Abstract
Introduction
The co-existence of malaria with bacterial infections is common in the tropics, hence the concurrent use of antimalarials and antibiotics.
Objective
This study aimed to investigate the effect on pharmacokinetics and antimicrobial activity of co-administration of quinine and combined ampicillin–cloxacillin.
Methods
In total, 14 healthy adults received single oral doses of ampicillin–cloxacillin combination alone and with quinine in a randomized crossover manner. Urine samples collected at predetermined intervals over 48 h were analysed. The effect of quinine on minimum inhibitory concentrations (MICs) of ampicillin and cloxacillin were determined against Staphylococcus aureus by agar diffusion, agar dilution, and broth dilution.
Results
Quinine significantly reduced the rate and extent of excretion of ampicillin and cloxacillin (p < 0.0002). The total amounts of ampicillin and cloxacillin excreted unchanged (Du∞) alone were 217.10 ± 53.82 and 199.0 ± 64.29 mg versus 126.40 ± 50.63 and 135.20 ± 52.24 mg, respectively, with quinine. Respective maximum excretion rates (dDu/dt max) for ampicillin and cloxacillin were 43.55 ± 19.41 and 77.64 ± 29.65 mg/h alone versus 18.01 ± 8.52 and 53.16 ± 20.72 mg/h with quinine. This indicates a significant reduction in Du∞and dDu/dt max by 41.78 and 58.65 % for ampicillin and 32.06 and 31.53 % for cloxacillin. Conversely, the disposition of quinine was unaffected by ampicillin–cloxacillin (p > 0.1). The MIC of antibiotics alone versus with quinine, respectively, were 0.11 ± 0.04 and 0.78 ± 0.1 µg/ml for ampicillin, and 0.18 ± 0.1 and 0.92 ± 0.4 µg/ml for cloxacillin, with a five- to sevenfold increase (p > 0.01); indicating a decrease in antimicrobial activity by quinine.
Conclusions
Quinine therefore, reduced the bioavailability and the antimicrobial activity of ampicillin–cloxacillin upon co-administration, which may have therapeutic implications. Caution is required with the co-administration of these medicines.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
This paper describes how quinine, a quinolone antimalarial, affects the pharmacokinetics and antibacterial properties of combined ampicillin–cloxacillin. |
Quinine markedly reduced the bioavailability of ampicillin–cloxacillin combination in healthy subjects. |
Quinine also reduced the sensitivity of cloxacillin–ampicillin to Staphylococcus aureus by increasing the minimum inhibitory concentration by over sixfold. |
1 Introduction
The co-administration of different drugs is imperative to achieve a desired therapeutic objective or treat coexisting diseases [1]. For example, the concurrent use of antibacterials and antimalarials is common in the tropics because malaria is frequently associated with other infections such as those of the respiratory tract, urinary tract, or ear, sexually transmitted infections (STIs), and diarrhea, among other infections [2]. Although numerous benefits can be derived from co-administration of different drugs, the expected therapeutic outcome is sometimes affected by drug–drug interactions [3], which have been demonstrated scientifically in the literature.
For instance, earlier studies carried out in healthy adults revealed the presence of pharmacokinetic interactions between quinoline antimalarials and antibiotics when co-administered [4–7]. These interactions markedly reduced bioavailability and could result in sub-therapeutic drug levels as well as treatment failure, with implications for therapeutic outcomes and the safety and efficacy of the antibiotics [8]. Worthy of note were scientific investigations that proved significant reduction in bioavailability of some penicillins (ampicillin and cloxacillin) following oral co-administration with quinoline antimalarials [4–7].
Nigeria is the largest country in Africa and the sixth largest in the world, with a current growing population of over 170 million people [9]. However, the country is plagued with diverse infectious diseases, including malaria and notable bacterial infections [10].
Patients, physicians, pharmacists, and other healthcare providers may be unaware of the possible interactions between antibiotics and antimalarials as well as the mechanisms involved. It is therefore common practice to co-administer antimalarial and antibiotic drugs.
