Abstract
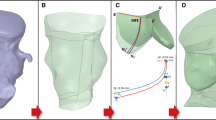
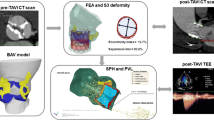
Aortic root rupture is one of the most severe complications of transcatheter aortic valve implantation (TAVI). The mechanism of this adverse event remains mostly unknown. The purpose of this study was to obtain a better understanding of the biomechanical interaction between the tissue and stent for patients with a high risk of aortic rupture. We simulated the stent deployment process of three TAVI patients with high aortic rupture risk using finite element method. The first case was a retrospective analysis of an aortic rupture case, while the other two cases were prospective studies, which ended with one canceled procedure and one successful TAVI. Simulation results were evaluated for the risk of aortic root rupture, as well as coronary artery occlusion, and paravalvular leak. For Case 1, the simulated aortic rupture location was the same as clinical observations. From the simulation results, it can be seen that the large calcified spot on the interior of the left coronary sinus between coronary ostium and the aortic annulus was pushed by the stent, causing the aortic rupture. For Case 2 and Case 3, predicated results from the simulations were presented to the clinicians at multidisciplinary pre-procedure meetings; and they were in agreement with clinician’s observations and decisions. Our results indicated that the engineering analysis could provide additional information to help clinicians evaluate complicated, high-risk aortic rupture cases. Since a systematic study of a large patient cohort of aortic rupture is currently not available (due to the low occurrence rate) to clearly understand underlying rupture mechanisms, case-by-case engineering analysis is recommended for evaluating patient-specific aortic rupture risk.







Similar content being viewed by others
References
Auricchio F, Conti M, Morganti S, Reali A (2013) Simulation of transcatheter aortic valve implantation: a patient-specific finite element approach. Comput Methods Biomech Biomed Eng. doi:10.1080/10255842.2012.746676
Barbanti M, Yang TH, Tamburino C, Wood DA, Jilaihawi H, Blanke P, Makkar RR, Latib A, Colombo A, Tarantini G, Raju R, Binder RK, Nguyen G, Freeman M, Ribeiro HB, Kapadia S, Min J, Feuchtner G, Gurtvich R, Alqoofi F, Pelletier M, Ussia GP, Napodano M, de Brito FS, Kodali S Jr, Norgaard BL, Hansson NC, Pache G, Canovas SJ, Zhang H, Leon MB, Webb JG, Leipsic J (2013) Anatomical and procedural features associated with aortic root rupture during balloon-expandable transcatheter aortic valve replacement. Circulation 128(3):244–253. doi:10.1161/CIRCULATIONAHA.113.002947
Berdajs D (2013) Aortic root rupture: implications of catheter-guided aortic valve replacement. Curr opin cardiol 28(6):632–638. doi:10.1097/HCO.0b013e3283655bb5
Capelli C, Bosi GM, Cerri E, Nordmeyer J, Odenwald T, Bonhoeffer P, Migliavacca F, Taylor AM, Schievano S (2012) Patient-specific simulations of transcatheter aortic valve stent implantation. Med Biol Eng Comput 50(2):183–192
Capelli C, Nordmeyer J, Schievano S, Lurz P, Khambadkone S, Lattanzio S, Taylor AM, Petrini L, Migliavacca F, Bonhoeffer P (2010) How do angioplasty balloons work: a computational study on balloon expansion forces. Eurointervention 6(5):638–642
Cribier A (2012) Development of transcatheter aortic valve implantation (TAVI): A 20-year odyssey. Arch Cardiovasc Dis 105(3):146–152.doi:10.1016/j.acvd.2012.01.005
Cribier A, Eltchaninoff H, Bash A, Borenstein N, Tron C, Bauer F, Derumeaux G, Anselme F, Laborde F, Leon MB (2002) Percutaneous transcatheter implantation of an aortic valve prosthesis for calcific aortic stenosis: first human case description. Circulation 106(24):3006–3008
De Beule M, Mortier P, Carlier SG, Verhegghe B, Van Impe R, Verdonck P (2008) Realistic finite element-based stent design: the impact of balloon folding. J Biomech 41(2):383–389
