Abstract
Purpose of review
The objective of this study is to answer few key questions in order to establish the best possible available diagnostic strategy for incidentally discovered pancreatic cystic lesions (PCLs).
Recent findings
Advances in EUS-guided sampling techniques, cross-sectional and intracystic confocal imaging, molecular biomarkers analysis, determination of cyst fluid glucose, and artificial intelligence, appear to be associated with an improved diagnostic accuracy in distinguishing mucinous from non-mucinous PCLs.
Summary
The diagnostic process has the aim of recognizing cysts with malignant potential and identifying those with high-risk stigmata and/or worrisome features. Clinicians should avoid performance of unnecessary tests from one side and misdiagnosis from the other, which can easily result in inadvertent surgery of an otherwise benign lesion or malignant progression of a precancerous cyst. Clinical studies to validate recent reported results utilizing novel diagnostic tests are needed, in order to gradually incorporate and combine them into updated guidelines.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Pancreatic cystic lesions (PCLs) include a broad spectrum of entities, which greatly differ in their malignant potential. Among all incidentally discovered PCLs that can undergo malignant transformation or be malignant at presentation, the most frequently encountered are intraductal papillary mucinous neoplasms (IPMNs), while mucinous cystic neoplasms (MCNs), cystic pseudopapillary neoplasms, and cystic pancreatic neuroendocrine neoplasms are infrequently diagnosed. Conversely, inflammatory pseudocysts and the rarely encountered retention cysts, cystic lymphangiomas, duplication cysts, ciliated foregut cysts, or lymphoepithelial cysts have no malignancy potential. Finally, serous cystic adenomas (SCA) are considered benign entities, even though rare cases of malignant transformation have been described [1].
Widespread use of imaging modalities, such as abdominal ultrasound (US), computed tomography (CT), and magnetic resonance imaging (MRI), has led, over the last years, to an exponential increase in the incidental detection of asymptomatic PCLs [2, 3•]. Proper diagnostic approach is fundamental to distinguish cysts potentially malignant from non-malignant cysts and to guide subsequent management. In the present review, we will answer few key questions necessary to establish the best possible available diagnostic strategy for incidentally discovered PCLs.
Epidemiological data
Epidemiological data represent the foundation to formulate key questions on how to approach newly diagnosed PCLs. In a recent meta-analysis, pooled prevalence of incidentally discovered PCLs was 8% (95%CI 4–14%), with considerable heterogeneity among different studies (I2 = 99.5%) [3•]. Real-life distribution of pancreatic cyst cases clearly emerges from a prospective Italian registry, which enrolled 1385 consecutive PCL patients. The vast majority (70.1%) had branch duct IPMN, 6.2% mixed-type IPMN, 4.6% main duct IPMN, 12.7% SCA, 2.8% MCN, 1.5% cystic neuroendocrine neoplasm, 0.7% solid-pseudopapillary cystic neoplasm, 0.3% cystic adenocarcinoma, and 1.2% an undetermined cystic neoplasm [4•]. Only a small proportion of these patients (5.7%) underwent surgery after the initial workup, suggesting that more invasive workup should be initially limited to a small proportion of incidentally discovered PCLs, with surveillance playing a major role in the majority of them [4•]. Based on the above epidemiological distribution, considering that MCNs are rare and with a characteristic localization and female preponderance, a unilocular or oligocystic lesion should be considered a side-branch IPMN until proven otherwise. Looking at surgical series, however, it appears that the number of patients with totally benign unilocular or oligocystic SCA who erroneously underwent surgery is still significant [5,6,7,8]. This phenomenon reflects the difficulty in distinguishing mucinous from non-mucinous cysts. Thus, when facing a newly detected PCL, there are some questions that need to be answered:
-
1.
Are the diagnostic imaging studies performed of enough quality to distinguish mucinous from non-mucinous PCLs, and if not, which and when additional tests should be ordered?
-
2.
In case additional tests fail to distinguish mucinous from non-mucinous PCLs, what else should be done to make this distinction more clear?
-
3.
Are the performed tests of sufficient accuracy to rule out presence of high-risk stigmata and/or worrisome features in large unilocular/oligocystic PCLs, once frank malignancy has been ruled out?
Are the diagnostic imaging studies performed of enough quality to distinguish mucinous from non-mucinous PCLs, and if not, which and when additional tests should be ordered?
Multiple guidelines have been published on the diagnostic approach to PLCs [9,10,11,12,13], but no one has clearly answered this important issue. The answer to this question starts from asking if subsequent imaging modalities would change the decision-making process. When CT/MRI imaging tests disclose presence of multifocal cystic disease, the pre-test probability for a diagnosis of IPMN is extremely high, and unless a large lesion is present, no further diagnostic workup is necessary. This approach can also be adopted for single lesions < 2 cm, where a more appropriate imaging modality, when needed, can be ordered at the subsequent surveillance visit. Conversely, when a > 2 cm lesion is first detected, alone or in the context of a multifocal disease, differentiation between mucinous and non-mucinous disease becomes mandatory. Indeed, association of unilocular SCA in the context of multifocal side-branch IPMN has been described and has occurred multiple times in our experience [14]. Conversely, diagnosis of a > 2 cm IPMN, especially in young/middle-aged patients, will require a more strict surveillance and an attempt to establish a more precise diagnosis.