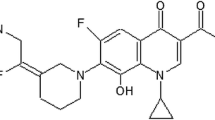
Quinine, a quinoline antimalarial, has been in use for over 400 years [11] and continues to play a significant role in the management of malaria as one of the most important drugs for the treatment of complicated, cerebral, and resistant malaria [12, 13]. Ampicillin and cloxacillin are among the most widely used penicillin derivatives [14], with a wide spectrum of antibiotic activity when used in combination or individually [15].
Penicillin antibiotics, including combined ampicillin–cloxacillin (Ampiclox®), amoxicillin and quinoline antimalarials such as quinine, artemisinin derivatives and proguanil (a prophylactic), and occasionally chloroquine, are readily available in the tropics for the management of bacterial infections and malaria. Additionally, self-medication is common among this vast population, where the average ratio of physicians to patients is extremely low [16]. Consequently, the consumption of oral formulations of antibiotics and antimalarials rank highest in the volume of medications frequently administered; this is a potential public health issue. A survey carried out in University College Hospital (UCH), Ibadan, Nigeria, revealed that the most prescribed medicines were antimalarials and more than 50 % of these were prescribed concurrently with antibacterial drugs [17].
Quinoline antimalarials have been found to reduce the bioavailability of penicillin antibiotics by 40–70 %, with a corresponding increase in minimum inhibitory concentration (MIC) and minimum bactericidal concentration (MBC) by two- to seven fold [4–7, 18]. The extent of interactions reported with the co-administration of these often used drugs is expected to increase as a potential public health issue; however, little has been done to create awareness or investigate the extent of interactions or their impact, especially on the therapeutic outcomes of penicillin antibiotics.
Given the potentially wide impact antimalarial–antibiotic drug interactions could exert on patient care, this study investigated the effect of co-administration of quinine and ampicillin–cloxacillin on their respective pharmacokinetic parameters in healthy Nigerian adult volunteers as well as the effect of concomitant use on the antimicrobial activity of ampicillin and cloxacillin.
2 Methods
2.1 Chemicals and Reagents
Quinine sulphate and secondary reference primaquine diphosphate were obtained from BDH Chemicals (Poole, UK). Cloxacillin sodium, amoxicillin trihydrate, and ampicillin trihydrate secondary reference samples were obtained from Fidson Pharmaceutical Ltd, Sango Ota, Ogun State, Nigeria.
HPLC-grade acetonitrile and methanol were supplied by Sigma Aldrich (BDH Chemicals). Analytical grade perchloric acid, diethyl ether, and sodium hydroxide pellets were procured from BDH Chemicals.
Ampiclox® capsules manufactured by Beecham Pharmaceuticals, Brentford, UK (batch no. 100434 and NAFDAC [the Nigerian National Agency for Food and Drug Administration and Control] no. 04-2401) and quinine sulphate tablets manufactured by NEM Laboratories (P) Ltd, Mumbai, India (batch no. 09-1 and NAFDAC no. A4-1880) were purchased from a reputable pharmacy at Ibadan. Other reagents and chemicals were of analytical grade. Wire loop, cork borer, spatula, MaCarteny universal bottles, transparent ruler, swab stick, cotton wool, aluminum foil, needle and syringes, slide, plastacin, cover slip, micropipette, and thermometer were supplied by and used at the Medical Microbiology Department, UCH, Ibadan, Nigeria.
2.2 In Vivo Analysis
2.2.1 Subjects
We recruited 14 healthy volunteers (ten males and four females) aged 18–42 years (mean ± standard deviation [SD] 26.71 ± 6.90) and weighing 49–77 kg (mean [SD] 64.92 ± 8.87) for the study; all provided written informed consent. The study protocol was approved by the Joint Ethics Committee of University of Ibadan/UCH, Ibadan, Nigeria. All subjects were non-smokers; medical examination confirmed they had experienced no recent illness. None of the subjects consumed any medication or alcohol 1 week prior to and throughout the period of the study.
