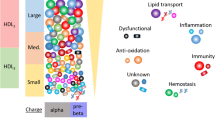
Abstract
Electronegative low-density lipoprotein (LDL) found in human plasma is highly atherogenic, and its level is elevated in individuals with increased cardiovascular risk. In this review, we summarize the available data regarding the elevation of the levels of electronegative LDL in the plasma of patients with various diseases. In addition, we discuss the harmful effects and underlying mechanisms of electronegative LDL in various cell types. We also highlight the known biochemical properties of electronegative LDL that may contribute to its atherogenic functions, including its lipid and protein composition, enzymatic activities, and structural features. Given the increasing recognition of electronegative LDL as a potential biomarker and therapeutic target for the prevention of cardiovascular disease, key future goals include the development of a standard method for the detection of electronegative LDL that can be used in a large-scale population survey and the identification and testing of strategies for eliminating electronegative LDL from the blood.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Goff Jr DC, Lloyd-Jones DM, Bennett G, et al. ACC/AHA guideline on the assessment of cardiovascular risk: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2013. doi:10.1016/j.jacc.2013.11.00.
Stone NJ, Robinson J, Lichtenstein AH, et al. ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2013. doi:10.1016/j.jacc.2013.11.002.
Taylor F, Huffman MD, Macedo AF, et al. Statins for the primary prevention of cardiovascular disease. Cochrane Database Syst Rev. 2013;1, CD004816.
Kjekshus J, Apetrei E, Barrios V, et al. Rosuvastatin in older patients with systolic heart failure. N Engl J Med. 2007;357:2248–61.
Gissi HFI, Tavazzi L, Maggioni AP, et al. Effect of rosuvastatin in patients with chronic heart failure (the GISSI-HF trial): a randomised, double-blind, placebo-controlled trial. Lancet. 2008;372:1231–9.
Schwandt P, Liepold E, Bertsch T, Haas GM. Lifestyle, cardiovascular drugs and risk factors in younger and elder adults: the PEP Family Heart Study. Int J Prev Med. 2010;1:56–61.
Yasue H, Hirai N, Mizuno Y, et al. Low-grade inflammation, thrombogenicity, and atherogenic lipid profile in cigarette smokers. Circ J. 2006;70:8–13.
Hansson GK. Inflammation, atherosclerosis, and coronary artery disease. N Engl J Med. 2005;352:1685–95.
Skaggs BJ, Hahn BH, McMahon M. Accelerated atherosclerosis in patients with SLE—mechanisms and management. Nat Rev Rheumatol. 2012;8:214–23.
Ruiz-Limon P, Barbarroja N, Perez-Sanchez C, et al. Atherosclerosis and cardiovascular disease in systemic lupus erythematosus: effects of in vivo statin treatment. Ann Rheum Dis. 2014. doi:10.1136/annrheumdis-2013-204351.
Marian AJ. The enigma of genetics etiology of atherosclerosis in the post-GWAS era. Curr Atheroscler Rep. 2012;14:295–9.
Chung CP, Solus JF, Oeser A, et al. Genetic variation and coronary atherosclerosis in patients with systemic lupus erythematosus. Lupus. 2014. doi:10.1177/0961203314530019.
Carmena R, Duriez P, Fruchart JC. Atherogenic lipoprotein particles in atherosclerosis. Circulation. 2004;109:III2–7.
Koba S, Hirano T, Ito Y, et al. Significance of small dense low-density lipoprotein-cholesterol concentrations in relation to the severity of coronary heart diseases. Atherosclerosis. 2006;189:206–14.
Libby P. Inflammation in atherosclerosis. Nature. 2002;420:868–74.
Witztum JL, Steinberg D. The oxidative modification hypothesis of atherosclerosis: does it hold for humans? Trends Cardiovasc Med. 2001;11:93–102.
Itabe H, Yamamoto H, Imanaka T, et al. Sensitive detection of oxidatively modified low density lipoprotein using a monoclonal antibody. J Lipid Res. 1996;37:45–53.
Palinski W, Horkko S, Miller E, et al. Cloning of monoclonal autoantibodies to epitopes of oxidized lipoproteins from apolipoprotein E-deficient mice. Demonstration of epitopes of oxidized low density lipoprotein in human plasma. J Clin Invest. 1996;98:800–14.
Mello AP, da Silva IT, Abdalla DS, Damasceno NR. Electronegative low-density lipoprotein: origin and impact on health and disease. Atherosclerosis. 2011;215:257–65.
