Abstract
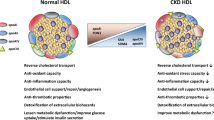
High-density lipoproteins (HDL) originate as discoidal particles that are rapidly converted by lecithin:cholesterol acyltransferase (LCAT) into the spherical particles that predominate in normal human plasma. Spherical HDL consist of multiple populations of particles that vary widely in size, composition and function. Human population studies have established that high plasma HDL cholesterol levels are associated with a reduced incidence of cardiovascular disease. The mechanistic basis of this relationship is not well understood, but most likely involves a number of the cardioprotective functions of HDL. These include the ability of apolipoprotein (apo) A-I, the main apolipoprotein constituent of HDL, to remove cholesterol from macrophages in the artery wall. HDL also have antioxidant and anti-inflammatory properties that are potentially cardioprotective. Evidence that some of these beneficial properties are compromised in people with diabetes and renal disease is emerging. Persistently elevated plasma glucose levels in people with diabetes and poor glycemic control can lead to irreversible, non-enzymatic glycation of plasma proteins, including apoA-I. Non-enzymatically glycated proteins are also prevalent in people with diabetes and end-stage renal disease who are at high cardiovascular risk. Evidence that non-enzymatically glycated apoA-I inhibits the LCAT reaction and impairs some of the cardioprotective properties of HDL is also emerging. This review is concerned with how non-enzymatic glycation of apoA-I affects the ability of LCAT to convert discoidal HDL into spherical HDL, how it affects cholesterol efflux from macrophages and how it affects the anti-inflammatory and antioxidant properties of HDL.

Similar content being viewed by others
References
Hamilton RL, Williams MC, Fielding CJ, Havel RJ. Discoidal bilayer structure of nascent high density lipoproteins from perfused rat liver. J Clin Invest. 1976;58(3):667–80.
Hara H, Yokoyama S. Interaction of free apolipoproteins with macrophages. Formation of high density lipoprotein-like lipoproteins and reduction of cellular cholesterol. J Biol Chem. 1991;266(5):3080–6.
Forte T, Norum KR, Glomset JA, Nichols AV. Plasma lipoproteins in familial lecithin: cholesterol acyltransferase deficiency: structure of low and high density lipoproteins as revealed by electron microscopy. J Clin Invest. 1971;50(5):1141–8.
Di Angelantonio E, Sarwar N, Perry P, Kaptoge S, Ray KK, Thompson A, et al. Major lipids, apolipoproteins, and risk of vascular disease. JAMA. 2009;302(18):1993–2000.
Rayner KJ, Esau CC, Hussain FN, McDaniel AL, Marshall SM, van Gils JM, et al. Inhibition of miR-33a/b in non-human primates raises plasma HDL and lowers VLDL triglycerides. Nature. 2011;478(7369):404–7.
Cockerill GW, Rye KA, Gamble JR, Vadas MA, Barter PJ. High-density lipoproteins inhibit cytokine-induced expression of endothelial cell adhesion molecules. Arterioscler Thromb Vasc Biol. 1995;15(11):1987–94.
Garner B, Waldeck AR, Witting PK, Rye KA, Stocker R. Oxidation of high density lipoproteins. II. Evidence for direct reduction of lipid hydroperoxides by methionine residues of apolipoproteins AI and AII. J Biol Chem. 1998;273(11):6088–95.
Zerrad-Saadi A, Therond P, Chantepie S, Couturier M, Rye KA, Chapman MJ, et al. HDL3-mediated inactivation of LDL-associated phospholipid hydroperoxides is determined by the redox status of apolipoprotein A-I and HDL particle surface lipid rigidity: relevance to inflammation and atherogenesis. Arterioscler Thromb Vasc Biol. 2009;29(12):2169–75.
Mineo C, Deguchi H, Griffin JH, Shaul PW. Endothelial and antithrombotic actions of HDL. Circ Res. 2006;98(11):1352–64.
Curtiss LK, Witztum JL. Plasma apolipoproteins AI, AII, B, CI, and E are glycosylated in hyperglycemic diabetic subjects. Diabetes. 1985;34(5):452–61.
Nobécourt E, Tabet F, Lambert G, Puranik R, Bao S, Yan L, et al. Nonenzymatic glycation impairs the antiinflammatory properties of apolipoprotein A-I. Arterioscler Thromb Vasc Biol. 2010;30(4):766–72.
Khera AV, Cuchel M, de la Llera-Moya M, Rodrigues A, Burke MF, Jafri K, et al. Cholesterol efflux capacity, high-density lipoprotein function, and atherosclerosis. N Engl J Med. 2011;364(2):127–35.