2.2.2 Drug Administration and Sample Collection
Each subject observed an overnight fast and remained in the fasting state for 4 h after drug administration. A standard meal was served thereafter and water was taken ad labium. In a random cross-over design, volunteers were distributed into three groups comprising four to five subjects each and monitored for drug–drug interactions. For the first study period, each volunteer in group 1 received a single oral dose of quinine sulphate tablets (500 mg), volunteers in group 2 each received a single oral dose of ampicillin–cloxacillin combination capsule (Ampiclox®; 1000 mg), and group 3 received both quinine sulphate tablets (500 mg) and ampicillin–cloxacillin combination capsule (1000 mg). A washout period of 1 week was observed, and at the end of the third study period, all 14 subjects had received the antimalarial drug (quinine sulphate tablets) alone, the antibiotic drugs (ampicillin–cloxacillin combination capsule) alone, and a combination of both antimalarial and antibiotic drugs
After drug administration for each arm, total urine voided was collected at 0, 0.25, 0.5, 1, 2, 4, 8, 12, 24, and 48 h. The pH was determined and aliquots of 20 ml were stored at –20 °C until analysis.
2.2.3 Drug Analysis
An Adept series Cecil CE 4200, dual piston pump (Cecil CE 4100), power stream, chromatography system manager CE 4900 fitted with a ultraviolet (UV) detector and LiChrospher® 100 RP-18 (5 µm) Column with LiChroCART 125 × 4.0 mm I.D were used for sample analysis. Two reverse-phase high-performance liquid chromatography (HPLC) methods were used to determine drug concentrations in urine samples. Cloxacillin and quinine were analyzed using a modified and validated HPLC method described by Babalola et al. [5] for quinine, while ampicillin was analyzed using a developed and validated method. Amoxicillin was used as the internal standard (IS) for the determination of ampicillin, while primaquine was the IS used for determining cloxacillin and quinine in urine samples.
For the determination of ampicillin, 40 µl (equivalent to 20 µg/ml) of amoxicillin (IS) was added to 50 µl urine in a 2-ml Eppendorf tube, and the final volume was made up to 1 ml, with the mobile phase consisting of acetonitrile and 0.02 M potassium phosphate buffer, pH 4.5 (15:85 % v/v). The mixture was vortex mixed for 20 s then centrifuged at 2500 rpm for 5 min. The supernatant (20 µl) was injected into a C-18 column and the mobile phase was pumped at a flow rate of 0.6 ml/min.
For cloxacillin, 20 µl (equivalent to 10 µg/ml) of the primaquine (IS) was added to 100 µl of urine in a 2.0-ml Eppendorf tube, and the final volume was made up to 1 ml, with the mobile phase consisting of methanol, acetonitrile, and 0.02 M potassium phosphate buffer (10:25:65 % v/v/v), at a pH of 4.2. The solution was mixed with the vortex mixer for 20 s then centrifuged at 2500 rpm for 5 min. A total of 20 µl of the supernatant was injected and the mobile phase was pumped at a flow rate of 1.0 ml/min.
For quinine, 1 ml of urine was placed in a 10-ml tapered extraction tube and 20 µl of 100 µg/ml IS (primaquine) solution was added. 200 µl of perchloric acid was also added and mixed for 5 s. 1 ml of 5 M NaOH and 4 ml of ether were further added, followed by whirl mixing for 1 min and centrifugation at 3000 rpm for 10 min. The ether layer was transferred into another tube and 100 µl of 0.1 M HCl was added. After whirl mixing for 1 min and centrifuging for 5 min, a 20-µl aliquot of the aqueous layer was injected into the HPLC. The mobile phase methanol:acetonitrile:buffer (0.02 M KH2PO4) in the ratio (10:25:65 v/v/v) at pH 4.2 used for cloxacillin was also used but with a flow rate of 0.5 ml/min.
Detection of the three drugs was achieved with a UV detector at a wavelength of 225 nm.
Between-day and within-day co-efficient of variation (CV %) were determined and found to vary between 1 and 9 %, while recovery ranged between 92 and 107 %. The limit of detection (LOD) for ampicillin, cloxacillin, and quinine were 2, 0.8, and 0.02 µg/ml, respectively.
