LO protein levels, no appreciable differences in 5-HETE levels were observed among treatment groups. LTB4, LTC4, LTD4, and LTE4 levels were measured in the pup lung tissues but were not consistently above the limits of detection for the methods described.
DISCUSSION
The goal of these studies was to identify distinct differences in the course of injury in newborn mice exposed to 85% or >95% O2. Detrimental effects of hyperoxic exposure were easily observable in newborn animals as deficits in overall body growth and these effects were different depending on the oxygen concentration (Fig. 2). Growth deficits have been reported in several animal models exposed to a variety of O2 concentrations (6,11,12). Although other studies have observed substantial mortality at earlier time points and lower O2 concentrations (7), no mortality was observed in these studies. These differences in mortality are likely attributable to the decreased susceptibility of the C3H/HeN mouse strain to hyperoxic injury. The apparent resumption of growth in the 85% O2-exposed pups after 7 d may indicate a time frame for the development of resolution or adaptive mechanisms.
Interestingly, both hyperoxia-exposed groups demonstrated evidence of arrested lung development as early as 3 d of exposure. This finding would support the theory that the initiating effects of hyperoxic exposure on lung growth occur very early in the time course before other physiologic parameters are evident but coinciding with the first evidence of neutrophil infiltration. However, the differential responses between the hyperoxia-treated groups occur later during the second week of exposure, and suggest adaptive responses in the mice exposed to 85% O2 (Fig. 3B) but greater inflammatory responses in the mice exposed to >95% oxygen (Fig. 4). These models may be relevant to human premature infants in that pronounced oxidation is noted early in infants that develop BPD (13,14), and the persistence of lung inflammation is associated with more severe disease (15).
The effects of hyperoxia on lung growth and development in our studies are consistent with those that have been previously described (Fig. 3A) (7,8,16–18). Lung tissue morphologic comparisons between 85% and >95% O2 demonstrate similar patterns of delayed growth at day 1 and 3 but between 7 and 14 d of exposure lung tissues from the 85% exposure group resumed patterns of growth similar to the RA controls. Lung tissues from the 95% exposure group have even more pronounced defects in alveolar development and larger airspace areas that might represent tissue destruction rather than an isolated effect of deficits in lung development (Fig. 3B). The apparent decrease in alveolar development we observed at 14 d of >95% O2 exposure could be explained as hyperoxia-induced cell death (12,19), but further characterization of this deficit is beyond the scope of the present study. The greater septal thickness in the 85% O2-exposed pups than in the RA pups at all days may indicate inhibition of pathways associated with septal thinning. More important than the relative differences between exposures is the fact that the septa did not thin between days 1 and 14 in either hyperoxia groups but did show signs of thinning in the RA pups.
Increases in the numbers of neutrophils in the lung due to hyperoxic exposure are considered indices of inflammation (6,7,20,21). The substantially greater number of neutrophils at day 14 in the tissues from pups exposed to >95% O2 than in those exposed 85% O2 or RA (Fig. 4) indicate that there is greater inflammation in the lungs of the pups exposed to >95% O2. These differences in inflammation may indicate induction of inflammatory resolution pathways in the 85% O2-exposed pups that fail to occur in the 95% O2-exposed pups.
Lipid mediators possess potent pro- and anti-inflammatory properties that could influence the responses to hyperoxia in the lung. cPLA2 levels have been associated with deficiencies in clara cell secretory protein, mechanical ventilation, and LPS-induced lung injury (22,23). We observed substantial increases in cPLA2 protein levels in both 85% and >95% O2-exposed groups at day 7 that persisted in the >95% O2 group through day 14 (Fig. 5). Increases in cPLA2 levels would be the first step in the propagation of metabolically active lipids and the decreased levels observed in the 85% O2-exposed group at 14 d further support the induction of adaptive pathways between 7 and 14 d of exposure.