Ebenstein DM, Coughlin D, Chapman J, Li C, Pruitt LA (2009) Nanomechanical properties of calcification, fibrous tissue, and hematoma from atherosclerotic plaques. J Biomed Mater Res A 91(4):1028–1037
Eker A, Sozzi FB, Civaia F, Bourlon F (2012) Aortic annulus rupture during transcatheter aortic valve implantation: safe aortic root replacement. Eur J Cardiothorac Surg 41(5):1205. doi:10.1093/ejcts/ezr146
Gasser TC, Ogden RW, Holzapfel GA (2006) Hyperelastic modelling of arterial layers with distributed collagen fibre orientations. J R Soc Interface 3(6):15–35
Gervaso F, Capelli C, Petrini L, Lattanzio S, Di Virgilio L, Migliavacca F (2008) On the effects of different strategies in modelling balloon-expandable stenting by means of finite element method. J Biomech 41(6):1206–1212. doi:10.1016/j.jbiomech.2008.01.027
Gessat M, Hopf R, Pollok T, Russ C, Frauenfelder T, Sundermann SH, Hirsch S, Mazza E, Szekely G, Falk V (2014) Image-based mechanical analysis of stent deformation: concept and exemplary implementation for aortic valve stents. IEEE Trans Biomed Eng 61(1):4–15. doi:10.1109/TBME.2013.2273496
Hayashida K, Bouvier E, Lefevre T, Hovasse T, Morice MC, Chevalier B, Romano M, Garot P, Farge A, Donzeau-Gouge P, Cormier B (2012) Potential mechanism of annulus rupture during transcatheter aortic valve implantation. Catheter Cardiovasc Interv. doi:10.1002/ccd.24524
Holzapfel GA, Sommer G, Regitnig P (2004) Anisotropic mechanical properties of tissue components in human atherosclerotic plaques. J Biomech Eng 126(5):657–665
Jeziorska M, McCollum C, Wooley DE (1998) Observations on bone formation and remodelling in advanced atherosclerotic lesions of human carotid arteries. Virchows Arch 433(6):559–565
Lange R, Bleiziffer S, Mazzitelli D, Elhmidi Y, Opitz A, Krane M, Deutsch MA, Ruge H, Brockmann G, Voss B, Schreiber C, Tassani P, Piazza N (2011a) Improvements in transcatheter aortic valve implantation outcomes in lower surgical risk patients: a glimpse into the future. J Am Coll Cardiol 59(3):280–287
Lange R, Bleiziffer S, Piazza N, Mazzitelli D, Hutter A, Tassani-Prell P, Laborde JC, Bauernschmitt R (2011b) Incidence and treatment of procedural cardiovascular complications associated with trans-arterial and trans-apical interventional aortic valve implantation in 412 consecutive patients. Eur J Cardiothorac Surg 40(5):1105–1113
Lee L, Henderson R, Baig K (2012) Successful treatment of aortic root rupture following transcatheter aortic valve implantation in a heavily calcified aorta: A novel approach to a serious complication. Catheter Cardiovasc Interv. doi:10.1002/ccd.24468
Leon MB, Smith CR, Mack M, Miller DC, Moses JW, Svensson LG, Tuzcu EM, Webb JG, Fontana GP, Makkar RR, Brown DL, Block PC, Guyton RA, Pichard AD, Bavaria JE, Herrmann HC, Douglas PS, Petersen JL, Akin JJ, Anderson WN, Wang D, Pocock S, Investigators PT (2010) Transcatheter aortic-valve implantation for aortic stenosis in patients who cannot undergo surgery. N Engl J Med 363(17):1597–1607
Lim D, Cho SK, Park WP, Kristensson A, Ko JY, Al-Hassani ST, Kim HS (2008) Suggestion of potential stent design parameters to reduce restenosis risk driven by foreshortening or dogboning due to non-uniform balloon-stent expansion. Ann Biomed Eng 36(7):1118–1129
Martin C, Pham T, Sun W (2011) Significant differences in the material properties between aged human and porcine aortic tissues. Eur J Cardiothorac Surg 40(1):28–34
Martin C, Sun W (2012) Biomechanical characterization of aortic valve tissue in humans and common animal models. J Biomed Mater Res A 100(6):1591–1599. doi:10.1002/jbm.a.34099
Messika-Zeitoun D, Serfaty JM, Brochet E, Ducrocq G, Lepage L, Detaint D, Hyafil F, Himbert D, Pasi N, Laissy JP, Iung B, Vahanian A (2010) Multimodal assessment of the aortic annulus diameter: implications for transcatheter aortic valve implantation. J Am Coll Cardiol 55(3):186–194. doi:10.1016/j.jacc.2009.06.063
Mummert J, Sirois E, Sun W (2013) Quantification of biomechanical interaction of transcatheter aortic valve stent deployed in porcine and ovine hearts. Ann Biomed Eng 41(3):577–586. doi:10.1007/s10439-012-0694-1