2.3 In Vitro Analysis
Microorganisms were first identified using catalase and coagulase tests for Staphylococcus aureus then indole and motility tests for the strains of Escherichia coli. An antimicrobial sensitivity test was carried out and Staphylococcus aureus was found out to be more susceptible to the drugs investigated.
The MICs of the antibiotics were determined alone and in combination with the antimalarial drug using three methods: agar diffusion, agar dilution, and broth dilution. The broth dilution method gave the best result. For the broth dilution method, a liter of sterile nutrient broth was prepared and 5 ml transferred into properly labeled test tubes (14 test tubes for each drug and each combination, with three controls). The tubes were corked with cotton wool and aluminum foil, then sterilized in an autoclave for 20 min. Upon cooling, 250 mg of each drug was dissolved in 10 ml sterile distilled water and diluted further to obtain 250 µg/ml. This concentration was serially diluted further using a double dilution method, thus reducing the concentrations to 125, 62.5, 31.25, 15.63, 7.81, 3.91, 1.98, 0.98, 0.49, 0.24, 0.12, 0.06, and 0.03 µg per 5 ml of each of the drugs. The solutions in the test tubes were mixed thoroughly and inoculated with about 0.1 ml of 1 in 70 dilution of an overnight broth culture of test organism. The solutions in the test tubes were incubated at 37 °C for 48 h. The MIC was the lowest concentration that prevented the growth of the controlled S. aureus (ATCC 25923) after 24 h incubation, which was indicated by clear broth solution.
2.4 Data Analysis
Pharmacokinetic parameters, including amounts of unchanged drug excreted in urine (Du∞), maximum peak of excretion (Dumax), elimination half-life (t ½), and time to maximum peak of excretion (t max), were computed using the non-compartmental pharmacokinetic computation.
Peak area ratios were generated from chromatograms for generating calibration curves, from which the concentrations where determined by interpolating peak area ratios to corresponding curves for each drug.
The following pharmacokinetic parameters were determined from urine data:
where Du is the amount excreted in time interval and t is the time midpoint.
Du∞ = Total amount of drug excreted unchanged in urine.
This is calculated by the sum of the amount of drug excreted unchanged in urine at intervals.
Maximum excretion rate (dDu/dt max) and time required to reach maximum peak of excretion t max were obtained directly from the urine data for each volunteer.
The t ½ was calculated using the formula
where K is the elimination rate constant, which was calculated by the linear regression analysis of log excretion rate-time profile.
Results were recorded as mean ± SD with 95 % confidence intervals (CIs). Student’s t test (two-tailed, paired) was performed on the pharmacokinetic parameters obtained using GraphPad Software (GraphPad Prism Version 3.0 for Windows) and Microsoft® Excel 2007 software. In all, a value of p < 0.05 was considered statistically significant.
3 Results
Details of the pharmacokinetic parameters obtained for ampicillin, cloxacillin, and quinine before and after co-administration in each subject are shown in Tables 1, 2, 3. Figures 1–3 show urinary profile of the drugs (ampicillin, cloxacillin and quinine) by excretion rate, cumulative and amount remaining to be excreted (ARE) methods. Wide inter- and intra-individual variations were observed in the results obtained. Table 4 shows the pH of urine voided by volunteers after drug administration. There was no significant effect on the pH values with drugs administered
Co-administration of quinine and ampicillin–cloxacillin resulted in a significant decrease in the Dumax and mean Du∞ of ampicillin (p < 0.001) and cloxacillin (p < 0.05). However, the parameters of quinine were not significantly affected (p > 0.1).
The Du∞ and Dumax for ampicillin were decreased in all subjects after co-administration with quinine. However, for cloxacillin, Du∞ and dDu/dt max decreased only in 11 of the 14 subjects after co-administration of ampicillin–cloxacillin with quinine. Du∞ and dDu/dt max for administration of quinine alone were comparable with the corresponding values when co-administered with ampicillin–cloxacillin in all subjects, indicating a lack of significant decrease in pharmacokinetics.