Brown BE, Nobécourt E, Zeng J, Jenkins AJ, Rye KA, Davies MJ. Apolipoprotein A-I glycation by glucose and reactive aldehydes alters phospholipid affinity but not cholesterol export from lipid-laden macrophages. PLoS One. 2013;8(5):e65430.
Passarelli M, Shimabukuro AF, Catanozi S, Nakandakare ER, Rocha JC, Carrilho AJ, et al. Diminished rate of mouse peritoneal macrophage cholesterol efflux is not related to the degree of HDL glycation in diabetes mellitus. Clin Chim Acta. 2000;301(1–2):119–34.
Passarelli M, Tang C, McDonald TO, O’Brien KD, Gerrity RG, Heinecke JW, et al. Advanced glycation end product precursors impair ABCA1-dependent cholesterol removal from cells. Diabetes. 2005;54(7):2198–205.
Nobécourt E, Davies MJ, Brown BE, Curtiss LK, Bonnet DJ, Charlton F, et al. The impact of glycation on apolipoprotein A-I structure and its ability to activate lecithin:cholesterol acyltransferase. Diabetologia. 2007;50(3):643–53.
Rader DJ, Ikewaki K, Duverger N, Schmidt H, Pritchard H, Frohlich J, et al. Markedly accelerated catabolism of apolipoprotein A-II (ApoA-II) and high density lipoproteins containing ApoA-II in classic lecithin: cholesterol acyltransferase deficiency and fish-eye disease. J Clin Invest. 1994;93(1):321–30.
Passarelli M, Catanozi S, Nakandakare ER, Rocha JC, Morton RE, Shimabukuro AF, et al. Plasma lipoproteins from patients with poorly controlled diabetes mellitus and “in vitro” glycation of lipoproteins enhance the transfer rate of cholesteryl ester from HDL to apo-B-containing lipoproteins. Diabetologia. 1997;40(9):1085–93.
Nicholls SJ, Dusting GJ, Cutri B, Bao S, Drummond GR, Rye KA, et al. Reconstituted high-density lipoproteins inhibit the acute pro-oxidant and proinflammatory vascular changes induced by a periarterial collar in normocholesterolemic rabbits. Circulation. 2005;111(12):1543–50.
Nicholls SJ, Cutri B, Worthley SG, Kee P, Rye KA, Bao S, et al. Impact of short-term administration of high-density lipoproteins and atorvastatin on atherosclerosis in rabbits. Arterioscler Thromb Vasc Biol. 2005;25(11):2416–21.
McGrath KC, Li XH, Puranik R, Liong EC, Tan JT, Dy VM, et al. Role of 3beta-hydroxysteroid-delta 24 reductase in mediating anti-inflammatory effects of high-density lipoproteins in endothelial cells. Arterioscler Thromb Vasc Biol. 2009;29(6):877–82.
Wu BJ, Chen K, Shrestha S, Ong KL, Barter PJ, Rye KA. High-density lipoproteins inhibit vascular endothelial inflammation by increasing 3beta-hydroxysteroid-delta24 reductase expression and inducing heme oxygenase-1. Circ Res. 2013;112(2):278–88.
Inoguchi T, Li P, Umeda F, Yu HY, Kakimoto M, Imamura M, et al. High glucose level and free fatty acid stimulate reactive oxygen species production through protein kinase C-dependent activation of NAD(P)H oxidase in cultured vascular cells. Diabetes. 2000;49(11):1939–45.
Tabet F, Lambert G, Cuesta Torres LF, Hou L, Sotirchos I, Touyz RM, et al. Lipid-free apolipoprotein A-I and discoidal reconstituted high-density lipoproteins differentially inhibit glucose-induced oxidative stress in human macrophages. Arterioscler Thromb Vasc Biol. 2011;31(5):1192–200.
Forbes JM, Coughlan MT, Cooper ME. Oxidative stress as a major culprit in kidney disease in diabetes. Diabetes. 2008;57(6):1446–54.
Robbesyn F, Garcia V, Auge N, Vieira O, Frisach MF, Salvayre R, et al. HDL counterbalance the proinflammatory effect of oxidized LDL by inhibiting intracellular reactive oxygen species rise, proteasome activation, and subsequent NF-κB activation in smooth muscle cells. Faseb J. 2003;17(6):743–5.
Acknowledgments
This work was supported by the National Health and Medical Research Council of Australia Grant 1037903.
Conflict of interest
The authors have declared that no conflict of interest exists.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Rye, KA. Biomarkers associated with high-density lipoproteins in atherosclerotic kidney disease. Clin Exp Nephrol 18, 247–250 (2014). https://doi.org/10.1007/s10157-013-0865-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-013-0865-x