Abstract
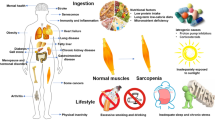
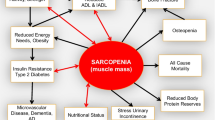
Frailty is a construct originally coined by gerontologists to describe cumulative declines across multiple physiological systems that occur with aging and lead individuals to a state of diminished physiological reserve and increased vulnerability to stressors. Fried et al. provided a standardized definition for frailty, and they created the concept of frailty phenotype which incorporates disturbances across interrelated domains (shrinking, weakness, poor endurance and energy, slowness, and low physical activity level) to indentify old people who are at risk of disability, falls, institutionalization, hospitalization, and premature death. Some authors consider the presence of lean mass reduction (sarcopenia) as part of the frailty phenotype. The frailty status has been documented in 7 % of elderly population and 14 % of not requiring dialysis CKD adult patients. Sarcopenia increases progressively along with loss of renal function in CKD patients and is high in dialysis population. It has been documented that prevalence of frailty in hemodialysis adult patients is around 42 % (35 % in young and 50 % in elderly), having a 2.60-fold higher risk of mortality and 1.43-fold higher number of hospitalization, independent of age, comorbidity, and disability. The Clinical Frailty Scale is the simplest and clinically useful and validated tool for doing a frailty phenotype, while the diagnosis of sarcopenia is based on muscle mass assessment by body imaging techniques, bioimpedance analysis, and muscle strength evaluated with a handheld dynamometer. Frailty treatment can be based on different strategies, such as exercise, nutritional interventions, drugs, vitamins, and antioxidant agents. Finally, palliative care is a very important alternative for very frail and sick patients. In conclusion, since the diagnosis and treatment of frailty and sarcopenia is crucial in geriatrics and all CKD patients, it would be very important to incorporate these evaluations in pre-dialysis, peritoneal dialysis, hemodialysis, and kidney transplant patients in order to detect and consequently treat the frailty phenotype in these groups.
Similar content being viewed by others
References
Roshanravan B, Khatri M, Robinson-Cohen C, Levin G, Patel KV, de Boer IH, Seliger S, Ruzinski J, Himmelfarb J, Kestenbaum B (2012) A prospective study of frailty in nephrology-referred patients with CKD. Am J Kidney Dis 60(6):912–921
Johansen KL, Delgado C, Bao Y, Kurella Tamura M (2013) Frailty and dialysis initiation. Semin Dial 26(6):690–696
Studenski S (2011) Gait speed and survival in older adults. JAMA 305(1):50–58
Romero-Cabrera AJ (2011) Frailty and chronic diseases in the elderly. Int Mex 27(5):455–462
Johansen KL, Chertow GM, Jin C, Kutner NG (2007) Significance of frailty among dialysis patients. J Am Soc Nephrol 18(11):2960–2967
Bonanni A, Mannucci I, Verzola D, Sofia A, Saffioti S, Gianetta E, Garibotto G (2011) Protein-energy wasting and mortality in chronic kidney disease. Int J Environ Res Public Health 8(5):1631–1635
Fried LP, Tangen CM, Walston J, Newman AB, Hirsch C, Gottdiener J, Seeman T, Tracy R, Kop WJ, Burke G, McBurnie MA (2001) Cardiovascular Health Study Collaborative Research Group. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci 56(3):M146–M156
Walker SR, Gill K, Macdonald K, Komenda P, Rigatto C, Sood MM, Bohm CJ, Storsley LJ, Tangri N (2013) Association of frailty and physical function in patients with non-dialysis CKD: a systematic review. BMC Nephrol 22(14):228. doi:10.1186/1471-2369-14-228