New advances in cross-sectional imaging have dramatically improved image quality for pancreas evaluation, a fact responsible for the cyst pandemia we are observing [2]. The most important finding to investigate is the presence of communication of the cyst with the main pancreatic duct (MPD), which when present strongly indicate side-branch IPMN [15•]. Endoscopic retrograde pancreatography (ERP), best test to assess this task, has been abandoned because of the high risk for adverse events (AEs). Among imaging studies, new-generation dedicated pancreatic protocol CT and pancreatic MRI/MRCP have similar accuracy for characterization of PCLs, while MRI/MRCP seems more sensitive than CT for identifying communication between PCLs and the pancreatic ductal system [15•]. Moreover, MRI/MRCP is not associated with radiation exposure and therefore should also be utilized for surveillance purposes, making this test the preferred one to first re-evaluate newly diagnosed PCLs, with the characteristics described above.
In case additional tests fail to distinguish mucinous from non-mucinous PCLs, what else should be done to make this distinction more clear?
Pancreatic cystic lesions, in which a distinction between a mucinous and non-mucinous nature could not be reached by imaging modalities, are defined as indeterminate cysts. At this stage even though more invasive than cross-sectional imaging studies, endoscopic ultrasound (EUS) examination with different acquisition techniques becomes appropriate.
EUS-guided cyst fluid sampling is regarded as a safe diagnostic procedure with an overall morbidity and associated mortality of 2.66% and 0.19%, respectively [16]. The most accurate cyst fluid biochemical marker in differentiating mucinous from non-mucinous PCLs is the carcinoembryonic antigen (CEA). The proposed cutoff value of 192 ng/mL, however, has suboptimal sensitivity (52–78%) and specificity (63–91%) for making such a differentiation [10, 17]. Conversely, when very low (< 5 ng/mL), CEA has 50% sensitivity and 95% specificity for a pseudocyst or SCA, while very high CEA levels (> 800 ng/mL) have 48% sensitivity and 98% specificity for mucinous cysts [18, 19].
Glucose determination in the cystic fluid has recently been added, and low levels (≤ 50 mg/dL) are extremely sensitive (88–94%), specific (92–96%), and accurate (90–95%), in identifying mucinous pancreatic cysts [20,21,22]. In a systematic review and meta-analysis, including eight studies and 609 lesions, intra-cystic glucose determination showed a significantly higher sensitivity (91% vs. 56%; p < 0.001) and diagnostic accuracy (94% vs. 85%; p < 0.001) in differentiating mucinous from non-mucinous PCLs, compared to CEA [23•]. This value can be easily obtained just after cyst fluid collection using a glucometer and combined with CEA levels might bring a slightly more increased sensitivity in differentiating PCLs [20, 24].
Reports of cyst fluid molecular analysis to detect different genetic mutations, protein expression, glycoproteomics, and metabolomic profiling have become available. Multiple studies have evaluated genetic molecular markers associated with identification of different PCL types (Table 1) [25,26,27,28], which might become a useful tool to reach a more accurate diagnosis. One of these landmark studies has been published in 2015, where 130 PCL patients prospectively enrolled after EUS-FNA underwent surgical resection. Multiple markers for identification of different cyst types were identified. Absence of a KRAS, GNAS, or RNF43 mutation, or absence of aneuploidy in chromosome 5p or 8p, identified SCAs with 100% sensitivity and 91% specificity. Absence of chromosome 3 loss of heterozygosity (LOH), CTNNB1, or GNAS mutations, or aneuploidy in chromosome 1q or 22q, identified MCNs with 100% sensitivity and 75% specificity. Finally, mutation in either GNAS or RNF43, LOH in chromosome 9, or aneuploidy in chromosome 1q or 8p was consistent for IPMNs, with 76% sensitivity and 97% specificity [25].
A recent meta-analysis on six studies and 785 lesions suggested that combination of cyst fluid KRAS and GNAS mutations was accurate for the diagnosis of mucinous cystic lesions and IPMNs, better than CEA [29]. The authors estimated that if cyst fluid KRAS/GNAS mutational testing is negative, post-test probability that the patient has an IPMN or a mucinous cystic neoplasm would be approximately 2% and 8%, respectively [29]. Moreover, in a concomitant study on 1290 patients, addition of molecular analysis to the standard workup improved concordance between preoperative and final histopathological PCLs diagnosis in up to 91% of cases [8].
