Abstract
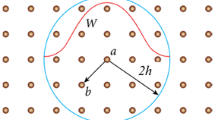
This study was designed to investigate the effect of sinotubular junction and sinus diameters on aortic valve closure to prevent the regurgitation of blood from the aorta into the left ventricle during ventricular diastole. The 2-dimensional geometry of a base aortic valve was reconstructed using the geometric constraints and modeling dimensions suggested by literature as the reference model A (aortic annulus diameter (DAA) = 26, diameters of sinotubular junction (DSTJ) = 26, sinus diameter (DS) = 40), and then the DSTJ and DS were modified to create five geometric models named as B (DSTJ = 31.2, DS = 40), C (DSTJ = 20.8, DS = 40), D (DSTJ = 26, DS = 48), E (DSTJ = 26, DS = 32) and F (DSTJ = 31.2, DS = 48) with different dimensions. Fluid structure interaction method was employed to simulate the movement and mechanics of aortic root. The performance of the aortic root was quantified in terms of blood flow velocity through aortic valve, annulus diameter as well as leaflet contact pressure. For comparison among A, B and C, the differences of annulus diameter and leaflet contact pressure do not exceed 5% with DSTJ increased by 1.2 times and decreased by 0.8 times. For comparison among A, D and E, annulus diameter was increased by 6.92% and decreased by 7.87%, and leaflet contact pressure was increased by 8.99% and decreased by 12.14% with DS increased by 1.2 times and decreased by 0.8 times. For comparison between A and F, annulus diameter was increased by 5.10%, and leaflet contact pressure was increased by 13.54% both with DSTJ and DS increased by 1.1 times. The results of leaflet contact pressure presented for all models were consistent with those of aortic annulus diameters. For the Ross operation involves replacing the diseased aortic valve, aortic valve closure function can be affected by various sinotubular junction and sinus diameter. Compared with the sinus diameters, sinotubular junction diameters have less effect on the performance of aortic valve closure, when the diameter difference is within a range of 20%. So surgical planning might give sinus diameter more consideration.





Similar content being viewed by others
References
David, T. E. Surgical treatment of aortic valve disease. Nat. Rev. Cardiol. 10:375–386, 2013.
David, T. E., A. Omran, G. Webb, H. Rakowski, S. Armstrong, and Z. Sun. Geometric mismatch of the aortic and pulmonary roots causes aortic insufficiency after the Ross procedure. J. Thorac. Cardiovasc. Surg. 112:1231–1239, 1996.
Dumont, K., J. Vierendeels, R. Kaminsky, G. Van Nooten, P. Verdonck, and D. Bluestein. Comparison of the hemodynamic and thrombogenic performance of two bileaflet mechanical heart valves using a CFD/FSI model. J. Biomech. Eng. 129:558–565, 2007.
Griffith, B. E., X. Luo, D. M. McQueen, and C. S. Peskin. Simulating the fluid dynamics of natural and prosthetic heart valves using the immersed boundary method. Int. J. Appl. Mech. 1:137–177, 2009.
Kemp, I., K. Dellimore, R. Rodriguez, C. Scheffer, D. Blaine, H. Weich, and A. Doubell. Experimental validation of the fluid–structure interaction simulation of a bioprosthetic aortic heart valve. Australas. Phys. Eng. Sci. 36:363–373, 2013.
Labrosse, M. R., K. Lobo, and C. J. Beller. Structural analysis of the natural aortic valve in dynamics: from unpressurized to physiologically loaded. J. Biomech. 43:1916–1922, 2010.
Labrosse, M. R., M. Boodhwani, B. Sohmer, and C. J. Beller. Modeling leaflet correction techniques in aortic valve repair: a finite element study. J. Biomech. 44:2292–2298, 2011.
Labrosse, M. R., C. J. Beller, F. Robicsek, and M. J. Thubrikar. Geometric modeling of functional trileaflet aortic valves: development and clinical applications. J. Biomech. 39:2665–2672, 2006.
Marom, G., R. Haj-Ali, E. Raanani, H. J. Schäfers, and M. Rosenfeld. A fluid–structure interaction model of the aortic valve with coaptation and compliant aortic root. Med. Biol. Eng. Comput. 50:173–182, 2012.