The dDu/dt max of ampicillin and cloxacillin was decreased by 58.65 and 31.53 %, whereas their Du∞ was decreased by 41.78 and 32.06 %, respectively (p < 0.05). The t max at maximum excretion and the t ½ of ampicillin and cloxacillin were in most cases longer after concurrent intake with quinine; however, differences were not statistically significant (p > 0.05). The percentage decrease in dDu/dt max and Du∞ of quinine when co-administered with ampicillin–cloxacillin in the 14 volunteers was <2 % in all subjects.
The results of the effect of quinine on the antimicrobial activities of ampicillin and cloxacillin against S. aureus are summarized in Table 5. The mean MIC of the drugs investigated alone and in combination with quinine were 0.11 ± 0.04 and 0.78 ± 0.1 μg/ml for ampicillin, indicating a sevenfold increase in MIC, 0.18 ± 0.1 and 0.92 ± 0.4 μg/ml for cloxacillin with a fivefold increase in MIC, and 0.02 ± 0.01 and 0.25 ± 0.1 μg/ml for ampicillin–cloxacillin, with a 13-fold increase in MIC. There was a significant decrease in the antimicrobial activity of ampicillin, (p = 0.0001), cloxacillin (p = 0.0122), and ampicillin–cloxacillin (p = 0.0145) when used concomitantly with quinine.
4 Discussion
This is the first time in vitro and correlating in vivo methodologies have been used to establish drug–drug interactions between quinoline antimalarials and penicillin antibiotics, confirming the stage of interaction to be the absorption phase after oral co-administration of penicillin antibiotics and quinoline antimalarials. The study also compared the effect of quinine on ampicillin as well as cloxacillin for the first time, unlike previous studies in which only the effects of quinoline antimalarials on cloxacillin [5–7] or ampicillin [4] have been evaluated. Additionally, this study is the first to investigate the effect of penicillin antibiotics on quinoline antimalarials and vice versa after co-administration.
In this study, in vivo drug–drug interactions were monitored using data from urinary drug excretion, which is non-invasive and useful for the determination of pharmacokinetic parameters when a drug or its metabolite is reasonably excreted in urine [19, 20]. Ampicillin and cloxacillin fall into the class of drugs excreted unchanged in reasonable amounts in urine after oral administration. The use of urinary data in this study is thus justified given that any drug that appears in urine must have been first absorbed into the blood. Although plasma data is the gold standard for pharmacokinetic/pharmacodynamic measurements, urinary excretion data were used in lieu of plasma data, especially as the drugs in this study, specifically the antibiotics, are largely excreted unchanged in urine, and urine collection is a non-invasive method for such studies [20].
The decrease in total amount of ampicillin and cloxacillin excreted unchanged in urine by 41.78 and 32.06 %, respectively, as well as the marked reduction in Dumax by 58.65 and 31.53 %, indicate significant reductions in ampicillin (p < 0.0001) and cloxacillin (p < 0.0190) bioavailability following oral co-administration of ampicillin–cloxacillin and quinine tablets. Quinine reduced the rates and extent of absorption of ampicillin and cloxacillin.
The pattern of results obtained and the half-life values in this study correlate with in vivo reports in earlier studies [4–6].
In 1985, Ali [4] reported a similar interaction between ampicillin and chloroquine, whereby a significant reduction in percentage of ampicillin excreted in urine (34 %; p < 0.005) was observed. However, the effect of quinine on rates and extents of excretion of ampicillin in this study were more pronounced than that reported for chloroquine.
The possible effect of chloroquine on the urinary excretion of cloxacillin when co-administered with ampicillin–cloxacillin was also investigated earlier in eight healthy adult volunteers [6]. A significant reduction (64 %) in the urinary excretion of cloxacillin was reported. Additionally, the effect of oral co-administration of proguanil with cloxacillin was also evaluated in seven healthy adult volunteers. A 48 % decrease in both rate and extent of absorption of cloxacillin was reported [6]. A recent study reported a reduction in the mean amount of cloxacillin excreted in urine following the co-administration of artesunate with amoxicillin–cloxacillin [7]. Nine of the 14 subjects showed a significant decrease 39 % (p = 0.0006) in the urinary excretion (Du∞) of cloxacillin, whereas five subjects (36 %) showed a significant increase of 27 % (p = 0.014) when amoxicillin and artesunate were co-administered. The result showed a significant reduction in the bioavailability of cloxacillin after co-administration with artesunate.