Proteomic profiling on cyst fluid in 91 patients by using mass spectrometry reported significantly differential abundance of 32 peptides and 33 proteins (p ≤ 0.05) in at least one of the five different cyst type groups, and 19 proteins appeared to be unique to a given cyst type [30]. Nine proteins were found to be differentially expressed in mucinous vs. non-mucinous lesions, and a combination of four of them (AFM, REG1A, LCN2, PIGR) identified mucinous lesions with 81% sensitivity, 90% specificity, and 86% accuracy [31]. Performance of metabolic profiling by untargeted mass spectrometry and quantitative nuclear magnetic resonance in 24 surgically resected specimens reported cyst fluid 5-oxoproline (p = 0.01) to differentiate mucinous from non-mucinous PCLs, with 90% accuracy, better than cyst fluid glucose (82% accuracy) [32].
The most recent ACG clinical guideline introduced cyst fluid molecular analysis to be considered in cases of unclear diagnosis to help identify IPMNs and MCNs [9]. However, this was rated as a conditional recommendation, with a very low quality of evidence. We strongly believe that all these tests seem more research tools, with still a limited utility to distinguish unilocular/oligocystic IPMN from SCA or other benign cyst types, a scarce widespread applicability, and costs that remain a major issue to their everyday utilization.
A through‑the‑needle microforceps biopsy (TTNB) device (Moray™ microforceps, Steris, Mentor, OH, USA), which can be inserted into the cyst through a previously placed 19-gauge needle, has been developed to collect samples from PCLs’ wall for histological examination. A meta-analysis on 11 studies and 518 patients reported a 79.6% diagnostic yield and 82.8% diagnostic accuracy [33•], significantly better compared to that of standard cyst fluid analysis. A mean of 2.47 ± 0.92 forceps passes was performed. Interobserver agreement performed among six expert pathologists on the blinded interpretation of TTNB collected biopsy specimens showed a moderate to substantial agreement for the ability to make a specific diagnosis (Gwet’s AC1 62%; 95% CI, 57–67%) and substantial agreement (Gwet’s AC1, 65%; 95% CI, 59–70%) for differentiating mucinous cysts from all the other diagnoses [34].
One of the main concerns of cyst wall biopsy is the occurrence of adverse events (AEs). In the abovementioned meta-analysis, severe AEs were encountered in 1.1% of cases [33•]. Other non-severe AEs reported in studies were intracystic hemorrhage (26/463 cases, 5.6%) and mild acute pancreatitis (11/463 cases, 2.4%) [35]. In the most recent prospective study, among 101 consecutive PCL patients enrolled in a single academic center, AEs were observed in 10 patients (9.9%) [36•], with acute pancreatitis occurring in nine cases. Four AEs were rated as severe, with one fatal outcome. The procedure changed clinical management in only 11.9% of cases, thus questioning from one side its utility and from the other proper patients’ selection. A strategy of perioperative hydration with Ringer’s lactate and rectal diclofenac administration was started after the first severe AE, without a statistical reduction in AEs [36•]. The lessons learned from this latter study were that (i) prophylaxis for acute pancreatitis with rectal diclofenac should probably be utilized for EUS-TTNB procedures and (ii) patient selection should be strict and limited to those in whom sampling of cyst walls has a high probability to change their management (Fig. 1).
Virtual histological images of the inner wall of PCLs can be obtained with needle-based confocal laser endomicroscopy (nCLE) (AQ-Flex nCLE miniprobe, Cellvizio, Mauna Kea Technologies, Paris, France). The miniprobe is inserted into the cyst through a standard 19-gauge FNA needle. Its feasibility and safety have been demonstrated by two prospective studies [37, 38•]. In one of this multicenter study including 175 patients with a conclusive diagnosis, the novel developed criteria to distinguish different PCL types showed 95% sensitivity and 100% specificity in differentiating SCAs from mucinous PCLs [37]. Similar nCLE performance has been reported in a study involving 144 patients with suspected PCLs greater than 20 mm, of whom 65 underwent surgical resection [38•]. Sensitivity, specificity, and accuracy were much higher than using combined CEA measurement and cytology determination.
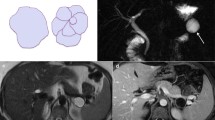
A recent consensus statement established that EUS-guided nCLE improves evaluation of PCLs and has a positive impact on patient management [39]. This technology, however, requires a specific structured training for a competent application and additional aspects, such as procedural costs and assessment of criteria for malignancy need to be defined (Fig. 2).
Confocal endomicroscopy images from PCLs; A branch-duct IPMN (papillae with epithelial border in gray with black fine line in the periphery and white center corresponding to the vascular core filled with fluorescein); B serous cystadenoma (tortuous and interconnected vessels with fluorescein appearing white and red cells inside appearing as black points) (courtesy of Bertrand Napoleon MD)
Are the performed tests of sufficient accuracy to rule out presence of high-risk stigmata and/or worrisome features in large-sized unilocular/oligocystic PCLs?
