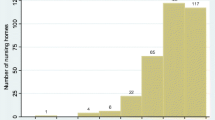
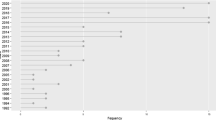
Abstract
Nursing homes may respond to the pressure to reduce costs by reducing quality of care, so the two are related. This study examines the determinants of nursing home costs and cost efficiency, and investigates how various measures of nursing home care quality influence both of these. It applies a one-step stochastic frontier approach to a large panel of California nursing homes surveyed between 2009 and 2013. Quality is measured by three different ratings available on the Nursing Home Compare website: rating on quality measures, rating on the health inspection, and rating on staffing levels. Results show that the rating on quality measures, an outcome-based measure of quality, is inversely related to costs but unrelated to mean cost efficiency. In other words, a better rating on quality measures is associated with lower nursing home costs. The health inspection rating is not associated with either costs or mean cost efficiency. The rating for staffing levels, a structural measure of quality, is negatively associated with cost efficiency. These findings reveal that different measures of quality have different relationships with costs and cost efficiency. The findings suggest that better quality outcomes in nursing homes may be achievable with fewer resources and/or improved care procedures, which in turn should reduce nursing home costs.

Similar content being viewed by others
References
Arrow KJ (1963) Uncertainty and the welfare economics of medical care. Am Econ Rev 53(5):941–973, Retrieved from http://www.jstor.org/stable/1812044
Donabedian A (1980) The definition of quality and approaches to its assessment. exploration in quality assessment and monitoring, volume 1. Health Administration Press, Ann Arbor
Laine J, Linna M, Hakkinen U, Noro A (2005) Measuring the productive efficiency and clinical quality of institutional long-term care for the elderly. Health Econ 14:245–256
Konetzka RT, Norton EC, Kilpatrick KE (2004) Effects of Medicare payment changes on nursing home staffing and deficiencies. Health Serv Res 39(3):463–488
Anderson R, Lewis D, Webb J (1999) The efficiency of nursing home chains and the implications of non-profit status. J Real Estate Portfolio Manag 5(3):235–245
Björkgren MA, Häkkinen U, Linna M (2001) Measuring efficiency of long-term care units in Finland. Health Care Manag Sci 4(3):193–200
D’Amico F, Fernandez JL (2012) Measuring inefficiency in long-term care commissioning: evidence from English Local authorities. Appl Econ Perspect Policy 34(2):275–299
Duffy JAM, Fitzsimmons JA, Jain N (2006) Identifying and studying best-performing services: an application of DEA to long-term care. Benchmarking: Int J 13(3):232–251
Heimeshoff M, Schreyӧgg J, Kwietnieski L (2014) Cost and technical efficiency of physician practices: a stochastic frontier approach using panel data. Health Care Manag Sci 17:150–161
Knox KJ, Blankmeyer EC, Stutzman JR (2006) Comparative performance and quality among nonprofit nursing facilities in Texas. Nonprofit Volunt Sect Q 35(4):631–667
Murillo-Zamarano LR, Petraglia C (2011) Technical efficiency in primary health care: does quality of care matter? Europ J Health Econo 12:115–125
Rosko MD, Chilingerian J, Zinn J, Aaronson W (1995) The effects of ownership, operating environment, and strategic choices on nursing home efficiency. Med Care 33:1001–1021
Laine J, Linna M, Noro A, Hakkinen U (2005) The cost efficiency and clinical quality of institutional long-term care for the elderly. Health Care Manag Sci 8:149–156
Zhang NJ, Unruh L, Wan TTH (2008) Has the Medicare prospective payment system led to increased nursing home efficiency? Health Serv Res 43(3):1043–1061
Shimshak DG, Lenard MG, Klimberg RK (2009) Incorporating quality into data envelope analysis of nursing home performance: a case study. Omega 37:627–685
Garavaglia G, Letterri E, Agasisti T, Lopez S (2011) Efficiency and quality of care in nursing homes: an Italian case study. Health Care Manag Sci 14:22–35
DeLellis NO, Ozcan YA (2013) Quality outcomes among efficient and inefficient nursing homes: a national study. Health Care Manag Rev 38(2):156–165
Rosko M, Mutter R (2008) stochastic frontier analysis of hospital inefficiency: a review of empirical issues and an assessment of robustness. Med Care Res Rev 65:131–166
