Abstract
Objective
The aim of this study was to measure any incremental costs or savings within the health system associated with the introduction of the new technology, prucalopride, for the management of chronic constipation.
Methodology
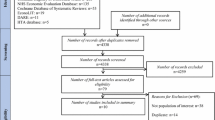
The study design was based on a budget impact analysis conducted by the National Institute of Clinical Excellence (NICE). To validate the findings of the NICE costing template, a case series audit capturing real world data was used to determine the financial impact of adopting prucalopride in 40 women suffering with chronic constipation. This facilitated the application of local unit costs to the resources used and determined whether the use of prucalopride, as an alternative treatment to laxatives, resulted in a reduction in the use of secondary care resources.
Results
Patients were treated with an average of 2.6 laxatives in the baseline (laxatives only) scenario. The total medication costs in the baseline (laxatives only) and the new treatment (prucalopride) scenario amounted to €17,440.84 and €18,417.62, respectively. There was a significant reduction in the number of investigations and procedures in the 12 months after commencing prucalopride, with cost savings of €41,923.28 (€1,048.08 per patient per year) demonstrated. Input cost variables were adjusted as part of sensitivity analysis.
Conclusion
This study validated the findings of the NICE costing template and suggests that the use of prucalopride for the treatment of chronic constipation in women refractory to laxatives has the potential to reduce secondary care resource use and hence led to cost savings.
Similar content being viewed by others
References
Longstreth GF, Thompson WG, Chey WD et al (2006) Functional bowel disorders. Gastroenterology 130:1480–1491
Higgins PD, Johanson JF (2004) Epidemiology of constipation in North America: a systematic review. Am J Gastroenterol 99:441–449
Stewart WF, Liberman JN, Sandler RS et al (1999) Epidemiology of constipation (EPOC) study in the United States: relation of clinical subtypes to sociodemographic features. Am J Gastroenterol 94:3530–3540
Wald A, Kamm M, Mueller-Lissner S et al (2006) The BI Omnibus study: an international survey of community prevalence of constipation and laxative use in adults. Gastroenterology 130:508
Dennison C, Prasad M, Lloyd A et al (2005) The health-related quality of life and economic burden of constipation. Pharmacoeconomics 23:461–476
Yost KJ, Haan MN, Levine RA et al (2005) Comparing SF-36 scores across three groups of women with different health profiles. Qual Life Res 14:1251–1261
Johanson JF (2007) Review of the treatment options for chronic constipation. Med Gen Med 9:25
Petticrew M, Rodgers M, Booth A (2001) Effectiveness of laxatives in adults. Qual Health Care 10:268–273
Jones MP, Talley NJ, Nuyts G et al (2002) Lack of objective evidence of efficacy of laxatives in chronic constipation. Dig Dis Sci 47:2222–2230
Tramonte SM, Brand MB, Mulrow CD et al (1997) The treatment of chronic constipation in adults: a systematic review. J Gen Intern Med 12:15–24
Quigley EMM (2012) Prucalopride: safety, efficacy and potential applications. Ther Adv Gastroenterol 5:23–30
Camilleri M, Kerstens R, Rykx A (2008) A placebo-controlled trial of prucalopride for severe chronic constipation. N Engl J Med 358:2344–2354
Tack J, van Outryve M, Beyens G et al (2009) Prucalopride (Resolor) in the treatment of severe chronic constipation in patients dissatisfied with laxatives. Gut 58:357–365
Quigley EMM, Vandeplassche L, Kerstens R et al (2008) Clinical trial: the efficacy, impact on quality of life, and safety and tolerability of prucalopride in severe chronic constipation—a 12-week, randomized, double-blind, placebo-controlled study. Aliment Pharmacol Ther 29:315–328
Tack J, Quigley E, Camilleri M et al (2013) Efficacy and safety of oral prucalopride in women with chronic constipation in whom laxatives have failed: an integrated analysis. UEG J 1:48–59
Mauskopf JA, Sullivan SD, Annemans L et al (2007) Principles of good practice for budget impact analysis: report of the ISPOR task force on good research practices—budget impact analysis. Value in Health 10:336–347
(2011) TA211 Prucalopride chronic constipation in women: costing template. Available at: http://guidance.nice.org.uk/TA211/CostingTemplate/xls/English. Accessed 14 May 2012
(2010) Constipation (women)—Prucalopride (TA211). Available at: http://guidance.nice.org.uk/TA211. Accessed 14 May 2012
Monthly Index of Medical Specialties Ireland (MIMS Ireland) (2012) MPI Media Ltd, Dublin, Ireland
Lynch J (2001) The health economic implications of treatment with quetiapine: an audit of long term treatment for patients with chronic schizophrenia. Eur Psychiatry 16(5):307–312
Rantis PC Jr, Vernava AM, Daniel GL et al (1997) Chronic constipation—is the work-up worth the cost? Dis Colon Rectum 40:280–286
Nyrop KA (2007) Costs of health care for irritable bowel syndrome, chronic constipation, functional diarrhoea and functional abdominal pain. Aliment Pharmacol Ther 26(2):237–248
Lynch J (2001) The health economic implications of treatment with quetiapine: an audit of long term treatment for patients with chronic schizophrenia. Eur Psychiatry 16(5):307–312
Addison R (2003) A national audit of chronic constipation in the community. Nurs Times 99(11):34–35
Jones MP (2002) Lack of objective evidence of efficacy of laxatives in chronic constipation. Dig Dis Sci 47(10):2222–2230
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Walsh, C., Murphy, J. & Quigley, E.M.M. Pharmacoeconomic study of chronic constipation in a secondary care centre. Ir J Med Sci 184, 863–870 (2015). https://doi.org/10.1007/s11845-014-1204-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11845-014-1204-2