Enhancing mural nodules and thickened walls/septa are the findings that need to be searched for when assessing the presence of high-risk stigmata and/or worrisome features in unilocular/oligocystic PCLs [40, 41], once frank malignancy has been ruled out by cross-sectional imaging. In a systematic review including 70 studies and 2297 resected IPMNs, the presence of mural nodules had a positive predictive value for malignancy of 62.2%, revealing a considerable effect of their size on predicting both invasive carcinoma and high-grade dysplasia [42]. The 8 mm cutoff was the most accurate, with a sensitivity of 100% and a specificity of 86% [42]. Performance of high-resolution CT and MRI in recognition of mural nodules and distinguishing between benign and malignant unilocular/oligocystic PCLs seems comparable, as recently reported in a meta-analysis [43], even though other data suggested MRI to be superior than CT [44].
When doubts about the presence of mural nodules and worrisome features on cross-sectional imaging remain, contrast-enhanced EUS (CE-EUS) should be performed because of its ability to distinguish hyperenhancing solid components within PCLs, from non-enhancing mucus plugs [45, 46]. Indeed, in a prospective study on 90 PCL patients, CE-EUS was more valuable for precise identification of mural nodules compared to CT (p = 0.018) and MRI (p = 0.033) [47]. Similar results have been found for detection of septal thickness [48]. Pooled sensitivity, specificity, and diagnostic accuracy of CE-EUS for identification of high-grade dysplasia were found to be 88.2%, 79.1%, and 89.6%, in a systematic review including ten studies and 532 patients [49•] (Fig. 3).
Once mural nodules are identified, EUS-FNA seems as a logical next step in order to better classify high-risk cysts. Lim et al. considered mural nodules like a neoplastic lesion and showed a 78% diagnostic yield for EUS-guided fine-needle aspiration (FNA), when more than one needle pass (vs. 44% with one pass, p = 0.016) was performed [50]. These results were confirmed in another study where cytology was diagnostic in 89.6% of patients with worrisome features, while no diagnostic benefit over radiologic findings alone was found if no such imaging findings were present [51].
There is, however, no consensus between different guidelines on the use of EUS-FNA in the diagnosis of high-risk PCLs. Two American guidelines (AGA and ASGE) [12, 52] recommend EUS‑FNA and use it to direct patients after a high‑risk cytology result to surgery, while apparently low‑risk lesions can be followed up with no recommendation to perform EUS-FNA. On the other hand, the Japanese guideline does not recommend routinely cyst sampling and address cysts of any size with worrisome features directly to surgery [11]. In comparison with the former, the revised Fukuoka guideline leads to a greater number of benign resections, but fewer missed advanced lesions [53,54,55]. Perhaps the best approach is the one proposed by the European evidence-based guidelines on PCLs, where EUS-FNA was recommended to be carried out after CE-EUS only when the results were expected to change clinical management [10]. In fact, an important drawback of EUS-FNA to take into consideration is the theoretical risk for seeding of malignant cells [56], even though a study showed no difference of peritoneal seeding between 175 resected IPMNs with a preoperative EUS‑FNA compared with 68 patients with no preoperative tissue sampling [57]. In our practice, we usually send patients with high-risk stigmata or worrisome features directly to surgery, reserving EUS-guided fine-needle biopsy (FNB) to those with high surgical risk in whom experimental treatments, such as EUS-guided radiofrequency ablation, are offered.
Regarding cyst fluid molecular tests, studies published before 2018 have suggested that detection of certain gene mutations or loss of heterozygosity could be able to differentiate benign from malignant cysts, with high sensitivity and specificity for the presence of high-grade dysplasia or invasive adenocarcinoma [25, 58, 59] (see Table 1). Similar results have been reported for untargeted mass spectrometry and quantitative nuclear magnetic resonance [60].
Given the presumed need for multimodal testing, with multiple variables to be computed, artificial intelligence (AI) is expected to play a major role in the proper differentiation of PCLs, as proven by a proof-of-concept study, where AI using deep learning and based on a number of cyst variables predicted cyst malignancy with a sensitivity, specificity, and accuracy of 95.7%, 91.9%, and 92.9%, respectively, much better than any other test [61].
Conclusions
Increased incidental detection of PCLs, with a potential for harboring or developing malignancy, imposes an accurate baseline diagnostic evaluation strategy to stratify PCL patients into a management decision algorithm (Fig. 4). This process should avoid performance of unnecessary tests from one side and misdiagnosis from the other side, which can easily result in malignant progression of a precancerous cyst or inadvertent surgery of an otherwise benign lesion.