Sanchez-Quesada JL, Villegas S, Ordonez-Llanos J. Electronegative low-density lipoprotein. A link between apolipoprotein B misfolding, lipoprotein aggregation and proteoglycan binding. Curr Opin Lipidol. 2012;23:479–86.
Hoff HF, Gaubatz JW. Isolation, purification, and characterization of a lipoprotein containing apo B from the human aorta. Atherosclerosis. 1982;42:273–97.
Hoff HF, Karagas M, Heideman CL, et al. Correlation in the human aorta of apo B fractions with tissue cholesterol and collagen content. Atherosclerosis. 1979;32:259–68.
Avogaro P, Bon GB, Cazzolato G. Presence of a modified low density lipoprotein in humans. Arteriosclerosis. 1988;8:79–87.
Chen CH, Jiang T, Yang JH, et al. Low-density lipoprotein in hypercholesterolemic human plasma induces vascular endothelial cell apoptosis by inhibiting fibroblast growth factor 2 transcription. Circulation. 2003;107:2102–8.
Yang CY, Raya JL, Chen HH, et al. Isolation, characterization, and functional assessment of oxidatively modified subfractions of circulating low-density lipoproteins. Arterioscler Thromb Vasc Biol. 2003;23:1083–90.
Lu J, Yang JH, Burns AR, et al. Mediation of electronegative low-density lipoprotein signaling by LOX-1: a possible mechanism of endothelial apoptosis. Circ Res. 2009;104:619–27.
Lee AS, Wang GJ, Chan HC, et al. Electronegative low-density lipoprotein induces cardiomyocyte apoptosis indirectly through endothelial cell-released chemokines. Apoptosis. 2012;17:1009–18. L5 indirectly induced cardiomyocyte apoptosis by enhancing secretion of ELR-positive CXC chemokines from ECs, which in turn activate CXCR2/phosphoinositide 3-kinase/NF-κB signaling to increase the release of tumor necrosis factor α and IL-1β.
Chu CS, Wang YC, Lu LS, et al. Electronegative low-density lipoprotein increases C-reactive protein expression in vascular endothelial cells through the LOX-1 receptor. PLoS One. 2013;8, e70533. L5 induces C-reactive protein expression and reactive oxygen species production in vitro, and its levels are reduced in the plasma of hypercholesterolemic patients treated with atorvastatin.
Gaubatz JW, Gillard BK, Massey JB, et al. Dynamics of dense electronegative low density lipoproteins and their preferential association with lipoprotein phospholipase A2. J Lipid Res. 2007;48:348–57.
Tang D, Lu J, Walterscheid JP, et al. Electronegative LDL circulating in smokers impairs endothelial progenitor cell differentiation by inhibiting Akt phosphorylation via LOX-1. J Lipid Res. 2008;49:33–47.
Urata J, Ikeda S, Koga S, et al. Negatively charged low-density lipoprotein is associated with atherogenic risk in hypertensive patients. Heart Vessels. 2012;27:235–42.
Chan HC, Ke LY, Chu CS, et al. Highly electronegative LDL from patients with ST-elevation myocardial infarction triggers platelet activation and aggregation. Blood. 2013;122:3632–41. L5 concentration is increased in the plasma of patients with STEMI and enhances ADP-stimulated platelet aggregation and platelet–EC adhesion in vitro, suggesting a role for L5 in thrombogenesis.
Oliveira JA, Sevanian A, Rodrigues RJ, et al. Minimally modified electronegative LDL and its autoantibodies in acute and chronic coronary syndromes. Clin Biochem. 2006;39:708–14.
Lobo J, Santos F, Grosso D, et al. Electronegative LDL and lipid abnormalities in patients undergoing hemodialysis and peritoneal dialysis. Nephron Clin Pract. 2008;108:c298–304.
Sawamura T, Kakino A, Fujita Y. LOX-1: a multiligand receptor at the crossroads of response to danger signals. Curr Opin Lipidol. 2012;23:439–45. Among various LOX-1 ligands, L5 and its interaction with LOX-1 are discussed in the context of the pathophysiological significance of LOX-1.
Lu J, Jiang W, Yang JH, et al. Electronegative LDL impairs vascular endothelial cell integrity in diabetes by disrupting fibroblast growth factor 2 (FGF2) autoregulation. Diabetes. 2008;57:158–66.
Chen HH, Hosken BD, Huang M, et al. Electronegative LDLs from familial hypercholesterolemic patients are physicochemically heterogeneous but uniformly proapoptotic. J Lipid Res. 2007;48:177–84.
Sanchez-Quesada JL, Camacho M, Anton R, et al. Electronegative LDL of FH subjects: chemical characterization and induction of chemokine release from human endothelial cells. Atherosclerosis. 2003;166:261–70.