Ogden RW (1972) Large deformation isotropic elasticity—on the correlation of theory and experiment for incompressible rubberlike solids. Proc R Soc Lond A 326(1567):565–584. doi:10.1098/rspa.1972.0026
Pant S, Bressloff NW, Limbert G (2012) Geometry parameterization and multidisciplinary constrained optimization of coronary stents. Biomech Model Mechanobiol 11(1–2):61–82. doi:10.1007/s10237-011-0293-3
Pasic M, Unbehaun A, Dreysse S, Buz S, Drews T, Kukucka M, D’Ancona G, Seifert B, Hetzer R (2012) Rupture of the device landing zone during transcatheter aortic valve implantation: a life-threatening but treatable complication. Circ Cardiovasc Interv 5(3):424–432. doi:10.1161/CIRCINTERVENTIONS.111.967315
Rezq A, Basavarajaiah S, Latib A, Takagi K, Hasegawa T, Figini F, Cioni M, Franco A, Montorfano M, Chieffo A, Maisano F, Corvaja N, Alfieri O, Colombo A (2012) Incidence, management, and outcomes of cardiac tamponade during transcatheter aortic valve implantation: a single-center study. JACC Cardiovasc Interv 5(12):1264–1272. doi:10.1016/j.jcin.2012.08.012
Russ C, Hopf R, Hirsch S, Sundermann S, Falk V, Szekely G, Gessat M Simulation of transcatheter aortic valve implantation under consideration of leaflet calcification. In: Engineering in Medicine and Biology Society (EMBC), 2013 35th Annual International Conference of the IEEE, 3–7 July 2013 2013. pp 711–714. doi:10.1109/EMBC.2013.6609599.
Samim M, Stella PR, Agostoni P, Kluin J, Ramjankhan F, Sieswerda G, Budde R, van der Linden M, Juthier F, Banfi C, Hurt C, Hillaert M, van Herwerden L, Bertrand ME, Doevendans PA, Van Belle E (2012) A prospective “oversizing” strategy of the Edwards SAPIEN bioprosthesis: Results and impact on aortic regurgitation. J Thorac Cardiovasc Surg. doi:10.1016/j.jtcvs.2011.12.067
Smith CR, Leon MB, Mack MJ, Miller DC, Moses JW, Svensson LG, Tuzcu EM, Webb JG, Fontana GP, Makkar RR, Williams M, Dewey T, Kapadia S, Babaliaros V, Thourani VH, Corso P, Pichard AD, Bavaria JE, Herrmann HC, Akin JJ, Anderson WN, Wang D, Pocock SJ (2011) Transcatheter versus surgical aortic-valve replacement in high-risk patients. N Engl J Med 364(23):2187–2198. doi:10.1056/NEJMoa1103510
Tzamtzis S, Viquerat J, Yap J, Mullen MJ, Burriesci G (2013) Numerical analysis of the radial force produced by the Medtronic–CoreValve and Edwards-SAPIEN after transcatheter aortic valve implantation (TAVI). Med Eng Phys 35(1):125–130. doi:10.1016/j.medengphy.2012.04.009
Vad S, Eskinazi A, Corbett T, McGloughlin T, Vande Geest JP (2010) Determination of coefficient of friction for self-expanding stent-grafts. J Biomech Eng 132(12):121007
Wang Q, Book G, Primiano C, McKay R, Kodali S, Sun W (2011) Dimensional analysis of aortic root eometry during diastole using 3D models reconstructed from clinical 64-slice computed tomography images. Cardiovasc Eng Technol 2(4):324–333. doi:10.1007/s13239-011-0052-8
Wang Q, Sirois E, Sun W (2012) Patient-specific modeling of biomechanical interaction in transcatheter aortic valve deployment. J Biomech 45(11):1965–1971. doi:10.1016/j.jbiomech.2012.05.008
Acknowledgments
This work was supported in part by NIH HL104080, HL108239 grants, and AHA predoctoral fellowship 13PRE14830002. We would like to thank Dr. Raymond McKay at the Hartford Hospital, CT for providing the image data. We would also like to thank Caitlin Martin, Thuy Pham, and Kewei Li for providing experimental data of the heart tissues, and technical support provided by Dura Biotech.
Conflict of interest
All authors disclose any financial and personal relationships with other people or organizations that could inappropriately influence (bias) their work.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wang, Q., Kodali, S., Primiano, C. et al. Simulations of transcatheter aortic valve implantation: implications for aortic root rupture. Biomech Model Mechanobiol 14, 29–38 (2015). https://doi.org/10.1007/s10237-014-0583-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10237-014-0583-7