Abstract
Background
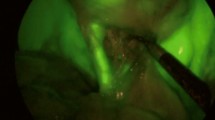
Intraoperative incisionless fluorescent cholangiogram (IOIFC) has been demonstrated to be a useful tool to increase the visualization of Calot’s triangle. This study evaluates the identification of extrahepatic biliary structures with IOIFC by medical students and surgery residents.
Methods
Two pictures were taken, one with xenon light and one with near-infrared (NIR) light, at the same stage during dissection of Calot’s triangle in ten different cases of laparoscopic cholecystectomy (LC). All twenty pictures were organized in a random fashion to remove any imagery bias. Twenty students and twenty residents were asked to identify the biliary anatomy.
Results
Medical students were able to accurately identify the cystic duct on an average 33.8 % under the xenon light versus 86 % under NIR light (p = 0.0001), the common hepatic duct (CHD) on an average 19 % under the xenon light versus 88.5 % under NIR light (p = 0.0001), and the junction on an average 24 % under xenon light versus 80.5 % under NIR light (p = 0.0001). Surgery residents were able to accurately identify the cystic duct on an average 40 % under the xenon light versus 99 % under NIR light (p = 0.0001), the CHD on an average 35 % under the xenon light versus 96 % under NIR light (p = 0.0001), and the junction on an average 24 % under the xenon light versus 95.5 % under NIR light (p = 0.0001).
Conclusions
IOIFC increases the visualization of Calot’s triangle structures when compared to xenon light. IOIFC may be a useful teaching tool in residency programs to teach LC.




Similar content being viewed by others
Abbreviations
- IOIFC:
-
Intraoperative incisionless fluorescent cholangiogram
- NIR:
-
Near infrared
- LC:
-
Laparoscopic cholecystectomy
- ICG:
-
Indocyanine green
- IOC:
-
Intraoperative cholangiogram
- CBD:
-
Common bile duct
- CHD:
-
Common hepatic duct
References
Richards MK, McAteer JP, Drake FT, Goldin AB et al (2015) A national review of the frequency of minimally invasive surgery among general surgery residents: assessment of ACGME case logs during 2 decades of general surgery resident training. JAMA Surg 150(2):169–172
Parsa CJ, Organ CH Jr, Barkan H (2000) Changing patterns of resident operative experience from 1990 to 1997. Arch Surg 135(5):570–573 discussion 3-5
Velanovich V, Morton JM, McDonald M et al (2006) Analysis of the SAGES outcomes initiative cholecystectomy registry. Surg Endosc 20(1):43–50
Davidoff AM, Pappas TN, Murray EA et al (1992) Mechanisms of major biliary injury during laparoscopic cholecystectomy. Ann Surg 215(3):196–202
Stewart L, Way LW (1995) Bile duct injuries during laparoscopic cholecystectomy. Factors that influence the results of treatment. Arch Surg 130(10):1123–1128 discussion 9
Elder S, Kunin J, Chouri H et al (1996) Safety of laparoscopic cholecystectomy on a teaching service: a prospective trial. Surg Laparosc Endosc 6(3):218–220
Arora S, Aggarwal R, Sirimanna P et al (2011) Mental practice enhances surgical technical skills: a randomized controlled study. Ann Surg 253(2):265–270
Dip F, Roy M, Lo Menzo E et al (2015) Routine use of fluorescent incisionless cholangiography as a new imaging modality during laparoscopic cholecystectomy. Surg Endosc 29(6):1621–1626
Pesce A, Piccolo G, La Greca G et al (2015) Utility of fluorescent cholangiography during laparoscopic cholecystectomy: a systematic review. World J Gastroenterol WJG 21(25):7877–7883
Dip FD, Asbun D, Rosales-Velderrain A et al (2014) Cost analysis and effectiveness comparing the routine use of intraoperative fluorescent cholangiography with fluoroscopic cholangiogram in patients undergoing laparoscopic cholecystectomy. Surg Endosc 28(6):1838–1843
Dip F, Nguyen D, Montorfano L et al (2016) Accuracy of near infrared-guided surgery in morbidly obese subjects undergoing laparoscopic cholecystectomy. Obes Surg 26(3):525–530
Cherrick GR, Stein SW, Leevy CM, Davidson CS (1960) IOC: observations on its physical properties, plasma decay, and hepatic extraction. J Clin Invest 39:592–600
Blom EM, Verdaasdonk EG, Stassen LP et al (2007) Analysis of verbal communication during teaching in the operating room and the potentials for surgical training. Surg Endosc 21(9):1560–1566
Way LW, Stewart L, Gantert W et al (2003) Causes and prevention of laparoscopic bile duct injuries: analysis of 252 cases from a human factors and cognitive psychology perspective. Ann Surg 237(4):460–469
Mirizzi PL (1950) Operative cholangiography. Revista espanola de las enfermedades del aparato digestivo y de la nutricion 9(3):306–308
Strasberg SM, Hertl M, Soper NJ (1995) An analysis of the problem of biliary injury during laparoscopic cholecystectomy. J Am Coll Surg 180(1):101–125
Aggarwal R, Darzi A (2006) Training in the operating theatre: is it safe? Thorax 61(4):278–279
Balaa F, Moloo H, Poulin EC et al (2007) Broad-based fellowships: a cornerstone of minimally invasive surgery education and dissemination. Surg Innov 14(3):205–210
Koulas SG, Tsimoyiannis J, Koutsourelakis I et al (2006) Laparoscopic cholecystectomy performed by surgical trainees. JSLS 10(4):484–487
Linn JG, Hungness ES, Clark S et al (2011) General surgery training without laparoscopic surgery fellows: the impact on residents and patients. Surgery 150(4):752–758
Fahrner R, Turina M, Neuhaus V et al (2012) Laparoscopic cholecystectomy as a teaching operation: comparison of outcome between residents and attending surgeons in 1,747 patients. Langenbecks Arch Surg 397(1):103–110
Ishizawa T, Bandai Y, Ijichi M et al (2010) Fluorescent cholangiography illuminating the biliary tree during laparoscopic cholecystectomy. Br J Surg 97(9):1369–1377
Aggarwal R, Ward J, Balasundaram I et al (2007) Proving the effectiveness of virtual reality simulation for training in laparoscopic surgery. Ann Surg 246(5):771–779
Gamarra A, Hogle NJ, Azab B et al (2012) Assessing the value of the SimPraxis laparoscopic cholecystectomy trainer. JSLS 16(2):191–194
Pucher PH, Brunt LM, Fanelli RD, Asbun HJ, Aggarwal R (2015) SAGES expert Delphi consensus: critical factors for safe surgical practice in laparoscopic cholecystectomy. Surg Endosc 29(11):3074–3085
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Mayank Roy, Fernando Dip, David Nguyen, Conrad H Simpfendorfer, Emanuele Lo Menzo, Samuel Szomstein and Raul J. Rosenthal have no conflict of interest.
Additional information
Poster presentation at the annual meeting of the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES), Boston, MA, USA March 16-19, 2016.
Rights and permissions
About this article
Cite this article
Roy, M., Dip, F., Nguyen, D. et al. Fluorescent incisionless cholangiography as a teaching tool for identification of Calot’s triangle. Surg Endosc 31, 2483–2490 (2017). https://doi.org/10.1007/s00464-016-5250-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-016-5250-x