Abstract
Purpose
Drain placement in retromuscular ventral hernia repair is controversial. Although it may reduce seroma formation, there is a concern regarding an increase in infectious complications. We aimed to perform a meta-analysis on retromuscular drain placement in retromuscular ventral hernia repair.
Methods
We performed a literature search of Cochrane, Scopus and PubMed databases to identify studies comparing drain placement and the absence of drain in patients undergoing retromuscular ventral hernia repair. Postoperative outcomes were assessed by pooled analysis and meta-analysis. Statistical analysis was performed using RevMan 5.4. Heterogeneity was assessed with I2 statistics.
Results
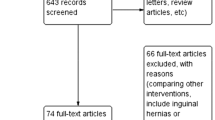
3808 studies were screened and 48 were thoroughly reviewed. Four studies comprising 1724 patients were included in the analysis. We found that drain placement was significantly associated with a decrease in seroma (OR 0.34; 95% CI 0.12–0.96; P = 0.04; I2 = 78%). Moreover, no differences were noted in surgical site infection, hematoma, surgical site occurrences or surgical site occurrences requiring procedural intervention.
Conclusions
Based on the analysis of short-term outcomes, retromuscular drain placement after retromuscular ventral hernia repair significantly reduces seroma and does not increase infectious complications. Further prospective randomized studies are necessary to confirm our findings, evaluate the optimal duration of drain placement, and report longer-term outcomes.








Similar content being viewed by others
References
Poulose BK, Shelton J, Phillips S et al (2012) Epidemiology and cost of ventral hernia repair: making the case for hernia research. Hernia 16:179–183. https://doi.org/10.1007/s10029-011-0879-9
Bower C, Roth JS (2013) Economics of abdominal wall reconstruction. Surg Clin North Am 93:1241–1253. https://doi.org/10.1016/j.suc.2013.06.007
Krpata DM, Prabhu AS, Carbonell AM et al (2017) Drain placement does not increase infectious complications after retromuscular ventral hernia repair with synthetic mesh: an AHSQC analysis. J Gastrointest Surg Off J Soc Surg Aliment Tract 21:2083–2089. https://doi.org/10.1007/s11605-017-3601-0
Miller BT, Tamer R, Petro CC et al (2022) Retromuscular drain versus no drain in robotic retromuscular ventral hernia repair: a propensity score-matched analysis of the abdominal core health quality collaborative. Hernia. https://doi.org/10.1007/s10029-022-02696-6
White TJ, Santos MC, Thompson JS (1998) Factors affecting wound complications in repair of ventral hernias. Am Surg 64:276–280
Ramshaw B, Dean J, Forman B et al (2016) Can abdominal wall reconstruction be safely performed without drains? Am Surg 82:707–712
Simchen E, Rozin R, Wax Y (1990) The Israeli study of surgical infection of drains and the risk of wound infection in operations for hernia. Surg Gynecol Obstet 170:331–337
Idrees M, Mare H, Lester L, Kariyawasam S (2021) Large ventral hernias: to drain… And what to drain… That is the question! ANZ J Surg 91:2081–2085. https://doi.org/10.1111/ans.17171
Deherkar J, Borkar P, Kakade K et al (2022) Comparative study between sublay (retrorectus) and onlay mesh placement in ventral hernia repair at a teaching hospital. Formos J Surg 55:215. https://doi.org/10.4103/fjs.fjs_123_22
Venclauskas L, Maleckas A, Kiudelis M (2010) One-year follow-up after incisional hernia treatment: results of a prospective randomized study. Hernia 14:575–582. https://doi.org/10.1007/s10029-010-0686-8
Sterne JA, Hernán MA, Reeves BC et al (2016) ROBINS-I: a tool for assessing risk of bias in non-randomized studies of interventions. BMJ 355:i4919. https://doi.org/10.1136/bmj.i4919
Sterne JAC, Savović J, Page MJ et al (2019) RoB 2: a revised tool for assessing risk of bias in randomized trials. BMJ 366:l4898. https://doi.org/10.1136/bmj.l4898
Page MJ, McKenzie JE, Bossuyt PM et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. https://doi.org/10.1136/bmj.n71
Holihan JL, Nguyen DH, Nguyen MT et al (2016) Mesh location in open ventral hernia repair: a systematic review and network meta-analysis. World J Surg 40:89–99. https://doi.org/10.1007/s00268-015-3252-9
Tastaldi L, Alkhatib H (2018) Incisional hernia repair: open retromuscular approaches. Surg Clin North Am 98:511–535. https://doi.org/10.1016/j.suc.2018.02.006
Miller BT, Baier KF, Zolin SJ et al (2022) Long-term outcomes of seromas after ventral hernia repair: a propensity score-matched analysis of the abdominal core health quality collaborative. Hernia. https://doi.org/10.1007/s10029-022-02613-x
Wysocki AP, McGowan B (2018) To drain or not to drain: supreme court has the answer. ANZ J Surg 88:115. https://doi.org/10.1111/ans.14285
Luo Y, Mohammed Jinnaah S, Masood D, Hodgson R (2021) Drain tube use in incisional hernia repair: a national survey. Hernia J Hernias Abdom Wall Surg 25:427–433. https://doi.org/10.1007/s10029-019-02115-3
Plymale MA, Harris JW, Davenport DL et al (2016) Abdominal wall reconstruction: the uncertainty of the impact of drain duration upon outcomes. Am Surg 82:207–211
Poli M, de Figueiredo S, Belyansky I, Lu R (2022) Pitfalls and complications of enhanced-view totally extraperitoneal approach to abdominal wall reconstruction. Surg Endosc. https://doi.org/10.1007/s00464-022-09843-1
Guzman-Pruneda FA, Huang L-C, Collins C et al (2021) Abdominal core quality of life after ventral hernia repair: a comparison of open versus robotic-assisted retromuscular techniques. Surg Endosc 35:241–248. https://doi.org/10.1007/s00464-020-07386-x
Lu R, Addo A, Ewart Z et al (2020) Comparative review of outcomes: laparoscopic and robotic enhanced-view totally extraperitoneal (eTEP) access retrorectus repairs. Surg Endosc 34:3597–3605. https://doi.org/10.1007/s00464-019-07132-y
Funding
No funding was received for this work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Patrícia Marcolin, Dr. Sergio Mazzola Poli de Figueiredo, Dr. Sérgio Walmir de Araújo, Marcella Mota Constante, Vítor Moura Fé de Melo and Dr. Rui-Min Diana Mao declare that they have no conflict of interest. Dr. Richard Lu received payment/honoraria for lectures and presentations from Intuitive Surgical that are unrelated to this work.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Marcolin, P., de Figueiredo, S.M.P., Constante, M.M. et al. Drain placement in retromuscular ventral hernia repair: a systematic review and meta-analysis. Hernia 27, 519–526 (2023). https://doi.org/10.1007/s10029-023-02792-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-023-02792-1