Marom, G., R. Halevi, R. Haj-Ali, M. Rosenfeld, H. J. Schäfers, and E. Raanani. Numerical model of the aortic root and valve: optimization of graft size and sinotubular junction to annulus ratio. J. Thorac. Cardiovasc. Surg. 146:1227–1231, 2013.
Marom, G., R. Haj-Ali, M. Rosenfeld, H. J. Schäfers, and E. Raanani. Aortic root numeric model: annulus diameter prediction of effective height and coaptation in post-aortic valve repair. J. Thorac. Cardiovasc. Surg. 145:406–411, 2013.
Maselli, D., R. De Paulis, R. Scaffa, L. Weltert, A. Bellisario, A. Salica, and A. Ricci. Sinotubular junction size affects aortic root geometry and aortic valve function in the aortic valve reimplantation procedure: an in vitro study using the Valsalva graft. Ann. Thorac. Surg. 84:1214–1218, 2007.
Mokhles, M. M., H. Körtke, U. Stierle, O. Wagner, E. I. Charitos, A. J. Bogers, and J. J. Takkenberg. Survival comparison of the ross procedure and mechanical valve replacement with optimal self-management anticoagulation therapy propensity-matched cohort study. Circulation 123:31–38, 2011.
Prodromo, J., G. D’Ancona, A. Amaducci, and M. Pilato. Aortic valve repair for aortic insufficiency: a review. J. Cardiothor. Vasc. Anest. 26:923–932, 2012.
Soncini, M., E. Votta, S. Zinicchino, V. Burrone, A. Mangini, M. Lemma, and A. Redaelli. Aortic root performance after valve sparing procedure: a comparative finite element analysis. Med. Eng. Phys. 31:234–243, 2009.
Shadden, S. C., M. Astorino, and J. F. Gerbeau. Computational analysis of an aortic valve jet with Lagrangian coherent structures. Interdiscip. J. Nonlinear Sci. 20:017512, 2010.
Slater, M., I. Shen, K. Welke, C. Komanapalli, and R. Ungerleider. Modification to the Ross procedure to prevent autograft dilatation. Semin. Thorac. Cardiovasc. Surg. Pediatr. Cardiac Surg. Annu. 8:181–184, 2005.
Takkenberg, J. J., L. M. Klieverik, P. H. Schoof, R. J. van Suylen, van L. A. Herwerden, P. E. Zondervan, and A. J. Bogers. The Ross procedure a systematic review and meta-analysis. Circulation 119:222–228, 2009.
Takkenberg, J. J., L. A. Van Herwerden, T. W. Galema, J. A. Bekkers, V. E. Kleyburg-Linkers, M. J. Eijkemans, and A. J. Bogers. Serial echocardiographic assessment of neo-aortic regurgitation and root dimensions after the modified Ross procedure. J. Heart Valve Dis. 15:100–106, 2006.
Uddin, A., J. D. Thomson, S. Plein, and J. P. Greenwood. Late dynamic right ventricular outflow obstruction after the Ross procedure for bicuspid aortic valve disease. Circulation 125:e1043–e1046, 2012.
Yacoub, M. H., L. M. Klieverik, G. Melina, S. E. Edwards, P. Sarathchandra, A. J. Bogers, and J. J. Takkenberg. An evaluation of the Ross operation in adults. J. Heart Valve Dis. 15:531–539, 2006.
Zhu, D., and Q. Zhao. Dynamic normal aortic root diameters: implications for aortic root reconstruction. Ann. Thorac. Surg. 91:485–489, 2011.
Acknowledgments
This work was supported by National Natural Science Foundation of China (11472023, 81270297).
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Umberto Morbiducci oversaw the review of this article.
Rights and permissions
About this article
Cite this article
Pan, Y., Qiao, A. & Dong, N. Fluid–Structure Interaction Simulation of Aortic Valve Closure with Various Sinotubular Junction and Sinus Diameters. Ann Biomed Eng 43, 1363–1369 (2015). https://doi.org/10.1007/s10439-014-1120-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-014-1120-7