Proposed algorithm for the diagnostic workup of incidentally discovered PCLs; #Mucinous cysts comprise IPMNs and MCNs; *worrisome features, enhancing mural cyst nodule < 5 mm; thickened or enhancing cyst walls or septa; MRCP, magnetic resonance cholangio-pancreatography; EUS, endoscopic ultrasound; TTNB, through-the-needle biopsy; FNB, fine-needle biopsy
Recent advances in EUS-guided sampling techniques, cross-sectional and intracystic confocal imaging, molecular biomarkers analysis, determination of cyst fluid glucose, and artificial intelligence, appear to be associated with an improved diagnostic accuracy for these lesions. However, better clinical studies to validate these initial results are needed, in order to gradually incorporate these novel tests and combine available tests into future guidelines.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Slobodkin I, Luu AM, Höhn P, Fahlbusch T, Tannapfel A, Uhl W, et al. Is surgery for serous cystic neoplasms of the pancreas still indicated? Sixteen years of experience at a high-volume center. Pancreatology. 2021;21:983–9.
Salom F, Prat F. Current indications and yield of endoscopic ultrasound and ancillary techniques in pancreatic cystic neoplasms. Clin J Gastroenterol. 2019;12:93–101.
• Zerboni G, Signoretti M, Crippa S, Falconi M, Arcidiacono PG, Capurso G. Systematic review and meta-analysis: prevalence of incidentally detected pancreatic cystic lesions in asymptomatic individuals. Pancreatology. 2019;19:2-9. Systematic review on 17 studies and 48,860 individuals showing an 8% prevalence of incidentally discovered pancreatic cystic lesions
• Pezzilli R, Buscarini E, Pollini T, Bonamini D, Marchegiani G, Crippa S, et al. Epidemiology, clinical features and diagnostic work-up of cystic neoplasms of the pancreas: interim analysis of the prospective PANCY survey. Dig Liver Dis. 2020;52:547-54. Prospective study offering a reliable real-life epidemiology picture of the pancreatic cystic lesions.
Goh BKP, Park RHS, Koh YX, Teo JY, Tan EK, Cheow PC, et al. Changing trends in the clinicopathological features, practices and outcomes in the surgical management for cystic lesions of the pancreas and impact of the international guidelines: single institution experience with 462 cases between 1995–2018. Pancreatology. 2020;20:1786–90.
Sun L, Wang W, Wang Y, Jiang F, Peng L, Jin G, et al. Validation of European evidence-based guidelines and American College of Gastroenterology guidelines as predictors of advanced neoplasia in patients with suspected mucinous pancreatic cystic neoplasms. J Gastroenterol Hepatol. 2020;35:1644–51.
Sun L, Wang W, Zhu H, Jiang F, Peng L, Jin G, et al. High-risk characteristics associated with advanced pancreatic cystic lesions: results from a retrospective surgical cohort. Dig Dis Sci. 2021;66:2075–83.
Roldán J, Harrison JM, Qadan M, Bolm L, Baba T, Brugge WR, et al. “Evolving trends in pancreatic cystic tumors: a 3-decade single-center experience with 1290 resections”. Ann Surg 2021 Aug 4. https://doi.org/10.1097/SLA.0000000000005142. Epub ahead of print.
Elta GH, Enestvedt BK, Sauer BG, Lennon AM. ACG clinical guideline: diagnosis and management of pancreatic cysts. Am J Gastroenterol. 2018;113:464–79.
European Study Group on Cystic Tumours of the Pancreas. European evidence-based guidelines on pancreatic cystic neoplasms. Gut. 2018;67:789–804.
Tanaka M, Fernández-Del Castillo C, Kamisawa T, Jang JY, Levy P, Ohtsuka T, et al. Revisions of international consensus Fukuoka guidelines for the management of IPMN of the pancreas. Pancreatology. 2017;17:738–53.
ASGE Standards of Practice Committee, Muthusamy VR, Chandrasekhara V, Acosta RD, Bruining DH, Chathadi KV, et al. The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms. Gastrointest Endosc. 2016;84:1‑9.
Lee ES, Kim JH, Yu MH, Choi SY, Kang HJ, Park HJ, et al. Diagnosis and surveillance of incidental pancreatic cystic lesions: 2017 Consensus Recommendations of the Korean Society of Abdominal Radiology. Korean J Radiol. 2019;20:542–57.
Chahal P, Saad AJ, Jeyarajah RD. An unusual case of a coexistent serous cystadenoma and intraductal papillary mucinous neoplasm of pancreas. EUS to the rescue! JOP. 2011;12:244–6.
• Udare A, Agarwal M, Alabousi M, McInnes M, Rubino JG, Marcaccio M, et al. Diagnostic accuracy of MRI for differentiation of benign and malignant pancreatic cystic lesions compared to CT and endoscopic ultrasound: systematic review and meta-analysis. J Magn Reson Imaging 2021;54:1126-37. Systematic review evaluating and comparing the diagnostic accuracy of MRI for differentiating malignant from benign pancreatic cystic lesions.
