Abstract
Objective
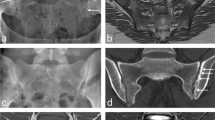
To provide magnetic resonance imaging (MRI) findings of compressive myelopathy simulating idiopathic acute transverse myelopathy (ATM).
Materials and methods
From 19,416 patients who had spinal MRI from 1 September 2004 to 10 July 2011, the patients who met inclusion criteria were enrolled as follows: (1) definable cord compression, (2) long-segmental intramedullary T2-high signal intensity (HSI) extending more than 2 vertebral segments, and (3) no history of trauma, malignancy, or demyelinating disease. The characteristics of T2-HSI and contrast enhancement pattern were analyzed. The patients’ clinical information was collected in the process.
Results
Thirteen patients (10 men, 3 women; mean age, 52.8 years; age range, 43–77 years) were included in this study. Twelve patients had cervical cord compression and one had thoracic compression. Common findings of T2-HSI included fusiform shape (100 %) with cord swelling (92.3 %), cord compression in midline location (76.9 %), diffuse distribution occupying more than two-thirds of the cross-sectional dimension of the cord in axial image (84.6 %), and focal and peripheral enhancement (63.6 %). Intravenous corticosteroid was administered to four patients, including two patients following decompressive surgery, and interval decrease in T2-HSI was seen in three patients, but with residual lesions at cord compression level.
Conclusions
Spinal cord compression can induce long-segmental cord signal change, such as idiopathic ATM.




Similar content being viewed by others
References
Kim R, Spencer S, Meredith R, et al. Extradural spinal cord compression: analysis of factors determining functional prognosis—prospective study. Radiology. 1990;176:279–82.
Yukawa Y, Kato F, Yoshihara H, Yanase M, Ito K. MR T2 image classification in cervical compression myelopathy: predictor of surgical outcomes. Spine. 2007;32:1675–8.
Ratliff J, Voorhies R. Increased MRI signal intensity in association with myelopathy and cervical instability: case report and review of the literature. Surg Neurol. 2000;53:8–13.
Takahashi M, Yamashita Y, Sakamoto Y, Kojima R. Chronic cervical cord compression: clinical significance of increased signal intensity on MR images. Radiology. 1989;173:219–24.
Ohshio I, Hatayama A, Kaneda K, Takahara M, Nagashima K. Correlation between histopathologic features and magnetic resonance images of spinal cord lesions. Spine. 1993;18:1140–9.
Matsumoto M, Toyama Y, Ishikawa M, Chiba K, Suzuki N, Fujimura Y. Increased signal intensity of the spinal cord on magnetic resonance images in cervical compressive myelopathy: does it predict the outcome of conservative treatment? Spine. 2000;25:677–82.
Fernandez de Rota JJ, Meschian S, Fernandez de Rota A, Urbano V, Baron M. Cervical spondylotic myelopathy due to chronic compression: the role of signal intensity changes in magnetic resonance images. J Neurosurg Spine. 2007;6:17–22.
Morio Y, Teshima R, Nagashima H, Nawata K, Yamasaki D, Nanjo Y. Correlation between operative outcomes of cervical compression myelopathy and MRI of the spinal cord. Spine. 2001;26:1238–45.
Chen CJ, Lyu RK, Lee ST, Wong YC, Wang LJ. Intramedullary high signal intensity on T2-weighted MR images in cervical spondylotic myelopathy: prediction of prognosis with type of intensity. Radiology. 2001;221:789–94.
Kelley BJ, Erickson BJ, Weinshenker BG. Compressive myelopathy mimicking transverse myelitis. Neurologist. 2010;16:120–2.
de Seze J, Lanctin C, Lebrun C, et al. Idiopathic acute transverse myelitis: application of the recent diagnostic criteria. Neurology. 2005;65:1950–3.
Awad A, Stüve O. Idiopathic transverse myelitis and neuromyelitis optica: clinical profiles, pathophysiology and therapeutic choices. Curr Neuropharmacol. 2011;9:417–28.
Choi KH, Lee KS, Chung SO, et al. Idiopathic transverse myelitis: MR characteristics. AJNR Am J Neuroradiol. 1996;17:1151–60.
Brinar VV, Habek M, Brinar M, Malojcic B, Boban M. The differential diagnosis of acute transverse myelitis. Clin Neurol Neurosurg. 2006;108:278–83.
Kang YS, Lee JW, Koh YH, et al. New MRI grading system for the cervical canal stenosis. AJR Am J Roentgenol. 2011;197:W134–40.
Brinar VV, Habek M, Zadro I, Barun B, Ozretic D, Vranjes D. Current concepts in the diagnosis of transverse myelopathies. Clin Neurol Neurosurg. 2008;110:919–27.
Kumar N. Pearls: myelopathy. Semin Neurol. 2010;30:38–43.
Miyanji F, Furlan JC, Aarabi B, Arnold PM, Fehlings MG. Acute cervical traumatic spinal cord injury: MR imaging findings correlated with neurologic outcome—prospective study with 100 consecutive patients. Radiology. 2007;243:820–7.
Bodley R. Imaging in chronic spinal cord injury—indications and benefits. Eur J Radiol. 2002;42:135–53.
Polman CH, Reingold SC, Edan G, et al. Diagnostic criteria for multiple sclerosis: 2005 revisions to the “McDonald Criteria”. Ann Neurol. 2005;58:840–6.
Wingerchuk D, Lennon V, Pittock S, Lucchinetti C, Weinshenker B. Revised diagnostic criteria for neuromyelitis optica. Neurology. 2006;66:1485–9.
Maus TP. Imaging of spinal stenosis: neurogenic intermittent claudication and cervical spondylotic myelopathy. Radiol Clin N Am. 2012;50:651–79.
Resnick D, Kransdorf MJ. Bone and joint imaging. Philadelphia: Elsevier; 2005.
Takahashi M, Sakamoto Y, Miyawaki M, Bussaka H. Increased MR signal intensity secondary to chronic cervical cord compression. Neuroradiology. 1987;29:550–6.
Haupts M, Haan J. Further aspects of MR-signal enhancements in stenosis of the cervical spinal canal. Neuroradiology. 1988;30:545–6.
Mizuno J, Nakagawa H, Inoue T, Hashizume Y. Clinicopathological study of “snake-eye appearance” in compressive myelopathy of the cervical spinal cord. J Neurosurg Spine. 2003;99:162–8.
Ozawa H, Sato T, Hyodo H, et al. Clinical significance of intramedullary Gd-DTPA enhancement in cervical myelopathy. Spinal Cord. 2009;48:415–22.
Boet R, Chan YL, King A, Mok CT, Poon WS. Contrast enhancement of the spinal cord in a patient with cervical spondylotic myelopathy. J Clin Neurosci. 2004;11:512–4.
Tartaglino LM, Croul SE, Flanders AE, et al. Idiopathic acute transverse myelitis: MR imaging findings. Radiology. 1996;201:661–9.
Conflict of interest
The authors declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bae, Y.J., Lee, J.W., Park, K.S. et al. Compressive myelopathy: magnetic resonance imaging findings simulating idiopathic acute transverse myelopathy. Skeletal Radiol 42, 793–802 (2013). https://doi.org/10.1007/s00256-012-1556-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-012-1556-5