Abstract
Purpose
Several studies have analyzed factors associated to hospitalization in chronic obstructive pulmonary disease (COPD) patients. However, data are lacking on the quality of treatment received by patients prior to hospital admission. The present study analyzed how often patients requiring hospitalization for a COPD exacerbation had received previous treatment for the exacerbation, particularly antibiotics.
Methods
This was a multicenter, cross-sectional, observational study conducted in 30 Spanish hospitals among COPD patients aged >40 years who were hospitalized for an acute exacerbation. Patients were grouped according to whether or not they had received treatment prior to admission and, subsequently, according to whether or not they had received antibiotics. Patient eligibility for antibiotic therapy was assessed using both national and European guidelines.
Results
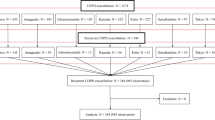
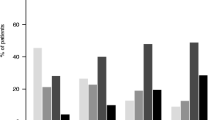
The study population consisted of 298 patients, of which 277 (93 %) were men, with a mean [standard deviation (SD)] age of 69.1 (9.5) years. One hundred and thirty-three patients (45 %) had received treatment prior to admission; among these, 76/133 (57 %) had received antibiotic therapy. However, 81–91 % of these patients fulfilled criteria for this therapy. Antibiotic use was significantly associated with yellow or green–yellow sputum prior to the exacerbation, a higher number of exacerbations in the previous year, more visits to emergency departments, and bronchiectasis. On the other hand, 10–20 % of patients who did receive antibiotics were not eligible for this therapy according to guidelines.
Conclusions
This study demonstrates a low rate of previous outpatient treatment and antibiotic use among patients with a COPD exacerbation requiring hospital admission.

Similar content being viewed by others
References
Miravitlles M, Ferrer M, Pont A, Zalacain R, Alvarez-Sala JL, Masa F, et al. Effect of exacerbations on quality of life in patients with chronic obstructive pulmonary disease: a 2 year follow up study. Thorax. 2004;59:387–95.
Miravitlles M, Mayordomo C, Artés M, Sánchez-Agudo L, Nicolau F, Segú JL. Treatment of chronic obstructive pulmonary disease and its exacerbations in general practice. EOLO Group. Estudio Observacional de la Limitación Obstructiva al Flujo aEreo. Respir Med. 1999;93:173–9.
Connors AF Jr, Dawson NV, Thomas C, Harrell FE Jr, Desbiens N, Fulkerson WJ, et al. Outcomes following acute exacerbation of severe chronic obstructive lung disease. The SUPPORT investigators (Study to Understand Prognoses and Preferences for Outcomes and Risks of Treatments). Am J Respir Crit Care Med. 1996;154:959–67.
Burrows B, Earle RH. Course and prognosis of chronic obstructive lung disease. A prospective study of 200 patients. N Engl J Med. 1969;280:397–404.
Soler J, Sánchez L, Latorre M, Alamar J, Román P, Perpiñá M. The impact of COPD on hospital resources: the specific burden of COPD patients with high rates of hospitalization. Arch Bronconeumol. 2001;37:375–81.
Garcia-Aymerich J, Serra Pons I, Mannino DM, Maas AK, Miller DP, Davis KJ. Lung function impairment, COPD hospitalisations and subsequent mortality. Thorax. 2011;66:585–90.
Matkovic Z, Huerta A, Soler N, Domingo R, Gabarrús A, Torres A, et al. Predictors of adverse outcome in patients hospitalised for exacerbation of chronic obstructive pulmonary disease. Respiration. 2012;84:17–26.
Soler-Cataluña JJ, Martínez-García MA, Román Sánchez P, Salcedo E, Navarro M, Ochando R. Severe acute exacerbations and mortality in patients with chronic obstructive pulmonary disease. Thorax. 2005;60:925–31.
Miravitlles M, Murio C, Guerrero T, Gisbert R; On behalf of the DAFNE Study Group. Costs of chronic bronchitis and COPD: a 1-year follow-up study. Chest. 2003;123:784–91.
Miravitlles M, Murio C, Guerrero T, Gisbert R; DAFNE Study Group. Pharmacoeconomic evaluation of acute exacerbations of chronic bronchitis and COPD. Chest. 2002;121:1449–55.
Garcia-Aymerich J, Barreiro E, Farrero E, Marrades RM, Morera J, Antó JM. Patients hospitalized for COPD have a high prevalence of modifiable risk factors for exacerbation (EFRAM study). Eur Respir J. 2000;16:1037–42.
Wilkinson TM, Donaldson GC, Hurst JR, Seemungal TA, Wedzicha JA. Early therapy improves outcomes of exacerbations of chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2004;169:1298–303.
Miravitlles M. Epidemiology of chronic obstructive pulmonary disease exacerbations. Clin Pulm Med. 2002;9:191–7.
