Abstract
Background
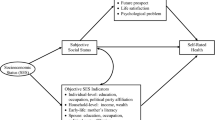
Subjective social status (SSS) predicts health outcomes independently of traditional, objective indicators of socioeconomic status (SES). However, the potential confounding and mediating effects of negative affect and similar psychosocial risk and resilience factors have not been adequately addressed through formal studies of convergent and discriminant validity of SSS measures.
Purpose
The current study provides such a test of construct validity and subsequently examines whether psychosocial factors mediate the relationship between SSS and self-rated health.
Methods
We examined the convergent and discriminant validity of the MacArthur scales of SSS relative to measures of psychosocial risk and resilience (i.e., neuroticism, depressive symptoms, optimism, and marital quality) as well as SES (i.e., income) in 300 middle-aged and older married US couples. We also tested a factor of psychosocial vulnerability as a mediator of the relationship between SSS and self-rated health.
Results
Findings indicated clear convergent and discriminant validity of the MacArthur scales. Further, controlling age and income, both the US and community measures of SSS predicted psychosocial factors for men, however, only the community measure was independently predictive for women. Psychosocial vulnerability significantly mediated the pathway between SSS and self-rated health for men and women after controlling age and income.
Conclusions
These results provide strong support for the construct validity of the MacArthur scales and provide additional evidence of the role of psychosocial risk and resilience factors as mediators of the effects of SSS on health.


Similar content being viewed by others
Notes
The main analyses reported above examined men and women separately, and therefore did not violate assumptions regarding the independence of observations by including members of couples. However, to address directly the issue of couples as participants, we also performed dyadic analysis of all participants simultaneously using Structural Equation Modeling/path analysis [41] in order to account for the dependency between husbands’ and wives’ responses. This analysis replicated all the main findings of the analyses reported above. Importantly, a model including the mediational path for Psychosocial Vulnerability linking SSS and SRH fit the data significantly better than a model in which the mediational paths were fixed to zero, for both SSSus and SSSc (χ 2 difference = 137.7 and 156.1 respectively, both p < .001). Hence, when accounting for the dependent responses of husbands and wives, the models including the mediator were a significantly better description of the data, consistent with findings when men and women were analyzed separately.
References
Adler NE, Chesney MA, Cohen S, et al. Socioeconomic status and health: the challenge of the gradient. Am Psychol. 1994;49:15–24.
Matthews K, Gallo LC, Taylor SE. Are psychosocial factors mediators of socioeconomic satus and health connections? A progress report and blueprint for the future. Ann N Y Acad Sci. 2010;1186:146–73. doi:10.1111/j.1749-6632.2009.05332.x.
Jackman MR, Jackman RW. An interpretation of the relation between objective and subjective social status. Am Sociol Rev. 1973;38:569–82.
Macleod J, Davey Smith G, Metcalfe C, Hart C. Is subjective social status a more important determinant of health than objective social status? Evidence from a prospective observational study of Scottish men. Soc Sci Med. 2005;61:1916–29.
Goodman E, Adler N, Daniels S, Morrison J, Slap G, Dolan L. Impact of objective and subjective social status on obesity in a biracial cohort of adolescents. Obes Res. 2003;11:1018–26.
Hu P, Adler NE, Goldman N, Weinstein M, Seeman TE. Relationship between subjective social status and measures of health in older Taiwanese persons. J Am Geriatr Soc. 2005;53:483–8.
Singh-Manoux A, Adler NE, Marmot MG. Subjective social status: its determinants and its association with measures of ill-health in the Whitehall II study. Soc Sci Med. 2003;56:1321–33.
Adler NE, Epel E, Castellazzo G, Ickovics J. Relationship of subjective and objective social status with psychological and physiological functioning: preliminary data in healthy white women. Heal Psychol. 2000;19:586–92.
Gallo LC, Bogart LM, Vranceanu A, Matthews KA. Socioeconomic status, resources, psychological experiences, and emotional responses: a test of the reserve capacity model. J Personal Soc Psychol. 2005;88:386–99.