Ayaz T, Sahin SB, Sahin OZ, Bilir O, Rakıcı H (2014) Factors affecting mortality in elderly patients hospitalized for nonmalignant reasons. J Aging Res 2014:584315. doi:10.1155/2014/584315
Forciea M, Lavizzo-Mourey R, Schwab E (2000) Geriatric secrets. Hanley & Belfus, Philadelphia
McAdams-DeMarco MA, Law A, Salter ML, Boyarsky B, Gimenez L, Jaar BG, Walston JD, Segev DL (2013) Frailty as a novel predictor of mortality and hospitalization in individuals of all ages undergoing hemodialysis. J Am Geriatr Soc 61(6):896–901
Montero-Odasso M, Schapira M, Soriano ER, Varela M, Kaplan R, Camera LA, Mayorga LM (2005) Gait velocity as a single predictor of adverse events in healthy seniors aged 75 years and older. J Gerontol A Biol Sci Med Sci. 60(10):1304–1309
Morley JE, Vellas B, van Kan GA, Anker SD, Bauer JM, Bernabei R, Cesari M, Chumlea WC, Doehner W, Evans J, Fried LP, Guralnik JM, Katz PR, Malmstrom TK, McCarter RJ, Gutierrez Robledo LM, Rockwood K, von Haehling S, Vandewoude MF, Walston J (2013) Frailty consensus: a call to action. J Am Med Dir Assoc 14(6):392–397
Cruz-Jentoft AJ, Baeyens JP, Bauer JM, Boirie Y, Cederholm T, Landi F, Martin FC, Michel JP, Rolland Y, Schneider SM, Topinková E, Vandewoude M, Zamboni M (2010) European Working Group on Sarcopenia in Older People. Sarcopenia: European consensus on definition and diagnosis: Report of the European Working Group on Sarcopenia in Older People. Age Ageing 39(4):412–423
Buford TW, Anton SD, Judge AR, Marzetti E, Wohlgemuth SE, Carter CS, Leeuwenburgh C, Pahor M, Manini TM (2010) Models of accelerated sarcopenia: critical pieces for solving the puzzle of age-related muscle atrophy. Ageing Res Rev 9(4):369–383
Shastri S, Katz R, Rifkin DE, Fried LF, Odden MC, Peralta CA, Chonchol M, Siscovick D, Shlipak MG, Newman AB, Sarnak MJ (2012) Kidney function and mortality in octogenarians: cardiovascular Health Study All Stars. J Am Geriatr Soc 60(7):1201–1207
Feng L, Yap KB, Yeoh LY, Ng TP (2012) Kidney function and cognitive and functional decline in elderly adults: findings from the Singapore longitudinal aging study. J Am Geriatr Soc 60(7):1208–1214
Rifkin DE, Shlipak MG, Katz R, Fried LF, Siscovick D, Chonchol M, Newman AB, Sarnak MJ (2008) Rapid kidney function decline and mortality risk in older adults. Arch Intern Med 168(20):2212–2218
Tessari P, Deferrari G, Robaudo C, Vettore M, Pastorin N, De Biasi L, Garibotto G (1999) Phenylalanine hydroxylation across the kidney in humans. Kidney Int 56:2168–2172
Garibotto G, Valli A, Anderstam B, Eriksson M, Suliman M, Balbi M, Rollando D, Vigo E, Lindholm B (2009) The kidney is a major site of S-adenosylhomocysteine disposal in humans. Kidney Int 76:293–296
Baylis C (2006) Arginine, arginine analogous and nitric oxid production in chronic kidney disease. Nat Clin Pract Nephrol 2:209–220
Sun DF, Zheng Z, Tummala P, Oh J, Schaefer F, Rabkin R (2004) Chronic uremia attenuates growth hormone-induced signal transduction in skeletal muscle. J Am Soc Nephrol 15:2630–2646
Chen Y, Biada J, Sood S, Rabkin R (2010) Uremia attenuates growth hormone-stimulated insulin-like growth factor-1 expression, a process worsened by inflammation. Kidney Int 78:89–95
Harman SM, Metter EJ, Tobin JD, Pearson J, Blackman MR (2001) Baltimore longitudinal study of aging. Longitudinal effects of aging on serum total and free testosterone levels in healthy men. J Clin Endocrinol Metab 86:724–731
Morley JE, Melmed S (1979) Gonadal dysfunction in systemic disorders. Metabolism 28:1051–1073
Bailey JL, Zheng B, Hu Z, Price SR, Mitch WE (2006) Chronic kidney disease causes defects in signalling through the insulin receptor substrate/phosphatidylinositol 3-kinase/Akt pathway: implications for muscle atrophy. J Am Soc Nephrol 17:1388–1394