Tai MH, Kuo SM, Liang HT, et al. Modulation of angiogenic processes in cultured endothelial cells by low density lipoproteins subfractions from patients with familial hypercholesterolemia. Atherosclerosis. 2006;186:448–57.
von Eckardstein A, Rohrer L. Transendothelial lipoprotein transport and regulation of endothelial permeability and integrity by lipoproteins. Curr Opin Lipidol. 2009;20:197–205.
Estruch M, Sanchez-Quesada JL, Beloki L, et al. The induction of cytokine release in monocytes by electronegative low-density lipoprotein (LDL) is related to its higher ceramide content than native LDL. Int J Mol Sci. 2013;14:2601–16.
Abe Y, Fornage M, Yang CY, et al. L5, the most electronegative subfraction of plasma LDL, induces endothelial vascular cell adhesion molecule 1 and CXC chemokines, which mediate mononuclear leukocyte adhesion. Atherosclerosis. 2007;192:56–66.
De Castellarnau C, Sanchez-Quesada JL, Benitez S, et al. Electronegative LDL from normolipemic subjects induces IL-8 and monocyte chemotactic protein secretion by human endothelial cells. Arterioscler Thromb Vasc Biol. 2000;20:2281–7.
Nichols TC. Bad cholesterol breaking really bad. Blood. 2013;122:3551–3.
Benitez S, Perez A, Sanchez-Quesada JL, et al. Electronegative low-density lipoprotein subfraction from type 2 diabetic subjects is proatherogenic and unrelated to glycemic control. Diabetes Metab Res Rev. 2007;23:26–34.
Ke LY, Engler DA, Lu J, et al. Chemical composition-oriented receptor selectivity of L5, a naturally occurring atherogenic low-density lipoprotein. Pure Appl Chem. 2011;83. A proteomic study of L5 showing that additional apolipoproteins in L5 contribute to its electronegativity and receptor selectivity.
Chappey B, Myara I, Benoit MO, et al. Characteristics of ten charge-differing subfractions isolated from human native low-density lipoproteins (LDL). No evidence of peroxidative modifications. Biochim Biophys Acta. 1995;1259:261–70.
Moro E, Alessandrini P, Zambon C, et al. Is glycation of low density lipoproteins in patients with type 2 diabetes mellitus a LDL pre-oxidative condition? Diabet Med. 1999;16:663–9.
Geromanos SJ, Vissers JP, Silva JC, et al. The detection, correlation, and comparison of peptide precursor and product ions from data independent LC-MS with data dependant LC-MS/MS. Proteomics. 2009;9:1683–95.
Li GZ, Vissers JP, Silva JC, et al. Database searching and accounting of multiplexed precursor and product ion spectra from the data independent analysis of simple and complex peptide mixtures. Proteomics. 2009;9:1696–719.
Bancells C, Canals F, Benitez S, et al. Proteomic analysis of electronegative low-density lipoprotein. J Lipid Res. 2010;51:3508–15.
Scheffer PG, Bakker SJ, Heine RJ, Teerlink T. Measurement of low-density lipoprotein particle size by high-performance gel-filtration chromatography. Clin Chem. 1997;43:1904–12.
Tselepis AD, John Chapman M. Inflammation, bioactive lipids and atherosclerosis: potential roles of a lipoprotein-associated phospholipase A2, platelet activating factor-acetylhydrolase. Atheroscler Suppl. 2002;3:57–68.
Zalewski A, Macphee C. Role of lipoprotein-associated phospholipase A2 in atherosclerosis: biology, epidemiology, and possible therapeutic target. Arterioscler Thromb Vasc Biol. 2005;25:923–31.
Sanchez-Quesada JL, Vinagre I, De Juan-Franco E, et al. Impact of the LDL subfraction phenotype on Lp-PLA2 distribution, LDL modification and HDL composition in type 2 diabetes. Cardiovasc Diabetol. 2013;12:112.
Yang CY, Chen HH, Huang MT, et al. Pro-apoptotic low-density lipoprotein subfractions in type II diabetes. Atherosclerosis. 2007;193:283–91.
Benitez S, Villegas V, Bancells C, et al. Impaired binding affinity of electronegative low-density lipoprotein (LDL) to the LDL receptor is related to nonesterified fatty acids and lysophosphatidylcholine content. Biochemistry. 2004;43:15863–72.
Karpe F, Dickmann JR, Frayn KN. Fatty acids, obesity, and insulin resistance: time for a reevaluation. Diabetes. 2011;60:2441–9.