Matthews KA, Räikkönen K, Gallo L, Kuller LH. Association between socioeconomic status and metabolic syndrome in women: testing the reserve capacity model. Heal Psychol. 2008;27(5):576–83.
Adler N, Singh-Manoux A, Schwartz J, Stewart J, Matthews K, Marmot MG. Social status and health: a comparison of British civil servants in Whitehall-II with European- and African-Americans in CARDIA. Soc Sci Med. 2008;66(5):1034–45.
Cohen S, Alper CM, Doyle WJ, Adler N, Treanor JJ, Turner RB. Objective and subjective socioeconomic status and susceptibility to the common cold. Heal Psychol. 2008;27(2):268–74.
Lundberg J, Kristenson M. Is subjective status influenced by psychosocial factors? Soc Indic Res. 2008;89:375–90.
Operario D, Adler NE, Williams DR. Subjective social status: reliability and predictive utility for global health. Psychol Heal. 2004;19:237–46.
Roberts BW, Kuncel NR, Shiner RL, Caspi A, Goldberg LR. The power of personality: the comparative validity of personality traits, socioeconomic status, and cognitive ability for predicting important life outcomes. Perspect Psychol Sci. 2007;2:313.
Suls J, Bunde J. Anger, anxiety, and depression as risk factors for cardiovascular disease: the problems and implications of overlapping affective dispositions. Psychol Bull. 2005;131(2):260–300.
Smith TW. Measurement in health psychology research. In: Silver R, Friedman HS, editors. Foundations of health psychology. New York: Oxford University Press; 2007. p. 19–51.
Adler NE. Health disparities through a psychological lens. Am Psychol. 2009;64(8):663–73.
Diehl M, Owen SK, Youngblade LM. Agency and communion attributes in adults’ spontaneous self-representations. Int J Behav Dev. 2004;28:1–15.
Demakakos P, Nazroo J, Breeze E, Marmot M. Socioeconomic status and health: the role of subjective social status. Soc Sci Med. 2008;67:330–40.
Steptoe A. Depression and physical illness. Cambridge: Cambridge University Press; 2007.
Gallo LC, Matthews KA. Understanding the association between socioeconomic status and physical health: do negative emotions play a role? Psychol Bull. 2003;129:10–51.
Rasmussen HN, Sheier MF, Greenhouse JB. Optimism and physical health: a meta-analytic review. Ann Behav Med. 2009;37:239–56.
Tindle HA, Chang Y, Kuller LH, et al. Optimism, cynical hostility, and incident coronary heart disease and mortality in the women’s health initiative. Circulation. 2009;120:656–62.
Taylor SE, Seeman TE, Adler NE, Marmot M, McEwen BS, Stewart J. Psychosocial resources and the SES-health relationship. Socioeconomic status and health in industrial nations: social, psychological, and biological pathways. New York: New York Academy of Sciences; 1999. p. 210–25.
Kiecolt-Glaser Jk, Newton TL. Marriage and health: his and hers. Psychol Bull. 2001;127(4):472–503.
Conger RD, Conger KJ, Martin MJ. Socioeconomic status, family processes, and individual development. J Marriage Fam. 2010;72:685–704.
Campbell DT, Fiske DW. Convergent and discriminant validation by the multitrait-multimethod matrix. Psychol Bull. 1959;56:81–105.
Idler EL, Benyamini Y. Self-rated health and mortality: a review of twenty-seven community studies. J Heal Soc Behav. 1997;3S:21–37.
Smith TW, Uchino BN, Berg CA, et al. Hostile personality traits and coronary artery calcification in middle-aged and older married couples: different effects for self-reports versus spouse-ratings. Psychosom Med. 2007;69:441–8.
Smith TW, Berg CA, Florsheim P, et al. Conflict and collaboration in middle-aged and older couples: I. Age differences in agency and communion during marital interaction. Psychol Aging. 2009;24(2):259–73.
Myers JK, Weissman MM. Use of a self-report symptom scale to detect depression in a community sample. Am J Psychiatry. 1980;137(9):1081–4.