Zhu H, Jiang F, Zhu J, Du Y, Jin Z, Li Z. Assessment of morbidity and mortality associated with endoscopic ultrasound-guided fine-needle aspiration for pancreatic cystic lesions: a systematic review and meta-analysis. Dig Endosc. 2017;29:667–75.
Ngamruengphong S, Lennon AM. Analysis of pancreatic cyst fluid. Surg Pathol Clin. 2016;9:677–84.
Kaplan JH, Gonda TA. The use of biomarkers in the risk stratification of cystic neoplasms. Gastrointest Endosc Clin N Am. 2018;28:549–68.
van der Waaij LA, van Dullemen HM, Porte RJ. Cyst fluid analysis in the differential diagnosis of pancreatic cystic lesions: a pooled analysis. Gastrointest Endosc. 2005;62:383–9.
Simons‑Linares CR, Bhatt A, Jang S, Bhatt A, Jang S, El-Khider F, et al. The utility of intracystic glucose levels in differentiating mucinous from non‑mucinous pancreatic cysts. Gastroenterol. 2018;154:S‑43.
Carr RA, Yip-Schneider MT, Simpson RE, Dolejs S, Schneider JG, Wu H, et al. Pancreatic cyst fluid glucose: rapid, inexpensive, and accurate diagnosis of mucinous pancreatic cysts. Surgery. 2018;163:600–5.
Ribaldone DG, Bruno M, Gaia S, Cantamessa A, Bragoni A, Caropreso P, et al. Differential diagnosis of pancreatic cysts: a prospective study on the role of intra-cystic glucose concentration. Dig Liver Dis. 2020;52:1026–32.
• McCarty TR, Garg R, Rustagi T. Pancreatic cyst fluid glucose in differentiating mucinous from nonmucinous pancreatic cysts: a systematic review and meta-analysis. Gastrointest Endosc 2021;94:698-712.e6. Systematic review showing low cyst fluid glucose to be associated with significantly improved diagnostic accuracy compared with CEA alone for differentiation mucinous vs. non-mucinous pancreatic cystic lesions.
Figueiredo M, Zaarour A, Eisendrath P. Intracystic glucose and CEA measurement: a quick tool for diagnosing mucinous pancreatic cysts. Endoscopy 2018;50:eP180V.
Springer S, Wang Y, Dal Molin M, Masica DL, Jiao Y, Kinde I, et al. A combination of molecular markers and clinical features improve the classification of pancreatic cysts. Gastroenterology. 2015;149:1501–10.
Wu J, Jiao Y, Dal Molin M. Whole-exome sequencing of neoplastic cysts of the pancreas reveals recurrent mutations in components of ubiquitin-dependent pathways. Proc Natl Acad Sci USA. 2011;108:21188–93.
Amato E, Molin MD, Mafficini A, Yu J, Malleo G, Rusev B, et al. Targeted next-generation sequencing of cancer genes dissects the molecular profiles of intraductal papillary neoplasms of the pancreas. J Pathol. 2014;233:217–27.
Sakhdari A, Moghaddam PA, Ok CY, Walter O, Tomaszewicz K, Caporelli ML, et al. Somatic molecular analysis augments cytologic evaluation of pancreatic cyst fluids as a diagnostic tool. Oncotarget. 2019;10:4026–37.
McCarty TR, Paleti S, Rustagi T. Molecular analysis of EUS-acquired pancreatic cyst fluid for KRAS and GNAS mutations for diagnosis of intraductal papillary mucinous neoplasia and mucinous cystic lesions: a systematic review and meta-analysis. Gastrointest Endosc. 2021;93:1019-33.e5.
Paziewska A, Polkowski M, Rubel T, Karczmarski J, Wiechowska-Kozlowska A, Dabrowska M, et al. Mass spectrometry-based comprehensive analysis of pancreatic cyst fluids. Biomed Res Int. 2018;2018:7169595.
Park J, Yun HS, Lee KH, Lee KT, Lee JK, Lee SY. Discovery and validation of biomarkers that distinguish mucinous and non-mucinous pancreatic cysts. Cancer Res. 2015;75:3227–35.
Shi J, Yi Z, Jin L, Zhao L, Raskind A, Yeomans L, et al. Cyst fluid metabolites distinguish malignant from benign pancreatic cysts. Neoplasia. 2021;23:1078–88.
• McCarty T, Rustagi T. Endoscopic ultrasound-guided through-the-needle microforceps biopsy improves diagnostic yield for pancreatic cystic lesions: a systematic review and meta-analysis. Endosc Int Open 2020;8:E1280-90. Systematic review showing the diagnostic performances of EUS-guided through-the-needle biopsy for pancreatic cystic lesions.
Larghi A, Manfrin E, Fabbri C, Crinò SF, Correale L, Chiarello G, et al. Interobserver agreement among expert pathologists on through-the-needle microforceps biopsy samples for evaluation of pancreatic cystic lesions. Gastrointest Endosc. 2019;90:784-92.e4.
