Abstract
Purpose
In the healing of osteoporotic vertebral fracture, global spinal mal-alignment might increase the load sharing at the fracture site and deteriorate the fracture healing. This study aimed to evaluate the effect of spinopelvic alignment on the union status of thoracolumbar osteoporosis-related vertebral compression fracture (OVCF).
Methods
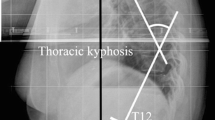
Consecutive 48 patients with a single-level thoracolumbar fresh OVCF were treated non-operatively. Union was judged by three independent observers at 6 months, and patients were divided into union group and non-union group. Spinopelvic alignment was measured using upright whole spine radiograph before treatment as follows: pelvic incidence (PI), pelvic tilt (PT), lumbar lordosis (LL), thoracic kyphosis (TK), sagittal vertical axis (SVA), and DSVA, defined as the distance from a plumb line dropped from the center of the C7 body to the center of fractured vertebral body.
Result
Global spinal alignment was different in union group and non-union group: SVA (4.7 ± 0.7 cm in union group vs. 8.9 ± 1.3 cm in non-union group, P = 0.007), DSVA (4.2 ± 0.6 cm in union group vs. 9.5 ± 1.0 cm in non-union group, P < 0.001), and PI–LL (18.9° ± 2.2° in union group vs. 30.3° ± 3.9° in non-union group, P = 0.014). Over 5 cm of DSVA [P = 0.022, adjusted odds 7.9 (95 % CI 1.3–77.0)] and/or over 30° of PI–LL [P = 0.026, adjusted odds 6.6 (95 % CI 1.5–44.2)] showed the significant risk factors for non-union using multivariate logistic regression analysis in the other background status.
Conclusions
Global spinal mal-alignment, showing over 5 cm of DSVA and/or over 30° of PI–LL, affected the union status of OVCF.



Similar content being viewed by others
References
Begerow BB (1999) Time since vertebral fracture: an important variable concerning quality of life in patients with postmenopausal osteoporosis. Osteoporos Int 10:26–33. doi:10.1007/s001980050190
Chang CYC (2015) The mortality and direct medical costs of osteoporotic fractures among postmenopausal women in Taiwan. Osteoporos Int. doi:10.1007/s00198-015-3238-3
Imai NN (2014) Mortality after hip fracture with vertebral compression fracture is poor. J Bone Miner Metab. doi:10.1007/s00774-014-0640-4
Nazrun ASAS (2014) A systematic review of the outcomes of osteoporotic fracture patients after hospital discharge: morbidity, subsequent fractures, and mortality. Ther Clin Risk Manag 10:937. doi:10.2147/tcrm.s72456
Ikeda YY (2010) Mortality after vertebral fractures in a Japanese population. J Orthop Surg (Hong Kong) 18:148
Briggs AMA (2007) The vertebral fracture cascade in osteoporosis: a review of aetiopathogenesis. Osteoporos Int 18:575–584. doi:10.1007/s00198-006-0304-x
Pappou IP, Papadopoulos EC, Swanson AN, Cammisa FP, Girardi FP (2008) Osteoporotic vertebral fractures and collapse with intravertebral vacuum sign (Kummel’s disease). Orthopedics 31:61–66. doi:10.3928/01477447-20080101-35
Hoshino M, Nakamura H, Terai H, Tsujio T, Nabeta M, Namikawa T, Matsumura A, Suzuki A, Takayama K, Takaoka K (2009) Factors affecting neurological deficits and intractable back pain in patients with insufficient bone union following osteoporotic vertebral fracture. Eur Spine J 18:1279–1286. doi:10.1007/s00586-009-1041-6
Kaneda KK (1992) The treatment of osteoporotic-posttraumatic vertebral collapse using the Kaneda device and a bioactive ceramic vertebral prosthesis. Spine (Phila Pa 1976) 17:S295–S303
Heggeness MHM (1993) Spine fracture with neurological deficit in osteoporosis. Osteoporos Int 3:215–221
Kanayama M, Ishida T, Hashimoto T, Shigenobu K, Togawa D, Oha F, Kaneda K (2010) Role of major spine surgery using Kaneda anterior instrumentation for osteoporotic vertebral collapse. J Spinal Disord Tech 23:53–56. doi:10.1097/BSD.0b013e318193e3a5
Kaneda K, Asano S, Hashimoto T, Satoh S, Fujiya M (1992) The treatment of osteoporotic posttraumatic vertebral collapse using the Kaneda device and a bioactive ceramic vertebral prosthesis. Spine 17:S295–S303. doi:10.1097/00007632-199208001-00015
Schwab FF (2012) Scoliosis Research Society-Schwab adult spinal deformity classification: a validation study. Spine (Phila Pa 1976) 37:1077–1082. doi:10.1097/BRS.0b013e31823e15e2
