Abstract
Purpose
To examine the time needed from a surgeon’s viewpoint to treat a patient operated for lumbar spinal stenosis. We firstly aimed to give evidence of the wide ranging duration of standardized procedure. Secondly, we investigated factors affecting the time allocated to each patient.
Methods
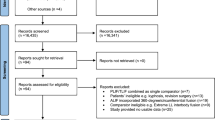
438 medical records of patients operated on for lumbar decompression without fusion (2005–2011) were retrospectively examined. Primary data were operative time (OT, min), length of stay (LoS, days) and number of postoperative visits. A fourth parameter was calculated, the time spent per patient (TSPP, min) by summing the time spent in surgery, during inpatient and outpatient follow-up visits. Factors that influenced these medical resources were examined.
Results
Median (5th–95th percentile) LoS was 5 days (2–15), OT 106 min (60–194), number of medical visits 5 (2–11) and TSPP 329 min (206–533). In descending order, factors predicting LoS were age, no. of levels, sex, operative technique, cardiovascular risk index, dural tear and haematoma. Factors predicting OT were number of levels, dural tear, foraminotomy, synovial cyst and body mass index. The statistical model could predict 36 % of the TSPP variance. We recommend that surgeons add 35 min for each level, 29 min for patients over 65 years, 30 min for women, 132 min for dural tear and 108 min for epidural haematoma.
Conclusion
TSPP treated for lumbar spinal stenosis is highly variable, yet partially predictable. These data may help individual surgeons or heads of departments to plan their activities.




Similar content being viewed by others
References
Du Bois M, Szpalski M, Donceel P (2012) A decade’s experience in lumbar spine surgery in Belgium: sickness fund beneficiaries, 2000-2009. European Spine Journal: Official Publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society
Kalichman L, Cole R, Kim DH, Li L, Suri P, Guermazi A, Hunter DJ (2009) Spinal stenosis prevalence and association with symptoms: the Framingham Study. Spine J 9:545–550
Ciol MA, Deyo RA, Howell E, Kreif S (1996) An assessment of surgery for spinal stenosis: time trends, geographic variations, complications, and reoperations. J Am Geriatr Soc 44:285–290
Deyo RA, Mirza SK (2006) Trends and variations in the use of spine surgery. Clin Orthop Relat Res 443:139–146
Weinstein JN, Tosteson TD, Lurie JD, Tosteson ANA, Blood E, Hanscom B, Herkowitz H, Cammisa F, Albert T, Boden SD, Hilibrand A, Goldberg H, Berven S, An H (2008) Surgical versus nonsurgical therapy for lumbar spinal stenosis. N Engl J Med 358:794–810
Deyo RA, Mirza SK, Martin BI, Kreuter W, Goodman DC, Jarvik JG (2010) Trends, major medical complications, and charges associated with surgery for lumbar spinal stenosis in older adults. JAMA 303:1259–1265
Fu Y-S, Zeng B-F, Xu J-G (2008) Long-term outcomes of two different decompressive techniques for lumbar spinal stenosis. Spine 33:514–518
Müslüman AM, Cansever T, Yılmaz A, Çavuşoğlu H, Yüce İ, Aydın Y (2012) Midterm outcome after a microsurgical unilateral approach for bilateral decompression of lumbar degenerative spondylolisthesis. J Neurosurg Spine 16:68–76
Yagi M, Okada E, Ninomiya K, Kihara M (2009) Postoperative outcome after modified unilateral-approach microendoscopic midline decompression for degenerative spinal stenosis. J Neurosurg Spine 10:293–299
Sasai K, Umeda M, Maruyama T, Wakabayashi E, Iida H (2008) Microsurgical bilateral decompression via a unilateral approach for lumbar spinal canal stenosis including degenerative spondylolisthesis. J Neurosurg Spine 9:554–559
Cavuşoğlu H, Kaya RA, Türkmenoglu ON, Tuncer C, Colak I, Aydin Y (2007) Midterm outcome after unilateral approach for bilateral decompression of lumbar spinal stenosis: 5-year prospective study. Eur Spine J 16:2133–2142
Nandi S, Aghazadeh M, Talmo C, Robbins C, Bono J (2012) Perioperative clopidogrel and postoperative events after hip and knee arthroplasties. Clin Orthop Relat Res 470:1436–1441