COX-2 is produced in response to inflammatory stimuli but low levels of constitutive expression are evident in the lung (24). COX-2 and COX-2 metabolites have been shown to be involved in acute lung injury in animal models of BPD (25–27). In the current study, COX-2 levels in hyperoxia-exposed pups were elevated by day 7 in both oxygen-exposed groups (Fig. 6) and this elevation persisted through 14 d. A doubling of COX-2 levels by 7 d in lung tissues from hyperoxia-exposed pups suggests the possibility of increased PG and/or TBX synthesis in the lungs of these animals.
The greatest increases in the PGs measured in these studies were at 7 d of hyperoxia exposure. However, the increases in PG levels were observed in the tissues from animals exposed to >95% O2 only. This suggests differential regulation of the COX-2 pathway between 85% and >95% O2 exposure. Whether this finding represents the inhibition of other enzymes necessary for synthesis of PGs or alternative regulation of COX-2 is unknown and necessitates further investigations into the adaptive mechanisms associated with hyperoxia in these models.
LTs are increased in animals exposed to hyperoxia, and inhibition of 5-LO activities have prevented deficits in alveolarization (28). We observed no differences in 5-LO levels for the first 3 d of O2 exposure, but at day 7 increases were evident in the >95% O2 group only (Fig. 7). The increased levels of 5-LO in the 85% O2-exposed group at 14 d, in the absence of increased numbers of neutrophils, are not easily explained but may indicate alternative activities of 5-LO or increases in inflammatory resolution pathways in the lungs of these animals.
LT levels were not consistently detectable in the tissues of the newborn mouse pups and would likely to be at the highest levels in either the BAL or blood. However, technical limitations make these studies difficult because of issues in obtaining sufficient quantities of BAL or blood from these extremely small pups. We did measure 5-HETE levels as an indicator of 5-LO activity and found no differences between exposures throughout the time course of hyperoxia. These findings would suggest that the 5-LO levels measured in the tissues are likely to be coming from neutrophils that are primarily present in the air spaces and exerting their effects on the cells and proteins at or near the gas exchange surface. Consequently, the relative abundance of the products of 5-LO may be difficult to measure in the background of a whole lung homogenate.
The mechanisms associated with the adaptive capabilities of mouse pups exposed to sub-lethal concentrations of oxygen are not easily understood. Our data indicate that pups exposed to 85% O2 are able to resume normal body growth rates after 7 d, but do not recover to the levels of their RA counterparts by 14 d. Neutrophil accumulations in the lungs of pups exposed to 85% O2 are remarkably less than in the lungs of pups exposed to >95% O2 by day 14. Our original hypothesis that lipid metabolizing enzymes would be greater in the pups exposed to >95% O2 than those exposed to 85% O2 or RA was refuted as induction of cPLA2, COX-2, and 5-LO was for the most part similar in both hyperoxia-exposed groups. However, measurable increases in PG levels were primarily evident in the 95% O2-exposed pups at 7 d suggesting alternative regulation of COX-2 metabolites and suppression of downstream enzymes in the 85% O2-exposed pups. Collectively, these data indicate that key events take place in the lungs of mouse pups at between 7 and 14 d of exposure to 85% O2 that result in either adaptation or inflammatory resolution. Alternatively, the differences in responses to hyperoxia between the two exposure groups could represent a continuum of injury mediated by differential contributions of oxidative and inflammatory mechanisms between the exposure groups.
Our data clearly indicate a difference in response to 85% and >95% O2 exposure, however, further studies are needed to define the mechanisms responsible for these differences. Understanding the mechanisms associated with these events could lead to therapeutic interventions against hyperoxic lung injury in premature infants and the subsequent development of BPD.
