Abstract
Purpose
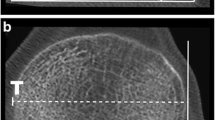
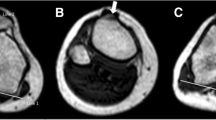
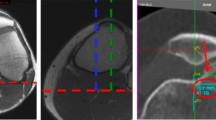
Tibial tuberosity–trochlear groove (TTTG) distance is currently considered as one of the main factors in decision-making for surgical intervention in patients with patellar instability. The current study aimed to provide a valid comparison of TTTG distance in the healthy knees with those with patellar instability.
Materials and methods
Patients with a history of two or more episodes of patellar dislocation in the same knee who were referred to our department for the assessment of TTTG distance were included. Asymptomatic knees of patients as well as both knees of 21 healthy individuals were used as controls.
Results
A total number of 42 patients, including 14 (33.3 %) male and 28 (66.7 %) female, with a mean age of 28.6 ± 12.3 years were included. Twenty-one controls with no significant difference of personal characteristics with patients were also enrolled. The mean TTTG distance in symptomatic and asymptomatic knees of patients were 18.71 ± 3.96 mm and 17.35 ± 4.39 mm with no significant difference (P = 0.298). The mean TTTG distances of both symptomatic and asymptomatic knees of patients were significantly higher than in knees of controls (P < 0.001).
Conclusion
The findings of the current study are not in favor of considering TTTG distance independently in decision-making for surgical interventions. However, greater TTTG in both asymptomatic and symptomatic knees of patients compared to controls indicates that this measure could still be considered as an indicator of knee instability and even the need for surgery if considered in addition to other factors.


Similar content being viewed by others
References
Fithian DC, Paxton EW, Stone ML, Silva P, Davis DK, Elias DA, White LM (2004) Epidemiology and natural history of acute patellar dislocation. Am J Sports Med 32:1114–1121
Nietosvaara Y, Aalto K, Kallio PE (1994) Acute patellar dislocation in children: incidence and associated osteochondral fractures. J Pediatr Orthop 14:513–515
Hawkins RJ, Bell RH, Anisette G (1986) Acute patellar dislocations. The natural history. Am J Sports Med 14:117–120
Atkin DM, Fithian DC, Marangi KS, Stone ML, Dobson BE, Mendelsohn C (2000) Characteristics of patients with primary acute lateral patellar dislocation and their recovery within the first 6 months of injury. Am J Sports Med 28:472–479
Dejour H, Walch G, Nove-Josserand L, Guier C (1994) Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports Traumatol Arthrosc 2:19–26
Colvin AC, West RV (2008) Patellar instability. J Bone Joint Surg Am 90:2751–2762
Balcarek P, Jung K, Ammon J, Walde TA, Frosch S, Schuttrumpf JP, Sturmer KM, Frosch KH (2010) Anatomy of lateral patellar instability: trochlear dysplasia and tibial tubercle-trochlear groove distance is more pronounced in women who dislocate the patella. Am J Sports Med 38:2320–2327
Balcarek P, Jung K, Frosch KH, Sturmer KM (2011) Value of the tibial tuberosity–trochlear groove distance in patellar instability in the young athlete. Am J Sports Med 39:1756–1761
Cooney AD, Kazi Z, Caplan N, Newby M, St Clair Gibson A, Kader DF (2012) The relationship between quadriceps angle and tibial tuberosity–trochlear groove distance in patients with patellar instability. Knee Surg Sports Traumatol Arthrosc 20:2399–2404
Lustig S, Servien E, Ait Si Selmi T, Neyret P (2006) Factors affecting reliability of TT-TG measurements before and after medialization: a CT-scan study. Rev Chir Orthop Reparatrice Appar Mot 92:429–436
Drexler M, Dwyer T, Marmor M, Reischl N, Attar F, Cameron J (2013) Total knee arthroplasty in patients with excessive external tibial torsion >45 degrees and patella instability–surgical technique and follow up. J Arthroplasty 28:614–619
Caplan N, Lees D, Newby M, Ewen A, Jackson R, St Clair Gibson A, Kader D (2014) Is tibial tuberosity–trochlear groove distance an appropriate measure for the identification of knees with patellar instability? Knee Surg Sports Traumatol Arthrosc 22:2377–2381
Williams AA, Elias JJ, Tanaka MJ, Thawait GK, Demehri S, Carrino JA, Cosgarea AJ (2016) The relationship between tibial tuberosity-trochlear groove distance and abnormal patellar tracking in patients with unilateral patellar instability. Arthroscopy 32(1):55–61. doi:10.1016/j.arthro.2015.06.037
Charan J, Biswas T (2013) How to calculate sample size for different study designs in medical research? Indian J Psychol Med 35:121–126
McNally EG, Ostlere SJ, Pal C, Phillips A, Reid H, Dodd C (2000) Assessment of patellar maltracking using combined static and dynamic MRI. Eur Radiol 10:1051–1055
Fithian DC, Paxton EW, Cohen AB (2004) Indications in the treatment of patellar instability. J Knee Surg 17:47–56
Monk AP, Doll HA, Gibbons CL, Ostlere S, Beard DJ, Gill HS, Murray DW (2011) The patho-anatomy of patellofemoral subluxation. J Bone Joint Surg Br 93:1341–1347
Dandy DJ (1996) Chronic patellofemoral instability. J Bone Joint Surg Br 78:328–335
Mulford JS, Wakeley CJ, Eldridge JD (2007) Assessment and management of chronic patellofemoral instability. J Bone Joint Surg Br 89:709–716
Sillanpaa P, Mattila VM, Iivonen T, Visuri T, Pihlajamaki H (2008) Incidence and risk factors of acute traumatic primary patellar dislocation. Med Sci Sports Exerc 40:606–611
Maenpaa H (1998) The dislocating patella. Predisposing factors and a clinical, radiological and functional follow-up study of patients treated primarily nonoperatively. Ann Chir Gynaecol 87:248–249
Maenpaa H, Huhtala H, Lehto MU (1997) Recurrence after patellar dislocation. Redislocation in 37/75 patients followed for 6–24 years. Acta Orthop Scand 68:424–426
Nikku R, Nietosvaara Y, Aalto K, Kallio PE (2005) Operative treatment of primary patellar dislocation does not improve medium-term outcome: a 7-year follow-up report and risk analysis of 127 randomized patients. Acta Orthop 76:699–704
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Funding
This study was financially supported by the AJA University of Medical Sciences.
Rights and permissions
About this article
Cite this article
Mohammadinejad, P., Shekarchi, B. Value of CT scan-assessed tibial tuberosity–trochlear groove distance in identification of patellar instability. Radiol med 121, 729–734 (2016). https://doi.org/10.1007/s11547-016-0647-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-016-0647-0