Lee TH, Marcantonio ER, Mangione CM, Thomas EJ, Polanczyk CA, Cook EF, Sugarbaker DJ, Donaldson MC, Poss R, Ho KK, Ludwig LE, Pedan A, Goldman L (1999) Derivation and prospective validation of a simple index for prediction of cardiac risk of major noncardiac surgery. Circulation 100:1043–1049
Rao JY, Yeriswamy MC, Santhosh MJ, Shetty GG, Varghese K, Patil CB, Iyengar SS (2012) A look into Lee’s score: peri-operative cardiovascular risk assessment in non-cardiac surgeries-usefulness of revised cardiac risk index. Indian Heart J 64:134–138
Rago R, Forfori F, Materazzi G, Abramo A, Collareta M, Miccoli P, Giunta F (2012) Evaluation of a preoperative pain score in response to pressure as a marker of postoperative pain and drugs consumption in surgical thyroidectomy. Clin J Pain 28:382–386
Keats AS (1978) The ASA classification of physical status–a recapitulation. Anesthesiology 49:233–236
Faciszewski T, Broste SK, Fardon D (1997) Quality of data regarding diagnoses of spinal disorders in administrative databases. A multicenter study. J Bone Joint Surg Am 79:1481–1488
Raffo CS, Lauerman WC (2006) Predicting morbidity and mortality of lumbar spine arthrodesis in patients in their ninth decade. Spine 31:99–103
Li G, Patil CG, Lad SP, Ho C, Tian W, Boakye M (2008) Effects of age and comorbidities on complication rates and adverse outcomes after lumbar laminectomy in elderly patients. Spine 33:1250–1255
Thomé C, Zevgaridis D, Leheta O, Bäzner H, Pöckler-Schöniger C, Wöhrle J, Schmiedek P (2005) Outcome after less-invasive decompression of lumbar spinal stenosis: a randomized comparison of unilateral laminotomy, bilateral laminotomy, and laminectomy. J Neurosurg Spine 3:129–141
Desai A, Ball PA, Bekelis K, Lurie J, Mirza SK, Tosteson TD, Weinstein JN (2011) SPORT: does incidental durotomy affect long-term outcomes in cases of spinal stenosis? Neurosurgery 69:38–44 discussion 44
Strömqvist F, Jönsson B, Strömqvist B (2012) Dural lesions in decompression for lumbar spinal stenosis: incidence, risk factors and effect on outcome. Eur Spine J 21:825–828
Sobottke R, Aghayev E, Röder C, Eysel P, Delank SK, Zweig T (2012) Predictors of surgical, general and follow-up complications in lumbar spinal stenosis relative to patient age as emerged from the Spine Tango Registry. Eur Spine J 21:411–417
Athiviraham A, Wali ZA, Yen D (2011) Predictive factors influencing clinical outcome with operative management of lumbar spinal stenosis. Spine J 11:613–617
Zheng F, Cammisa FP Jr, Sandhu HS, Girardi FP, Khan SN (2002) Factors predicting hospital stay, operative time, blood loss, and transfusion in patients undergoing revision posterior lumbar spine decompression, fusion, and segmental instrumentation. Spine 27:818–824
Khoo LT, Fessler RG (2002) Microendoscopic decompressive laminotomy for the treatment of lumbar stenosis. Neurosurgery 51:S146–S154
Mirza SK, Deyo RA, Heagerty PJ, Konodi MA, Lee LA, Turner JA, Goodkin R (2008) Development of an index to characterize the “invasiveness” of spine surgery: validation by comparison to blood loss and operative time. Spine 33:2651–2661 discussion 2662
Adogwa O, Parker SL, Shau DN, Mendenhall SK, Aaronson O, Cheng JS, Devin CJ, McGirt MJ (2012) Cost per quality-adjusted life year gained of revision neural decompression and instrumented fusion for same-level recurrent lumbar stenosis: defining the value of surgical intervention. J Neurosurg Spine 16:135–140
Parker SL, Fulchiero EC, Davis BJ, Adogwa O, Aaronson OS, Cheng JS, Devin CJ, McGirt MJ (2011) Cost-effectiveness of multilevel hemilaminectomy for lumbar stenosis-associated radiculopathy. Spine J 11:705–711
Lotter O, Amr A, Chiarello P, Bihler M, Schaller H-E, Stahl S (2012) Diagnosis-Related Groups in Hand Surgery–a comparison of six European countries. Ger Med Sci 10: Doc08
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kaminski, L., Banse, X. Time spent per patient in lumbar spinal stenosis surgery. Eur Spine J 22, 1868–1876 (2013). https://doi.org/10.1007/s00586-013-2691-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-013-2691-y