Wilson R. Bacteria, antibiotics and COPD. Eur Respir J. 2001;17:995–1007.
Anthonisen NR, Manfreda J, Warren CPW, Hershfield ES, Harding GKM, Nelson NA. Antibiotic therapy in exacerbations of chronic obstructive pulmonary disease. Ann Intern Med. 1987;106:196–204.
Balter MS, La Forge J, Low DE, Mandell L, Grossman RF; The Chronic Bronchitis Working Group. Canadian guidelines for the management of acute exacerbations of chronic bronchitis. Can Respir J. 2003;10(Suppl B):3B–32B.
Lindenauer PK, Pekow P, Gao S, Crawford AS, Gutierrez B, Benjamin EM. Quality of care for patients hospitalized for acute exacerbations of chronic obstructive pulmonary disease. Ann Intern Med. 2006;144:894–903.
Incalzi RA, Corsonello A, Pedone C, Masotti G, Rengo F, Grassi V, et al. Use of antibiotics in elderly patients with exacerbated COPD: the OLD-Chronic Obstructive Pulmonary Disease Study. J Am Geriatr Soc. 2006;54:642–7.
Miravitlles M, Monsó E, Mensa J, Aguarón Pérez J, Barberán J, Bárcena Caamaño M, et al. Tratamiento antimicrobiano de la agudización de la EPOC: Documento de Consenso 2007. Arch Bronconeumol. 2008;44:100–8.
Woodhead M, Blasi F, Ewig S, Garau J, Huchon G, Ieven M, et al. Guidelines for the management of adult lower respiratory tract infections—summary. Clin Microbiol Infect. 2011;17(Suppl 6):1–24.
Langsetmo L, Platt RW, Ernst P, Bourbeau J. Underreporting exacerbation of chronic obstructive pulmonary disease in a longitudinal cohort. Am J Resp Crit Care Med. 2008;177:396–401.
Miravitlles M, Brosa M, Velasco M, Crespo C, Gobartt E, Diaz S, et al. An economic analysis of pharmacological treatment of COPD in Spain. Respir Med. 2009;103:714–21.
Sánchez López J, Bueno Cavanillas A. Factores asociados al uso inadecuado de un servicio de urgencias hospitalario. Emergencias. 2005;17:138–44.
Garcia-Aymerich J, Escarrabill J, Marrades RM, Monsó E, Barreiro E, Antó JM; EFRAM Investigators. Differences in COPD care among doctors who control the disease: general practitioner vs. pneumologist. Respir Med. 2006;100:332–9.
Murio C, Soler X, Pérez M, Calero G, Ruiz-Manzano J. Acute exacerbation of chronic obstructive pulmonary disease in primary care setting in Spain: the EPOCAP study. Ther Adv Respir Dis. 2010;4:215–23.
Aaron SD, Donaldson GC, Whitmore GA, Hurst JR, Ramsay T, Wedzicha JA. Time course and pattern of COPD exacerbation onset. Thorax. 2012;67:238–43.
Miravitlles M. Is it possible to reduce the use of antibiotics in severe exacerbations of chronic obstructive pulmonary disease? Respiration. 2008;76:249–50.
Adams SG, Melo J, Luther M, Anzueto A. Antibiotics are associated with lower relapse rates in outpatients with acute exacerbations of COPD. Chest. 2000;117:1345–52.
Miravitlles M, Murio C, Guerrero T; On behalf of the DAFNE Study Group. Factors associated with relapse after ambulatory treatment of acute exacerbations of chronic bronchitis. A prospective multicenter study in the community. Eur Respir J. 2001;17:928–33.
Beauchesne MF, Julien M, Julien LA, Piquette D, Forget A, Labrecque M, et al. Antibiotics used in the ambulatory management of acute COPD exacerbations. Int J Chron Obstruct Pulmon Dis. 2008;3:319–22.
Miravitlles M, Marín A, Monsó E, Vilà S, de la Roza C, Hervás R, et al. Colour of sputum is a marker for bacterial colonisation in chronic obstructive pulmonary disease. Respir Res. 2010;11:58.
Martínez-García MÁ, Soler-Cataluña JJ, Donat Sanz Y, Catalán Serra P, Agramunt Lerma M, Ballestín Vicente J, et al. Factors associated with bronchiectasis in patients with COPD. Chest. 2011;140:1130–7.
Miravitlles M, Soler-Cataluña JJ, Calle M, Molina J, Almagro P, Quintano JA, et al. Spanish COPD guidelines (GesEPOC): pharmacological treatment of stable COPD. Arch Bronconeumol. 2012;48:247–57.
Miravitlles M, Marín A, Monsó E, Vilà S, de la Roza C, Hervás R, et al. Efficacy of moxifloxacin in the treatment of bronchial colonisation in COPD. Eur Respir J. 2009;34:1066–71.
