Abstract
Purpose
To evaluate the self-assessed competency of graduating residents (GRs) in Japan upon completion of their residency and to identify the gap between their competency and the competency expected by their program directors (PDs).
Method
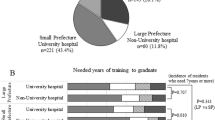
A list of 31 essential surgical procedures was compiled according to the consensus of surgical educators from around the country. A survey with this list was sent to all 909 GRs and their 611 PDs in 2016. The GRs rated their competency to perform these procedures and the PDs were asked to evaluate the expected competency of their GRs using the Zwisch Scale.
Result
The response rate was 56.3% for the GRs and 76.8% for the PDs. Fewer than half of the GRs who responded felt confident performing ten (32%) of the surgical procedures evaluated. For most procedures, the GRs’ self-reported competency was lower than the expectation reported by their PDs. This gap was more than 10% for 13 of the procedures.
Conclusion
More than half of the GRs in Japan lacked the confidence in their skill to perform one-third of the surgical procedures selected for evaluation in this study. These findings should be used to update the surgical education curriculum in Japan.
Similar content being viewed by others
References
Bucholz EM, Sue GR, Yeo H, Roman SA, Bell RH Jr, Sosa JA. Our trainees' confidence: results from a national survey of 4136 US general surgery residents. Arch Surg. 2011;146:907–14.
Friedell ML, VanderMeer TJ, Cheatham ML, Fuhrman GM, Schenarts PJ, Mellinger JD, et al. Perceptions of graduating general surgery chief residents: are they confident in their training? J Am Coll Surg. 2014;218:695–703.
Fonseca AL, Reddy V, Longo WE, Gusberg RJ. Are graduating surgical residents confident in performing open vascular surgery? Results of a national survey. J Surg Educ. 2015;72:577–84.
Fonseca AL, Reddy V, Longo WE, Gusberg RJ. Graduating general surgery resident operative confidence: perspective from a national survey. J Surg Res. 2014;190:419–28.
Fonseca AL, Reddy V, Longo WE, Udelsman R, Gusberg RJ. Operative confidence of graduating surgery residents: a training challenge in a changing environment. Am J Surg. 2014;207:797–805.
Bell RH Jr, Biester TW, Tabuenca A, Rhodes RS, Cofer JB, Britt LD, et al. Operative experience of residents in US general surgery programs: a gap between expectation and experience. Ann Surg. 2009;249:719–24.
Shofler D, Chuang T, Argade N. The residency training experience in podiatric medicine and surgery. J Foot Ankle Surg. 2015;54:607–14.
Elfenbein DM. Confidence crisis among general surgery residents: a systematic review and qualitative discourse analysis. JAMA Surg. 2016;151:1166–75.
Poudel S, Hirano S, Kurashima Y, Stefanidis D, Akiyama H, Eguchi S, et al. A snapshot of surgical resident training in Japan: results of a national-level needs assessment survey. Surg Today. 2019;49:870–6.
George BC, Teitelbaum EN, Meyerson SL, Schuller MC, DaRosa DA, Petrusa ER, et al. Reliability, validity, and feasibility of the Zwisch scale for the assessment of intraoperative performance. J Surg Educ. 2014;71:e90–96.
DaRosa DA, Zwischenberger JB, Meyerson SL, George BC, Teitelbaum EN, Soper NJ, et al. A theory-based model for teaching and assessing residents in the operating room. J Surg Educ. 2013;70:24–30.
Nadler A, Ashamalla S, Escallon J, Ahmed N, Wright FC. Career plans and perceptions in readiness to practice of graduating general surgery residents in Canada. J Surg Educ. 2015;72:205–11.
Abe T, Hachiro Y, Ebisawa Y, Hishiyama H, Kunimoto M. Distal hemorrhoidectomy with ALTA injection: a new method for hemorrhoid surgery. Int Surg. 2014;99:295–8.
Hachiro Y, Kunimoto M, Abe T, Kitada M, Ebisawa Y. Aluminum potassium sulfate and tannic acid (ALTA) injection as the mainstay of treatment for internal hemorrhoids. Surg Today. 2011;41:806–9.
Moris D, Dimitriou N, Griniatsos J. Laparoscopic splenectomy for benign hematological disorders in adults: a systematic review. Vivo. 2017;31:291–302.
Rattner DW, Apelgren KN, Eubanks WS. The need for training opportunities in advanced laparoscopic surgery. Surg Endosc. 2001;15:1066–70.
Kohnen B, Schurmeyer C, Schurmeyer TH, Kress P. Surgery of benign thyroid disease by ENT/head and neck surgeons and general surgeons: 233 cases of vocal fold paralysis in 3509 patients. Eur Arch Otorhinolaryngol. 2018;275:2397–402.
Gillman LM, Vergis A. General surgery graduates may be ill prepared to enter rural or community surgical practice. Am J Surg. 2013;205:752–7.
Debas HT, Bass BL, Brennan MF, Flynn TC, Folse JR, Freischlag JA, et al. American Surgical Association Blue Ribbon Committee Report on Surgical Education: 2004. Ann Surg. 2005;241:1–8.
Coleman JJ, Esposito TJ, Rozycki GS, Feliciano DV. Early subspecialization and perceived competence in surgical training: are residents ready? J Am Coll Surg 2013;216:764–771 (discussion 771–763).
Watanabe Y, Madani A, Bilgic E, McKendy KM, Enani G, Ghaderi I, et al. Don't fix it if it isn't broken: a survey of preparedness for practice among graduates of Fellowship Council-accredited fellowships. Surg Endosc. 2017;31:2287–98.
Klingensmith ME, Potts JR, Merrill WH, Eberlein TJ, Rhodes RS, Ashley SW, et al. Surgical training and the early specialization program: analysis of a national program. J Am Coll Surg. 2016;222:410–6.
Larson JL, Williams RG, Ketchum J, Boehler ML, Dunnington GL. Feasibility, reliability and validity of an operative performance rating system for evaluating surgery residents. Surgery. 2005;138:640–647 (discussion 647–649)
McKee R. The intercollegiate surgical curriculum programme (ISCP). Surg (Oxf). 2008;26:411–6.
Phillips AW, Madhavan A. A critical evaluation of the Intercollegiate surgical curriculum and comparison with its predecessor the "Calman" curriculum. J Surg Educ. 2013;70:557–62.
Latif A, Hopkins L, Robinson D, Brown C, Abdelrahman T, Egan R, et al. Influence of trainer role, subspecialty and hospital status on consultant workplace-based assessment completion. J Surg Educ. 2019;76:1068–75.
Acknowledgements
We acknowledge the Association of Surgical Education, Surgical Education Research Fellowship (SERF) program for supporting Dr Saseem Poudel during this project. We thank all of the individuals who participated in this survey. We also thank Hidetaka Suzuki, Takamichi Sugiyama, Suguru Kuramochi, Azumi Hirano, and the other staff members of the Japan Surgical Society Secretariat for providing us with logistical support during this study.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
Authors Saseem Poudel and the co-authors of this study have no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Poudel, S., Hirano, S., Kurashima, Y. et al. Are graduating residents sufficiently competent? Results of a national gap analysis survey of program directors and graduating residents in Japan. Surg Today 50, 995–1001 (2020). https://doi.org/10.1007/s00595-020-01981-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-020-01981-0