Abbreviations
- BPD:
-
bronchopulmonary dysplasia
- COX-2:
-
cyclooxygenase-2
- cPLA2:
-
cytoplasmic phospholipase A2
- LO:
-
lipoxygenase
- LT:
-
leukotriene
- PG:
-
prostaglandin
- RA:
-
room air;,
- TBX:
-
thromboxane
References
Wispe JR, Roberts RJ 1987 Molecular basis of pulmonary oxygen toxicity. Clin Perinatol 14: 651–666
O'Donovan DJ, Rogers LK, Kelley DK, Welty SE, Ramsay PL, Smith CV 2002 CoASH and CoASSG levels in lungs of hyperoxic rats as potential biomarkers of intramitochondrial oxidant stresses. Pediatr Res 51: 346–353
Tipple TE, Welty SE, Rogers LK, Hansen TN, Choi YE, Kehrer JP, Smith CV 2007 Thioredoxin-related mechanisms in hyperoxic lung injury in mice. Am J Respir Cell Mol Biol 37: 405–413
Wong YL, Smith CV, McMicken HW, Rogers LK, Welty SE 2001 Mitochondrial thiol status in the liver is altered by exposure to hyperoxia. Toxicol Lett 123: 179–193
Zhao B, Ramsay PL, Park MS, Welty SE, De MA 2000 In vivo and in vitro analysis of hyperoxia-induced gene expression in mouse lung and mouse transformed Clara cells. Ann NY Acad Sci 923: 346–347
Crapo JD, Barry BE, Foscue H, Shelburne J 1980 Structural and biochemical changes in rat lungs ocurring during exposures to lethal and adaptive doses of oxygen. Am Rev Respir Dis 122: 123–143
Warner BB, Stuart LA, Papes RA, Wispe JR 1998 Functional and pathological effects of prolonged hyperoxia in neonatal mice. Am J Physiol 275: L110–L117
Park MS, Rieger-Fackeldey E, Schanbacher BL, Cook AC, Bauer JA, Rogers LK, Hansen TN, Welty SE, Smith CV 2007 Altered expressions of fibroblast growth factor receptors and alveolarization in neonatal mice exposed to 85% oxygen. Pediatr Res 62: 652–657
Rehan VK, Wang Y, Patel S, Santos J, Torday JS 2006 Rosiglitazone, a peroxisome proliferator-activated receptor-g agonist, prevents hyperoxiz-induced neonatoal rat lung injury in vivo. Pediatr Pulmonol 41: 558–569
Nakamura T, Henson PM, Murphy RC 1998 Occurrence of oxidized metabolites of arachidonic acid esterified to phospholipids in murine lung tissue. Anal Biochem 262: 23–32
Pappas CT, Obara H, Bensch KG, Northway WH Jr 1983 Effect of prolonged exposure to 80% oxygen on the lung of the newborn mouse. Lab Invest 48: 735–748
McGrath-Morrow SA, Stahl J 2001 Apoptosis in neonatal murine lung exposed to hyperoxia. Am J Respir Cell Mol Biol 25: 150–155
Ogihara T, Hirano K, Morinobu T, Kim HS, Hiroi M, Ogihara H, Tamai H 1999 Raised concentrations of aldehyde lipid peroxidation products in premature infants with chronic lung disease. Arch Dis Child Fetal Neonatal Ed 80: F21–F25
Nycyk JA, Drury JA, Cooke RW 1998 Breath pentane as a marker for lipid peroxidation and adverse outcome in preterm infants. Arch Dis Child Fetal Neonatal Ed 79: F67–F69
Speer CP 2003 Inflammation and bronchopulmonary dysplasia. Semin Neonatol 8: 29–38
Massaro D, Massaro GD 2002 Invited review: pulmonary alveoli: formation, the “call for oxygen,” and other regulators. Am J Physiol Lung Cell Mol Physiol 282: L345–L358
Massaro GD, Olivier J, Dzikowski C, Massaro D 1990 Postnatal development of lung alveoli: suppression by 13% O2 and a critical period. Am J Physiol 258: L321–L327
Alejandre-Alcazar MA, Kwapiszewska G, Reiss I, Amarie OV, Marsh LM, Sevilla-Perez J, Wygrecka M, Eul B, Kobrich S, Hesse M, Schermuly RT, Seeger W, Eickelberg O, Morty RE 2007 Hyperoxia modulates TGF-beta/BMP signaling in a mouse model of bronchopulmonary dysplasia. Am J Physiol Lung Cell Mol Physiol 292: L537–L549