Balaban VD, Cazacu IM, Pinte L, Jinga M, Bhutani MS, Saftoiu A. EUS-through-the-needle microbiopsy forceps in pancreatic cystic lesions: a systematic review. Endosc Ultrasound. 2021;10:19–24.
• Kovacevic B, Klausen P, Rift CV, Toxværd A, Grossjohann H, Karstensen JG, et al. Clinical impact of endoscopic ultrasound-guided through-the-needle microbiopsy in patients with pancreatic cysts. Endoscopy 2021;53:44-52. Large prospective study reporting 4% severe adverse events, including 1% fatality, from EUS-guided through-the-needle microbiopsy in patients with pancreatic cystic lesions.
Napoleon B, Palazzo M, Lemaistre AI, Caillol F, Palazzo L, Aubert A, et al. Needle-based confocal laser endomicroscopy of pancreatic cystic lesions: a prospective multicenter validation study in patients with definite diagnosis. Endoscopy. 2019;51:825–35.
• Krishna SG, Hart PA, Malli A, Kruger AJ, McCarthy ST, El-Dika S, et al. Endoscopic ultrasound-guided confocal laser endomicroscopy increases accuracy of differentiation of pancreatic cystic lesions. Clin Gastroenterol Hepatol 2020;18:432-440.e6. Prospective study showing needle-based confocal laser endomicroscopy to identify mucinous cysts with greater accuracy than measurement of CEA and fluid cytology.
Napoleon B, Krishna SG, Marco B, Carr-Locke D, Chang KJ, Ginès À, et al. Confocal endomicroscopy for evaluation of pancreatic cystic lesions: a systematic review and international Delphi consensus report. Endosc Int Open. 2020;8:E1566–81.
Faias S, Cravo M, Pereira da Silva J, Chaves P, Dias Pereira A. Endoscopic ultrasound with fine needle aspiration is useful in pancreatic cysts smaller than 3 cm. BMC Gastroenterol. 2020;20:413.
Wong J, Weber J, Centeno BA, Vignesh S, Harris CL, Klapman JB, et al. High-grade dysplasia and adenocarcinoma are frequent in side-branch intraductal papillary mucinous neoplasm measuring less than 3 cm on endoscopic ultrasound. J Gastrointest Surg. 2013;17:78–84; discussion p.84–5.
Marchegiani G, Andrianello S, Borin A, Dal Borgo C, Perri G, Pollini T, et al. Systematic review, meta-analysis, and a high-volume center experience supporting the new role of mural nodules proposed by the updated 2017 international guidelines on IPMN of the pancreas. Surgery. 2018;163:1272–9.
Liu H, Cui Y, Shao J, Shao Z, Su F, Li Y. The diagnostic role of CT, MRI/MRCP, PET/CT, EUS and DWI in the differentiation of benign and malignant IPMN: A meta-analysis. Clin Imaging. 2021;72:183–93.
Min JH, Kim YK, Kim SK, Kim H, Ahn S. Intraductal papillary mucinous neoplasm of the pancreas: diagnostic performance of the 2017 international consensus guidelines using CT and MRI. Eur Radiol. 2021;31:4774–84.
Fusaroli P, Serrani M, De Giorgio R, D’Ercole MC, Ceroni L, Lisotti A, et al. Contrast harmonic endoscopic ultrasound is useful to identify neoplastic features of pancreatic cysts (with videos). Pancreas. 2016;45:265–8.
Yamashita Y, Ueda K, Itonaga M, Yoshida T, Maeda H, Maekita T, et al. Usefulness of contrast enhanced endoscopic sonography for discriminating mural nodules from mucous clots in intraductal papillary mucinous neoplasms: a single-center prospective study. J Ultrasound Med. 2013;32:61–8.
Sun Y, Yang S, Qi E, Liu F, Zhou F, Lu Y, et al. Comparative diagnostic evaluation with contrast-enhanced ultrasound, computed tomography and magnetic resonance imaging in patients with pancreatic cystic neoplasms. Cancer Manag Res. 2020;12:2889–98.
Iwaya H, Hijioka S, Mizuno N, Kuwahara T, Okuno N, Tajika M, et al. Usefulness of septal thickness measurement on endoscopic ultrasound as a predictor of malignancy of branched-duct and mixed-type intraductal papillary mucinous neoplasm of the pancreas. Dig Endosc. 2019;31:672–81.
• Lisotti A, Napoleon B, Facciorusso A, Cominardi A, Crinò SF, Brighi N, et al. Contrast-enhanced EUS for the characterization of mural nodules within pancreatic cystic neoplasms: systematic review and meta-analysis. Gastrointest Endosc 2021;94:881-9.e5. Systematic review providing robust evidence on value of contrast-enhanced endoscopic ultrasound for the characterization of mural nodules within pancreatic cystic lesions.