All except one [4] of these earlier studies were conducted in our laboratory, and both in vivo and in vitro results correlate with those observed in this study.
dDu/dt max and Du∞, t max, and t ½ obtained for quinine in urine after a single oral dose of 500 mg and when co-administered with ampicillin–cloxacillin 1000 mg in 14 healthy volunteers showed no significant difference (p > 0.1), indicating that quinine was not affected by co-administration with ampicillin–cloxacillin . The results of this study thus suggest a significant drug–drug interaction between quinine and ampicillin–cloxacillin in a manner that primarily affects the bioavailability of the penicillin antibiotics.
The significant decrease in total amount of antibiotics (such as ampicillin and cloxacillin) excreted unchanged in urine as well as the marked reduction in maximum peak of excretion clearly indicate significant reductions in their bioavailability following oral co-administration of these penicillins with quinoline antimalarials, since only drugs absorbed in the blood can be eliminated via the kidney. In general, the quinoline antimalarials reduced the rates and extent of absorption of the penicillin antibiotics.
Although the mechanism of this interaction has not been fully explained, the reduction of the bioavailability of these antibiotics might be attributed to slower gastric emptying and inhibition of gastric motility produced by antimalarials [4]. Quinine has an anti-spasmodic effect [21, 22] and has been shown to significantly attenuate extracellular potassium transients in vitro [22]. Quinine thus initiates smooth muscle contraction, especially in tubular organs of the gastrointestinal tract, thereby preventing spasms of the intestine. Such reduction in gastric motility may give rise to acid hydrolysis of a β-lactam ring, with a lesser effect on cloxacillin as a result of the presence of bulky side chains that exhibit stearic hindrance around the β-lactam ring. This, in addition to the chlorine atom on its phenyl ring, makes it resistant to acid catalyzed hydrolysis in the stomach or gastric breakdown [23] and hence may account for the lesser effect of interaction on the bioavailability of cloxacillin compared with ampicillin as observed in this study.
Reduction of ampicillin and cloxacillin bioavailability on oral co-administration with quinine could also be attributed to adsorption of ampicillin and cloxacillin to quinine in the gastrointestinal tract, formation of a complex between the drugs that can result in reduction in bioavailability of these antibiotics.
The in vitro results suggest that quinine significantly (p < 0.05) increased the MIC of ampicillin, cloxacillin, and ampicillin–cloxacillin on S. aureus by sevenfold, fivefold, and 13-fold, respectively. This strongly indicates a significant in vitro interaction between the penicillin antibiotics and quinoline antimalarial (quinine) tested. MIC is used to establish the sensitivity and effectiveness of antibiotics, and could also be a possible measure of antimicrobial activity. The marked increase in MICs of ampicillin, cloxacillin, and ampicillin–cloxacillin by sevenfold, fivefold, and 13-fold, respectively, when combined with quinine and used against S. aureus is thus indicative of a sharp decrease in sensitivity of the antibiotics tested. This also suggests a significant decrease in antimicrobial activity of the antibiotics investigated, which may translate into poor treatment outcome in clinical situations as well as drug resistance in the long run. Although the mechanism by which this happened is not clear, it could be attributed to the formation of a complex between both drugs that possibly leads to reduced antimicrobial activity of the penicillin antibiotics or an interaction that affects the beta-lactam ring. More studies are needed to confirm the mechanism of interaction. Consequently, the effect of quinoline antimalarials on penicillin antibiotics is central to public health, especially where people self-medicate or physicians prescribe antimalarials and antibiotics in areas endemic for malaria and infections.
The results obtained in this study were comparable with those reported in earlier studies [4–7, 24] and also showed a clear correlation between in vivo and in vitro studies, thus validating the significant reduction in bioavailability of ampicillin and cloxacillin when co-administered with quinoline antimalarials. However, it is imperative to note that this interaction is at an absorption level based on a proposed mechanism of action and in vitro interaction studies; previous studies by our team have shown that the dissolution of some antibiotics is reduced by quinoline antimalarials [24].