Pupim LB, Flakoll PJ, Majchrzak KM (2005) Aftab Guy DL, Stenvinkel P, Ikizler TA. Increased muscle protein breakdown in chronic hemodialysis patients with type 2 diabetes mellitus. Kidney Int 68:1857–1865
Vanholder R, Ringoir S (1993) Infectious morbidity and defects of phagocytic function in end-stage renal disease: a review. J Am Soc Nephrol 3:1541–1554
Nguyen-Khoa T, Massay ZA, De Bandt JP, Kebede M, Salama L, Lambrey G, Witko-Sarsat V, Drüeke TB, Lacour B, Thévenin M (2001) Oxidative stress and haemodialysis: role of inflammation and duration of dialysis treatment. Nephrol Dial Transpl 16:335–340
Panichi V, Migliori M, De Pietro S, Taccola D, Bianchi AM, Giovannini L, Norpoth M, Metelli MR, Cristofani R, Bertelli AA, Sbragia G, Tetta C, Palla R, Colombo R (2002) C-reactive protein and interleukin-6 levels are related to renal function in predialytic chronic renal failure. Nephron 91:594–600
Bao Y, Dalrymple L, Chertow GM, Kaysen GA, Johansen KL (2012) Frailty, dialysis initiation, and mortality in end-stage renal disease. Arch Intern Med 172(14):1071–1077
Eustace JA, Astor B, Muntner PM, Ikizler TA, Coresh J (2004) Prevalence of acidosis and inflammation and their association with low serum albumin in chronic kidney disease. Kidney Int 65:1031–1040
Macías Núñez JF, Ghais Z, Bustamante J, Lopez-Novoa JM, Arrieta J, Barril G, Del Pino MD, Escaja C, Martín IM, Fernández Andrade C, García F, Núñez J, Onaindía JM, González J, Pérez-Prieto M, Fernández M, Lopez J, Santiago JM, Vicens M, Sousa F (2010) Evaluation of oxidant-antioxidant balance in patients on maintenance haemodialysis: a comparative study ofdialyzers membranes. Nephron Clin Pract 114(1):c67–c73
Huang CX, Tighiouart H, Beddhu S, Cheung AK, Dwyer JT, Eknoyan G, Beck GJ, Levey AS, Sarnak MJ (2010) Both low muscle mass and low fat are associated with higher all-cause mortality in hemodialysis patients. Kidney Int 77:624–629
Kutner NG, Zhang R, Huang Y, Wasse H (2014) Gait speed and hospitalization among ambulatory hemodialysis patients: USRDS special study data. World J Nephrol 3(3):101–106
Arnold RM, Zeidel ML (2009) Dialysis in frail elders—a role for palliative care. N Engl J Med 361(16):1597–1598
Burns A, Davenport A (2010) Functional status of elderly adults receiving dialysis. N Engl J Med 362(5):468
Jassal SV, Chiu E, Hladunewich M (2009) Loss of independence in patients starting dialysis at 80 years of age or older. N Engl J Med 361(16):1612–1613
Kurella Tamura M, Covinsky KE, Chertow GM, Yaffe K, Landefeld CS, McCulloch CE (2009) Functional status of elderly adults before and after initiation of dialysis. N Engl J Med 361(16):1539–1547
Roderick PJ (2011) Chronic kidney disease in older people: a cause for concern? Nephrol Dial Transpl 26(10):3083–3086
Musso CG, Trigka K, Dousdampanis P, Jauregui J (2015) Therapeutic alternatives and palliative care for advanced renal disease in the very elderly: a review of the literature. Int Urol Nephrol 47(4):647–654
Johansen KL, Chertow GM, Jin C, Kutner NG (2007) Significance of frailty among dialysis patients. J Am Soc Nephrol 18(11):2960–2967
Rockwood K, Song X, MacKnight C, Bergman H, Hogan DB, McDowell I, Mitnitski A (2005) A global clinical measure of fitness and frailty in elderly people. CMAJ 173(5):489–495
Jauregui JR, Kecskes C, Patiño O, Musso CG, Galich A, Rodota L (2012) Sarcopenia. A relevant entity in the very elderly. Rev Hop Ital B Aires 32(4):162–168
Painter P, Kuskowski M (2013) A closer look at frailty in ESRD: getting the measure right. Hemodial Int 17(1):41–49
Clegg A, Young J, Iliffe S, Rikkert MO, Rockwood K (2013) Frailty in elderly people. Lancet 381(9868):752–762. doi: 10.1016/S0140-6736(12)62167-9. Review. Erratum in: Lancet. 2013 Oct 19;382(9901):1328
