Abstract
Purpose
To determine the influence of endometriosis on the ovarian response during controlled ovarian hyperstimulation measured by number of oocytes retrieved and the follicular output rate (FORT).
Methods
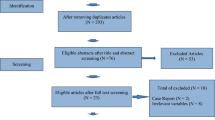
A retrospective, single center study included 96 women, who underwent ICSI treatments for male factor infertility according to World Health Organisation between 2016 until 2018. A total of 96 patients were included in the study with 205 fresh ICSI cycles. The study group included 26 patients with endometriosis after surgical and medical treatment; the control group included 70 patients without endometriosis. The women with endometriosis underwent 47 and the control group 158 ICSI cycles. Women underwent fresh intracytoplasmatic sperm injection cycles after controlled ovarian hyperstimulation following a GnRH-antagonist protocol. The FORT was calculated as the ratio of pre-ovulatory follicle count × 100/small antral follicle count at baseline.
Results
A lower number of retrieved oocytes (5.89 vs. 7.25, p = 0.045), lower FORT (75.67 vs. 94.63, p = 0.046), lower number of metaphase II oocytes (4.87 vs. 6.04, p = 0.046), and lower fertilization rate after intracytoplasmatic sperm injection (40.61 vs. 57.76, p = 0.003) were found in women with endometriosis compared to women without endometriosis. The number of oocyctes retrieved was 0.71 lower in the group with endometriosis than in the group without (p = 0.026). The FORT was 24.55% lower in the group with endometriosis (p = 0.025).
Conclusions
Endometriosis reduces the FORT and the number of metaphase-II oocytes after controlled ovarian hyperstimulation independly of women’s age, antral follicle count and anti-Müllerian hormone.
Similar content being viewed by others
References
Kennedy S, Bergqvist A, Chapron C, D’Hooghe T, Dunselman G, Greb R, Hummelshoj L, Prentice A, Saridogan E (2005) ESHRE guideline for the diagnosis and treatment of endometriosis. Hum Reprod 20:2698–2704
Giudice LC, Kao LC (2004) Endometriosis. Lancet 364:1789–1799
Ozkan S, Murk W, Arici A (2008) Endometriosis and infertility: epidemiology and evidence-based treatments. Ann NY Acad Sci 1127:92–100
Mio Y, Toda T, Harada T, Terakawa N (1992) Luteinized unruptured follcile in the early stages of endometriosis as a cause of unexplained infertility. Am J Obstet Gynecol 167:271–273
Yoo JH, Cha SH, Park CW, Kim JY, Yang KM, Song IO, Koong MK, Kang IS, Kim HO (2011) Serum anti-Mullerian hormone is a better predictor of ovarian response than FSH and age in IVF patients with endometriosis. Clin Exp Reprod Med 38:222–227
Opøien HK, Fedorcsak P, Omland AK, Abyholm T, Bjercke S, Ertzeid D, Oldereid N, Mellembakken JR, Tanbo T (2012) In vitro fertilization is a successful treatment in endometriosis-associated infertility. Fertil Steril 97:912–918
Ozkan S, Arici A (2009) Advanced in treatment options of endometriosis. Gynecol Obstet Invest 67:81–91
Jahrbuch DIR (2017) Deutsches IVF Register. https://www.deutsches-ivf-register.de/perch/resources/downloads/dir-jahrbuch-2017-deutsch-prefinal.pdf
Fauser BC, Diedrich K, Devroey P, Evian Annual Reproduction Workshop Group 2007 (2008) Predictors of ovarian response: progress towards individualized treatment in ovulation induction and ovarian stimulation. Hum Reprod Update 14(1):1–14
Tsakos E, Tolikas A, Daniilidis A, Asimakopoulos B (2014) Predictive value of anti-Müllerian hormone, follicle-stimulating hormone and antral follicle count on the outcome of ovarian stimulation in women following GnRH-antagonist protocol for IVF/ET. Arch Gynecol Obstet 290:1249–1253
Zhu M, Wang S, Yi S, Huang X, Meng J, Chen L, Sun H, Zhou J (2019) A predictive formula for selecting individual FSH starting dose based on ovarian reserve markers in IVF/ICSI cycles. Arch Gynecol Obstet. https://doi.org/10.1007/s00404-019-05156-2
Nelson SM, Yates RW, Lyall H, Jamieson M, Traynor I, Gaudoin M, Mitchell P, Ambrose P, Fleming R (2009) Anti-Müllerian hormone-based approach to controlled ovarian stimulation for assisted conception. Hum Reprod 24(4):867–875