Dieperink HI, Blackwell TS, Prince LS 2006 Hyperoxia and apoptosis in developing mouse lung mesenchyme. Pediatr Res 59: 185–190
Ramsay PL, Smith CV, Geske RS, Montgomery CA, Welty SE 1998 Dexamethasone enhancement of hyperoxic lung inflammation in rats independent of adhesion molecule expression. Biochem Pharmacol 56: 259–268
Crapo JD 1986 Morphologic changes in pulmonary oxygen toxicity. Annu Rev Physiol 48: 721–731
Yoshikawa S, Miyahara T, Reynolds SD, Stripp BR, Anghelescu M, Eyal FG, Parker JC 2005 Clara cell secretory protein and phospholipase A2 activity modulate acute ventilator-induced lung injury in mice. J Appl Physiol 98: 1264–1271
Nagase T, Uozumi N, Aoki-Nagase T, Terawaki K, Ishii S, Tomita T, Yamamoto H, Hashizume K, Ouchi Y, Shimizu T 2003 A potent inhibitor of cytosolic phospholipase A2, arachidonyl trifluoromethyl ketone, attenuates LPS-induced lung injury in mice. Am J Physiol Lung Cell Mol Physiol 284: L720–L726
Simmons DL, Botting RM, Hla T 2004 Cyclooxygenase isozymes: the biology of prostaglandin synthesis and inhibition. Pharmacol Rev 56: 387–437
Fukunaga K, Kohli P, Bonnans C, Fredenburgh LE, Levy BD 2005 Cyclooxygenase 2 plays a pivotal role in the resolution of acute lung injury. J Immunol 174: 5033–5039
Hodges RJ, Jenkins RG, Wheeler-Jones CP, Copeman DM, Bottoms SE, Bellingan GJ, Nanthakumar CB, Laurent GJ, Hart SL, Foster ML, McAnulty RJ 2004 Severity of lung injury in cyclooxygenase-2-deficient mice is dependent on reduced prostaglandin E(2) production. Am J Pathol 165: 1663–1676
Park GY, Christman JW 2006 Involvement of cyclooxygenase-2 and prostaglandins in the molecular pathogenesis of inflammatory lung diseases. Am J Physiol Lung Cell Mol Physiol 290: L797–L805
Manji JS, O'Kelly CJ, Leung WI, Olson DM 2001 Timing of hyperoxic exposure during alveolarization influences damage mediated by leukotrienes. Am J Physiol Lung Cell Mol Physiol 281: L799–L806
Acknowledgements
We thank Xiaomei Meng, Molly Augustine, and Kathryn Heyob for their technical support.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was supported by NHLBI, HL068948.
Rights and permissions
About this article
Cite this article
Rogers, L., Tipple, T., Nelin, L. et al. Differential Responses in the Lungs of Newborn Mouse Pups Exposed to 85% or >95% Oxygen. Pediatr Res 65, 33–38 (2009). https://doi.org/10.1203/PDR.0b013e31818a1d0a
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/PDR.0b013e31818a1d0a
- Springer Nature America, Inc.
This article is cited by
-
The CD146-HIF-1α axis regulates epithelial cell migration and alveolar maturation in a mouse model of bronchopulmonary dysplasia
Laboratory Investigation (2022)
-
IL-33-induced neutrophil extracellular traps degrade fibronectin in a murine model of bronchopulmonary dysplasia
Cell Death Discovery (2020)
-
Early Life Supraphysiological Levels of Oxygen Exposure Permanently Impairs Hippocampal Mitochondrial Function
Scientific Reports (2019)
-
Alterations in VASP phosphorylation and profilin1 and cofilin1 expression in hyperoxic lung injury and BPD
Respiratory Research (2018)
-
Loss of CD73-mediated extracellular adenosine production exacerbates inflammation and abnormal alveolar development in newborn mice exposed to prolonged hyperoxia
Pediatric Research (2017)