The wide range of differences obtained from the CI in this study is an indication of wide intra- and inter-individual variability.
4.1 Limitations of the Study
Urinary elimination data were used in lieu of plasma data, which is the gold standard. In this study, ampicillin and cloxacillin were not analysed in plasma due to their polarity and difficulties in carrying out solvent extraction or precipitation methods, which led to low sensitivity. Again, the already published plasma methods were not reproducible after many attempts.
5 Conclusion
Quinoline antimalarials have repeatedly reduced the in vivo and in vitro bioavailability as well as the antimicrobial activity of penicillins on co-administration in various studies. This is significant for oral administration of the drugs and may be occurring at the absorption phase of disposition.
The present study demonstrated significant drug-drug interaction between ampicillin and cloxacillin versus quinine (quinoline antimalarial) in a manner that correlates with previous in vivo reports [5-7]. There seems to be an in vitro–in vivo correlation in the interaction between penicillins and some antimalarials, and dissolution is probably the rate-limiting step in the absorption of penicillins. Findings from this study are of utmost importance and caution is required in the co-administration of these two classes of anti-infectives. It is also of public health concern, as the interactions can contribute towards observed antibiotic resistance and treatment failure being experienced in recommended antibiotic treatment regimens.
This interaction may also have clinical implications judging from bacterial kill studies. The antagonism demonstrated against antibiotics in these studies suggests that penicillin antibiotics and quinoline antimalarials should not be administered concurrently. Clinically, drugs that interact should be avoided or given sufficiently far apart that the interaction is minimized. In situations involving two drugs of choice that may interact, dose adjustment based on pharmacokinetic and therapeutic considerations of one or both of the drugs may be necessary. Drug administration can be separated by 2 h to avoid interaction at the absorption level based on the disposition of the penicillins, which have short half-lives.
References
Ojewole JAO. Drug interactions. In: Aguwa CN, editor. Therapeutic bases of clinical pharmacy in the tropics. Enugu: Optimal publishers; 1996. p. 19–145.
O’Dempsey T. Malaria in children. Afr Health. 2000;22:21–6.
Martinbiancho J, Zuckermann J, Dos Santos L, Silva MM. Profile of drug interactions in hospitalized children. Pharm Pract. 2007;5(4):157–61.
Ali HM. Reduced ampicillin bioavailability following oral coadministration with chloroquine. J Antimicrob Chemother. 1985;1985(15):781–4.
Babalola CP, Iwheye GB, Olaniyi AA. Effects of proguanil interaction on bioavailability of cloxacillin. J Clin Pharm Ther. 2002;27:461–4.
Babalola CP, Fashedemi TT, Olaniyi AA. Choloroquine reduces urinary excretion of cloxacillin when it is administered concurrently with ampicillin-cloxacillin combination. Trop J Pharm Res. 2003;2(1):169–73.
Babalola CP, Olori EO, Kotila OA, Falade O, Kolade YT, Sylva BO. Effect of artesunate on the urinary excretion of cloxacillin in healthy subjects. Nig J Pharm Res. 2009; 7(1):29–36.
Ojewole JAO. Drug interactions. In: Aguwa CN, editor, Therapeutic bases of clinical pharmacy in the tropics, 3rd ed. Enugu: Optimal Publishers; 2004. p. 23–49.
Population Reference Bureau World population data sheet. 2012. Available at http://www.prb.org/pdf12/2012-population-data-sheet_eng.pdf. Accessed 14 Mar 2015.
Ukaga CN, Orji CN, Orogwu S, Nwoke BEB, Anosike JC, Udujih OS, Onyeka PIK, Awujo NC. Concomitant bacteria in the blood of malaria patients in Owerri, southeastern Nigeria. Tanzan Health Res Bull. 2006;8(3):186–8.
Achan J, Talisuna AO, Erhart A, Yeka A, Tibenderana JK, Baliraine FN, Rosenthal PJ, D’Alessandro U. Quinine, an old anti-malarial drug in a modern world: role in the treatment of malaria. Malar J. 2011;10:144–55.
