Abstract
Background
Contrast extravasation (CE) in spontaneous intracerebral hemorrhage (ICH), coined the spot sign, predicts hematoma expansion (HE) and poor clinical outcome. The dynamic relationship between CE and the mode of ICH growth are poorly understood. We characterized the in vivo pattern and rate of HE using a novel animal model of acute ICH.
Methods
Basal ganglia ICH was created in 14 Yorkshire swine utilizing a novel MRI integrated model, permitting real-time CE observation using dynamic contrast-enhanced (DCE) MRI. Computerized planimetry measured CE volume at each time point. Spatial vector analysis along three orthogonal axes determined distance vectors. Maximizing and minimizing the coefficient of determination defined the temporal phases of growth and stability, respectively. CE rate was calculated using a Patlak model.
Results
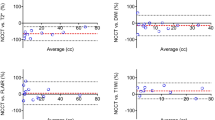
Asymmetric growth and variable rates of expansion characterized HE defining three distinct growth phases and patterns. A primary growth phase (duration 160 s; IQR 50–130) demonstrated rapid linear growth (0.04 mm/s IQR 0.01–0.10) accounting for 85 ± 15 % of total HE. The stationary phase demonstrated stability (duration 145 s; IQR 0–655). A secondary growth phase (duration 300; 130–600 s) accounted for 23 ± 8 % of total HE. In the primary and secondary growth phase, asymmetric growth occurred in the anterior–posterior (AP) planes (0.056 mm/s; p = 0.026 and 0.0112 mm/s; p = 0.03). Monophasic 2 (14 %), biphasic 4 (35 %) (primary followed by secondary growth), and triphasic 8 (56 %) patterns (primary, stationary, and secondary growth phase) were observed.
Conclusions
A novel model of ICH provides real-time study of the dynamics and rate of CE. This data facilitates the understanding of pattern and rate of ICH formation.

Similar content being viewed by others
References
Morgenstern LB, et al. Guidelines for the management of spontaneous intracerebral hemorrhage: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2010;41(9):2108–29.
Dowlatshahi D, et al. Defining hematoma expansion in intracerebral hemorrhage: relationship with patient outcomes. Neurology. 2011;76(14):1238–44.
Bermejo PG, et al. Spot sign and live-imaged dramatic intracerebral hematoma expansion. Neurology. 2010;75(9):834.
Jeong D, Jhaveri MD, Prabhakaran S. Magnetic resonance imaging characteristics at onset of spontaneous intracerebral hemorrhage. Arch Neurol. 2011;68(6):826–7.
Rizos T, et al. Ongoing intracerebral bleeding despite hemostatic treatment associated with a spot sign in a patient on oral anticoagulation therapy. Cerebrovasc Dis. 2009;28(6):623–4.
Fisher CM. Pathological observations in hypertensive cerebral hemorrhage. J Neuropathol Exp Neurol. 1971;30(3):536–50.
Greenberg CH, et al. Modeling intracerebral hemorrhage growth and response to anticoagulation. PLoS One. 2012;7(10):e48458.
Mayer SA. Ultra-early hemostatic therapy for intracerebral hemorrhage. Stroke. 2003;34(1):224–9.
Wada R, et al. CT angiography “spot sign” predicts hematoma expansion in acute intracerebral hemorrhage. Stroke. 2007;38(4):1257–62.
Demchuk AM, et al. Prediction of haematoma growth and outcome in patients with intracerebral haemorrhage using the CT-angiography spot sign (PREDICT): a prospective observational study. Lancet Neurol. 2012;11(4):307–14.
d’Esterre CD, et al. Early rate of contrast extravasation in patients with intracerebral hemorrhage. AJNR Am J Neuroradiol. 2011;32(10):1879–84.
Dowlatshahi D, et al. Ongoing bleeding in acute intracerebral haemorrhage. Lancet. 2013;381(9861):152.
Koculym A, et al. CT perfusion spot sign improves sensitivity for prediction of outcome compared with CTA and postcontrast CT. AJNR Am J Neuroradiol. 2013;34(5):965–70 (S1).
Aviv RI, et al. An in vivo, MRI-integrated real-time model of active contrast extravasation in acute intracerebral hemorrhage. AJNR Am J Neuroradiol. 2014;35(9):1693–9. doi:10.3174/ajnr.A3939.
Roberts HC, et al. Correlation of microvascular permeability derived from dynamic contrast-enhanced MR imaging with histologic grade and tumor labeling index: a study in human brain tumors. Acad Radiol. 2001;8(5):384–91.
Chakraborty S, et al. Dynamic nature of the CT angiographic “spot sign”. Br J Radiol. 2010;83(994):e216–9.
Boulouis G, et al. Anatomic pattern of intracerebral hemorrhage expansion: relation to CT angiography spot sign and hematoma center. Stroke. 2014;45(4):1154–6.
Edlow BL, et al. The pattern and pace of hyperacute hemorrhage expansion. Neurocrit Care. 2012;17(2):250–4.
San Millan Ruiz D, et al. The perianeurysmal environment: influence on saccular aneurysm shape and rupture. AJNR Am J Neuroradiol. 2006;27(3):504–12.
Biffi A, et al. APOE genotype and extent of bleeding and outcome in lobar intracerebral haemorrhage: a genetic association study. Lancet Neurol. 2011;10(8):702–9.
Brouwers HB, et al. Apolipoprotein E genotype is associated with CT angiography spot sign in lobar intracerebral hemorrhage. Stroke. 2012;43(8):2120–5.
Mayer SA, et al. Efficacy and safety of recombinant activated factor VII for acute intracerebral hemorrhage. N Engl J Med. 2008;358(20):2127–37.
Acknowledgments
Dr Aviv was supported by the Heart and stroke foundation of Ontario.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Liu, R., Huynh, T.J., Huang, Y. et al. Modeling the Pattern of Contrast Extravasation in Acute Intracerebral Hemorrhage Using Dynamic Contrast-Enhanced MR. Neurocrit Care 22, 320–324 (2015). https://doi.org/10.1007/s12028-014-0071-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-014-0071-z