Sethi S, Jones PW, Theron MS, Miravitlles M, Rubinstein E, Wedzicha JA, et al. Pulsed moxifloxacin for the prevention of exacerbations of chronic obstructive pulmonary disease: a randomized controlled trial. Respir Res. 2010;11:10.
Albert RK, Connett J, Bailey WC, Casaburi R, Cooper JAD Jr, Criner GJ, et al. Azithromycin for prevention of exacerbations of COPD. N Engl J Med. 2011;365:689–98.
Pomares X, Montón C, Espasa M, Casabon J, Monsó E, Gallego M. Long-term azithromycin therapy in patients with severe COPD and repeated exacerbations. Int J Chron Obstruct Pulmon Dis. 2011;6:449–56.
Miravitlles M, Calle M, Soler-Cataluña JJ. Clinical phenotypes of COPD: identification, definition and implications for guidelines. Arch Bronconeumol. 2012;48:86–98.
Miravitlles M, Kruesmann F, Haverstock D, Perroncel R, Choudhri SH, Arvis P. Sputum colour and bacteria in chronic bronchitis exacerbations: a pooled analysis. Eur Respir J. 2012;39:1354–60.
Ruef C. Antibiotic resistance really starts to hurt. Infection. 2011;39:499–500.
Chalupa P, Beran O, Herwald H, Kaspříková N, Holub M. Evaluation of potential biomarkers for the discrimination of bacterial and viral infections. Infection. 2011;39:411–7.
Bourbeau J, Julien M, Maltais F, Rouleau M, Beaupré A, Bégin R, et al. Reduction of hospital utilization in patients with chronic obstructive pulmonary disease: a disease-specific self-management intervention. Arch Intern Med. 2003;163:585–91.
Gadoury M-A, Schwartzman K, Rouleau M, Maltais F, Julien M, Beaupré A, et al. Self-management reduces both short- and long-term hospitalisation in COPD. Eur Resp J. 2005;26:853–7.
Stenton C. The MRC breathlessness scale. Occup Med (Lond). 2008;58:226–7.
Acknowledgments
The authors wish to thank Beatriz Viejo for the editorial support. The following investigators participated in the study: María del Carmen Aguar, Hospital de Vilanova, Valencia (Valencia); Néstor Almeida, Clínica San Roque, Las Palmas de Gran Canaria (Las Palmas); Félix Baranda, Hospital Universitario Cruces, Bilbao (Vizcaya); Marina Blanco, Hospital Universitario A Coruña (A Coruña); Myriam Calle, Hospital Clínico San Carlos, Madrid (Madrid); Francisco Casas, Hospital Clínico San Cecilio, Granada (Granada); José Celdrán, Hospital Nuestra Señora del Prado, Toledo (Toledo); Pedro Cordero, Hospital Nisa 9 de Octubre, Valencia (Valencia); Hugo Dante, Hospital Santa Bárbara, Puertollano (Ciudad Real); David de la Rosa, Clínica Platón, Barcelona (Barcelona); Gustavo de Luiz, Hospital Xanit, Benalmádena (Málaga); Cristobal Esteban, Hospital Galdakao-Usansolo, Galdakao (Vizcaya); Jesús Fernández, Hospital General Universitario de Guadalajara, Guadalajara (Guadalajara); María Ángeles Fernández, Hospital General Río Carrión, Palencia (Palencia); José Vicente Greses, Hospital Nisa 9 de Octubre, Valencia (Valencia); Lourdes Lázaro, Hospital Universitario de Burgos (Burgos); Damián Malía, Hospital General Universitario Los Arcos del Mar Menor, San Javier (Murcia); Pedro Jorge Marcos, Complexo Hospitalario de Ourense (Ourense); Esperanza Martín, Fundació Althaia, Manresa (Barcelona); Luis Molinos, Instituto Nacional de Silicosis, Oviedo (Asturias); Juan Luis Muñoz, Hospital Reina Sofía, Córdoba (Córdoba); Francisco Ortega, Hospital Universitario Virgen del Rocío, Sevilla (Sevilla); Juan Miguel Sánchez, Hospital General Universitario Morales Meseguer, Murcia (Murcia); José Gregorio Soto, Hospital de Jerez, Jerez de la Frontera (Cádiz); Joan Valdeperas, Hospital Universitari de Bellvitge, Barcelona (Barcelona). This work was supported by Bayer Hispania S.L.
Conflict of interest
Marc Miravitlles and Juan José Soler-Cataluña have received speaker fees from Bayer Hispania S.L. Félix Baranda, Pedro Cordero, and José-Vicente Greses declare that they have no conflict of interest. Cristian de la Roza is a full-time employee of Bayer Hispania S.L.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Miravitlles, M., Soler-Cataluña, J.J., Baranda, F. et al. Previous outpatient antibiotic use in patients admitted to hospital for COPD exacerbations: room for improvement. Infection 41, 361–370 (2013). https://doi.org/10.1007/s15010-012-0316-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-012-0316-8