Sanchez-Quesada JL, Vinagre I, de Juan-Franco E, et al. Effect of improving glycemic control in patients with type 2 diabetes mellitus on low-density lipoprotein size, electronegative low-density lipoprotein and lipoprotein-associated phospholipase A2 distribution. Am J Cardiol. 2012;110:67–71. Optimal glycemic control in patients with type 2 diabetes promotes atheroprotective changes that include decreased levels of LDL(–).
Benitez S, Camacho M, Arcelus R, et al. Increased lysophosphatidylcholine and non-esterified fatty acid content in LDL induces chemokine release in endothelial cells. Relationship with electronegative LDL. Atherosclerosis. 2004;177:299–305.
Holmes MV, Simon T, Exeter HJ, et al. Secretory phospholipase A2-IIA and cardiovascular disease: a Mendelian randomization study. J Am Coll Cardiol. 2013;62:1966–76.
Xu H, Valenzuela N, Fai S, et al. Targeted lipidomics - advances in profiling lysophosphocholine and platelet-activating factor second messengers. FEBS J. 2013;280:5652–67.
Benítez S, Sanchez-Quesada JL, Ribas V, et al. Platelet-activating factor acetylhydrolase is mainly associated with electronegative low-density lipoprotein subfraction. Circulation. 2003;108:92–6.
Sanchez-Quesada JL, Benitez S, Perez A, et al. The inflammatory properties of electronegative low-density lipoprotein from type 1 diabetic patients are related to increased platelet-activating factor acetylhydrolase activity. Diabetologia. 2005;48:2162–9.
Ito S, Noguchi E, Shibasaki M, et al. Evidence for an association between plasma platelet-activating factor acetylhydrolase deficiency and increased risk of childhood atopic asthma. J Hum Genet. 2002;47:99–101.
Stafforini DM. Biology of platelet-activating factor acetylhydrolase (PAF-AH, lipoprotein associated phospholipase A2). Cardiovasc Drugs Ther. 2009;23:73–83.
Bancells C, Benitez S, Jauhiainen M, et al. High binding affinity of electronegative LDL to human aortic proteoglycans depends on its aggregation level. J Lipid Res. 2009;50:446–55.
Bancells C, Benitez S, Ordonez-Llanos J, et al. Immunochemical analysis of the electronegative LDL subfraction shows that abnormal N-terminal apolipoprotein B conformation is involved in increased binding to proteoglycans. J Biol Chem. 2011;286:1125–33. The amino-terminal region of apo B-100 has an abnormal conformation in LDL(–) that may promote its increased binding to arterial proteoglycans and influence its receptor affinity.
Bancells C, Benitez S, Villegas S, et al. Novel phospholipolytic activities associated with electronegative low-density lipoprotein are involved in increased self-aggregation. Biochemistry. 2008;47:8186–94.
Doehner W, Bunck AC, Rauchhaus M, et al. Secretory sphingomyelinase is upregulated in chronic heart failure: a second messenger system of immune activation relates to body composition, muscular functional capacity, and peripheral blood flow. Eur Heart J. 2007;28:821–8.
Gorska M, Baranczuk E, Dobrzyn A. Secretory Zn2+-dependent sphingomyelinase activity in the serum of patients with type 2 diabetes is elevated. Horm Metab Res. 2003;35:506–7.
Chavez JA, Summers SA. A ceramide-centric view of insulin resistance. Cell Metab. 2012;15:585–94.
Estruch M, Sanchez-Quesada JL, Ordonez-Llanos J, Benitez S. Ceramide-enriched LDL induces cytokine release through TLR4 and CD14 in monocytes. Similarities with electronegative LDL. Clin Investig Arterioscler. 2014. doi:10.1016/j.arteri.2013.12.003.
Yu J, Novgorodov SA, Chudakova D, et al. JNK3 signaling pathway activates ceramide synthase leading to mitochondrial dysfunction. J Biol Chem. 2007;282:25940–9.
Obama T, Kato R, Masuda Y, et al. Analysis of modified apolipoprotein B-100 structures formed in oxidized low-density lipoprotein using LC-MS/MS. Proteomics. 2007;7:2132–41.
Segrest JP, Jones MK, Mishra VK, et al. apoB-100 has a pentapartite structure composed of three amphipathic alpha-helical domains alternating with two amphipathic beta-strand domains. Detection by the computer program LOCATE. Arterioscler Thromb. 1994;14:1674–85.
Walters MJ, Wrenn SP. Effect of sphingomyelinase-mediated generation of ceramide on aggregation of low-density lipoprotein. Langmuir. 2008;24:9642–7.