Broer SL, Broekmans FJ, Laven JS, Fauser BC (2014) Anti-Müllerian hormone: ovarian reserve testing and its potential clinical implications. Hum Reprod Update 20(5):688–701
Pellicer A, Oliveira N, Ruiz A, Remohi J, Simon C (1995) Exploring the mechanism(s) of endometriosis-related infertility: an analysis of embryo development and implantation in assisted reproduction. Hum Reprod 2:91–97
Panidis DK, Matalliotakis IM (1998) Subfertility associated with minimal to mid endometriosis. Main mechanisms. J Reprod Med 43:1034–1042
Yovich JL, Matson PL, Richardson PA, Hilliard C (1988) Hormonal profiles and embryo quality in women with severe endometriosis treated by in vitro fertilization and embryo transfer. Fertil Steril 50:308–313
Aboulghar MA, Mansour RT, Serour GI, Al-Inany HG, Aboulghar MM (2003) The outcome of in vitro fertilization in advanced endometriosis with previous surgery: a case-controlled study. Am J Obstet Gynecol 188:371–375
Grynberg M, Labrosse J (2019) Understanding follicular output rate (FORT) and its Implications for POSEIDON criteria. Front Endocrinol (Lausanne) 10:246
Genro VK, Grynberg M, Scheffer JB, Roux I, Frydman R, Fanchin R (2011) Serum anti-Mullerian hormone levels are negatively related to follicular output rate (FORT) in normo-cycling women undergoing controlled ovarian hyperstimulation. Hum Reprod 26:671–677
Matalliotakis I, Cakmal H, Mahutte N, Fragouli Y, Arici A, Sakkas D (2007) Women with advanced-stage endometriosis and previous surgery respond less well to gonadotropin stimulation, but have similar IVF implantation and delivery rates compared with women with tubal factor infertility. Fertil Steril 88:1568–1572
Nakamura M, Yamashita Y, Hayashi A, Saito N, Yu M, Hayashi M, Terai Y, Ohmichi M (2017) Analyzing the risk factors for a diminished oocyte retrieval rate under controlled ovarian stimulation. Reprod Med Biol 16:40–44
Dong X, Liao X, Wang R, Zhang H (2013) The impact of endometriosis on IVF/ICSI outcomes. Int J Clinc Exp Pathol 6:1911–1918
Barnhart K, Dunsmoor-Su R, Coutifaris C (2002) Effect of endometriosis on in vitro fertilization. Fertil Steril 77:1148–1155
Garrido N, Navarro J, Remohi J, Simon C, Pellicer A (2000) follicular hormonal environment and embryo quality in women with endometriosis. Reprod Update 6:67–74
Safdarian L, Ghalandarpoor Attar SN, Aleyasin A, Aghahosseini M, Sarfjoo FS, Hosseinimousa S (2018) Investigation of anti-mullerian hormone (AMH) level and ovarian response in infertile women with endometriosis in IVF cycles. Int J Reprod Biomed 16(11):719–722
Ashrafi M, Fakheri T, Kiani K, Sadeghi M, Akhoond MR (2014) Impact oft he endometrioma on ovarian response and pregnancy rate in in vitro fertilization cycles. Int J Fertil Steril 8:29–34
Senapti S, Barnhart K (2011) Managing endometriosis-associated infertility. Clin Obstet Gynecol 54:720–726
Harb HM, Gallos ID, Chu J, Harb M, Coomarasamy A (2013) The effect of endometriosis on in vitro fertilzation outcome: a systematic review and meta-analysis. BJOG 120:1308–1320
Acknowledgements
The authors wish to thank Dr. Thomas Lehmann, Institute of Medical Statistics, Informatics and Documentation, University Hospital, Friedrich-Schiller-University Jena, Germany for assistance with statistical analysis.
Author information
Authors and Affiliations
Contributions
KN: protocol/project development, data collection and data management and manuscript writing/editing. DB: data collection. RS: data collection. JJ-C: statistics and data management. IH: providing the embryological data. KB: project development. IBR: manuscript writing/editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nicolaus, K., Bräuer, D., Sczesny, R. et al. Endometriosis reduces ovarian response in controlled ovarian hyperstimulation independent of AMH, AFC, and women’s age measured by follicular output rate (FORT) and number of oocytes retrieved. Arch Gynecol Obstet 300, 1759–1765 (2019). https://doi.org/10.1007/s00404-019-05337-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-019-05337-z