Radloff LS, Teri L. Use of the center for epidemiological studies-depression scale with older adults. Rev Clin Gerontol. 1986;5:119–36.
Radloff LS. The CES-D scale: a self-report depression scale for research in the general population. Appl Psychol Meas. 1977;1:385–401.
Costa PT, McCrae RR. NEO-PI-R professional manual. Odessa, FL: Psychological Assessment Resources, Inc; 1992.
Scheier MF, Carver CS, Bridges MW. Distinguishing optimism from neuroticism (and trait anxiety, self-mastery, and self-esteem): a reevaluation of the Life Orientation Test. J Personal Soc Psychol. 1994;67(6):1063–78.
Locke HJ, Wallace KM. Short marital-adjustment and prediction tests: their reliability and validity. Marriage Fam Living. 1954;21:251–5.
Snyder DK, Heyman RE, Haynes SN. Evidence-based approaches to assessing couple distress. Psychol Assess. 2005;17(3):288–307.
Baron RM, Kenny DA. The moderator–mediator variable distinction in social psychological research: conceptual, strategic and statistical considerations. J Personal Soc Psychol. 1986;51:1173.
MacKinnon DP, Lockwood CM, Huffman JM, West SG, Sheets V. A comparison of methods to test the significance of the mediated effect. Psychol Methods. 2002;7:83–104.
Kenny DA, Kashy DA, Cook WL. Dyadic data analysis. New York: Guilford Press; 2006.
Heckhausen J. Developmental regulation across adulthood: primary and secondary control of age-related challenges. Dev Psychol. 1997;33(1):176–87.
Marmot M, Wilkinson RG. Psychosocial and material pathways in the relation between income and health: a response to Lynch et al. Br Med J. 2001;322(7296):1233–6.
Wilkinson RG. Socioeconomic determinants of health: health inequalities: relative or absolute material standards? Br Med J. 1997;314:591.
Helgeson VS. Gender-related traits and health. In: Suls J, Wallston K, editors. Social psychological foundations of health and illness. Oxford: Blackwell; 2003. p. 367–94.
Smith TW, Gallo LC, Goble L, Ngu LQ, Stark KA. Agency, communion, and cardiovascular reactivity during marital interaction. Heal Psychol. 1998;17(6):537–45.
Smith TW, Limon JP, Gallo LC, Ngu LQ. Interpersonal control and cardiovascular reactivity: goals, behavioral expression, and the moderating effects of sex. J Personal Soc Psychol. 1996;70(5):1012–24.
Singh-Manoux A, Marmot MG, Adler NE. Does subjective social status predict health and change in health status better than objective status? Psychosom Med. 2005;67:855–61.
Ostrove JM, Adler NE, Kuppermann M, Washington AE. Objective and subjective assessments of socioeconomic status and their relationship to self-rated health in an ethnically diverse sample of pregnant women. Heal Psychol. 2000;19:613–8.
Wolff LS, Acevedo-Garcia D, Sabramanian SV, Weber D, Kawachi I. Subjective social status, a new measure in health disparities research: do race/ethnicity and choice of reference group matter? J Health Psychol. 2010;15:560–74.
Smith TW, Gallo LC, Ruiz J. Toward a social psychophysiology of cardiovascular reactivity: Interpersonal concepts and methods in the study of psychosocial risk of cardiovascular disease. In: Suis J, Wallston K, editors. Social psychological foundations of health and illness. Weinheim: Wiley; 2003. p. 335–66.
Smith TW, Cundiff JM. Risk for coronary heart disease: an interpersonal perspective. In: Horowitz LM, Strack S, editors. Handbook of interpersonal psychology: theory, research, assessment, and therapeutic interventions. Hoboken: Wiley; 2011. p. 471–89.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cundiff, J.M., Smith, T.W., Uchino, B.N. et al. Subjective Social Status: Construct Validity and Associations with Psychosocial Vulnerability and Self-Rated Health. Int.J. Behav. Med. 20, 148–158 (2013). https://doi.org/10.1007/s12529-011-9206-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12529-011-9206-1