Oestvang J, Bonnefont-Rousselot D, Ninio E, et al. Modification of LDL with human secretory phospholipase A2 or sphingomyelinase promotes its arachidonic acid-releasing propensity. J Lipid Res. 2004;45:831–8.
Devlin CM, Leventhal AR, Kuriakose G, et al. Acid sphingomyelinase promotes lipoprotein retention within early atheromata and accelerates lesion progression. Arterioscler Thromb Vasc Biol. 2008;28:1723–30.
Hamilton RT, Asatryan L, Nilsen JT, et al. LDL protein nitration: implication for LDL protein unfolding. Arch Biochem Biophys. 2008;479:1–14.
Parasassi T, Bittolo-Bon G, Brunelli R, et al. Loss of apoB-100 secondary structure and conformation in hydroperoxide rich, electronegative LDL(-). Free Radic Biol Med. 2001;31:82–9.
Holopainen JM, Medina OP, Metso AJ, Kinnunen PK. Sphingomyelinase activity associated with human plasma low density lipoprotein. J Biol Chem. 2000;275:16484–9.
Kinnunen PK, Holopainen JM. Sphingomyelinase activity of LDL: a link between atherosclerosis, ceramide, and apoptosis? Trends Cardiovasc Med. 2002;12:37–42.
Hevonoja T, Pentikainen MO, Hyvonen MT, et al. Structure of low density lipoprotein (LDL) particles: basis for understanding molecular changes in modified LDL. Biochim Biophys Acta. 2000;1488:189–210.
Yang CY, Kim TW, Weng SA, et al. Isolation and characterization of sulfhydryl and disulfide peptides of human apolipoprotein B-100. Proc Natl Acad Sci U S A. 1990;87:5523–7.
Zhao Y, McCabe JB, Vance J, Berthiaume LG. Palmitoylation of apolipoprotein B is required for proper intracellular sorting and transport of cholesteroyl esters and triglycerides. Mol Biol Cell. 2000;11:721–34.
Chen R, Jiang X, Sun D, et al. Glycoproteomics analysis of human liver tissue by combination of multiple enzyme digestion and hydrazide chemistry. J Proteome Res. 2009;8:651–61.
Liu T, Qian WJ, Gritsenko MA, et al. Human plasma N-glycoproteome analysis by immunoaffinity subtraction, hydrazide chemistry, and mass spectrometry. J Proteome Res. 2005;4:2070–80.
Yang CY, Gu ZW, Weng SA, et al. Structure of apolipoprotein B-100 of human low density lipoproteins. Arteriosclerosis. 1989;9:96–108.
Sun HY, Chen SF, Lai MD, et al. Comparative proteomic profiling of plasma very-low-density and low-density lipoproteins. Clin Chim Acta. 2010;411:336–44.
Yang CY, Chen SH, Gianturco SH, et al. Sequence, structure, receptor-binding domains and internal repeats of human apolipoprotein B-100. Nature. 1986;323:738–42.
Yoshimoto R, Fujita Y, Kakino A, et al. The discovery of LOX-1, its ligands and clinical significance. Cardiovasc Drugs Ther. 2011;25:379–91.
Chang PY, Chen YJ, Chang FH, et al. Aspirin protects human coronary artery endothelial cells against atherogenic electronegative LDL via an epigenetic mechanism: a novel cytoprotective role of aspirin in acute myocardial infarction. Cardiovasc Res. 2013;99:137–45.
Acknowledgments
Our work described in this review was supported in part by grants from the American Diabetes Association (1-04-RA-13), the National Heart, Lung, and Blood Institute (HL-63364), Merck/Schering-Plough Pharmaceuticals (research grant), the Mao-Kuei Lin Research Fund of Chicony Electronics, the National Science Council (NSC 100-2314-B-039-040-MY3), and Kaohsiung Medical University Hospital, Taiwan (research grant 101-KMUH-M047).
Compliance with Ethics Guidelines
ᅟ
Conflict of Interest
Liang-Yin Ke, Nicole Stancel, Henry Bair, and Chu-Huang Chen declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Additional information
Liang-Yin Ke and Nicole Stancel contributed equally to the article.
This article is part of the Topical Collection on Genetics
Rights and permissions
About this article
Cite this article
Ke, LY., Stancel, N., Bair, H. et al. The Underlying Chemistry of Electronegative LDL’s Atherogenicity. Curr Atheroscler Rep 16, 428 (2014). https://doi.org/10.1007/s11883-014-0428-y
Published:
DOI: https://doi.org/10.1007/s11883-014-0428-y