Boirie Y, Gachon P, Cordat N, Ritz P, Beaufrère B (2001) Differential insulin sensitivities of glucose, amino acid, and albumin metabolism in elderly men and women. J Clin Endocrinol Metab 86:638–644
Katz S, Akpom CA (1976) A measure of primary sociobiological functions. Int J Health Serv 6:493–508
Pianta TF, Kutner NG (1999) Improving physical functioning in the elderly dialysis patient: relevance of physical therapy. ANNA J 26(1):11–14
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declare to have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Appendix
Appendix
Frailty phenotype domains Fried et al. [7]
-
Shrinking: ≥10 pound (4.5 kg) of unintentionally weight loss in prior year.
-
Weakness: Grip strength in the lowest 20 % at baseline, adjusted to gender and body mass index.
-
Poor endurance and energy: Self-report exhaustion.
-
Slowness: Walking time/15 feet (4.5 m)—slowest 20 % The slowest 20 %, adjusting to gender and standing height.
-
Low physical activity level: Kilocalories (Kcals) expended per week—lowest 20 %.
Male: <383 Kcals/week.
Female: <270 Kcals/week.
Comorbidity Fried et al. [7]
Presence of 4 or more of the following conditions: peripheral vascular disease, rheumatoid arthritis, cancer, hypertension, chronic obstructive pulmonary disease, diabetes, congestive heart failure, angina, and myocardial infarction.
Disability Fried et al. [7, 47]
Inability to perform at least 2 of the following domains without assistance: feeding, dressing, ambulation, grooming, using a toilet, and bathing.
Clinical frailty scale [13, 43]
Very fit | People who are robust, active, energetic and motivated. These people commonly exercise regularly. They are among the fittest for their age |
Well | People who have no active disease, symptoms but are less fit than category 1. Often, they exercise or are very active occasionally |
Managing well | People whose medical problems are well controlled, but are not regularly active beyond routine walking |
Vulnerable | While not dependent on others for daily help, often symptoms limit activities. A common complaint is being “slowed up”, and/or being tired during the day |
Mildly frail | These people often have more evident slowing and need help in high orders (finances, medication, transportation, heavy housework) |
Moderately frail | People need help with all outdoor activities. Indoors they need help with housekeeping, and often have problems with stairs. They also need help with bathing and might need minimal assistance with dressing |
Severely frail | Completely dependent for personal care, from either cause (physical or cognitive). Even so, they seem stable and not at high risk of dying |
Very Severely frail | Completely dependent, and approaching the end of life (within 6 months) |
Terminally ill | Approaching the end of life. This category applies to any people with a life expectancy <6 months, who are not otherwise evidently frail |
If dementia is present, the degree of frailty usually corresponds to the degree of dementia
-
Mild dementia: includes forgetting the details of a recent events though still remembering the event itself, repeating the same question/story and social withdrawal
-
Moderate dementia: recent memory is very impaired, even though they seemingly can remember their past life events well. They can do personal care with prompting
-
Severe dementia: they cannot do personal care without help
Rights and permissions
About this article
Cite this article
Musso, C.G., Jauregui, J.R. & Macías Núñez, J.F. Frailty phenotype and chronic kidney disease: a review of the literature. Int Urol Nephrol 47, 1801–1807 (2015). https://doi.org/10.1007/s11255-015-1112-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-015-1112-z