Greene W (2004) Distinguishing between heterogeneity and inefficiency: stochastic frontier analysis of the world health organization’s panel data on national health care systems. Health Econ 13:959–980
Newhouse J (1994) Frontier estimation: how useful a tool for health economics? J Health Econ 13:317–322
Meeusen W, van den Broeck J (1977) Efficiency estimation from Cobb-Douglass production functions with composed error. Int Econ Rev 18:435–444
Aigner D, Lovell K, Schmidt P (1977) Formulation and estimation of stochastic frontier production models. J Econ 6:21–37
Coelli T, Rao D, O’Donnell C et al. (2005) An introduction to efficiency and productivity analysis (2nd ed.). New York
The Centers for Medicare and Medicaid Services (2014) http://www.medicare.gov/NursingHomeCompare/About/Ratings.html. Last accessed June 4, 2015
Abt Associates Inc. (2014) Nursing home compare five-star quality rating system: year five report. http://www.cms.gov/Medicare/Provider-Enrollment-and- Certification/CertificationandComplianc/Downloads/NHC-Year-Five-Report.pdf. Last accessed June 9, 2015
Rosko MD, Mutter RL (2014) The association of hospital cost-inefficiency with certificate-of-need regulation. Med Care Res Rev 71(3):280–298
Battese GE, Coelli TJ (1995) A model for technical inefficiency effects in a stochastic frontier production function for panel data. Empir Econ 20(2):325–332
Battese G, Heshmati A, Hjalmarsson L (2000) Efficiency of labour use in the Swedish banking industry: a stochastic frontier approach. Empir Econ 25:623–640
Herr A (2008) Cost and technical efficiency of German hospitals: does ownership matter? Health Econ 17(9):1057–1071
Grannemann T, Brown R, Pauly M (1986) Estimating hospital costs: a multiple-output analysis. J Health Econ 5:107–127
Cohen JW, Spector WD (1996) The effect of Medicaid reimbursement on quality of care in nursing homes. J Health Econ 15(1):23–48
Ozcan YA, Wogen SE, Mau LW (1998) Efficiency evaluation of skilled nursing facilities. J Med Syst 22(4):211–223
Grabowski DC, Angelelli JJ, Mor V (2004) Medicaid payment and risk-adjusted nursing home quality measures. Health Aff 23(5):243–252
Wang HJ (2002) Heteroscedasticity and non-monotonic efficiency effects of a stochastic frontier model. J Prod Anal 18(3):241–253
Author information
Authors and Affiliations
Corresponding author
Appendices
Appendix A: Measures of quality for long-stay and short-stay residents
Quality measures for long-stay residents are:
-
1.
Percent of residents whose need for help with daily activities has increased.
-
2.
Percent of high risk residents with pressure sores.
-
3.
Percent of residents who had a bladder inserted and left in the bladder.
-
4.
Percent of residents who were physically restrained.
-
5.
Percent of residents with a urinary tract infection.
-
6.
Percent of residents who self-report moderate to severe pain.
-
7.
Percent of residents experiencing one or more falls with major injury.
Quality measures for short-stay residents are:
-
1.
Percent of residents with pressure ulcers (sores) that are new and worsened.
-
2.
Percent of residents who self-report moderate to severe pain.
Appendix B: Case-mix index calculation
Following Cohen and Spector [31], the case mix index of a nursing home is measured at the facility-level as the number of minutes of staff time required for the care of the average resident. More specifically, using weights based on the management minutes system developed by Thoms and Schlesinger, the case-mix index is calculated as:
where
- A:
-
percentage of patients needing full assistance bathing
- B:
-
percentage of patients needing partial assistance bathing
- C:
-
percentage of patients needing full assistance dressing
- D:
-
percentage of patients needing partial assistance dressing
- E:
-
percentage of patients catheterized
- F:
-
percentage of patients incontinent
- G:
-
percentage of patients needing parental feeding
- H:
-
percentage of patients needing tube feeding
- I:
-
percentage of needing assistance eating
- J:
-
percentage of patients non-ambulatory
- K:
-
percentage of patients with pressure sores
- L:
-
percentage of patients receiving bowl/bladder retraining, and
- M:
-
percentage of patients receiving special skin care.
Rights and permissions
About this article
Cite this article
Dulal, R. Cost efficiency of nursing homes: do five-star quality ratings matter?. Health Care Manag Sci 20, 316–325 (2017). https://doi.org/10.1007/s10729-016-9355-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10729-016-9355-5