Lalloo DG, Shingadia D, Pasvol G, Chiodini PL, Whitty CJ, Beeching NJ, Hill DR, Warrell DA, Bannister BA. UK malaria treatment guidelines. J Infect. 2007;54:111–21.
World Health Organisation. World Malaria Report 2009. Geneva: World Health Organisation; 2010.
Kumar V, Bhutani H, Singh S. ICH guidance in practice: validated stability-indicating HPLC method for simultaneous determination of ampicillin and cloxacillin in combination drug products. J Pharm Biomed Anal. 2007;43(2):769–73.
Bru JP, Garraffo R. Role of intravenous cloxacillin for inpatient infections. Med Mal Infect. 2012;42(6):241–6.
Awad A, Eltayeb I, Matowe L, Thalib L. Self-medication with antibiotics and antimalarials in the community of Khartoum State, Sudan. J Pharm Pharm Sci. 2005;8:326–31.
Uchefunah OA. Antimalarial and antimicrobial usage in paediatrics in a tertiary Hospital. M. Pharm. Thesis. Clinical Pharmacy. Faculty of Pharmacy, University of Ibadan; 2007.
Ezeasor C. In vitro drug-drug interactions between some classical anti-malarials and some classical antibacterials. M. Pharm. Thesis. Clinical Pharmacy, Faculty of Pharmacy, University of Ibadan; 2011.
Babalola CP. Bioavailability/bioequivalence assessment. In: Olaniyi AA, Babalola CP, Oladedeinde FO, Adegoke AO, editors, Biopharmaceutical methods in drug quality assurance. Ibadan: Department of Pharmaceutical Chemistry, University of Ibadan, Nigeria; 2001. p. 79–99.
Shargel L, Wu-Pong S, Yu ABC. Applied biopharmaceutics and pharmacokinetics. MacGraw-Hill Publishers; 2005. p. 454–93.
Bikson M, Id Bihi R, Vreugdenhil M, Fox JE, Jefferys JGR. Effect of quinine on spontaneous low-Ca2+ epileptiform activity and intrinsic cell properties. J Physiol. 2001;2001(536P):S249.
Smirnov S, Paalasmaa P, Uusisaari M, Voipio J, Kaila K. Pharmacological isolation of the synaptic and nonsynaptic components of the GABA-mediated biphasic response in rat CA1 hippocampal pyramidal Cells Sergei. J Neurosci. 1999;19:9252–60.
Ito K, Iwatsubo T, Kanamitsu S, Ueda K, Suzuki H, Sugiyama Y. Prediction of pharmacokinetic alteration caused by drug-drug interaction in the liver. Pharmacol Rev. 1998;50(3):387–90.
Babalola CP, Olaniyi AA, Iwheye GB, Fashedemi TT, Ajoku CE, Adeniyi BA, Falade O, Olori EO. Significant interactions between some antibiotics and antimalarial drugs. In: Proceedings of Second Unibadan conference on biomedical research, University of Ibadan, Nigeria; 6–9 July, 2010.
Acknowledgments
The authors would like to acknowledge University of Ibadan Multidisciplinary Central Research Laboratory for the use of laboratory equipment and facilities for analysis. The authors thank Fidson Pharmaceuticals Ltd, Sango Ota, Ogun State, Nigeria for donating reference standards.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Author’s declaration
No funding was received for the conduct of this study.
Conflict of interest
OF, AGF, AAO, CE, DAK, and CPB have no conflicts of interest to declare.
Ethical consideration
This study protocol was approved by University of Ibadan-University College Hospital Ibadan (UI-UCH) Ethics Review Committee. The study was carried out in accordance with specified guuidelines for human subject research.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Falade, O.B., Falusi, A.G., Olaniyi, A.A. et al. Significant Pharmacokinetic Interactions Between Quinine and Ampicillin–Cloxacillin Combination. Drugs R D 16, 193–203 (2016). https://doi.org/10.1007/s40268-016-0128-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40268-016-0128-x