Myers ERE (1997) Biomechanics of osteoporosis and vertebral fracture. Spine (Phila Pa 1976) 22:25S
Yang HH (2012) Micromechanics of the human vertebral body for forward flexion. J Biomech 45:2142–2148. doi:10.1016/j.jbiomech.2012.05.044
Buckley JMJM (2009) Relative strength of thoracic vertebrae in axial compression versus flexion. Spine J 9:478–485. doi:10.1016/j.spinee.2009.02.010
Briggs AMAM (2006) The effect of osteoporotic vertebral fracture on predicted spinal loads in vivo. Eur Spine J 15:1785–1795. doi:10.1007/s00586-006-0158-0
King TT (1957) Compression of the bone ends as an aid to union in fractures; a report on forty-nine ununited and four recent fractures. J Bone Joint Surg Am 39-A:1238–1248
Georgiadis GMG (1990) Effects of dynamization after interlocking tibial nailing: an experimental study in dogs. J Orthop Trauma 4:323–330
Wu CCC (1997) The effect of dynamization on slowing the healing of femur shaft fractures after interlocking nailing. J Trauma 43:263–267
Gelalis IDID (2012) Diagnostic and treatment modalities in nonunions of the femoral shaft: a review. Injury 43:980–988. doi:10.1016/j.injury.2011.06.030
Freedman BABA (2009) Kummel disease: a not-so-rare complication of osteoporotic vertebral compression fractures. J Am Board Fam Med 22:75–78. doi:10.3122/jabfm.2009.01.080100
He DD (2016) Pathogenesis of the intravertebral vacuum of Kümmell’s disease. Exp Ther Med 12:879–882. doi:10.3892/etm.2016.3369
Dai J (2015) Relationship between sagittal spinal alignment and the incidence of vertebral fracture in menopausal women with osteoporosis: a multicenter longitudinal follow-up study. Eur Spine J 24:737–743. doi:10.1007/s00586-014-3637-8
Huang M-HMH (2006) Hyperkyphotic posture and risk of future osteoporotic fractures: the Rancho Bernardo study. J Bone Miner Res 21:419–423. doi:10.1359/jbmr.051201
Heini PFPF (2005) The current treatment—a survey of osteoporotic fracture treatment. Osteoporotic spine fractures: the spine surgeon’s perspective. Osteoporos Int 16(Suppl 2):S92. doi:10.1007/s00198-004-1723-1
Kanayama MM (2015) Does balloon kyphoplasty improve the global spinal alignment in osteoporotic vertebral fracture? Int Orthop 39:1137–1143. doi:10.1007/s00264-015-2737-3
Friedrich HCH (2011) Balloon kyphoplasty improves back pain but does not result in a permanent realignment of the thoracolumbar spine. Cent Eur Neurosurg 72:176–180. doi:10.1055/s-0031-1284415
Tsuchie HH (2016) The effect of teriparatide to alleviate pain and to prevent vertebral collapse after fresh osteoporotic vertebral fracture. J Bone Miner Metab 34:86–91. doi:10.1007/s00774-014-0646-y
Park JHJ (2014) Preventive effects of conservative treatment with short-term teriparatide on the progression of vertebral body collapse after osteoporotic vertebral compression fracture. Osteoporos Int 25:613–618. doi:10.1007/s00198-013-2458-7
Acknowledgments
We would like to express sincere gratitude to our colleagues, nurses, physical therapists, X-ray technicians, pharmacists, and clerks in our hospital who provided effort to the patients. We always thank our families for supporting our work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Akira Iwata and Norimasa Iwasaki declare that they have no conflict of interest. Masahiro Kanayama is a member of International Society for the Study of the Lumbar Spine. He has received speaker honorarium from Stryker, Medtronic, Century Medical, Taisho Toyama Pharmaceutical, Otsuka Pharma Inc., Astelas Pharma Inc., Mitsubishi Tanabe Pharma, and Depuy-Synthes. He also has received consultancy from Robert Reid Industry. Fumihiro Oha has received speaker honorarium from Depuy-Synthes. Tomoyuki Hashimoto has received speaker honorarium from Century Medical, Eisai, Taisho Toyama Pharmaceutical, Chugai Pharmaceutical, Asahikasei Pharma, Daiichi Sankyo, and Depuy-Synthes.
Research involving human participants and/or animals
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Iwata, A., Kanayama, M., Oha, F. et al. Does spinopelvic alignment affect the union status in thoracolumbar osteoporotic vertebral compression fracture?. Eur J Orthop Surg Traumatol 27, 87–92 (2017). https://doi.org/10.1007/s00590-016-1844-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-016-1844-1