Lim LG, Lakhtakia S, Ang TL, Vu CK, Dy F, Chong VH, et al. Factors determining diagnostic yield of endoscopic ultrasound guided fine-needle aspiration for pancreatic cystic lesions: a multicentre Asian study. Dig Dis Sci. 2013;58:1751–7.
Shirley LA, Walker J, Krishna S, El-Dika S, Muscarella P, Ellison EC, et al. Routine cyst fluid cytology is not indicated in the evaluation of pancreatic cystic lesions. J Gastrointest Surg. 2016;20:1581–5.
Scheiman JM, Hwang JH, Moayyedi P. American Gastroenterological Association technical review on the diagnosis and management of asymptomatic neoplastic pancreatic cysts. Gastroenterology. 2015;148:824–34.
Xu MM, Yin S, Siddiqui AA, Salem RR, Schrope B, Sethi A, et al. Comparison of the diagnostic accuracy of three current guidelines for the evaluation of asymptomatic pancreatic cystic neoplasms. Medicine (Baltimore). 2017;96:e7900.
Sighinolfi M, Quan SY, Lee Y, Ibaseta A, Pham K, Dua MM, et al. Fukuoka and AGA criteria have superior diagnostic accuracy for advanced cystic neoplasms than Sendai criteria. Dig Dis Sci. 2017;62:626–32.
Ma GK, Goldberg DS, Thiruvengadam N, Chandrasekhara V, Kochman ML, Ginsberg GG, et al. Comparing American Gastroenterological Association Pancreatic Cyst Management Guidelines with Fukuoka Consensus Guidelines as predictors of advanced neoplasia in patients with suspected pancreatic cystic neoplasms. J Am Coll Surg. 2016;223:729-37.e1.
Hirooka Y, Goto H, Itoh A, Hashimoto S, Niwa K, Ishikawa H, et al. Case of intraductal papillary mucinous tumor in which endosonography-guided fine needle aspiration biopsy caused dissemination. J Gastroenterol Hepatol. 2003;18:1323e4.
Yoon WJ, Daglilar ES, Fernández-del Castillo C, Mino-Kenudson M, Pitman MB, Brugge WR. Peritoneal seeding in intraductal papillary mucinous neoplasm of the pancreas patients who underwent endoscopic ultrasound-guided fine-needle aspiration: the PIPE study. Endoscopy. 2014;46:382–7.
Singhi AD, McGrath K, Brand RE, Khalid A, Zeh HJ, Chennat JS, et al. Preoperative next generation sequencing of pancreatic cyst fluid is highly accurate in cyst classification and detection of advanced neoplasia. Gut. 2018;67:2131–41.
Guo X, Zhan X, Li Z. Molecular analyses of aspirated cystic fluid for the differential diagnosis of cystic lesions of the pancreas: a systematic review and meta-analysis. Gastroenterol Res Pract. 2016;2016:3546085.
Do M, Kim H, Shin D, Park J, Kim H, Han Y, et al. Marker identification of the grade of dysplasia of intraductal papillary mucinous neoplasm in pancreatic cyst fluid by quantitative proteomic profiling. Cancers (Basel). 2020;12:2383.
Kurita Y, Kuwahara T, Hara K, Mizuno N, Okuno N, Matsumoto S, et al. Diagnostic ability of artificial intelligence using deep learning analysis of cyst fluid in differentiating malignant from benign pancreatic cystic lesions. Sci Rep. 2019;9:6893.
Yip-Schneider MT, Wu H, Dumas RP, Hancock BA, Agaram N, RadovichM, et al. Vascular endothelial growth factor, a novel and highly accurate pancreatic fluid biomarker for serous pancreatic cysts. J Am Coll Surg. 2014;218:608–17.
Carr RA, Yip-Schneider MT, Dolejs S, Hancock BA, Wu H, Radovich M, et al. Pancreatic cyst fluid vascular endothelial growth factor A and carcinoembryonic antigen: a highly accurate test for the diagnosis of serous cystic neoplasm. J Am Coll Surg. 2017;S1072–7515(17):30452.
Blaszczak AM, Krishna SG. Endoscopic diagnosis of pancreatic cysts. Curr Opin Gastroenterol. 2019;35:448–54.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval
The paper is in compliance with current ethical standards.
Conflict of Interest
Dr. Larghi reports personal fees from Boston Scientific and Pentax Medical, grant support from Medtronic, and lecture fees from Taewoong, all outside of the submitted work. Dr. Rimbaș and Dr. Rizzatti have no conflict of interest to declare.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Rimbaș, M., Rizzatti, G. & Larghi, A. Diagnostic Approach to Incidentally Detected Pancreatic Cystic Lesions. Curr Treat Options Gastro 20, 20–33 (2022). https://doi.org/10.1007/s11938-022-00368-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11938-022-00368-z