Abstract
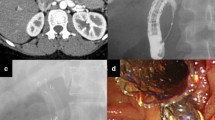
Postoperative biliary strictures are usually complications of cholecystectomy. Endoscopic plastic stent prosthesis is generally undertaken for treating benign biliary strictures. Recently, fully covered metal stents have been shown to be effective for treating benign distal biliary strictures. We present the case of a 53-year-old woman with liver injury in which imaging studies showed a common hepatic duct stricture. Endoscopic retrograde cholangiopancreatography also confirmed the presence of a common hepatic duct stricture. Temporally fully covered metal stents with dilated diameters of 6 mm were placed in a side-by-side fashion in the left and right hepatic ducts, respectively. We removed the stents 2 months after their placement. Subsequent cholangiography revealed an improvement in the biliary strictures. Although we were apprehensive about the fully covered metal stents obstructing the biliary side branches, we noted that careful placement of the bilateral metal stents did not cause any complications. Side-by-side deployment of bilateral endoscopic fully covered metal stents can be one of the safe and effective therapies for postoperative biliary stricture.




Similar content being viewed by others
References
Lillemoe KD, Melton GB, Cameron JL, et al. Postoperative bile duct strictures: management and outcome in the 1990s. Ann Surg. 2000;232:430–41.
Sugawara G, Ebata T, Yokoyama Y, et al. Management strategy for biliary stricture following laparoscopic cholecystectomy. J Hepatobiliary Pancerat Sci. 2014;21:889–95.
Bergman JJGHM, Burgemeister L, Bruno MJ, et al. Long-term follow-up after biliary stent placement for postoperative bile duct stenosis. Gastrointest Endosc. 2001;54:154–61.
Costamagna G, Boskoski I. Current treatment of benign biliary strictures. Ann Gastroenterol. 2013;26:1–4.
Costamagna G, Shah SK, Tringali A. Current management of postoperative complications and benign biliary strictures. Gastrointest Endosc Clin N Am. 2003;13:635–48.
Misra S, Melton GB, Geschwind JF, et al. Percutaneous management of bile duct strictures and injuries associated with laparoscopic cholecystectomy: a decade of experience. J Am Coll Surg. 2004;198:218–26.
Vitale GC, Tran TC, Davis BR, et al. Endoscopic management of postcholecystectomy bile duct stricture. J Am Coll Surg. 2008;206:918–23.
Weber A, Feussner H, Winkelmann F, et al. Long-term outcome of endoscopic therapy in patients with bile duct injury after cholecystectomy. J Gastroenterol Hep. 2009;24:762–9.
Kahaleh M, Behm B, Clarke BW, et al. Temporary placement of covered self-expandable metal stents in benign biliary strictures: a new paradigm? (with video). Gastrointest Endosc. 2008;67:446–54.
Garcia-Cano J. Endoscopic management of benign biliary stricture. Curr Gastroenterol Rep. 2013;15:336.
Cote GA, Slivka A, Tarnasky P, et al. Effect of covered metallic stents compared with plastic stents on benign stricture resolution. A randomized clinical trial. JAMA. 2016;315:1250–7.
Deviere J, Reddy DN, Puspok A, et al. Successful management of benign biliary strictures with fully covered self-expandable metal stents. Gastroenterol. 2014;147:385–95.
Nam HS, Kang DH. Current status of biliary metal stents. Clin Endosc. 2016;49:124–30.
Yoshida T, Hara K, Imaoka H, et al. Benefits of side-by-side deployment of 6-mm civered self-expandable metal stents for hilar malignant biliary obstructions. J Hepatobiliary Pancreat Sci. 2016;23:548–55.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Human rights
All procedures followed have been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
Informed consent
Informed consent was obtained from this patient for being included in the study.
Rights and permissions
About this article
Cite this article
Kaino, S., Sen-yo, M., Shinoda, S. et al. Side-by-side placement of bilateral endoscopic metal stents for the treatment of postoperative biliary stricture. Clin J Gastroenterol 10, 68–72 (2017). https://doi.org/10.1007/s12328-016-0694-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12328-016-0694-z